All oral health articles
793 results





















Bad Breath
What To Do About Chronic Bad Breath?
If you have chronic bad breath, then you know how embarrassing this problem can be. Instead of temporarily masking odour with breath mints, gum, and...
Read More
Bad Breath
5 Foods That Zap Bad Breath Fast
Are you suffering from bad breath? If you are, here are 5 natural bad breath remedies to brighten your day.
Read More
Bad Breath
The Best Mouthwash For Bad Breath: 3 Things To Look For
Mouthwashes fall into one of two categories: therapeutic or cosmetic. Cosmetic mouthwashes are those that mask bad breath, rather than cure it.
Read More
Bad Breath
Trimethylaminuria And The Fishy Odour
Bad breath may be caused by a genetic condition known as trimethylaminuria. Find out more about the causes of trimethylaminuria, treatment, and more.
Read More
Bad Breath
Using a Halimeter: How Bad Is Your Breath, Really?
Let's face it: Bad breath, or what your dentist calls halitosis, stinks. Here's how a device called the Halimeter works to measure your breath odour.
Read More



















Bad Breath
What Causes Bad Breath?
Uncover the reasons behind bad breath and learn effective solutions for fresher breath and improved oral health. Learn more!
Read More



Bad Breath
Effective Tips for Bad Breath Treatment
Struggling with bad breath? Check out our top tips and treatments to achieve lasting fresh breath from lifestyle changes to dental advice. Learn more!
Read More







Bad Breath
3 Foods That Cause Bad Breath and Tips to Fight It
There are many ways to combat it and still enjoy the foods you love. Here are some foods that cause bad breath, and how to control or prevent them from affecting your oral hygiene.
Read More
Bad Breath
How To Get Rid Of Garlic Breath
Fortunately, there are many things you can do to quickly get your breath under control. Here's how to get rid of garlic breath before an important event.
Read More
Bad Breath
How To Tell If You Have Bad Breath
Knowing how to tell if you have bad breath can be tricky, because you can't identify it yourself. Nonetheless, there are a few things you can do to improve it if needed.
Read More
Bad Breath
How To Prevent Bad Breath If You're An Older Adult
Bad breath can be a problem for anyone. However, older adults are more prone to bad breath due to a number of dental conditions. Find out more, here.
Read More
Bad Breath
How To Manage Alcohol Breath
Drinking too much alcohol is bad news for your body and also for your breath. Find out how you can manage and get rid of alcohol breath, here.
Read More
Bad Breath
Why should you use a tongue cleaner?
In addition to using a toothbrush to clean your teeth, you can improve your mouth's freshness by using a tongue cleaner.
Read More
Bad Breath
How to Clean Your Tongue & Avoid Bad Breath | Colgate IN
Cleaning your tongue can leave you feeling refreshed. Learn how cleaning your tongue can improve your breath and discover simple tongue cleaning techniques.
Read More
Bad Breath
Ammonia Breath And Associated Health Concerns
Bad breath may stem from factors you can control. Ammonia breath, however, may be a sign of a serious health condition. Learn more, here.
Read More
Bad Breath
What To Do About Mothball Breath
Bacteria and food particles in the mouth and throat cause many cases of bad breath, and eating odorous food is another common cause.
Read More
Bad Breath
Hormones and Bad Breath: What's the Connection?
Women are especially prone to this hormones bad breath connection, and it could be cause for a visit to both the doctor and the dentist. Learn more, here.
Read More
Bad Breath
What is Perio Breath? - Gum Disease & Bad Breath
Some problems with your gums may contribute to bad odors in your mouth. Visit Colgate now and learn how gum disease and bad breath are connected.
Read MoreBad Breath
How Gargling Can Help You
Learn from video and guide from dental experts on the topics of: how gargling can help you.
Read MoreBad Breath
The Numbers Behind Good Oral Care
Ready for some stats that will knock your socks off? Let’s just hope they don’t knock your teeth out…
Read MoreBad Breath
Travel DO's For Your Mouth
Learn from video and guide from dental experts on the topics of: travel do's for your mouth
Read More












Mouth & Teeth Anatomy
Bone Resorption: Why It Happens And What To Do Next
Bone resorption is part of a complex biological process that can result in shrinkage or loss of bone. Here's how it may affect your mouth.
Read More
Mouth & Teeth Anatomy
Do You Know All The Human Teeth Names?
Get a better understanding of the human teeth names, each tooth's location in the mouth and how you use them in daily functions.
Read More
Mouth & Teeth Anatomy
How To Get Rid Of A Dry Throat
Wondering how to get rid of a dry throat? Learn about some of the common causes, including allergies, dehydration, the common cold and more.
Read More





Fluoride
Who Should Use a Fluoride Mouth Rinse and Why?
As an adult, there are times when you are at higher risk for tooth decay, and a fluoride rinse may be an appropriate addition to your oral hygiene routine. Learn more here.
Read More
Fluoride
Can Fluoride Help Adults?
The use of fluoride can benefit both children and adults. Research has shown that fluoride applied directly to the teeth is important for fighting decay. Learn more here.
Read More
Fluoride
The Facts About Fluoride
While tap water is your first line of defense, if your tap water doesn't have added fluoride, talk to your dentist to find out how you'd benefit from other sources.
Read More
Fluoride
Stannous Fluoride Toothpaste: Pros, Cons and Alternatives
Stannous fluoride toothpaste is an oral care product that offers powerful benefits when used as part of a good oral hygiene routine. Here's what you need to know about its unique properties.
Read More
Fluoride
The Facts About Fluoride
While tap water is your first line of defense, if your tap water doesn't have added fluoride, talk to your dentist to find out how you'd benefit from other sources.
Read More
Fluoride
What Does Fluoride Do to Protect Your Smile?
If you've ever wondered what fluoride does to improve your oral health, here's what you need to know.
Read More
Fluoride
Why Use a Fluoride-Free Toothpaste?
Should you be using a fluoride-free toothpaste? The answer has a lot to do with your age. Learn more about fluoride and whether to use it or not here.
Read More
Fluoride
Fluoride Dangers: How Much Is Too Much?
As the teeth develop, fluoride from water, food or supplements helps build strong tooth enamel, which is better able to resist decay. Learn more about fluoride here and how much is too much.
Read More
Fluoride
Fluoride for Babies: Is It Safe?
It's critical that parents understand the benefits of fluoride and how fluoride for babies can ensure your child has a healthy smile.
Read More
Fluoride
Fluoride FAQs
Find out a list of answers to frequently asked questions about Colgate fluoride products.
Read More
Fluoride
Fluoride Deficiency & Signs
Fluoride is a powerful tool in oral health. You could be suffering from a fluoride deficiency. Visit Colgate now and learn the signs of fluoride deficiency.
Read More
Fluoride
Fluoride Treatments In The Dental Office
Fluoride treatments are especially good for people with a higher risk for tooth decay. Visit Colgate now and learn about how these treatments can benefit you.
Read More
Fluoride
Why Look For Fluoride In Toothpaste?
Medically Reviewed By Colgate Global Scientific Communications
Read More










Cavities
Dental Caries (Cavities): How They Are Formed and What You Can Do to Prevent Them
Read More
Cavities
Enamel Decay: How It Starts And How To Stop It
When lactic acid attacks the minerals in your enamel, it turns white – but unfortunately not the white you want. This is the first sign of enamel decay.
Read More
Cavities
Can You Remineralise Teeth?
Advertisements have flooded the dental market recently with products that claim to remineralise teeth. But are these items effective? Get your answers here!
Read More
Cavities
Cavity Prevention
Pit and fissure cavity prevention can start right at home. Make sure to brush your teeth twice a day for at least two minutes each session.
Read More
Cavities
Preventing Tooth Decay Disease
The main culprit in tooth decay disease is acid formed by sugars in our foods. When food is frequently left on your teeth, bacteria that lives in the mouth wi...
Read More
Cavities
Rampant Caries: What Are They?
Anyone of any age is susceptible to rampant caries, but luckily there are treatments that can restore your oral health. Find out more about rampart caries.
Read More
Cavities
What Are Incipient Caries?
Incipient caries are the beginning stages of a cavity. Find out more about incipient caries and how you can stop them in their tracks and avoid the drill.
Read More
Cavities
Five Ways To Reverse Tooth Decay
If your dentist has told you that you have cavities, it's time to start thinking about ways to reverse tooth decay.
Read More
Cavities
What Are Sugar Drinks Doing To Your Teeth?
When it comes to keeping your family's teeth healthy, it's important to ensure they brush and floss, but it's just as important… Read more at Colgate.com
Read More
Cavities
What Are The Classes Of Cavities?
In fact, there are six classes of cavities based on the tooth type and the location of the decay, as well as four classifications that describe the severity of decay.
Read More
Cavities
What Are The Effects Of Sugar On Teeth?
It's not the sugar itself that does the damage, but rather the chain of events that takes place after. Here's how you can prevent tooth decay from hijacking your family's oral health.
Read More
Cavities
Your Guide To Tooth Decay Stages
Decay worsens over time, and more advanced tooth decay stages require more extensive treatments. If caught early on, you can stop decay in its tracks.
Read More
Cavities
What Does A Cavity Feel Like?
Your teeth might feel sensitive and you might feel some pain, especially after eating sweets, hot foods or cold foods. Learn more here.
Read More
Cavities
Watch Out for These Signs of a Cavity
You bite down and feel a slight twinge in your mouth. Learn all the signs and symptoms of a cavity and why maintaining dental appointments is essential.
Read More
Cavities
Antibiotics for Tooth Infections & Tooth Pain
It's important to get treatment for tooth pain. In some cases, you may need antibiotics for a toothache. Here's what to know before seeing your dentist.
Read More
Cavities
What Is a Smooth Surface Cavity?
A smooth surface cavity is a type of cavity that appears on the sides of the teeth. Here's what you should know about this type of dental decay.
Read More
Cavities
Toothache Home Remedies
If a toothache strikes when you can't see your dentist, consider trying one of these toothache home remedies for temporary relief. Learn more, here.
Read More
Cavities
How to Relieve Cavity Pain: Home remedies to Soothe Your Toothache
Medically Reviewed By Colgate Global Scientific Communications
Read More

