All oral health articles
1987 results

Fluoride
What Is Stannous Fluoride Toothpaste?
Discover what is Stannous Fluoride Toothpaste and its importance to prevent cavities and other oral health problems.
Read More

Fluoride
What Is Fluoride? How It Works and Who Needs It
Fluoride is a naturally occurring mineral found in water, soil, and foods and is an important part of oral health that supports strong teeth for people of all ages.
Read More
Fluoride
The Benefits and Safety of Fluoride
Using fluoride as instructed and as recommended by dental professionals is one of the most effective and safe ways to support the health of your family’s smiles.
Read More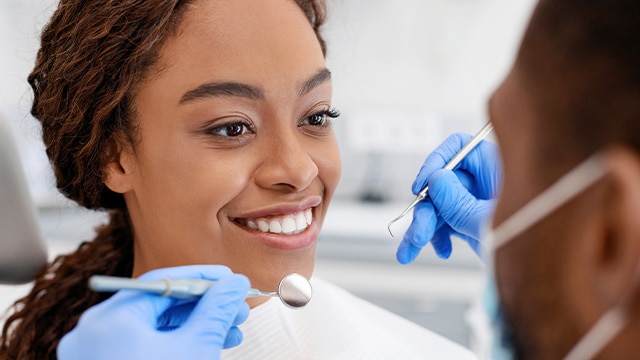
Fluoride
How Fluoride Protects Your Smile and Treatment Options
Fluoride remains one of the most trusted and effective ways to keep teeth strong. It’s a simple, trusted way to safeguard your smile for the long haul at every stage of life.
Read More
Bad Breath (Halitosis)
Natural Food Remedies For Bad Breath
Are you suffering from bad breath? If you are, here are some natural bad breath remedies to brighten your day.
Read More
Bad Breath (Halitosis)
Ammonia Breath And Associated Health Concerns
Bad breath may stem from factors you can control. Ammonia breath, however, may be a sign of a serious health condition. Learn more, here.
Read More
Bad Breath (Halitosis)
Bad Breath And Its Relationship To Oral And Systemic Diseases
Bad breath may be the result of something more serious, learn causes and how to resolve halitosis.
Read More
Bad Breath (Halitosis)
Bad Breath From Dry Mouth And How To Treat It
Learn how to combat dry mouth and bad breath with Colgate's expert advice, ensuring fresh breath and optimal oral health.
Read More
Bad Breath (Halitosis)
Bad Breath From Lungs: Oral Hygiene May Not Be The Cause
Have you ever suffered from bad breath and struggled to find a cause? It could be bad breath from lungs due to respiratory conditions. Find out more, here.
Read More
Bad Breath (Halitosis)
What To Do About Mothball Breath
Struggling with mothball breath? Discover causes and effective solutions for fresher breath, from oral hygiene tips to professional advice at Colgate.
Read More
Bad Breath (Halitosis)
Brushing Teeth To Boost Your Confidence
Brushing teeth is a regular part of everyone's morning and nighttime routine. Consider this routine task as an investment in yourself. Read more at Colgate.com Read more at Colgate.com
Read More.jpg)
Bad Breath (Halitosis)
Cure Your Toddlers Bad Breath With These 6 Healthy Snacks
If your toddler has bad breath, read up on some of these healthy snacks that can help remedy the stinky situation.
Read More
Bad Breath (Halitosis)
Effective Home Remedies For Bad Breath
Discover effective home remedies for bad breath on Colgate. Explore natural solutions to freshen your breath and improve oral health.
Read More
Bad Breath (Halitosis)
3 Foods That Cause Bad Breath and Tips to Fight It
There are many ways to combat bad breath and still enjoy the foods you love. Here are some foods that cause bad breath, and how to control or prevent them from affecting your oral hygiene.
Read More
Bad Breath (Halitosis)
Halitosis Treatment Options
Halitosis, or bad breath, treatment can be somewhat tricky, unless you figure out what's causing the problem in the first place....
Read More
Bad Breath (Halitosis)
Hormones and Bad Breath: What's the Connection?
Understand the link between hormonal changes and bad breath during pregnancy with expert insights and tips on Colgate's dedicated page.
Read More
Bad Breath (Halitosis)
How To Cure Bad Breath
Discover how to cure bad breath effectively with our expert tips. Learn the causes and simple remedies for fresh breath at Colgate. Perfect for those seeking solutions for bad breath.
