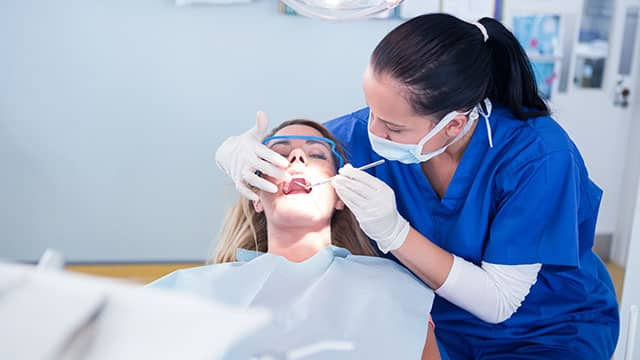
Your regular scale and polish removes plaque and tartar that has built up above the gum line since your last dentist visit, giving you the extra boost of confidence that comes with a brighter, whiter smile. Scaling and polishing also serves a more serious purpose: preventing periodontal (gum) disease.
If gum disease does develop, your hygienist will need to perform a deeper type of cleaning. Called scaling and root planing, this non-surgical procedure treats and sometimes reverses the earlier stages of periodontal disease. Read on to find out exactly what scaling and root planing involves, when you might need it, and how it can help to keep your gums healthy.
What Is Periodontal Disease?
Periodontal disease is an infection of the structures that hold your teeth in place. In the earlier stage, known as gingivitis, only the gums are affected. Plaque accumulates on the teeth and around the gums, and the bacteria in plaque irritate and inflame the gum tissue.
If left untreated, the infection can spread to the ligaments, bone and other tissues below the gum line. This is known as periodontitis, or advanced gum disease.
It causes the gum tissue to detach from your teeth, forming pockets between the gums and teeth that harbor even more plaque bacteria. As the infection attacks the bone and ligaments, the teeth loosen and can eventually fall out.
That's when scaling and root planing comes into the picture.
What Is Scaling and Root Planing?
Scaling and root planing is a two-step procedure that aims to thoroughly remove all plaque, bacteria, and tartar (calculus) deposits from your teeth and root surfaces.
Step One: Scaling
The first step is to clean the tooth surfaces. Your dentist or hygienist uses a manual hand scaler, an ultrasonic scaler, or both, to dive deeper under the gum line and clear hard-to-reach deposits.
If they use an ultrasonic scaling device, sonic vibrations will remove the plaque bacteria and tartar from the tooth surface and underneath the gum line. A manual dental scaler can do the same thing, but requires more force and is not as gentle on the teeth and gums. It is sometimes used to supplement the ultrasonic device by removing more stubborn deposits.
Step Two: Root Planing
Root planing involves an even deeper dive smooth out the root surfaces of the tooth. Smooth root surfaces keep bacteria, plaque, and tartar from re-adhering underneath the gum line. Root planing also decreases gum tissue inflammation, allowing your gums to heal and reattach themselves more firmly to your teeth.
If needed to prevent infection, your dentist might administer medicine directly into the area undergoing the procedure.
How Long Does Scaling and Root Planing Take?
In total, scaling and root planing can take 1-2 hours, depending on the amount of plaque and tartar that needs to be removed. It can be done in a single session, but some patients will have two sessions. If this is the case, half of your mouth will be cleaned in the first session and the other half in the second session. Your dentist or hygienist will be able to give you an accurate time frame based on your dental exam and unique needs.
Is Scaling and Root Planing Painful?
If your teeth and gums are particularly sensitive, you might find scaling and root planing to be uncomfortable or even painful. However, don’t let that discourage you! Your dentist or hygienist can numb the area with local anesthesia beforehand so you won’t feel any discomfort during the procedure.
Your gums might feel tender for a day or two afterwards, but your dental professional will advise you how to manage this. They may recommend you have anti-inflammatories or painkillers, like ibuprofen or acetaminophen, on hand for when your anesthesia wears off.
What Should I Expect After the Procedure?
After the procedure, your gums will be swollen for a couple of days and may bleed. Your teeth might also feel quite sensitive for up to a week afterwards. Your dentist may prescribe you pain medication if needed, and may also give you antibiotics or an antiseptic oral rinse to protect against infection.
You’ll need to schedule a follow-up visit with your dentist or hygienist. Most people get the good news that their inflamed gum tissue is once again firm and pink at this visit. Other positive signs are that the bleeding stopped, and the pockets surrounding your gum tissue are smaller.
If all looks good, you might not need any further treatment. You can then set up periodic maintenance visits. However, if the pockets have not improved or have become deeper, additional treatment might be in order. Some advanced conditions might require periodontal surgery. Your scaling and root planing treatment, though, often lessens the amount of surgery you need.
How Can I Prevent Periodontal Disease?
Gum disease can develop without warning, so it is essential to keep up with regular dental check-ups and periodontal examinations. A good home care routine is also vital in preventing gum disease from developing. You know what to do:
- Brush with a soft toothbrush and fluoride toothpaste at least twice a day.
- Replace your toothbrush every three months or when the bristles are worn.
- Floss daily to clean between your teeth and bridgework, crowns, or implants.
- Use an antimicrobial mouthwash.
- Eat a balanced diet.
- Don't smoke! Or stop using tobacco. (We know it isn't easy, but you can do it!)
Whether you call it deep cleaning or scaling and root planing, this procedure will help to keep your teeth and gums healthy and your smile bright and confident. Speak to your dentist or hygienist to see if it’s suitable for you.
This article is intended to promote understanding of and knowledge about general oral health topics. It is not intended to be a substitute for professional advice, diagnosis or treatment. Always seek the advice of your dentist or other qualified healthcare provider with any questions you may have regarding a medical condition or treatment.
ORAL HEALTH QUIZ
What's behind your smile?
Take our Oral Health assessment to get the most from your oral care routine
ORAL HEALTH QUIZ
What's behind your smile?
Take our Oral Health assessment to get the most from your oral care routine