Cavities
How To Get Rid Of Cavities
Can you get rid of cavities in two days? No, that isn't true. Cavities can only be repaired by a dental professional. Learn more at Colgate IN now.
Read More
Cavities
What Is A Gumline Cavity?
Did you know that cavities can form in the pits & grooves of the molars, between teeth, or even along the gumline. Learn more about gumline cavities here.
Read More
Cavities
What Is a Root Cavity and How Can You Prevent It? | Colgate® Oral Care
A root cavity occurs on the root of your tooth rather than the enamel. Learn more about how to prevent and treat this type of cavity.
Read MoreCavities
Cavities
Whilst medicines may put the smile back on your dial if you’re ill, you may end up frowning from some antibiotics that can stain your teeth.
Read More








Dry Mouth
Causes Of Dry Mouth And The Problems It Can Create
There are many causes of dry mouth, not to mention a number of related dental problems that it can lead to.
Read More
Dry Mouth
Dry Mouth And Diabetes: Four Tips For Prevention
Dry mouth and diabetes often go hand in hand, but here are four tips for managing the problem.
Read More
Dry Mouth
Dry Mouth At Night: The Causes And Management Tips
Have you ever woken up from a sound sleep with a dry mouth at night? Dry mouth, or xerostomia, can be caused by a variety of conditions and habits.
Read More
Dry Mouth
10 Home Remedies For Dry Mouth
Dry mouth can develop for many reasons: medications, nutritional deficiencies, stress, cancer treatment, and even some systemic diseases. Learn how to help dry mouth here.
Read More
Dry Mouth
Dry Toothpaste 101: What Is It And How Does It Work?
Dry mouth toothpaste can stave off discomfort and potential health issues. Find out if dry mouth toothpaste can be the remedy for your dry mouth.
Read More
Dry Mouth
Dry Mouth At Night? Why You Shouldn't Ignore The Symptoms
Dry mouth at night might seem like a harmless nuisance, but it could indicate deeper problems with your oral health. Learn more with Colgate.
Read More
Dry Mouth
Essential Oils For Dry Mouth: Will They Help?
People turn to natural remedies for a whole host of mild conditions, but do essential oils for dry mouth work? Find out more keeping a hydrated mouth here.
Read More
Dry Mouth
How Do Dry Mouth Lozenges Work?
Saliva plays an important role in keeping your mouth healthy. If you have dry mouth, dry mouth lozenges may help stimulate your saliva production.
Read More
Dry Mouth
What Is Saliva And Why Is It Important?
What is saliva? You might be surprised to know that it contains much more than just water and serves a host of functions for your health! Learn more.
Read More.jpg)
Dry Mouth
Dry Mouth After Drinking Alcohol
If you've ever indulged in alcohol beverages, you've experienced dry mouth after drinking. Here's what that condition does to your oral health. Learn more.
Read More
Dry Mouth
Foamy Saliva: What Does It Mean
What causes foamy saliva and what may it indicate about your overall health? Visit Colgate India now and learn how you can prevent it.
Read More
Dry Mouth
How To Treat Dry Mouth
Deciding how to treat dry mouth often depends upon its root cause. There are multiple causes and various methods of treatment. Learn more now at Colgate.
Read More
Dry Mouth
What Can You Do About Chronic Dry Lips?
Knowing what's causing your persistently chapped lips is the first step to understanding what you can do to treat and soothe them. Learn more now at Colgate.
Read More



.jpg)



Bruxism
Do I Need a Night Guard for Teeth Clenching
Clenching your teeth while you're asleep is pretty common. Visit Colgate now and learn more about sleep bruxism and night guards to protect your teeth.
Read More





Brushing & Flossing
Travel Toothpaste Holder? How To Protect Your Oral Care Supplies On The Go
Read More



Brushing & Flossing
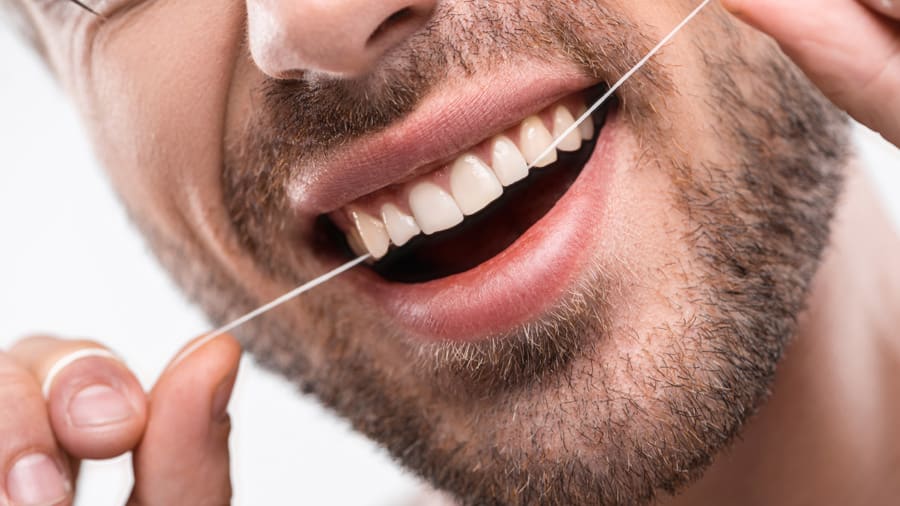
Over Brushing Teeth: Too Much of a Good Thing
If frequent brushing is a good thing, then how can over brushing teeth be risky? Visit Colgate India now and learn more about over brushing teeth.
Read More





Brushing & Flossing
Bleeding Gums When Flossing: Should You Call Your Dentist?
If you notice bleeding gums when flossing, then should you call your dentist? Gums that bleed after daily flossing can be a warning sign of gingivitis,...
Read More
Brushing & Flossing
Dental Floss: Make The Most Of Your Flossing Session
Find out everything you wanted to know about dental floss, including the benefits of flossing, the proper technique, choosing a floss, and more.
Read More
Brushing & Flossing
3 Tooth Brushing Techniques That Get The Job Done
The key to preventing and controlling gum disease is brushing around and under the gumline where bacteria and plaque tend to accumulate. Learn more here.
Read More
Brushing & Flossing
Myth Busting: Is Nap Breath A Thing?
Similar to morning breath, sometimes you can get bad breath after napping. Find out what causes nap breath and how you can manage and prevent nap breath.
Read More
Brushing & Flossing
Help! My Child Wants To Eat Toothpaste!
For some children, brushing their teeth can be more than a good hygiene practice, it can be an opportunity to snack on some… Read more at Colgate.com
Read More
Brushing & Flossing
Is Brushing Teeth After Eating Good For You?
Certain foods and drinks - especially those high in carbohydrates and sugars - spur the creation of certain bacteria in your… Read more at Colgate.com
Read More
Brushing & Flossing
What happens if you don’t brush your teeth at night?
You've probably heard this several times that brushing your teeth two times (morning & night) daily is essential. After a while, you might take this sound advice for granted. Here's a 'brush up' on what happens when you don't brush your teeth at night, and why committing to good oral care benefits your health — and your wallet.
Read More
Brushing & Flossing
Why brush your teeth twice a day?
Discover why brushing your teeth twice a day is necessary and how it reduces the risk of cavities by 50% and contributes to a healthier mouth.
Read More
Brushing & Flossing
Unlocking 3 benefits of brushing teeth at night
Do not skip night brushing! Learn about the benefits of brushing teeth at night and improving your technique to maintain good oral health while you sleep.
Read More
Brushing & Flossing
When to Start Using Toothpaste for Your Baby
When should you start brushing my baby's teeth with toothpaste? Visit Colgate now and learn about the steps for keeping your baby's teeth in perfect condition.
Read More