Read More
Bad Breath (Halitosis)
How To Get Rid Of Garlic Breath
Fortunately, there are many things you can do to quickly get your breath under control. Here's how to get rid of garlic breath before an important event.
Read More
Bad Breath (Halitosis)
How To Tell If You Have Bad Breath
Knowing how to tell if you have bad breath can be tricky, because you can't identify it yourself. Nonetheless, there are a few things you can do to improve it if needed.
Read More
Bad Breath (Halitosis)
How To Treat Bad Breath In Teenagers
Bad breath is a common problem for teenagers. Learn more on the causes and treatment for bad breath and how to prevent it from happening again here.
Read More
Bad Breath (Halitosis)
Not At Home? How To Get Rid Of Bad Breath On The Go
Scoring fresh breath at home is simple, but knowing how to get rid of bad breath while you're out and about can be a bit trickier.
Read More
Bad Breath (Halitosis)
Dental Probiotics for Bad Breath: A Solution With Impressive Potential
New research shows using probiotics can be used to help bad breath. Learn more about the possibility of using good bacteria to your advantage.
Read More
Bad Breath (Halitosis)
Can A Sinus Infection Cause Bad Breath?
When it comes to a sinus infection, bad breath is often the first side effect as the sinuses drain into the back of your throat. Luckily, it is treatable.
Read More
Bad Breath (Halitosis)
The Best Mouthwash for Bad Breath: Key Ingredients to Look For
Discover the best mouthwashes for bad breath with Colgate’s expert guide. Learn the key ingredients to freshen breath and enhance oral health.
Read More
Bad Breath (Halitosis)
White Tongue and Bad Breath: Causes And Treatment
White tongue usually goes hand in hand with bad breath. Before examining the link between a white tongue and bad breath, here are some causes of white tongue.
Read More
Bad Breath (Halitosis)
Trimethylaminuria And The Fishy Odor
Bad breath may be caused by a genetic condition known as trimethylaminuria. Find out more about the causes of trimethylaminuria, treatment, and more.
Read More
Bad Breath (Halitosis)
Trouble With Tonsil Stones and Bad Breath
What's the deal with tonsil stones? Bad breath, irritation, and a whitish mark at the back of your throat are a few signs that you have a tonsil stone.
Read More
Bad Breath (Halitosis)
Using A Tongue Cleaner For A Cleaner Mouth
In addition to using a toothbrush to clean your teeth, you can improve your mouth's freshness by using a tongue cleaner.
Read More
Bad Breath (Halitosis)
What To Do About Chronic Bad Breath
If you have chronic bad breath, then you know how distressing this problem can be. Instead of temporarily masking the odor, find a solution!
Read More
Bad Breath (Halitosis)
Halitosis: Causes Of Bad Breath
Discover the leading causes of halitosis with Colgate. Learn how to prevent halitosis and maintain oral health.
Read More
Bad Breath (Halitosis)
Do Cavities Cause Bad Breath?
We've all had bad breath, and it can be embarrassing. But what's the underlying cause? Do cavities cause bad breath? Here are the answer and prevention.
Read More
Bad Breath (Halitosis)
Using a Halimeter: How Bad Is Your Breath, Really?
Let's face it: bad breath, or what your dentist calls halitosis, stinks. Here's how a device called the halimeter works to measure your breath odor.
Read More
Bad Breath (Halitosis)
What Is Perio Breath? The Connection Between Gum Disease and Halitosis
Everyone gets bad breath sometimes. But occasionally, bad breath can be a symptom of an underlying dental issue. Learn more about perio breath.
Read More
Bad Breath (Halitosis)
How To Manage Alcohol Breath
Drinking too much alcohol is bad news for your body and also for your breath. Find out how you can manage and get rid of alcohol breath, here.
Read More
Bad Breath (Halitosis)
How to Clean Your Tongue to Avoid Bad Breath
Cleaning your tongue can leave you feeling refreshed. Learn how cleaning your tongue can improve your breath and discover simple tongue cleaning techniques.
Read More
Bad Breath (Halitosis)
Morning Breath: Prevention, Treatment & Tips
Beat morning breath with expert tips on prevention and treatment. Discover simple steps for a fresh start every day.
