All oral health articles
254 results
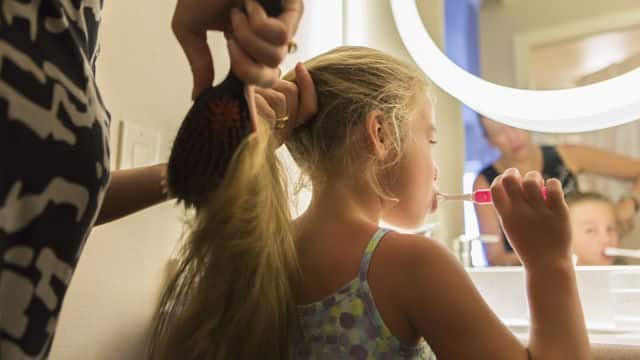

Fluoride
Can Fluoride Help Adults?
The use of fluoride can benefit both children and adults. Research has shown that fluoride applied directly to the teeth is important for fighting decay. Learn more here.
Read More
Fluoride
Stannous Fluoride Toothpaste: Pros, Cons & Alternatives
Stannous fluoride toothpaste is an oral care product that offers powerful benefits when used as part of a good oral hygiene routine. Here's what you need to know about its unique properties.
Read More
Fluoride
What does fluoride do? An overview
If you've ever wondered what fluoride does to improve your oral health and fight cavities, here's what you need to know.
Read More
Fluoride
Who Should Use a Fluoride Mouth Rinse and Why
As an adult, however, there are times when you are at higher risk for tooth decay, and a fluoride rinse may be an appropriate addition to your oral hygiene routine. Learn more here.
Read More
Fluoride
Why Use A Fluoride-Free Toothpaste?
Should you be using a fluoride-free toothpaste? The answer has a lot to do with your age. Learn more about fluoride and whether to use it or not here.
Read More
Fluoride
Fluoride Dangers: How Much Is Too Much?
As the teeth develop, fluoride from water, food or supplements helps build strong tooth enamel, which is better able to resist decay. Learn more about fluoride here and how much is too much.
Read More
Fluoride
Fluoride for Babies: Is It Safe?
By sticking to some simple guidelines and portions, fluoride is safe and recommended for babies and young children. Find out what you need to know here.
Read More
Fluoride
Fluoride FAQs: Your Questions Answered
Find out a list of answers to frequently asked questions about Colgate fluoride products.
Read More
Fluoride
What Is Stannous Fluoride Toothpaste?
Stannous fluoride toothpaste helps prevent cavities, reduce sensitivity, fight plaque, and support daily gum and enamel health.
Read More



Bad Breath (Halitosis)
5 Quick Fixes for Constant Bad Breath
Bad breath is a common problem that can affect your everyday life. Click here to discover 5 quick fixes to cure bad breath.
Read More
Bad Breath (Halitosis)
How to clean your tongue for fresher breath
Brushing twice a day, but until you learn how to clean your tongue, you may not be able to get rid of bad breath. Learn more about how to get a fresh breath.
Read More
Bad Breath (Halitosis)
Treating Bad Breath from Dry Mouth
Some people suffer with bad breath from dry mouth problems, which have little to do with poor hygiene. The good news is, you can take steps to identify and treat the problem, as well as prevent it from recurring.
Read More
Bad Breath (Halitosis)
The Best Mouthwash For Bad Breath: 3 Things To Look For
Mouthwashes fall into one of two categories: therapeutic or cosmetic. Cosmetic mouthwashes are those that mask bad breath, rather than get rid of the cause.
Read More
Bad Breath (Halitosis)
Morning Breath: Prevention & Treatment Tips
The phone alarm sounds each morning waking you from a restful night's slumber. You rub the sleep from your eyes and then you notice it: morning breath.
Read More
Bad Breath (Halitosis)
Bad Breath from Stomach: Causes & Solutions
In fact, bad breath from stomach issues can be even more perplexing than typical bad breath, because it's harder to identify, isolate and treat. Learn more about what's causing your bad breath here.
Read More
Bad Breath (Halitosis)
How To Tell If You Have Bad Breath
Knowing how to tell if you have bad breath can be tricky, because you can't identify it yourself. Nonetheless, there are a few things you can do to improve it if needed.
Read More
Bad Breath (Halitosis)
How to Cure Bad Breath: Effective Tips
Halitosis, more commonly known as bad breath, is an embarrassing hygiene issue that nobody wants to have. Read more at Colgate.com
Read More

Bad Breath (Halitosis)
Tonsil Stones & Bad Breath: Causes
What's the deal with tonsil stones? Bad breath, irritation and a whitish mark at the back of your throat are a few signs that you have a tonsil stone.
Read More