.jpg)








Nutrition & Oral Health
Foods That Prevent Tooth Decay
Sugary treats, sticky snacks and syrup-laden sodas are bad news for your teeth, of course, but did you know there are some foods that prevent tooth decay?
Read More
Nutrition & Oral Health
Is Milk Good For Your Teeth?
Dairy products keep your teeth as healthy as your bones throughout your life. So, is milk good for your teeth? The answer is a resounding yes, and here's why.
Read More
Nutrition & Oral Health
Tea Tree Oil & Your Teeth
Tea tree oil has become a very popular natural remedy for oral health. Learn more about the benefits and how to properly use it.
Read More















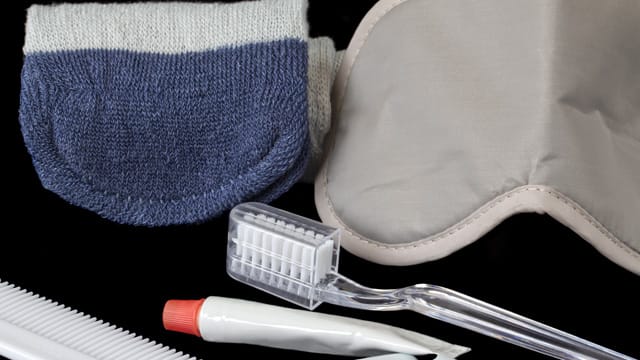
Selecting Dental Products
Is A Disposable Toothbrush With Toothpaste A Good Travel Choice?
Read More




Selecting Dental Products
Personalised Toothbrushes: Fun For Kids And Sanity-Saving For Parents
Read More












Selecting Dental Products
Guidelines on Brushing: What Toothpaste Is the Best for Your Babies & Kids?
Read More
Selecting Dental Products
Is Baking Soda Mouthrinse Safe And Effective?
While there are many mouthwashes on the market today, would a baking soda mouthrinse be safe and effective for daily use?
Read More
Selecting Dental Products
How Does Mouthwash Work?
What type of mouthwash should you choose? How does mouthwash work? This guide will answer those questions and more.
Read More
Selecting Dental Products
Mouth Guards: Everything You Need To Know
Dentists might recommend mouth guards for their patients who grind their teeth at night, play contact sports, or have TMJ problems or sleep disorders.
Read More


Selecting Dental Products
Best Toothpaste in India: Five Dentist-Recommended Types
Medically Reviewed By Colgate Global Scientific Communications
Read More
Selecting Dental Products
Soft Vs. Hard Toothbrush: Which One Should You Use?
Choices abound when it comes to your toothbrush. Find out how to choose between a soft bristle toothbrush, a hard toothbrush, or an electric-powered brush.
Read More

Selecting Dental Products
Using Tartar Removal Toothpaste For Healthy Teeth And Gums
Tartar removal toothpaste helps remove plaque and prevent tartar build-up on teeth. Learn how it works and some of the best tartar control toothpaste picks.
Read More
Selecting Dental Products
Antiseptic vs. Antibacterial Mouthwash: What's the Difference?
Learn the differences between antiseptic and antibacterial mouthwash for optimal oral health. Choose the right one for your needs.
Read More
Selecting Dental Products
Choosing a baby toothbrush
You can establish a regimen of infant oral care early on, even before that first tooth sprouts. Choosing an infant toothbrush makes it easy to practice good oral care from the start.
Read More
Selecting Dental Products
Kids Electric Toothbrush: Why is it important?
You can establish a regimen of infant oral care early on, even before that first tooth sprouts. Choosing an infant toothbrush makes it easy to practice good oral care from the start.
Read More
Selecting Dental Products
Choosing The Right Toothpaste For Your Kids
Explore the importance of choosing the right toothpaste for your kids. Discover expert tips and insights to make brushing fun and effective. Learn more!
Read More
Selecting Dental Products
How to choose toothbrushes for kids?
Lack of awareness is a major issue when choosing kids toothbrushes. Using the wrong toothbrushes can damage your kid’s teeth and gums. Let's see how to choose the correct toothbrush for your kids.
Read More

Threats to Dental Health
Dental Grills — The New Trend Affecting Dentistry And The Health Of Your Teeth
Read More



Threats to Dental Health
VANITY New Research For Toothpaste And Mouthwash Effects on Covid-19 Virus
Can toothpaste and mouthwash neutralize and reduce the virus that can cause COVID-19 in your mouth? Read more on this new Colgate-Palmolive research for toothpaste and mouthwash effects on the COVID-19 virus.
Read More
Threats to Dental Health
New Research For Toothpaste And Mouthwash Effects on Covid-19 Virus
Can toothpaste and mouthwash neutralize and reduce the virus that can cause COVID-19 in your mouth? Read more on this new Colgate-Palmolive research for toothpaste and mouthwash effects on the COVID-19 virus.
Read More
Threats to Dental Health
How Mouth Spray Helps Dry Mouth
A mouth spray may be good option if you need short-term relief of dry mouth. Learn how sprays work and what you can do for longer-term solutions, here.
Read More
Threats to Dental Health
Rotten Teeth: Symptoms And Treatment
How can you tell if you have rotten teeth? Can a dentist save them and make your mouth healthy again? Learn the signs and treatments for rotten teeth.
Read More
Threats to Dental Health
Effects Of Smoking On Teeth
Although they aren't addressed very often, the effects of smoking on teeth and the oral cavity are important in the process of quitting.
Read More
Threats to Dental Health
How Acidic Drinks Affect Teeth
Acidic drinks are very damaging to tooth enamel, no matter how long you've held the habit, so be sure to consume the following in moderation... Learn more.
Read More
Threats to Dental Health
The Many Causes Of Loose Teeth
As children, wiggly, loose teeth meant that we would soon be richer, thanks to the tooth fairy. As adults, we want to keep our teeth for a lifetime.
Read More
Threats to Dental Health
How Vitamin D Effects Your Oral Health
How does vitamin D help your teeth? Learn more of the benefits of Vitamin D for Your Mouth from Colgate.
Read More
Threats to Dental Health
What Causes Cheek Swelling?
Noticing that your cheeks are swollen can be distressing. There are many possible causes of cheek swelling, and a doctor or dentist can diagnose the issue.
Read More
Threats to Dental Health
Do You Have Acid Erosion on Your Teeth?
Do you have acid erosion on your teeth? What causes acid erosion on your teeth? Visit Colgate India now and learn more information on dental erosion.
Read More
Threats to Dental Health
The Truth About Tartar: Can You Remove Them At Home?
Tartar can have negative effects on your oral health, so it shouldn't be allowed to build up. No matter what you may hear or read, it's not a good idea to remove tartar at home.
Read More
Threats to Dental Health
What Causes Pale Gums? 3 Possibilities To Discuss With Your Dentist
If your gums appear paler than usual, it may indicate that you have a health problem. Here are three possibilities to discuss with a doctor or dentist.
Read More
Threats to Dental Health
Anaemia Gums and Your Oral Health
Anemia can lead to a variety of problems affecting your oral health. Visit Colgate now and learn more about the symptoms, treatment, and prevention.
Read More























Teeth Whitening
How Can I Get Whiter Teeth? A Guide to Teeth Whitening Methods
Medically Reviewed By Colgate Global Scientific Communications
Read More



Teeth Whitening
5 things to consider while picking the best whitening toothpaste
The best whitening toothpaste gives you quick and effective results. Consider these 5 things to pick the ideal teeth-whitening toothpaste for you.
Read More


Teeth Whitening
Three types of teeth stains and how to remove them
Understand teeth stain types, causes and removal methods with this comprehensive guide on professional whitening treatments and at-home solutions.
Read More

Teeth Whitening
Top Tips on How to Remove Yellow Stains From Teeth
Learn how to remove yellow stains from teeth with home remedies. Explore the causes of yellow teeth, prevention & professional teeth whitening options.
Read More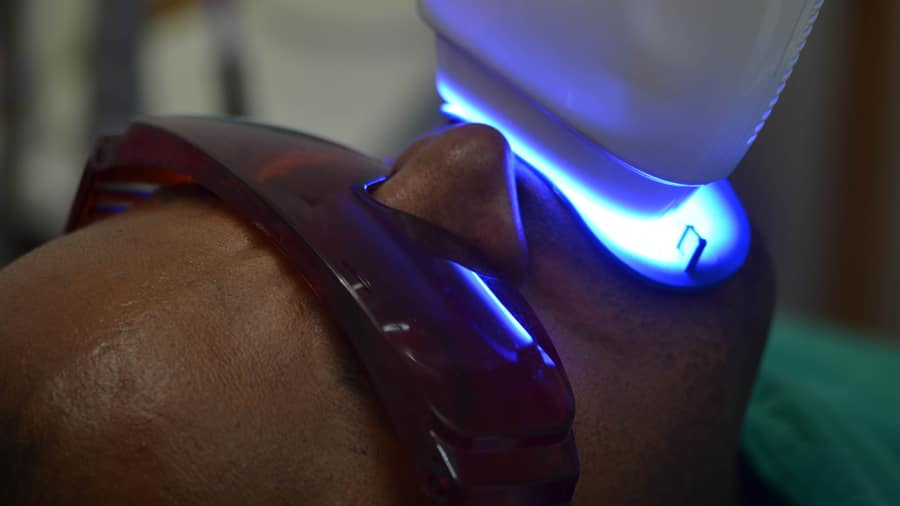