Read More
Bad Breath (Halitosis)
Bad Breath From Stomach Problems? What It Means And How To Fix It
In fact, bad breath from stomach issues can be even more perplexing than typical bad breath, because it's harder to identify, isolate, and treat. Learn more.
Read More
Bad Breath (Halitosis)
5 Surprising Causes for Bad Breath in Children and What You Can Do About It
A toothbrush doesn't always cure bad breath in toddlers and children. Here are five surprising causes to consider.
Read More
Bad Breath (Halitosis)
Bad Breath: Causes & Treatments
Discover the causes and solutions for bad breath with Colgate's comprehensive guide. Learn about oral hygiene habits and treatments to freshen your breath.
Read More
Bad Breath (Halitosis)
How to Get Rid of Stress-Induced Bad Breath
Does your breath tend to get worse during anxiety-inducing situations? Can stress cause bad breath? Learn the tips and tricks that may be able to help you here.
Read More
Bad Breath (Halitosis)
The Unspoken Truth About Bad Breath: A Guide to Halitosis
By: Mandy Dennis
Registered Dental Hygienist
Read More
Cavities
10 Homemade Toothache Remedies
If a toothache strikes when you can’t see your dentist, you may feel desperate to relieve the pain. Try one of these 10 home remedies for toothache relief.
Read More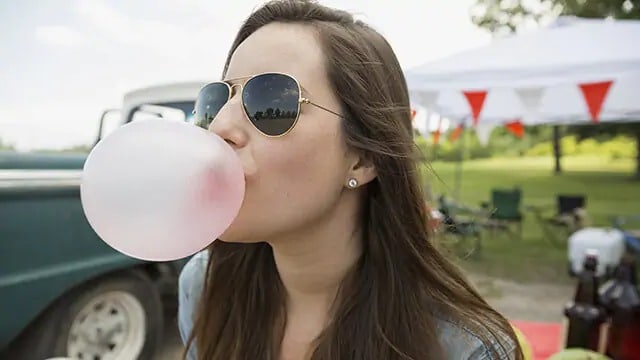
Cavities
Prevent Cavities: Tips for Sugar Lovers
Whenever food is consumed, the bacteria naturally found inside the mouth work to break it down, causing acid to develop. Read & learn more at Colgate.com.
Read More

Cavities
Can You Heal A Cavity At Home?
Can you heal cavity pain at home, without your dentist's help? Find out how catching cavities early is the key to healing them without an unpleasant treatment.
Read More
Cavities
How To Remineralize Your Teeth
Advertisements have flooded the dental market recently with products that claim to remineralize teeth. But are these items effective? Get your answers here!
Read More
Cavities
What Is a Caries Risk Assessment?
The key factor to stopping cavity formation is controlling the bacteria present in the mouth. Learn more about caries risk assessment here.
Read More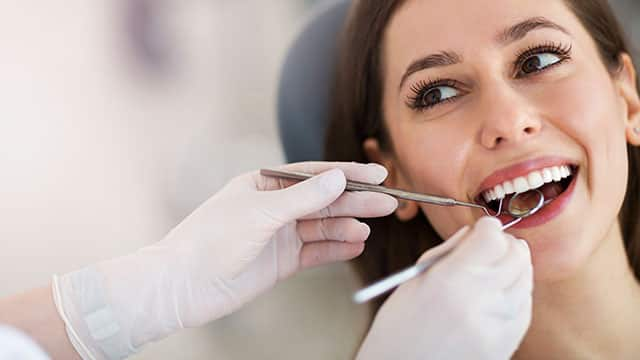
Cavities
Do Cavity Fillings Hurt?
Do cavity fillings hurt? They shouldn't, although you can expect some tenderness and soreness during the first few days after you get a tooth filled.
Read More
Cavities
Children And Tooth Decay: Three Bad Habits That Could Be Damaging
Children and tooth decay shouldn't go together, so make sure you're not unwittingly teaching your kids poor dental hygiene. Parents need to be on guard.
Read More
Cavities
Does A Tooth Worm Really Exist?
Once upon a time, dental patients believed a toothache was caused by a tooth worm eating away their tooth from the inside out. Do tooth worms really exist?
Read More
Cavities
Enamel Decay: How It Starts And How To Stop It
When lactic acid attacks the minerals in your enamel, it turns white – but unfortunately not the white you want. This is the first sign of enamel decay.