Cavities
What Is A Gumline Cavity?
Did you know that cavities can form in the pits & grooves of the molars, between teeth, or even along the gumline? Learn more about gumline cavities here.
Read More
Cavities
Effects of Sugar on Teeth
Sugar can lead to damage to teeth. Here's how you can prevent tooth decay from hijacking your family's oral health.
Read More


Dry Mouth
Handling a Dry Mouth and Throat
Learn how to effectively handle dry mouth and throat. Explore causes, home remedies, and treatment options for lasting relief.
Read More

Dry Mouth
Dry Mouth Home Remedies
Find effective dry mouth home remedies and natural tips to relieve discomfort. Learn how to manage symptoms and improve oral health.
Read More

Wisdom Teeth
Impacted Tooth: Causes, Symptoms & Treatment
Understand an impacted tooth, including causes, symptoms, and potential complications. Learn when and why treatment might be necessary.
Read More




Wisdom Teeth
Wisdom Teeth Age & Eruption
If you and your teen are maintaining your regular dental appointments, you'll be in good stead to track that the wisdom teeth are erupting healthily or catch if they need intervention.
Read More
Wisdom Teeth
When to consider wisdom teeth removal
Have you ever felt like you were teething as an adult? It was probably in the back of your mouth, and the swelling you felt there was really a tooth trying to erupt.
Read More


Mouth & Teeth Anatomy
Mandibular Tori: Causes & Treatment
Medically Reviewed By Melisa Sahin
Read More
Mouth & Teeth Anatomy
How To Get Rid Of A Dry Throat
Wondering how to get rid of a dry throat? Learn about some of the common causes, including allergies, dehydration, the common cold and more.
Read More






Teeth Whitening
Is Teeth Whitening Safe?
Many people wish their teeth were whiter, but are nervous about bleaching treatment. So, is teeth whitening safe? Yes, save three common side effects.
Read More
Teeth Whitening
Choosing a Teeth Whitening System
Many people want a whiter smile, so how do you choose the best teeth whitening system for you? Find out more about teeth whitening systems here.
Read More


Teeth Whitening
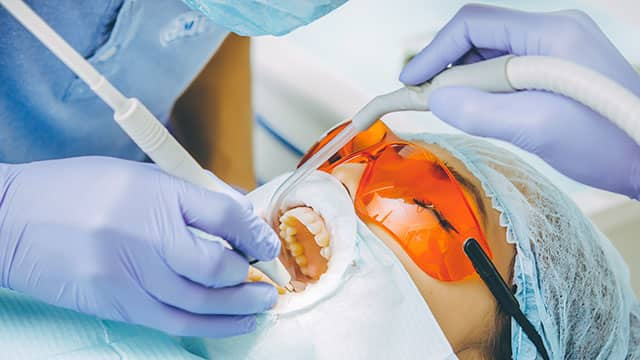
Maintain White Teeth: Your Comprehensive Guide
Whether you already have white teeth or you've just completed a whitening treatment, keep in mind that you've still got some work to do.
Read More
Teeth Whitening
Three tips for preventing stained teeth from braces
Medically Reviewed By Melisa Sahin
Read More
Teeth Whitening
How to Smile in Pictures for a Genuine Result
Saying cheese doesn't always work. Here's how to get a natural smile in pictures so you appear genuine, relaxed and willing show off your white teeth to the best effect.
Read More
Teeth Whitening
How to Get the Perfect Smile
How to have a great smile on camera? Click here to learn the healthiest ways to have a beautiful smile on and off-camera with Colgate.
Read More
Teeth Whitening
Five foods that cause stains and six foods that prevent them
Medically Reviewed By Melisa Sahin
Read More

Teeth Whitening
How to treat burned gums from teeth whitening
If you've been whitening your teeth at home, you could have burned your gums from teeth whitening. Find out more about it here from Colgate®.
Read More
Teeth Whitening
Best Over-the-Counter Teeth Whitening Products
Whether you're on a budget or need results for a big event, here are the best over-the-counter teeth whitening treatments for any lifestyle. Learn more, here.
Read More

Teeth Whitening
Banana peel for teeth whitening: will it whiten stained teeth?
Some claim that banana peel for teeth whitening works, but does the science support it? Learn more about bananas and what you can do for a whiter smile, here.
Read More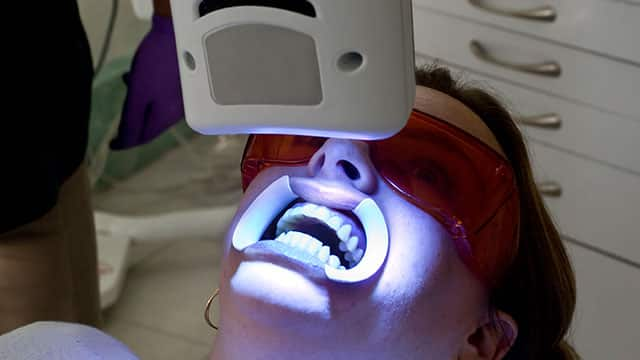
Teeth Whitening
Is UV Teeth Whitening Safe?
Is UV teeth whitening safe and can you do it yourself at home? Find out more about UV teeth whitening, including safety information and alternatives.
Read More