Teeth Whitening
Banana Peel Teeth Whitening: Will It Give You A Brighter Smile?
Some claim that banana peel teeth whitening works, but does the science support it? Learn more about bananas and what you can do for a whiter smile, here.
Read More
Teeth Whitening
What are teeth whitening options if you have a crown?
Can you whiten a crown when you've had dental work and want to brighten your smile? Before you proceed, it's best to speak with your dentist about your options.
Read More
Teeth Whitening
Burned Gums from Teeth Whitening: What You Need to Know
If you've been whitening your teeth at home, you could have burned your gums from teeth whitening. Find out more about it, here from Colgate®.
Read More
Teeth Whitening
Best Over The Counter Teeth Whitening (For Any Lifestyle)
Whether you're on a budget or need results for a big event, here are the best over the counter teeth whitening options for any lifestyle. Learn more, here.
Read More
Teeth Whitening
Build Your Home Teeth Whitening Kit
You can make an effective home tooth whitening kit with over the counter products, at home. Find out more about making a home tooth whitening kit, here.
Read More
Teeth Whitening
Do Teeth Whitening Strips Work?
Explore the effectiveness of teeth whitening strips, the cost, pros & cons of teeth whitening strips, and alternative methods in this comprehensive guide.
Read More
Teeth Whitening
Five Foods that Cause Stains and Six Foods that Prevent Them
Watch what you eat and drink because certain foods and beverages cause discoloured teeth.
Read More
Teeth Whitening
Does Tea Stain Teeth?
We know that coffee can stain those pearly whites, but does tea stain teeth? The answer is yes. In fact, tea might be even more… Read more at Colgate.com
Read More
Teeth Whitening
Different Types of Teeth Whitening Products
Professional teeth whitening products are known for their quick and effective whitening results. Here are some over-the-counter whitening products to know.
Read More
Teeth Whitening
What Works Best To Remove Coffee Stains From Your Teeth?
Most of us can't live without a daily dose of coffee to jump start the day, but could the beverage that puts morning smiles on… Read more at Colgate.com
Read More
Teeth Whitening
How To Maintain White Teeth
Whether you already have white teeth or you've just completed a whitening treatment, keep in mind that you've still got some wor...
Read More
Teeth Whitening
How to Whiten Your Teeth?
Learn how to whiten teeth effectively with at-home whitening and professional treatments to achieve a brighter smile and prevent tooth discolouration.
Read More
Teeth Whitening
How To Whiten With Braces
Knowing how to whiten teeth with braces on isn't impossible, but special care must be taken to ensure treatment is successful. Here are three options.
Read More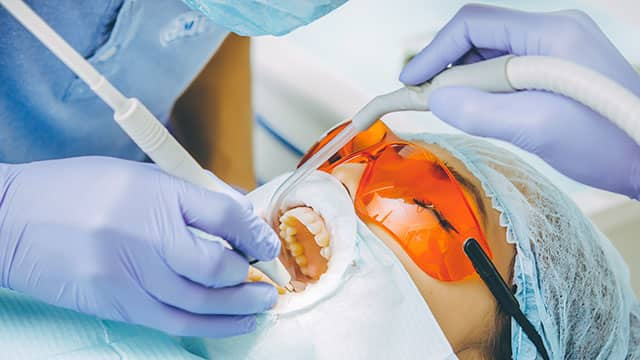
Teeth Whitening
Teeth Whitening Treatment Options
Learn about teeth whitening treatments, from professional procedures to at-home kits. Discover popular teeth whitening products for brighter teeth.
Read More
Teeth Whitening
Is a Teeth Whitening Light Effective?
Looking for a way to brighten your smile with teeth whitening? Learn more about both UV and blue light teeth whitening to decide which is the best option for you.
Read More
Teeth Whitening
Is Professional Teeth Whitening Right For You?
Professional teeth whitening can seem like a miracle solution for stubborn stains and yellowing teeth, but is it the best option...
Read More
Teeth Whitening
Is The Cost Of Professional Teeth Whitening Worth It?
If you've considered whitening your teeth, you may already know the professional teeth whitening cost can be high — much more expensive than at-home alternatives. Learn more here.
Read More
Teeth Whitening
Should You Try DIY Teeth Whitening Paste?
Tooth whitening is the process which lightens teeth, helps remove stains, and corrects tooth discoloration. Learn more on teeth whitening procedures, types, risks, and more.
Read More
Teeth Whitening
Types of Tooth Discoloration And What They Mean
Tooth discoloration may occur due to various reasons. Understand types and shades of teeth discoloration, causes, prevention, and effective treatment.
Read More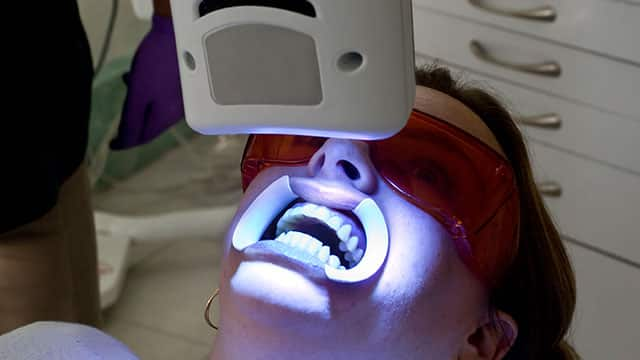
Teeth Whitening
Is UV Teeth Whitening Safe?
Is UV teeth whitening safe to do yourself at home? Find out more about UV teeth whitening including safety information and alternatives.
Read More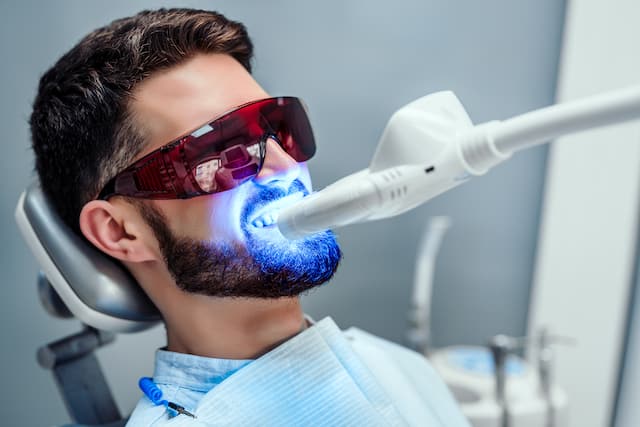
Teeth Whitening
Is LED Teeth Whitening Right For You?
The process is minimally invasive and can offer great results. LED teeth whitening is a popular option for achieving a brighter smile, but is it the best at-home treatment for you?
Read More
Teeth Whitening
How much does teeth whitening cost?
What impacts teeth whitening cost? Learn about professional in-office whitening, at-home kits, everyday brushing routine & factors affecting the price for achieving a brighter smile.
Read More
Teeth Whitening
Home Remedies For Teeth Whitening
Explore home remedies for teeth whitening and professional teeth whitening options available over the counter to brighten your smile.
Read More



Teeth Whitening
The Best Whitening Mouthwash: What to Look For
What is the best whitening mouthwash out there and is using it going to help you get a brighter smile? Find out here!
Read More
Teeth Whitening
How Custom Whitening Trays Brighten Your Smile
If your teeth aren't as white as you'd like, there are safe and simple ways to improve it. One of them involves custom whitening trays.
Read More
Teeth Whitening
What Are the Benefits of Turmeric for Your Teeth?
Does turmeric for teeth whitening actually work? Read on to learn more about turmeric, if it whitens teeth and if there are other oral health benefits.
Read More
Teeth Whitening
3 Tips For Preventing Teeth Stains From Braces
Learn about our top 3 tips for preventing teeth stains from braces and whitening your teeth evenly once they come off with Colgate.
Read More
Teeth Whitening
How To Remove Smoking Stains From Your Teeth?
Discover effective methods to remove smoking stains from your teeth and restore your bright smile. Learn about natural remedies, prevention and more.
Read More
Teeth Whitening
How To Remove Smoking Stains From Your Teeth?
Unveil the secrets of teeth brightening: From home remedies to professional treatments, learn how to achieve a radiant smile!
Read More
Teeth Whitening
Does Teeth Whitening Foam Work?
Discover effective methods to remove smoking stains from your teeth and restore your bright smile. Learn about natural remedies, prevention and more.
Read More
Teeth Whitening
How Does Teeth Brightening Work?
Unveil the secrets of teeth brightening: From home remedies to professional treatments, learn how to achieve a radiant smile!
Read More
Teeth Whitening
Top Teeth Whitening Tips to Brighten Your Smile
Tooth discoloration may occur due to various reasons. Understand types and shades of teeth discoloration, causes, prevention, and effective treatment.
Read More