Read More


Cavities
Preventing Tooth Decay Disease
Explore effective strategies for preventing tooth decay disease on Colgate.com. Learn oral health tips to safeguard your smile. Visit us to learn more!
Read More
Cavities
Rampant Caries: What Are They?
Anyone of any age is susceptible to rampant caries, but luckily there are treatments that can restore your oral health. Find out more about rampant caries.
Read More
Cavities
Streptococcus Mutans: Where And How To Confront It
Many people know streptococcus mutans is the true culprit in the development of tooth decay and cavities. Learn more about streptococcus mutans, here.
Read More
Cavities
What Are Incipient Caries?
Incipient caries are the beginning stages of a cavity. Find out more about incipient caries and how you can stop them in their tracks and avoid the drill.
Read More
Cavities
What Are Sugary Drinks Doing to Your Teeth?
When it comes to keeping your family's teeth healthy, it's important to ensure they brush and floss, but it's just as important… Read more at Colgate.com
Read More
Cavities
What Are the Classes Of Cavities?
Explore our guide on cavities classification, diving into the various types, causes, and treatments. Your go-to resource for understanding cavities.
Read More
Cavities
What Does Sugar Do to Teeth?
Uncover the impact of sugar on your teeth with our informative guide. Learn about the effects of sugar on dental health, including cavities and gum issues.
Read More
Cavities
What Causes A Cavity On The Front Tooth?
If your child has a cavity on the front tooth or you have one yourself, you may be wondering why it happened and how your dentist might treat it.
Read More
Cavities
What Is A Gumline Cavity?
Did you know that cavities can form in the pits & grooves of the molars, between teeth, or even along the gumline. Learn more about gumline cavities here.
Read More
Cavities
What To Expect From A Tongue Biopsy | Colgate® Oral Care
Learn about what you can expect from a tongue biopsy, including how it's performed and the after-care.
Read More
Cavities
Your Guide to Tooth Decay Stages
Decay worsens over time, and more advanced tooth decay stages require more extensive treatments. If caught early on, you can stop decay in its tracks.
Read More
Cavities
Cavity Prevention
Pit and fissure cavity prevention can start right at home. Make sure to brush your teeth twice a day for at least two minutes each session.
Read More
Cavities
What Are Cavities?
Explore the causes, symptoms, and prevention of cavities or tooth decay with Colgate. Learn effective oral care tips for a healthier, cavity-free smile.
Read More
Cavities
What Causes Cavities? What You Need to know About Cavity Formation, Treatment, and Prevention
Discover the root causes of cavities and learn prevention methods. Explore insights on cavity formation and get tips for maintaining optimal oral health.
Read More
Cavities
Arrested Caries: What to Know About This Type of Dental Decay
Dental caries is the scientific term for cavities, and that cavities refer to areas of decay in teeth. Learn more about arrested caries at Colgate® Oral Care.
Read More
Cavities
What Is a Root Cavity and How Can You Prevent It?
The risk of developing cavities and tooth decay doesn't end once you become an adult. Find out what is a root cavity and how you can prevent it at Colgate®.
Read More
Cavities
What Is a Smooth Surface Cavity?
A smooth surface cavity is a type of cavity that appears on the sides of the teeth. Here's what you should know about this type of dental decay.
Read More
Cavities
What Should You Do About a Wisdom Tooth Cavity?
If you have a wisdom tooth cavity, you may be wondering if you should get the tooth extracted or filled. Here's what to consider.
Read More
Cavities
When Might You Need Antibiotics for a Toothache?
It's important to get treatment for tooth pain. In some cases, you may need antibiotics for a toothache. Here's what to know before seeing your dentist.
Read More
Cavities
Why a Homemade Tooth Filling Won't Fix Your Cavity
A homemade tooth filling may seem like an easy way to treat decay — however, only a trained dental professional can properly fill a cavity. Here's why.
Read More
Cavities
Five Ways to Reverse Tooth Decay
If your dentist has told you that you have cavities, it's time to start thinking about ways to reverse tooth decay. Visit Colgate.com to learn more.
Read More

Cavities
Dental Cavities: What You Should Know
Prevent cavities with Colgate, the world leader in dental health. Discover how to enjoy a happy, healthy smile for years to come. Visit us online.