Teeth Whitening
Best Whitening Mouthwash: How to Choose
Medically Reviewed By Melisa Sahin
Read More
Teeth Whitening
How to Avoid Red Wine Teeth This Holiday Season
How do you enjoy your favourite reds this season without the self-consciousness associated with red wine teeth? Here's the scoop on dental discolouration.
Read More
Teeth Whitening
How to Get Whiter Teeth With the Right Foods
If you're wondering how to get whiter teeth, whether or not you also use a whitening product, keep the following foods in mind to help you along the way.
Read More
Teeth Whitening
How to Whiten Teeth with Braces
Knowing how to whiten teeth with braces on isn't impossible, but special care must be taken to ensure treatment is successful. Here are three options.
Read More
Teeth Whitening
How to whiten yellow teeth: 5 top tips
Whether the discolouration is due to staining or other factors, learn how to get rid of yellow teeth through over-the-counter products and professional whitening from the dentist.
Read More
Teeth Whitening
Green Tooth & Other Discoloration Causes
Tooth discolouration like a green tooth can occur under many circumstances. These stains may be extrinsic or intrinsic.
Read More
Teeth Whitening
What is Enamel Microabrasion?
A brighter smile can boost your confidence, consider a professional enamel microabrasion. Click here to learn more about enamel microabrasion with Colgate®
Read More
Teeth Whitening
What Is Oil Pulling? What You Need to Know
Though oil pulling is has been known to enhance mouth health, it's not necessarily the best solution. But first, what is oil pulling? Learn more here.
Read More

Teeth Whitening
Whitening Bonded Teeth: Perfect Your Smile
Medically Reviewed By Melisa Sahin
Read More
Teeth Whitening
What is Teeth Whitening Gel?
Learn about teeth whitening gel, a popular method for achieving a whiter smile. Get tips on how to use it effectively, potential risks and side effects, and how to maintain the results.
Read More
Teeth Whitening
What is a Teeth Whitening Kit?
Looking for a teeth whitening kit and not sure if it's for you? Learn more about how you can easily and quickly achieve a brighter, whiter smile in the comfort of your own home.
Read More
Teeth Whitening
How to Choose the Best Teeth Whitening Kit
Discover the key factors to choosing the best teeth whitening kit for your needs. Get tips on how to find the most suitable kit for your teeth and budget. Plus, find out about any potential risks and side effects to watch out for.
Read More

Teeth Whitening
Can I brush my teeth after using teeth whitening strips?
Find out if it’s safe to brush your teeth after using whitening strips and what experts recommend.
Read More

Teeth Whitening
How long does LED teeth whitening last?
Medically Reviewed By Melisa Sahin
Read More
Teeth Whitening
How to safely use whitening gel at home
With your dentist’s advice and guidance, you can safely and effectively brighten your smile at home with teeth whitening gel. Read more here.
Read More

Teeth Whitening
Laser teeth whitening cost
If you’re thinking about professional dental bleaching, laser teeth whitening might be a good option. Learn about the costs, safety, benefits and drawbacks.
Read More
Teeth Whitening
Whitening strips for sensitive teeth
Discover if whitening strips cause tooth sensitivity and gum irritation, as well as what you can do to alleviate pain.
Read More



Oral Care: Kids (5-12)
How Do I Care for My Toddler's Teeth?
Master toddler oral care. Learn how to clean your toddler's teeth, prevent cavities, and when to schedule dentist visits.
Read More
Oral Care: Kids (5-12)
Oral Health for Children
Teaching your child proper oral care at a young age is an investment in their health that will pay lifelong dividends. Discover teaching methods here.
Read More
Oral Care: Kids (5-12)
Teething Rash: Symptoms And Treatment
Teething can be a painful experience for babies, and one of the most common symptoms is a teething rash. Find out what a teething rash looks like, its causes, and treatment.
Read More
Oral Care: Kids (5-12)
Toddler Tooth Decay And How To Prevent It
Prevent Toddler Tooth Decay: Tips and Tricks for Parents - Keep your toddler's teeth healthy and strong with these helpful tips.
Read More
Oral Care: Kids (5-12)
Best Toothpaste For Kids With Cavities
For kids, tooth decay is a common problem. What is the best toothpaste for kids who have cavities? Find out at Colgate.com.
Read More
Oral Care: Kids (5-12)
Kids Tooth Decay: All Kids Are at Risk
Start taking good care of your little one's teeth early to keep his mouth healthy and prevent kids tooth decay. Read more, here.
Read More