Infant & Kids Oral Care 101
Dental Care for Kids: The Best Secrets for Keeping Your Child's Smile Bright
Read More



















Infant & Kids Oral Care 101
Toothpaste for Toddlers 2 Years Old and Under: What to Look For?
Read More
Infant & Kids Oral Care 101
9 Causes of Bad Breath in Children
Even healthy children can sometimes experience bad breath. If you've noticed that your little one's breath is not so pleasant, there is hope.
Read More
Infant & Kids Oral Care 101
Top Teething Remedies For Babies: Helping Your Little One Overcome The Pain
When your baby's first tooth breaks through the gums, you have both reached an exciting milestone. But it's a painful one. These remedies can help.
Read More
Infant & Kids Oral Care 101
Baby Bottle Tooth Decay
In infants, tooth decay is commonly referred to as baby bottle tooth decay. This occurs when sugars from food & liquids attach to teeth for periods of time.
Read More
Infant & Kids Oral Care 101
Bleeding Gums In Children: Should You Be Worried?
Are bleeding gums in kids a cause for concern or nothing to worry about? For adults, gums that bleed during brushing or flossing may be a sign of gingivitis.
Read More
Infant & Kids Oral Care 101
Toddlers And Bleeding Gums: What Should You Do?
Toddlers and bleeding gums don't have to be a cause for alarm, but they're definitely a warning sign that your little one's oral habits should be improved.
Read More
Infant & Kids Oral Care 101
Space Maintainers To Help With A Perfect Smile
Space maintainers are a dental device used for children as they lose teeth and wait for adult teeth to grow in. Read more information here, at Colgate.com.
Read More
Infant & Kids Oral Care 101
What To Do For A Child With A Toothache?
Most of the time, a toothache is caused by injury to the tooth or a cavity. Here are some things that you can do to help your child when he has a toothache.
Read More
Infant & Kids Oral Care 101
Natural Toothache Pain Relief for Your Child
Whether your little one complains of a loose tooth after playing in the yard or your older child has unexpected tooth pain in the night, you can naturally and effectively administer toothache pain relief until you can visit with a dentist.
Read More
Infant & Kids Oral Care 101
Kids' Teeth And Cavity Protection
Even if you had cavities when you were young, your child doesn't have to develop them. Find out how to protect kids' teeth from tooth decay.
Read More
Infant & Kids Oral Care 101
What Causes White Spots on Baby Teeth?
Although you don't want to panic, you do want to take action if you see white spots on baby teeth. Here are two reasons these blemishes may develop.
Read More
Infant & Kids Oral Care 101
What Parents Should Know About Mouthwash For Children
Toothpaste and mouthwash for children often feature kid-friendly flavours and graphics that make mouth care a bit more fun. Is your child ready to swish?
Read More
Infant & Kids Oral Care 101
When To Take Your Baby To The Dentist And Doctor: Dental Care, Teething Issues And More
Paediatric dentists and family dentists agree that you should take your baby to the dentist for the first time no later than the child's first birthday.
Read More
Infant & Kids Oral Care 101
When To Start Brushing Baby Teeth
Get your baby's toothbrush ready! Learn more about when to start brushing your baby's teeth to begin good oral health care habits.
Read More

Infant & Kids Oral Care 101
Best Toothpaste for Kids With Cavities
For kids, tooth decay is a common problem. What is the best toothpaste for kids who have cavities? Find out at Colgate
Read More
Infant & Kids Oral Care 101
How Do I Know If My Baby Is Teething?
Discover common baby teething symptoms and learn how to ease your little one's discomfort. Get helpful tips to take care of your baby's oral health.
Read More












.jpg)






























Dental Emergencies & Sports Safety
Can I Use Clove Oil For Toothache Pain?
Using clove oil for toothache pain can provide you with relief now, but it doesn't last as long as treatment from your dentist. Here's why.
Read More
Dental Emergencies & Sports Safety
Instant Relief from Tooth Pain: Essential Tips
Discover straightforward remedies on how to relief from tooth pain. Learn essential techniques to alleviate tooth pain and restore comfort effortlessly.
Read More



Dentures
How To Clean Dentures To Avoid Bacteria Build-up
Learning how to clean dentures is important to maintaining good daily hygiene, but occasionally you may find it necessary to take these additional steps.
Read More





Fillings
Tooth Pain After A Filling: Is It Normal?
There are several reasons why you may experience tooth pain after a filling. Is It Normal? Is there anything you can do about it? Learn more, here.
Read More
















Mouth Sores and Infections 101
Everything You Need to Know About Oral Thrush: Causes, Symptoms, and Treatment
Read More
Mouth Sores and Infections 101
Understanding Sore Tongue and Throat: What You Need to Know?
Read More


Mouth Sores and Infections 101
Oral Care for Babies & Kids With Canker Sores (Mouth Ulcer)
Read More
Mouth Sores and Infections 101
Understanding Mouth Ulcers in Kids: Causes, Symptoms, and Treatments
Read More
Mouth Sores and Infections 101
How Salt Water Mouth Rinse Benefits Oral Health
A salt water mouth rinse is useful for a number of different reasons. It's a great option for anyone who has a sore throat, gum sores or recently underwent dental procedures. It doesn't take the place of modern dental hygiene, but is used as a supportive measure for adults and children alike.
Read More
Mouth Sores and Infections 101
How To Kill Mouth Bacteria And Keep It Away
There's a party going on in your mouth, to which you might not have been invited. The human mouth can be home to more than 700 species of bacteria, some of which might be more harmful than others. While many types of bacteria will help break down food and actually protect your teeth, some, such as Streptococcus mutans, play a part in tooth decay, and others, such as Porphyromonas gingivalis, can lead to gum disease. If you've ever dealt with bad breath, you can blame bacteria for that, too.Luckily, figuring out how to kill mouth bacteria isn't that tricky. It comes down to developing a great at-home oral care routine and doing what you can to minimise the presence of the bad bacteria.
Read More
Mouth Sores and Infections 101
What Are Tonsil Stones?
Tonsil stones, clinically called tonsilloliths, are small, white discharges that form in the crevices of the tonsils. They are typically found on the surfaces of the pharyngeal tonsils on either side at the back of the throat. They can be as small as a grain of rice or as large as a pea. They are quite common and usually harmless, but they may spark alarm in patients when noticed for the first time.
Read More

Mouth Sores and Infections 101
What A Gum Boil Could Mean For Your Dental Health
Medically Reviewed By Colgate Global Scientific Communications
Read More
Mouth Sores and Infections 101
What Causes a Black Spot on Your Gums?
Oral conditions like dark spots on your gums have various causes and can be challenging to diagnose. Learn more now at Colgate India.
Read More
Mouth Sores and Infections 101
Everything You Need to Know About Aphthous Stomatitis
Discover everything you need to know about aphthous stomatitis, including its causes, symptoms, and effective treatment options for canker sores
Read More
Mouth Sores and Infections 101
Median Rhomboid Glossitis: Causes, Symptoms, and Treatments
Learn about Median Rhomboid Glossitis, its causes, symptoms, and effective treatment options and how common oral fungal infections impact oral health
Read More
Mouth Sores and Infections 101
What Are Canker And Mouth Sores?
Learn why your gums might be white or pale. From canker sores to serious conditions, get insights on symptoms, diagnosis & effective treatments for healthy gums.
Read More










Plaque & Tartar
How Bacterial Plaque Causes Gum Disease And Tooth Decay
When bacteria overstay their welcome in your mouth, numerous dental problems can set in. Visit Colgate now and learn how this happens.
Read More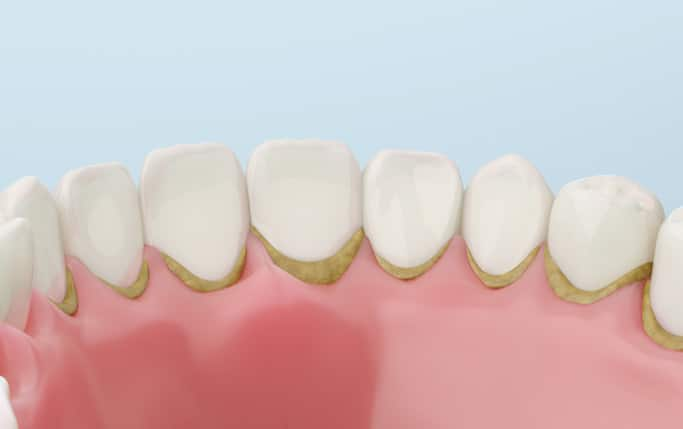
Plaque & Tartar
Dental Plaque: Meaning, Causes and Treatment
Dental plaque meaning: Plaque is a sticky biofilm that develops on teeth as a result of the bacteria that naturally live in the mouth. Learn more!
Read More
Plaque & Tartar
Black Tartar on Teeth: Causes, Prevention & Removal
Black tartar on teeth forms below the gum line and causes many dental issues. Though it isn't difficult to treat, only dentists can remove it.
Read More
Plaque & Tartar
How To Remove Plaque From Teeth?
What exactly is plaque? Visit Colgate India now, and learn what plaque is and how to remove and prevent it from damaging your teeth.
Read More


