Read More
Cavities
Watch Out for These Signs of a Cavity
You bite down and feel a slight twinge in your mouth. Learn all the signs and symptoms of a cavity and why maintaining dental appointments is essential.
Read More
Cavities
Too Much Drilling? Not All Early Tooth Decay Needs a Filling
Regular dental checkups are your best defense to spot tooth decay as early as possible so that non-drilling options are still in your scope of treatment.
Read More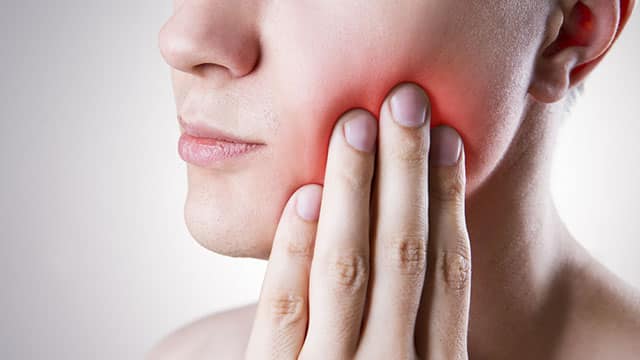
Cavities
What Does A Cavity Feel Like?
Your teeth might feel sensitive and you might feel some pain, especially after eating sweets, hot foods or cold foods. Learn more here.
Read More
Dry Mouth
4 Causes Of Sticky Saliva And Home Remedies
Wondering why you're suddenly experiencing sticky saliva? Here are some possible causes and home remedies to help you get your mouth back to normal.
Read More.jpeg)
Dry Mouth
Can Allergies Cause Dry Mouth?
Your allergies can cause dry mouth. Here's what to look for during allergy season and how to treat it to protect your oral health. Learn more, here.
Read More
.jpeg)
.jpeg)
Dry Mouth
Common Dry Mouth Causes In Adults
Persistent dry mouth, also called xerostomia, can be a cause for concern. Dry mouth causes often include medications, dehydration and medical conditions.
Read More
Dry Mouth
Dehydrated Tongue? What Your Mouth Is Telling You
A dry, dehydrated tongue isn't just a sign that your mouth is dehydrated; it's a sign that your entire body requires more fluids. Find out more, here.
Read More
Dry Mouth
Dry Mouth 101
Learn more about dry mouth and how it affects your oral health. Find information on the causes of dry mouth and how you and your dentist can treat it effectively.
Read More
Dry Mouth
Dry Mouth after Drinking Alcohol
If you've ever indulged in alcohol beverages, you've experienced dry mouth after drinking. Here's what that condition does to your oral health. Learn more.
Read More
Dry Mouth
Dry Mouth and Diabetes: Four Tips for Prevention
Dry mouth and diabetes often go hand in hand, but here are four tips for managing the problem.
Read More.jpeg)
Dry Mouth
Dry Mouth At Night: The Causes And Management Tips
Have you ever woken up from a sound sleep with a dry mouth at night? Dry mouth, or xerostomia, can be caused by a variety of conditions and habits.
Read More
Dry Mouth
Dry Mouth At Night? Why You Shouldn't Ignore The Symptoms
Dry mouth at night might seem like a harmless nuisance, but it could indicate deeper problems with your oral health. Learn more with Colgate.
Read More
Dry Mouth
Dry Mouth Products for Symptom Relief
Certain fluoride toothpastes, soft-bristled toothbrushes and alcohol-free mouthwashes can be the perfect dry mouth products for your condition.
Read More
Dry Mouth
Dry Mouth Treatment: How Your Dental Professional Can Help
Dry mouth can be uncomfortable, and the lack of saliva can attract oral bacteria. Make an appointment with your dentist, who can help cure the condition...
Read More
Dry Mouth
Dry Mouth Toothpaste 101: What Is It And How Does It Work?
Dry mouth toothpaste can stave off discomfort and potential health issues. Find out if dry mouth toothpaste can be the remedy for your dry mouth.
Read More
Dry Mouth
Essential Oils For Dry Mouth: Will They Help?
People turn to natural remedies for a whole host of mild conditions, but do essential oils for dry mouth work? Find out more keeping a hydrated mouth here.
Read More
Dry Mouth
Foamy Saliva: What Does It Mean?
What causes foamy saliva and what may it indicate about your overall health? Find out more, here.