Oral Care: Kids (5-12)
Four Developmental Milestones in Your Child's Oral Health
Different stages of tooth development are milestones in your child's oral care. Learn more from Colgate on kids dental care for a lifetime of healthy smiles.
Read More
Oral Care: Kids (5-12)
Mouth Sores in Children
Mouth sores in children can sometimes appear without explanation. Find out what can cause them, the differences between mouth inflammation, ulcers and more.
Read More
Oral Care: Kids (5-12)
Best Toothpaste For Kids With Cavities
Discover what causes bleeding gums in children and learn how to prevent it happening, along with treatment options.
Read More


Tooth Extraction
Tooth Extraction Healing Time: What's Normal
Sometimes, it's necessary to have a tooth pulled out. Discover our guidelines on the typical tooth extraction healing time and tips for a quick recovery.
Read More
Tooth Extraction
Dry Socket Prevention: Caring For Yourself After An Extraction
Medically Reviewed By Melisa Sahin
Read More

Dental Product Guidance
Choosing the Right Toothbrush
Choosing the right toothbrush is very important. Learn how to choose the right toothbrush, when you should replace your toothbrush and more at Colgate.com
Read More
Dental Product Guidance
Six Natural Ingredients In Fluoride-Free Toothpaste
Fluoride free toothpaste is a great option for those who are sensitive to fluoride. Find more about toothpaste ingredients here.
Read More
Dental Product Guidance
What Products Are Available From My Dentist For Home Tooth Whitening?
Discover products available from your dentist for home tooth whitening. Learn about types, how they work, and their effectiveness.
Read More
Dental Product Guidance
How Does Mouthwash Work?
What type of mouthwash should you choose? How does mouthwash work? This guide will answer those questions and more.
Read More
Dental Product Guidance
Choosing The Best Toothbrush For You
The best toothbrush for the job depends on a variety of things that are unique to you. Here are three things to look for in a product that does this.
Read More
Dental Product Guidance
Antiseptic Vs Antibacterial Mouthwash: What's the Difference?
Mouthwash can freshen your breath and protect against cavities. When it comes to antiseptic vs antibacterial mouthwash, is one better than the other?
Read More
Dental Product Guidance
Using Tartar Control Toothpaste for Healthy Teeth and Gums
Brushing your teeth properly using tartar control toothpaste regularly is an important part of establishing and maintaining good oral health.
Read More


Mouth Sores and Infections
Sore in Roof of Mouth: Causes & Solutions
Medically Reviewed By Lone Lenes
Read More

Mouth Sores and Infections
White Spot on Tongue: Causes & Treatment
Medically Reviewed By Lone Lenes
Read More




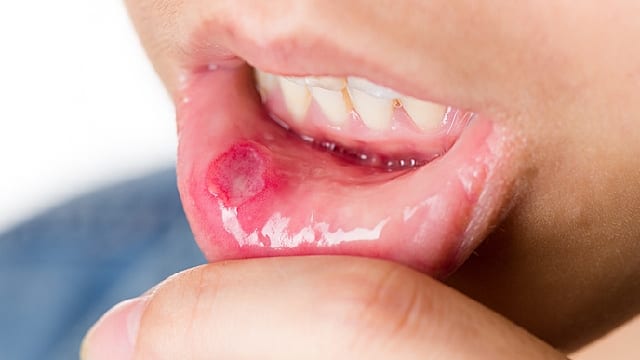
Mouth Sores and Infections
Eight Common Oral Infections
Medically Reviewed By Melisa Sahin
Read More






Mouth Sores and Infections
Toothpaste on Cold Sore: Does it Work?
Medically Reviewed By Melisa Sahin
Read More
Mouth Sores and Infections
Angular Cheilitis: Symptoms, Risks & Treatment
Medically Reviewed By Lone Lenes
Read More