Tooth Removal
When Surgical Extraction Of Teeth Is Necessary
Although many of your teeth are easily removable, it's occasionally more complicated. Here's why the surgical extraction of teeth may become necessary.
Read More


Oral Care During Pregnancy
Sensitive Teeth During Pregnancy: What To Expect And How To Cope
Read More

Oral Care During Pregnancy
Avoiding A Toothache During Pregnancy
To avoid a toothache during pregnancy, or any other dental problem when expecting a baby, your best strategy starts with a dental visit.
Read More
Oral Care During Pregnancy
Relief For Dry Mouth During Pregnancy
What can you do about dry mouth during pregnancy? While dry mouth may not be as talked about as other common pregnancy symptoms, that dry, sticky...
Read More
Oral Care During Pregnancy
Bleeding Gums During Pregnancy: Should You Worry?
Chances are good that, during your pregnancy, you will experience a myriad of symptoms you have never had before. Bleeding gums is one such condition.
Read More




















Wisdom Teeth
Wisdom Tooth Extraction
A wisdom tooth extraction is a surgical procedure to remove one or more of your wisdom teeth. Learn what to expect, before during and after the surgery.
Read More
Wisdom Teeth
What Will Tooth Extraction Cost?
Numerous factors can determine how tooth extraction and type of anaesthesia will affect your budget, so your dentist or oral surgeon will be there to evaluate your mouth and guide you.
Read More
Wisdom Teeth
Wisdom Tooth Pain Relief: Simple and Effective Methods
Discover effective wisdom tooth pain relief methods. Learn how to alleviate discomfort with home remedies and medical treatments.
Read More












Dental Visits
How Often Should You Go to the Dentist
While it’s true that a twice-yearly cleaning schedule is a good rule of thumb for many people, scheduling dental visits should be based on each person’s oral hygiene, habits and medical conditions.
Read More
Dental Visits
Do You Fear Going to the Dentist | Colgate®
Keep in mind the apprehension of going to the dentist can also be learned and passed down from parent to child. Learn more here.
Read More
Dental Visits
Five Types Of Cosmetic Dentistry Procedures
Learn more about oral care for adults, including how to properly brush and floss, adult toothbrushes, and much more, from the Colgate Oral Care Centre.
Read More
Dental Visits
The History Of Dentistry
A look at the history of dentistry will help you understand where the modern dentistry came from and how they led to today's practices. Learn more at Colgate.
Read More
Dental Visits
What is Teledentistry?
Did you know that you can get dental care virtually? Visit Colgate now and learn about teledentistry, how it works, the benefits, and how you can use it.
Read More
Dental Visits
What Is A Paediatric Dentist?
Visit Colgate now and learn about the difference between pediatric dentists and general dentists, and the benefits pediatric dentists provide.
Read More
Dental Visits
How Teeth Cleaning Works?
Learn why regular teeth cleaning is crucial for dental health. Prevent tooth decay, gum diseases, and maintain oral well-being with proper dental care.
Read MoreDental Visits
A Trip To The Dentist
Learn from video and guide from dental experts on the topics of: A trip to the dentist
Read More
















Tooth Sensitivity
How Does Mouthwash For Sensitive Teeth Work?
Regular rinsing with mouthwash for sensitive teeth can actually bring relief to many who suffer from tooth sensitivity. Here's how it kills the pain.
Read More
Tooth Sensitivity
How To Pursue Sensitive Teeth Treatment
Ice cream is a futile craving if you have sensitive teeth. With the proper sensitive teeth treatment, you can dive right (back) into your favourite flavour.
Read More
Tooth Sensitivity
Sensitive Teeth After Cleaning By The Dentist
If you experience sensitive teeth after cleaning treatment, and it continues longer than normal, your dentist can offer the following help and advice.
Read More
Tooth Sensitivity
What Causes Sensitive Teeth?
Approximately 40 million adults in the United States experience tooth sensitivity. What Causes Sensitive Teeth? Any number of dental problems. Find your answers here.
Read More
Tooth Sensitivity
Is Sparkling Water Bad For Your Teeth?
Is sparkling water bad for your teeth? Here's what you need to know about the popular beverage.
Read More




Tooth Sensitivity
The Best Toothpaste For Sensitive Teeth: What's In It?
Learn more from Colgate to protect important surfaces of your teeth. Try the best toothpaste for sensitive teeth that can relieve your discomfort shortly.
Read More
Tooth Sensitivity
Sensitive Teeth Causes: What You Need to Know?
Having sensitive teeth triggers a sudden pain upon eating anything hot, cold or sour. Learn what makes your teeth sensitive and what you can do about it.
Read More

Tooth Sensitivity
Sensitive Gums? Here Are Three Surprising Causes
Gum disease is typically to blame for sensitive gums, but there may be another issue hiding right under your nose. Here are a few causes of sensitive gums.
Read More
Tooth Sensitivity
Dental Desensitizing Agents: What You Need to Know?
Discover everything you need to know about dental desensitizing agents, from how they work to their benefits, application methods, and choosing the right one for you.
Read More



Early Orthodontics
Why Does My Child Need A Palate Expander?
Is a palate expander necessary? Is it painful? What does it do? Find out more about how this treatment can help guide the growth of your child's mouth.
Read More
Early Orthodontics
5 Most Common Questions Kids Have About Braces
Getting braces can be a stressful endeavour for parents and children. Take a look at some of the best ways to combat the fear.
Read More
Early Orthodontics
Are Gold Braces Right For You?
These days, braces can be a fun fashion statement. Here's what to know about gold braces versus other options before you visit the orthodontist.
Read More
Early Orthodontics
Braces Colours: How To Choose Your Perfect Shade
Braces colours abound! How can you pick the right colour for your braces? Learn more here.
Read More
Early Orthodontics
Getting Braces: What You Need to Know
What to know before getting braces? Learn more about the preparation and procedure of getting braces with this article from Colgate.
Read More
Early Orthodontics
Foods You Can Eat With Braces
You know to avoid taffy, but what foods are safe and comfortable to eat? Here's a rundown of foods you can eat with braces to keep them intact.
Read More
Early Orthodontics
What Is An Open Bite?
If your child's teeth aren't lining up quite right, he or she may have an open bite.
Read More
Early Orthodontics
What Is The Best Age For Braces?
While the best age for braces tends to be during the childhood years when teeth are developing, it's never too late to pursue a healthier smile.
Read More
Early Orthodontics
Braces Pain: The Gain Is A Beautiful Smile!
Experiencing braces pain? Why does this happen, and what can you do about it? Visit Colgate now and learn about causes this discomfort and how to relieve it.
Read More
Early Orthodontics
Ceramic Braces Vs Metal Braces
Your child might be worried about the difference between metal and ceramic braces, both in appearance and functionality. Get the facts straight now at Colgate.
Read More
Early Orthodontics
First Paediatric Orthodontist Visit: What To Expect
Not sure what to expect at your first orthodontic consultation? No need to worry. Visit Colgate now and find out what happens at the first orthodontist visit.
Read More








Veneers
Can You Whiten Veneers?
After a few years your once-bright veneers may look discoloured. Can You Whiten Veneers? Find out more about caring for your veneers and keeping them white.
Read More

Diabetes & Other Endocrine Disorders
Prevent Diabetes Problems, Keep Your Teeth And Gums Healthy
Read More




.png)
Diabetes & Other Endocrine Disorders
Diabetes And Dental Treatment: What You Should Know
Dealing with diabetes and dental treatment can be tricky. Diabetes can lead to oral health complications, and it's important to balance both health areas
Read More
Diabetes & Other Endocrine Disorders
Can You Get Diabetes From Eating Too Much Sugar?
Can you get diabetes from eating too much sugar? The answer is complicated, but diets and lifestyles can lead to this disease. Learn more, here.
Read More