Read More.jpeg)
Dry Mouth
How Alcohol-Free Mouthwash For Dry Mouth Provides Relief
A dry mouth can cause you a fair amount of discomfort. Fortunately, various types of toothpaste and mouthwash for dry mouth can treat your specific cause.
Read More
Dry Mouth
How Do Dry Mouth Lozenges Work?
Saliva plays an important role in keeping your mouth healthy. If you have dry mouth, dry mouth lozenges may help stimulate your saliva production.
Read More
Dry Mouth
How the Common Cold, Your Teeth, and Your Overall Oral Health Are Connected
The common cold, teeth and your oral health are more connected than you think. When dealing with sinus troubles, consider these remedies for oral issues.
Read More
Dry Mouth
How To Keep Your Salivary Glands Healthy
Your salivary glands, which produce saliva, play a critical role in not just your oral health, but your overall health. Learn how to keep them healthy.
Read More
Dry Mouth
Prescription Medications And Dry Mouth
Dry mouth or xerostomia is a condition that occurs when the salivary glands of a person do not function normally, resulting in inadequate secretion of saliva in the mouth.
Read More
Dry Mouth
Saliva Substitute For Dry Mouth Relief
Learn more about dry mouth and how it affects your oral health. Find information on the causes of dry mouth and how you and your dentist can treat it effectively.
Read More
Dry Mouth
Sjögren's Syndrome: Oral Signs and Symptoms
Sjogren's syndrome symptoms – including dry mouth, oral sores and dental decay – can be difficult to cope with. Learn more.
Read More
Dry Mouth
The Link Between Anxiety and Dry Mouth
Anxiety and dry mouth can be harmful, so reach out to your dentist if you suffer from them regularly. But can anxiety cause dry mouth? Learn more here.
Read More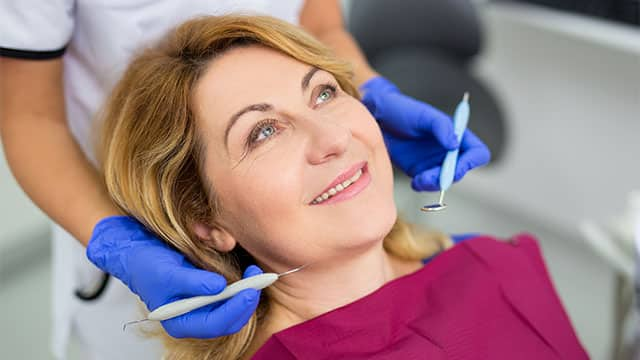
Dry Mouth
The Link Between Hormones and Dry Mouth
Dry mouth may be a result of menopause and can have an effect on your overall health. Find out more about you can deal with hormonal shifts and dry mouth.
Read More.jpeg)
Dry Mouth
Top Three Dry Mouth Causes And How To Cope
Dry mouth can affect anyone, but there are ways to fight back. By learning the top dry mouth causes, you can prevent it from getting the best of you.
Read More
Dry Mouth
What Can You Do About Chronic Dry Lips?
Chapped lips are a common condition, but knowing what causes chronic dry lips will help you understand what you can do to treat and soothe them.
Read More.jpeg)
Dry Mouth
What's Causing The Roof Of Your Mouth To Feel Dry?
From a sticky, uncomfortable palate to trouble chewing and swallowing, you may experience a few different things if you suffer from a dry roof of mouth.
Read More.jpeg)
Dry Mouth
What Causes Dry Mouth After Surgery?
Most cases of dry mouth after surgery are temporary. If the problem lingers, you may need to see a dentist. Check out these symptoms and treatments.
Read More.jpeg)
Dry Mouth
What Causes Dry Mouth And How Do You Alleviate It?
Dry mouth is an uncomfortable feeling that makes a drink of water sound like heaven. But what causes dry mouth? Well, it varies ...
Read More.jpeg)
Dry Mouth
What Is Cottonmouth?
What is cottonmouth? This condition occurs when your salivary glands don't make enough saliva to keep your mouth wet. Find out more about cottonmouth here.
Read More.jpeg)
.jpeg)
Dry Mouth
What Is Saliva And Why Is It Important?
What is saliva? You might be surprised to know that it contains much more than just water and serves a host of functions for your health! Learn more.