Mouth Sores and Infections
How To Get Rid Of A Cold Sore Fast
These sores are common and will go away on their own, but if you have a major event coming up, you might be wondering how to get rid of a cold sore fast.
Read More
Mouth Sores and Infections
Managing Blood Blisters in the Mouth
If you've ever had the displeasure of accidentally biting your cheek while chewing food, you might recall a sore forming in the area. While mouth sores caused by cheek biting are usually no cause for concern, what if you notice a sore in the mouth that's filled with blood? Finding a blood blister in the mouth may be worrying, but rest assured that these blisters are generally harmless and may heal on their own.
Read More
Mouth Sores and Infections
How to Prevent a Cold Sore Scab
If you suffer from cold sores, you know that the accompanying redness and blisters can make you feel self-conscious. But when those blisters become scabs and possibly scars, what should be a fairly short-term issue can have long-term repercussions. Cold sore scabs can be the result of picking and irritation, so make sure that you properly care for and prevent cold sores to stop them from becoming worse over time. By educating yourself on what can cause a cold sore scab and result in scarring, you can heal faster so cold sores don't become a permanent problem.
Read More

Dental Health Threats
VANITY New Research For Toothpaste And Mouthwash Effects on Covid-19 Virus
Can toothpaste and mouthwash neutralize and reduce the virus that can cause COVID-19 in your mouth? Read more on this new Colgate-Palmolive research for toothpaste and mouthwash effects on the COVID-19 virus.
Read More
Dental Health Threats
What is sodium lauryl sulphate and is It safe?
Discover what sodium lauryl sulphate is and find out if it is safe to use. Learn more about the dental products that contain it.
Read More
Dental Visits
Finding a Dentist
Learn effective ways to find a dentist that suits your needs, including seeking referrals and understanding different dental specialities.
Read More

Dental Visits
How Often Should You Go to the Dentist?
While it’s true that a twice-yearly cleaning schedule is a good rule of thumb for many people, scheduling dentist appointments should be based on each person’s oral hygiene, habits and medical conditions.
Read More
Dental Visits
Dentist Requirements: What It Takes To Become A Dentist
Dentist requirements extend beyond additional education, though. Your dentist needed to pass a number of tests and more. Find out additional information here.
Read More
Veneers
How Do Veneers Work?
How do veneers work? Get the facts. Learn about the procedure, benefits, and aftercare.
Read More

Veneers
How Long Do Veneers Last?
How long do veneers last? The answer depends heavily upon how you care for them. Learn how to care for them and more, here.
Read More
Veneers
How Porcelain Dental Veneers Can Rebuild Your Smile
How do porcelain dental veneers work? Get the facts. Learn about the procedure, benefits, and aftercare.
Read More
Veneers
What are Veneers and How Should You Care for Them?
Porcelain veneers can give you a beautiful, healthy smile. Learn how to care for them and keep them looking great.
Read More



Dental Emergencies & Sports Safety
I Bit My Tongue: What Now?
Medically Reviewed By Melisa Sahin
Read More
Dental Emergencies & Sports Safety
Fixing a Chipped Tooth Fast
Fixing a chipped tooth as soon as it happens ensures your mishap doesn't cause further problems, but what are your options? Find out more, here.
Read More
Oral Care: Adults (18+)
How do I Care for my Teeth as an Adult?
Learn how to care for your teeth as an adult. Discover common dental issues and preventive measures.
Read More
Oral Care: Adults (18+)
What is Good Oral Hygiene?
Good oral hygiene is essential for a healthy smile. Learn what it involves and how to practice it daily.
Read More
Oral Care: Adults (18+)
The Dangers Of Using A Plaque Scraper At Home
Learn the dangers of using a plaque scraper at home and opt for professional dental cleanings. Maintain a healthy smile with Colgate.
Read More
Oral Care: Adults (18+)
Sinus Infection Tooth Pain Relief
Experiencing tooth pain from a sinus infection? Learn about the causes of sinus-related toothache and effective relief strategies.
Read More
Oral Care: Adults (18+)
What Causes a Swollen Gum Around One Tooth?
Medically Reviewed By Melisa Sahin
Read More
Oral Care: Adults (18+)
Coated Tongue: What a White Tongue Means and How to Treat It
Medically Reviewed By Lone Lenes
Read More
Oral Care: Adults (18+)
Excessive Saliva: Ptyalism causes and treatment
Discover the causes of excessive saliva and how to manage it effectively. Improve your oral health with our expert tips and advice.
Read More
Oral Care: Adults (18+)
Blisters in Mouth Tissue and Treatment
Understand blisters in mouth tissue. Learn about causes, symptoms, and available treatments.
Read More
Oral Care: Adults (18+)
Can Tooth Enamel Be Restored?
Can weakened tooth enamel be repaired? It depends on the state it's in. Keeping tooth enamel healthy is most effective when done through prevention. Here's how.
Read More
Oral Care: Adults (18+)
Bumps On The Back Of The Tongue: Normal Or Abnormal?
Bumps on the back of the tongue can occur due to sores and infections among other conditions. Learn more about it and when to consult your dentist in case of abnormal bumps.
Read More
Oral Care: Adults (18+)
Dental Erosion: What Food and Drinks Can Impact the Teeth?
Find out which food and drinks are at high risk of causing dental erosion and how you can prevent enamel erosion.
Read More
Oral Care: Adults (18+)
Enamel erosion: causes, prevention and treatment
Enamel erosion is a common dental problem. Learn about the causes, symptoms and treatments for enamel erosion.
Read More
Oral Care: Adults (18+)
How do enamel toothpastes work?
For decades, dental hygiene products containing fluoride, such as toothpaste, have been “repairing tooth enamel”. Discover how they work.
Read More
Oral Care: Adults (18+)
Regular Physical Activity and Dental Erosion
Discover the link between regular physical activity and dental erosion. Find out why many athletes have dental problems.
Read More