Diabetes & Other Endocrine Disorders
Gum Disease and Diabetes: Detection and Treatment
Knowing the stages of diabetes where you're most likely to see these partner symptoms, and what preventive steps to take, will help improve the quality of your life with diabetes.
Read More
Diabetes & Other Endocrine Disorders
Adding a Smile Helps with Your Diabetes Management
While oral care should be an important part of everybody’s lives, paying more attention to your gums and mouth will play a greater role if you have diabetes.
Read More
Diabetes & Other Endocrine Disorders
If You Have Diabetes, You May Need to Pay Closer Attention to Your Gums
If you are a person living with and managing diabetes, good healthcare for you goes beyond just balancing the blood sugar; taking care of your mouth and gums is also an important goal.
Read More
Diabetes & Other Endocrine Disorders
Oral Care is Diabetes Care: Top Tips from Colgate
Oral hygiene is at the forefront of everyone’s healthcare priorities, and rightfully so: the confidence boost that a healthy smile can give you has no parallel!
Read More
Diabetes & Other Endocrine Disorders
Prevention is Better Than Cure: Why Oral Check-ups are Important for Patients with Diabetes
Keeping yourself healthy is an active venture. All the healthy choices you make build up to a wholesome life, and this is true for oral health as well.
Read More





Adult Orthodontics
What Are the Different Types of Teeth Braces, and Which Is Right for Me?
Read More

Adult Orthodontics
Are Ceramic Braces Right For You?
Ceramic braces are well-suited for many patients without severe misalignments. Your orthodontist will let you know if you're a good candidate for these braces after they examine your teeth.
Read More
Adult Orthodontics
Are White Braces Right For You?
Traditional metal braces can make you insecure about your smile during treatment. White braces made from ceramic may blend in better with your teeth.
Read More
Adult Orthodontics
Do Braces Hurt?
Are you feeling anxious about getting braces? You may be wondering,
Read More
Adult Orthodontics
How To Clean Retainers
The two most common types of removable retainers are the Hawley retainer and the Essix retainer. Learn how to clean retainers and avoid plaque build-up.
Read More
Adult Orthodontics
What Are Lingual Braces?
Lingual braces, one of the more recent forms of orthodontic work, is proving popular for people conscious about the look of braces.
Read More
Adult Orthodontics
What To Know About Metal Braces?
A variety of orthodontic options exist today for people looking into getting braces. From traditional metal braces to Invisalign...
Read More
Adult Orthodontics
Tips For Adults With Braces | Colgate®
When you have braces on teeth, those teeth need extra attention to protect them from decay, staining and gum disease. You should also take precautions to avoid damaging the braces.
Read More
Adult Orthodontics
Teeth Reshaping Treatments and Costs
Teeth reshaping is a cost-effective way to fix chipped teeth. It's usually combined with bonding to create a beautiful new smile.
Read More
Adult Orthodontics
Orthodontist Vs. Dentist: Who Should You See?
It can be confusing to determine the differences between an orthodontist vs. dentist. Here's what you need to know about these dental professionals.
Read More
Adult Orthodontics
What Are Damon Braces? 5 Things You Should Know
Traditional braces can add to an already stressful school year for your kids. What are Damon braces? A solution to crooked teeth, minus tightening pain.
Read More
Adult Orthodontics
Why Use Rubber Bands With Braces?
Why do orthodontists use rubber bands with braces? Rubber bands are an important part of the orthodontic treatment. Learn more here.
Read More
Adult Orthodontics
What Is Tooth Wax and How to Use It Properly?
Tooth wax, also called dental wax, is a soft material that can be used to temporarily cover sharp surfaces inside your mouth. Learn more now at Colgate IN.
Read More
Adult Orthodontics
Caring for Braces: You're on Your Way to a Healthy Smile
Caring for braces is important. The better care you take of your braces, the more comfortable and effective they'll be. Learn more now at Colgate India.
Read More
Adult Orthodontics
How Does A Retainer Work?
Retainers are commonplace in oral care. It helps retain the position of your teeth. But how exactly does a retainer work? Learn more now at Colgate.
Read More
Adult Orthodontics
When & How To Use Mouthwash: Before Or After Brushing?
Should you use mouthwash before or after brushing? Here's the answer that will help you improve your daily oral care routine.
Read More










Gum Disease
Gum Disease: Causes, Symptoms & Treatment
Protect your smile with our comprehensive guide to gum disease. Learn about symptoms, prevention, and effective treatments to maintain healthy gums.
Read More











Gum Disease
Home Remedies For Swollen Gum
Discover effective home remedies for swollen gums. Learn natural solutions to alleviate discomfort and promote oral health effortlessly.
Read More




Gum Disease
Gingivitis: Overview And Prevention
Gingivitis is a treatable and reversible form of gum disease. It is the first and mildest stage.
Read More
Gum Disease
Professional Gingivitis Treatment And Home Care
If you have tender, red, swollen, and bleeding gums you will need gingivitis treatment. This is the earliest form of gum disease that can resolve with...
Read More
Gum Disease
Gingivitis And Your Children
Although gingivitis is the earliest and mildest form of gum disease, severe gingivitis can lead to chronic cases that require more diligent management.
Read More
Gum Disease
How to Cure Gingivitis: Causes And Treatment
Discover effective treatments and prevention tips for gingivitis. Learn about the causes, symptoms, and home remedies to keep your gums healthy.
Read More
Gum Disease
What Is The Best Toothpaste For Bleeding Gums (Gingivitis)?
Struggling with sensitive or bleeding gums? Our blog explains how specialized toothpaste can help alleviate these issues and improve your dental health
Read More
Gum Disease
How To Clean Teeth At Home Naturally
Empower your oral care routine with easy-to-follow steps for teeth cleaning at home. From brushing techniques to natural remedies, unlock the secrets to a radiant smile.
Read More
Gum Disease
Bleeding Gums: What You Should Know?
Noticing that your gums bleed when you brush or floss can be alarming. What are the possible causes of bleeding gums? Learn more here.
Read More
Gum Disease
Antimicrobial Therapy For Gum Disease
Antimicrobial therapy is a form of oral treatment used to eliminate or reduce the development of bacterial infections in the mouth.
Read More
Gum Disease
Gum Graft Pain: What To Expect & How To Relieve Pain
Usually gum grafts are done by a periodontist, which is a dentist who treats conditions of the gums and the bone that supports them.
Read More
Gum Disease
Prevent Gum Disease With The Right Oral Care Products
Do you have what it takes to stop plaque from harming your mouth? The first stage of gum disease, gingivitis, is caused by plaque that has built up...
Read More
Gum Disease
What Are Periodontal Pockets?
Gum disease is an inflammation of the gums that can progress to affect the bone that supports your teeth. Find out the causes of gum disease and how to prevent it.
Read More
Gum Disease
What Is Trench Mouth?
One of the most serious and painful types of gum disease is called trench mouth. The name dates back to World War I. Find out more about trench mouth here.
Read More.png)
Gum Disease
Why Is Mouthwash For Bleeding Gums Beneficial?
Bleeding gums are an early sign of gum disease. Using an antimicrobial mouthwash for bleeding gums can help stop it in its tracks. Here's how it works.
Read More
Gum Disease
How To Fight Gingivitis In Three Easy Steps
Gum disease is very common. If you want to know how to fight gingivitis, it's as easy as one-two-three: brushing, flossing and professional cleanings.
Read More
Gum Disease
Gum Disease Symptoms And What To Do About Them
By familiarising yourself with gum disease symptoms, you can get proper care immediately if you develop a problem.
Read More
Gum Disease
Periodontal Charting: What It Is & Why It's Important
Have you ever noticed that the dental hygienist or dentist was taking measurements of your gums? Periodontal charting is a part of your preventative care.
Read More
Gum Disease
Can Receding Gums Grow Back?
Gum recession happens for a number of reasons, from brushing your teeth with too much pressure to grinding your teeth. Learn more about what causes gums to recede and how to treat it here.
Read More
Gum Disease
Gingivectomy Surgery: What You Need To Know
A gingivectomy may be performed to heal the effects of periodontal disease or to correct a gum condition involving the structure of teeth. Learn more here.
Read More.jpg)
Gum Disease
How Poor Dental Care Can Affect Your Overall Health
Although you probably understand that poor dental care can lead to cavities, did you know that other, more serious health issues can arise? Learn more here.
Read More
Gum Disease
Mouthrinse for Gum Disease: Another Good Tool
Although gum disease comes from bacteria living in your mouth, mouthwash for gum disease is actually the ideal complement to traditional oral care.
Read More
Gum Disease
Successful Treatments For Periodontal Disease
Today, with so many successful treatment options available for advanced periodontal disease, losing teeth doesn't have to be your next step with an unhealthy gumline.
Read More
Gum Disease
Understanding Diabetes Gum Problems
Due to the prevalence of diabetes, it is critical to know how it can affect your body, and what to do if you detect gum problems.
Read More
Gum Disease
What Is Strawberry Gum Disease?
What is strawberry gum disease? Click here to read more about strawberry gum disease and the signs with Colgate.
Read More
Gum Disease
Why Do You Have Itchy Gums?
The most likely reason for your itchy gums is plaque. check-in with your dentist so they can properly examine your gums and teeth.
Read More