Read More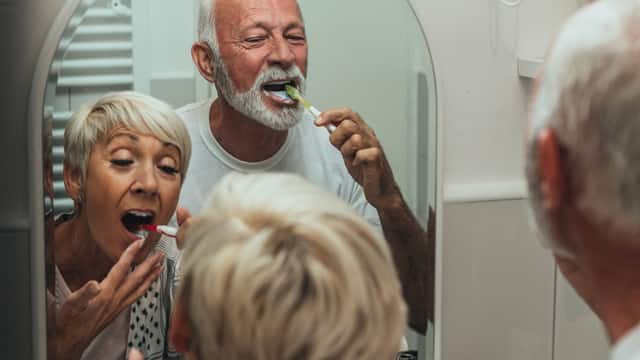
Dry Mouth
What to Do About CPAP Dry Mouth
If you use a CPAP machine for your sleep apnea, dry mouth can occur. Why does it happen and what can you do about dry mouth if it happens.
Read More
Dry Mouth
Does Dehydration Negatively Impact Your Oral Health?
Staying hydrated is important for both your body and oral health. Learn how dehydration from exercise or heat exposure can put your oral health at risk.
Read More
Dry Mouth
How To Handle A Dry Mouth And Throat
Your allergies can cause dry mouth. Here's what to look for during allergy season and how to treat it to protect your oral health. Learn more, here.
Read More
Dry Mouth
What Can You Do About Chronic Dry Lips?
Even if you keep water close by to sip at night, dry mouth, or xerostomia, can still creep in. Here's how you can manage your dry mouth effectively.
Read More
Dry Mouth
The Facts About Dry Mouth
Dry mouth is a frustrating problem that can be all too common for people with certain lifestyles, medications, and health conditions. But what exactly causes dry mouth? What are its symptoms?
Read More
Dry Mouth
Dental Effects of Constant Dry Mouth
If you're suffering from constant dry mouth, knowing the cause and how to find relief can go a long way to preventing more serious dental complications.
Read More
Dry Mouth
10 Home Remedies for Dry Mouth
Dry mouth can develop for many reasons: medications, nutritional deficiencies, stress, cancer treatment, and even some systemic diseases. Learn how to help dry mouth here.
Read More
Dry Mouth
How to Treat Dry Mouth
Deciding how to treat dry mouth often depends upon its root cause. There are multiple causes and various methods of treatment. Learn more with Colgate.
Read More
Wisdom Teeth
5 Possible Wisdom Teeth Removal Complications
Here are five of the most common complications with wisdom teeth removal to help you jump-start a discussion with your dentist.
Read More
Wisdom Teeth
Broken Wisdom Tooth Treatment Options
Teeth do occasionally chip or break. Learn more about a broken wisdom tooth, causes, and what your treatment options are if your wisdom tooth breaks.
Read More
Wisdom Teeth
Can Wisdom Teeth Grow Back After Extraction?
Can wisdom teeth grow back? Not really, but some people have more than just the standard four.
Read More
Wisdom Teeth
Common Wisdom Teeth Problems And Smart Solutions
When wisdom teeth problems arise, dentists often recommend removing them, and there are a few reasons this may be the smartest thing to do.
Read More
Wisdom Teeth
Coronectomy: An Alternative To Wisdom Teeth Extraction
A standard wisdom teeth removal isn't right for some patients. Sometimes a coronectomy is required. Read on to learn more about this procedure.
Read More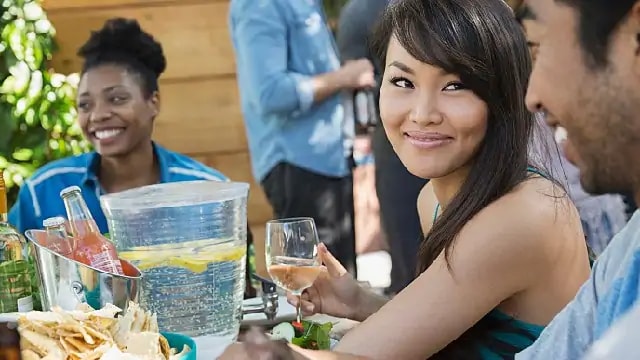
Wisdom Teeth
Drinking After Wisdom Teeth Removal: Do's And Don'ts
If you're wondering about drinking after wisdom teeth removal, keep in mind tooth extraction and alcohol don't always mix. Here's how you can still imbibe.