Implants
Bone Grafts for Dental Implants: Your Guide to the Procedure
Explore bone grafting for dental implants. Understand the procedure, its necessity, and if it's right for your tooth replacement journey.
Read More
Pregnancy Oral Care
Oral Health Through Pregnancy
Oral health through pregnancy is crucial for both mom and baby. Get tips on how to maintain good oral hygiene during this time.
Read More
Pregnancy Oral Care
Sensitive Teeth During Pregnancy: What to Expect and How to Cope
Medically Reviewed By Melisa Sahin
Read More
Root Canals
What can you do with the severe pain after root canal?
If you have severe pain after root canal treatment, learn more about what may be the cause and when you should consult a dentist.
Read More
Plaque & Tartar
Tips for Removing Plaque
Learn what plaque and tartar are, what causes their build-up, their effects on oral health and effective removal strategies.
Read More
Plaque & Tartar
How To Prevent Tartar Build-up On Teeth
Tartar build-up on teeth can often be prevented by regular brushing, but you'll need the help of your dentist to remove it if it decides to stick around.
Read More
Plaque & Tartar
Bleeding Gums When Flossing: Should You Call Your Dentist?
Combat bleeding gums when flossing. Learn about causes, prevention strategies, and treatments.
Read More
Jaw Pain (TMD)
Dislocation of the Temporomandibular Joint (TMJ)
Understand dislocation of the Temporomandibular Joint (TMJ). Learn about its causes, symptoms, and treatment options.
Read More
Jaw Pain (TMD)
When a Clicking Jaw Is a Sign of TMD
When is a clicking jaw a sign of TMD? Get the facts. Learn about symptoms, causes, and treatments.
Read More
Jaw Pain (TMD)
What's Causing Your Facial And Jaw Pain?
Discover the causes of facial and jaw pain, including TMJ. Learn about symptoms, treatments and prevention strategies to improve your oral health.
Read More
Jaw Pain (TMD)
What is the TMJ?
What is TMJ? Learn about this disorder that affects the jaw joint and how to manage it.
Read More
Jaw Pain (TMD)
Three Ways A TMJ Massage Can Relieve Jaw Pain
A TMJ disorder is usually the result of inflamed and painful chewing muscles around your jaw. Luckily, a TMJ massage can act as an effective, non-medicinal solution.
Read More
Digestive (Gastrointestinal) Disorders
Natural Mouth Ulcer Remedies
Discover natural ways to get rid of mouth ulcers and maintain oral health. Learn more about causes, prevention, and treatment today!
Read More
Bridges & Crowns
What are Dental Crowns and Tooth Bridges?
Discover what dental crowns and tooth bridges are. Learn about their uses, the procedure, and aftercare.
Read More
Bridges & Crowns
Different Types Of Dental Crowns
There are different types of dental crowns. Understand each type and choose the one that suits your needs.
Read More
Bridges & Crowns
Your Dental Crown Procedure: What To Expect
Your dentist may recommend that you undergo a dental crown procedure for one of several reasons:… Read more at Colgate.com
Read More
Fillings
Fillings: the Basics
Fillings are common in dental care. Understand the basics of fillings and what to expect during the procedure.
Read More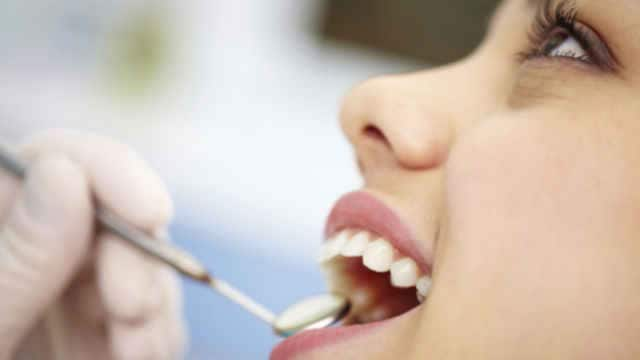
Fillings
What is a Filling? Understanding Dental Fillings
What is a filling? Understand why fillings are needed, the procedure, and different types of filling materials.
Read More
Fillings
Tooth Pain After Filling: Is It Normal?
Learn if tooth pain after a filling is normal and when to seek dental care. Ensure proper oral care by understanding post-filling symptoms.
Read More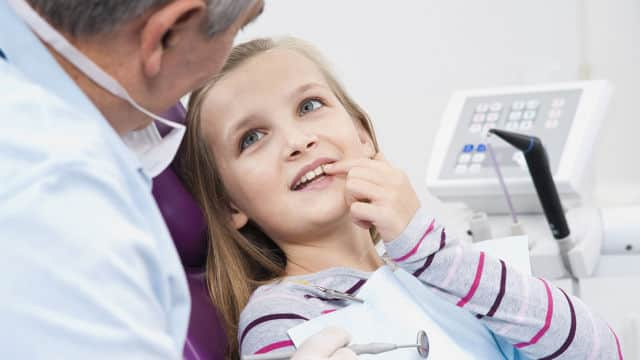