Gum Disease
Bleeding Gums: Causes & Treatment
Learn about effective treatments for bleeding gums, including professional advice and home care tips. Prevent gum disease and maintain optimal oral health with our expert insights
Read More
Gum Disease
Common Warning Signs Of Gingivitis
Learn the warning signs of gingivitis to combat the condition immediately. Gingivitis, the first stage of gum disease, is revers...
Read More
Gum Disease
4 Simple Causes of Irritated Gums
Gum irritation has many possible causes, but some of them come out of a personal habit you may not be paying attention to. Here are a few you should know.
Read More
Gum Disease
The Link Between Gum Disease and Blood Pressure
Learn what you need to know about gum disease and its link to high blood pressure with Colgate ®. Click here for more information.
Read More
Gum Disease
Receding Gums Treatment and Causes
Receding gums cannot grow back. However, your dentist or periodontist can help you treat and prevent it from getting worse. Learn more now at Colgate IN.
Read More
Gum Disease
What is Root Planing and Scaling Teeth?
If gum disease develops, your hygienist will need to implement a deeper type of cleaning - scaling teeth and root planning. Learn more now at Colgate India.
Read More
Gum Disease
Gum Paint Explained: Uses, Benefits, and Application Tips
Learn how gum paint can help treat gum inflammation, bleeding, and infections. Discover the benefits, proper usage, and why it's essential for healthy gums
Read More
Gum Disease
Tips for Gum Pain Relief
Discover the causes and effective strategies for gum pain relief, from home remedies to over-the-counter medications and professional dental care.
Read More










Adult Oral Care
Choosing the Best Toothbrush for You
Brushing your teeth is an essential part of your daily oral care. Visit Colgate IN now and learn about how to find a toothbrush that is right for you.
Read More
Adult Oral Care
Root Resorption: Complications, Causes, And Treatment
Root resorption is a natural process, but problems can sometimes arise. Visit Colgate now and learn what happens and what you can do about it.
Read More




Adult Oral Care
Understanding Causes of Yellow Teeth
Explore yellow teeth causes from genetics to poor oral hygiene. Learn when to consult a dentist for yellow teeth.
Read More


Adult Oral Care
What is Referred Tooth Pain?
At times tooth pain may not be what it seems. A pain that originated elsewhere in the body may be felt in the teeth. Learn more about referred tooth pain.
Read More

Adult Oral Care
Hydrogen Peroxide and Oral Care Benefits
Hydrogen peroxide is a whitening agent, but it can also help kill bacteria that damage your gums. Learn how hydrogen peroxide gums treatment works, here.
Read More
Adult Oral Care
Taking Care Of Swollen, Bleeding Gums
When swollen, bleeding gums cause discomfort, there may be several reasons.
Read More
Adult Oral Care
What Causes A Swollen Gum Around One Tooth?
Explore the causes, symptoms, and remedies for swollen gums. Learn how to soothe discomfort and restore gum health effectively.
Read More
Adult Oral Care
How to Get Rid of White Spot Lesions on Teeth
Don't let discoloration keep you from smiling. Like most oral issues, figuring out how to get rid of white spots on teeth may be easier than you thought.
Read More
Adult Oral Care
Benefits of Mint for Oral Health and Overall Wellness
Discover how mint can transform your dental care routine! Explore its benefits for fresh breath, gum health, and overall oral hygiene
Read More
Adult Oral Care
Causes Of Brown Spots On Teeth
Brown spots on teeth may worry you, but there's plenty you can do to fix them. Your dentist can offer a solution based on the following causes.
Read More
Adult Oral Care
Chew on This: Ice Crunching and Your Teeth
While blenders and ice crushers are perfect for crunching ice cubes, teeth are not. Find the perfect alternative to ice crunching here!
Read More
Adult Oral Care
How To Find Relief for Abscessed Teeth
You're experiencing some serious pain in your mouth. Are there any home remedies for abscessed teeth that could help you?
Read More
Adult Oral Care
Is It Bad to Be a Mouth Breather? | Colgate®
Most people naturally breathe through their nose. But if you're a mouth breather, it's worth reviewing the causes, effects and treatments for this issue.
Read More
Adult Oral Care
Tongue Brush Vs. Toothbrush: Which Is Better?
A tongue brush or tongue scraper may provide a more thorough clean than most toothbrushes when it comes to the tongue. Why? Learn more, here.
Read More
Adult Oral Care
Black Gums: Symptoms, Causes, and Treatments
Discover the causes of black gums and learn effective treatments to restore the natural pink colour. Get expert tips on oral health and gum care here.
Read More
Adult Oral Care
What Causes Tooth Erosion?
Tooth erosion is a common dental concern. Knowing how to prevent tooth erosion can help your teeth stay strong and healthy!
Read More
Adult Oral Care
Coated Tongue: Symptoms, Causes, and Treatment
A coated tongue may be harmless. Learn what may be the cause and when you should see your dentist for an evaluation, here.
Read More
Adult Oral Care
What Causes Sour Tongue and How to Prevent it
Have you ever had a sour tongue or experience a metallic or bitter taste in your mouth? Find out the possible causes and preventing it from happening, here.
Read More
Adult Oral Care
Tongue Bacteria: Know What's Healthy (And What's Not)
Have you ever noticed a white film on your tongue? Here's what to look for when it comes to cleaning your tongue properly to have a good oral care routine.
Read More
Adult Oral Care
What is Oral Allergy Syndrome?
What is oral allergy syndrome? Learn about OAS including the signs, symptoms & more with Colgate®. Click here for the full article.
Read More
Adult Oral Care
Yellow Tongue: Symptoms, Causes, And Treatments
What does a yellow tongue signal? Read more for common symptoms, causes and treatment options for yellow tongue.
Read More
Adult Oral Care
Gum Stimulator: What Is It And How Do I Use It?
What is a gum stimulator and should you add one to your oral hygiene routine? Learn more, here.
Read More
Adult Oral Care
Blue Or Grey Teeth: Causes And Treatments
Gray or blue teeth may be natural, but it may also indicate problems needing professional attention. Visit Colgate now and learn the causes and treatments.
Read More
Adult Oral Care
Cheek Biting: What You Need To Know
There are a few reasons why people bite their cheeks and other areas inside the mouth. Visit Colgate now and learn more about cheek biting and how to stop it.
Read More
Adult Oral Care
Effect of Alcohol on Teeth - 3 Things to Know
Whether you prefer champagne to wine or mixed drinks to beer, be aware alcohol and teeth aren't natural allies. Learn more now at Colgate India.
Read More
Adult Oral Care
Dental Health Care: What Is It & What Does It Mean to You?
What exactly is dental health care, and what does it mean to you? Visit Colgate now and learn the main aspect of dental health care and why it's important.
Read More
Adult Oral Care
Excessive Saliva? What It Could Mean (and How to Deal)
Excessive saliva could be a clue about the state of your overall health. Are there ways you can deal with this condition? Learn more now at Colgate India.
Read More
Adult Oral Care
Is Gum Reshaping Right For You?
Gum contouring, involves changing the shape of your gums to be more aesthetically pleasing. Visit Colgate now and learn if this procedure is right for you.
Read More
Adult Oral Care
How To Strengthen Weak Tooth Enamel
While some damage to your enamel can’t be repaired on your own, there are steps you can take to protect it. Visit Colgate and learn how to strengthen enamel.
Read More
Adult Oral Care
The Dangers Of Using A Plaque Scraper At Home
Plaque removal is important for good oral health, but it's not a DIY project. Leave the plaque scraper to your dental hygienist. Learn more now at Colgate.
Read More
Adult Oral Care
What are The Signs of Dead Tooth?
Did you know that teeth can die? Visit Colgate now and learn more about why this happens, the signs your teeth are dying, and what your treatment options are.
Read More
Adult Oral Care
What Is a Salivary Stone?
Curious about the symptoms, risk factors and potential treatments for salivary stones? Visit Colgate now and learn all you need to know about salivary stones.
Read More
Adult Oral Care
What to Expect from Tonsil Removal
Even though tonsils are an important part of the body, sometimes a doctor will recommend tonsil removal. Learn more now at Colgate India.
Read More
Adult Oral Care
Can Tooth Enamel Be Restored?
Can you restore your tooth enamel? Visit Colgate India now and learn everything you need to know on the subject of tooth enamel restoration.
Read More
Adult Oral Care
When to Receive Gum Abscess Treatment
If you suddenly find that your gums are swollen or bleeding, or pain is reverberating through your jaw, you may have a gum abscess. Learn more now at Colgate.
Read More
Adult Oral Care
5 Pale Tongue Causes
If your tongue looks lighter than normal, it could be due to one of the 5 common pale tongue causes. Visit Colgate now and learn more the causes and treatments.
Read More



Oral Health Quiz
What's behind your smile?
Take our Oral Health assessment to get the most from your oral care routine.
Oral Health Quiz
What's behind your smile?
Take our Oral Health assessment to get the most from your oral care routine.