Fillings
Dental Amalgam: A Health Risk?
Understand the safety and potential health risks of dental amalgam. Make informed decisions about your dental fillings with Colgate.
Read More


Fillings
What is tooth decay? Commonly known as ‘a hole in the tooth’
If you have a hole in your tooth caused by tooth decay, you’ll want to know what to do. Read our guide to learn more about holes in your teeth.
Read More



Dentures
What Are Flexible Dentures?
Discover what flexible dentures are, their advantages in comfort and durability, and important care tips for maintaining this type of dental appliance.
Read More

Nutrition & Oral Health
What Are the Best Foods for Gum Health?
Many people have heard that milk is good for their bones and carrots are good for their eyes. But what are the best foods for healthy gums? Learn more.
Read More
Nutrition & Oral Health
How can a vegan diet affect your teeth?
Find out how being vegan can affect your teeth and how to protect them if you follow a vegan diet.
Read More
Nutrition & Oral Health
The impact of oral health on sports performance
Learn how oral health influences sports performance and overall wellbeing. Boost your game with Colgate and discover tips for achieving a healthier smile.
Read More
Brushing & Flossing
Family Guide To Oral Health
Follow our family guide to oral health. Learn about common dental issues and preventive measures for the whole family.
Read More
Brushing & Flossing
How To Brush
How to Brush Your Teeth: A Step-by-Step Guide - Get expert tips on how to brush your teeth properly for optimal oral health.
Read More

Brushing & Flossing
Is Brushing Teeth After Eating Good For You?
Learn about tongue ulcers, including their types, causes, symptoms, treatment, and whether they are contagious.
Read More
Brushing & Flossing
Why is dental flossing good for gums?
Daily flossing helps to prevent gingivitis by removing plaque and food debris, keeping your teeth and gums healthy. Learn more.
Read More
Gum Disease (Gingivitis)
What Is Gingivitis? Signs And Symptoms
People with gingivitis have inflamed gum tissue around their teeth. This condition is caused by bacteria found in dental plaque.
Read More

Gum Disease (Gingivitis)
Five Things You Can Do If Your Gums Are Bleeding
You're brushing your teeth and notice a bit of pink when you spit out the toothpaste. You might notice some bleeding when you floss.
Read More
Gum Disease (Gingivitis)
Can Receding Gums Grow Back?
If you think your teeth look longer than they did before, it could be because of your gums. Gum recession happens for many reasons, from brushing your teeth with too much pressure to grinding your teeth.
Read More
Gum Disease (Gingivitis)
What to Do About Gum Swelling
Swollen gums are a common problem and can have many different causes. If you are suffering from gum swelling that lasts longer than a few days, you should contact your dental professional.
Read More
Gum Disease (Gingivitis)
Receding Gums And Treatment And Causes
It can be scary and painful to have receding gums, but you don't need to worry. There are several steps you can take at home that may serve as effective treatment for receding gums, depending on the severity of the problem.
Read More
Gum Disease (Gingivitis)
Four Signs of Healthy Interdental Papilla
Identify the four key signs of healthy interdental papilla (gums between teeth) and learn how to maintain their health for overall oral well-being.
Read More
Gum Disease (Gingivitis)
Chlorhexidine Gluconate Oral Rinse: What Is It?
Discover what chlorhexidine gluconate mouthwash is, how it treats gingivitis, its benefits for gum health, and important usage information.
Read More
Gum Disease (Gingivitis)
Bleeding Gums Treatment and Home Remedies
You brush your teeth. You floss or clean in between them. Then, you notice your gums are bleeding a little. You may think this isn’t a big deal (and maybe it’s not), but you should have your dental professional check it out.
Read More
Gum Disease (Gingivitis)
Gum Disease 101
Gum disease is an inflammation of the gums that can progress to affect the bone that supports your teeth. Find out the causes of gum disease and how to prevent it.
Read More
Gum Disease (Gingivitis)
Sore Gums Causes and Treatments
Worried about bleeding or sore gums? Find out what may be causing them and what you can do to prevent gum pain and damage. Learn more.
Read More
Gum Disease (Gingivitis)
Gum Irritation Four Self-Induced Causes
Gum irritation has many possible causes, but some of them come from a personal habit you may not be paying attention to. Here are a few you should know.
Read More
Gum Disease (Gingivitis)
Gum inflammation: causes, treatment and prevention
Find out what causes gum inflammation and how you can treat it for good oral health.
Read More
Gum Disease (Gingivitis)
How to strengthen gums?
Good oral hygiene and regular rinsing with a mouthwash is an excellent way to strengthen gums. Find out how to improve and maintain healthy gums.
Read More

Tooth Sensitivity
Causes and Treatments of Extremely Sensitive Teeth
Medically Reviewed By Melisa Sahin
Read More

Tooth Sensitivity
Three Surprising Causes of Sensitive Gums
Medically Reviewed By Melisa Sahin
Read More



Tooth Sensitivity
How Does Mouthwash for Sensitive Teeth Work?
Medically Reviewed By Melisa Sahin
Read More
Tooth Sensitivity
What to Use for Sensitive Teeth in Children
Medically Reviewed By Melisa Sahin
Read More
Tooth Sensitivity
Is One Sensitive Tooth a Serious Issue?
Is one sensitive tooth a serious issue? Understand the potential causes of isolated tooth sensitivity and when to consult your dentist for advice.
Read More
Tooth Sensitivity
Tooth Sensitive to Hot or Cold: What it Means
Is your tooth sensitive to hot or cold? Discover what it means, its causes, and how to effectively help alleviate this common dental sensitivity.
Read More


Tooth Sensitivity
Understanding tooth sensitivity and its causes
It is estimated that one in eight people in the United Kingdom experience tooth sensitivity. So what causes sensitive teeth? Any number of dental problems. Find your answers here.
Read More
Tooth Sensitivity
How Tooth Nerve Pain Occurs
Here are some foods and drinks to avoid when suffering from tooth pain, and some insight into how the nerve becomes exposed in the first place.
Read More
Tooth Sensitivity
Treat Super Sensitive Teeth with Sensitive Toothpaste
Sensitivity in the teeth can be uncomfortable and inconvenient. Fortunately, sensitive toothpaste can often be the answer to your pain by Colgate.
Read More

Tooth Sensitivity
Sensitive teeth after cleaning
If you experience sensitive teeth after a cleaning or root planing treatment, and it continues longer than a week, read the following help and advice.
Read More
Teeth Bonding
Improving My Smile (Tooth Whitening and Tooth Bonding)
Improve your smile with bonding and whitening options. Get tips on how to achieve a brighter, more confident smile.
Read More
Receding Gums
Preventing Further Gum Recession
Prevent further gum recession effectively. Understand causes, symptoms, and treatment options for receding gums.
Read More
Tooth Fairy
Tooth Fairy Letters: Answer Kids' Questions
Tooth fairy letters can answer kidss; questions. Discover how to make this tradition educational and fun.
Read More
Oral Care: Babies (0-4)
Early Childhood Cavities
Early childhood cavities can be a serious issue. Learn about causes, prevention, and treatment options to protect your child's oral health.
Read More
Oral Care: Babies (0-4)
Baby Teething Timeline
Understand baby teething timeline. Learn about the process, symptoms, and how to soothe your baby.
Read More
Oral Care: Babies (0-4)
Permanent Teeth Chart to Track Your Child's New Teeth
Track your child's new teeth with our permanent teeth chart for parents. Keep track of their dental development easily.
Read More
Oral Care: Babies (0-4)
Oral Thrush in Babies: Causes, Symptoms and Treatment
Understand oral thrush in babies. Learn about causes, symptoms, and effective treatments.
Read More
Oral Care: Babies (0-4)
The Importance of Pediatric Dental Care
Pediatric dental care is crucial for your child's oral health. Understand its importance and how to ensure proper care.
Read More
Oral Care: Babies (0-4)
Your Baby's First Tooth: What To Expect
Do you see a white bud that could be your baby's first tooth? Between four and six months of age, your little angel will begin teething.
Read MoreOral Health Quiz
What's behind your smile?
Take our Oral Health assessment to get the most from your oral care routine.
Oral Health Quiz
What's behind your smile?
Take our Oral Health assessment to get the most from your oral care routine.