Read More
Wisdom Teeth
Dry Socket Paste: Is It Worth Trying?
Visit your dentist right away if you have a dry socket, and he or she may relieve your pain with a dry socket paste. Learn more about it, here.
Read More
Wisdom Teeth
Infected Wisdom Tooth: What Your Options Are
Impaction isn't always the only reason for removal. An infected wisdom tooth can also land you in this common form of oral surgery. Find out more, here.
Read More
Wisdom Teeth
What Is an Operculectomy?
An operculectomy is a minor surgical procedure to remove excess gum tissue covering a partially erupted tooth, which in most cases is a wisdom tooth.
Read More
Wisdom Teeth
Using Tea Bags After Wisdom Teeth Removal
Did you know minor wisdom teeth bleeding may be relieved with this surprising pantry staple? Click here to learn more about teabags remedy with Colgate.
Read More
Wisdom Teeth
Tooth Swelling: Causes And How To Relieve Discomfort
The causes of tooth swelling can be numerous. Whatever the cause, it can be a serious issue that is often the result of bacterial infection.
Read More
Wisdom Teeth
What Age Do Wisdom Teeth Come In?
If you and your teen are maintaining your regular dental appointments, you'll be in good stead to track that the wisdom teeth are erupting healthily or catch if they need intervention.
Read More.png)
Wisdom Teeth
What Is A Wisdom Tooth?
Learn more about wisdom teeth from Colgate. Find out what wisdom teeth are, common infections, impacted wisdom teeth, and if you should have your wisdom teeth removed.
Read More
Wisdom Teeth
What To Eat After Wisdom Teeth Removal
Hearty and equally soft foods like scrambled eggs, soft fish, finely cut meats, mashed potatoes, oatmeal and thin soups can keep you feeling fuller for a longer amount of time.
Read More
Wisdom Teeth
What Does Wisdom Tooth Extraction Cost?
Numerous factors can determine how tooth extraction and type of anesthesia will affect your budget, so your dentist or oral surgeon will be there to evaluate your mouth and guide you.
Read More
Wisdom Teeth
Wisdom Teeth 101
Learn more about wisdom teeth from Colgate. Find out what wisdom teeth are, common infections, impacted wisdom teeth, and if you should have your wisdom teeth removed.
Read More
Wisdom Teeth
Wisdom Teeth Anesthesia Options
Learn more about wisdom teeth from Colgate. Find out what wisdom teeth are, common infections, impacted wisdom teeth, and if you should have your wisdom teeth removed.
Read More
Wisdom Teeth
Wisdom Teeth Symptoms That Indicate Time Extraction
Have you ever felt like you were teething as an adult? It was probably in the back of your mouth, and the swelling you felt there was really a tooth trying to erupt.
Read More
Wisdom Teeth
Wisdom Teeth Pain Relief: How To Find Comfort
Learn more about wisdom teeth from Colgate. Find out what wisdom teeth are, common infections, impacted wisdom teeth, and if you should have your wisdom teeth removed.
Read More
Wisdom Teeth
Tips for Preventing and Treating Dry Socket
The true pain from having a tooth pulled comes from developing a dry socket (alveolar osteitis). Learn more about dry sockets here.
Read More
Wisdom Teeth
Impacted Tooth: Wisdom Teeth Pain
An impacted tooth is a tooth that gets blocked as it is pushing through the gum into your mouth. Learn more about this here.
Read More
Wisdom Teeth
How to Sleep After Wisdom Teeth Removal: 4 Post-Procedure Tips
After any surgery, sleeping can be difficult. Here are some tips for how to sleep after wisdom teeth removal.
Read More
Wisdom Teeth
Pericoronitis Treatment: How To Clear This Wisdom Tooth Infection
Erupting wisdom teeth can cause problems, including pericoronitis, but your dentist can offer pericoronitis treatment. Learn more about what this entails.
Read More
Wisdom Teeth
What Is An Operculum?
Wisdom tooth eruption can be tedious and troublesome. An operculum, or flap of tissue over the tooth, is one related problem that's treatable. Learn how.
Read More
Wisdom Teeth
What Is The Recovery Time After Wisdom Teeth Removal?
How long is wisdom teeth recovery time? When will you be back to chewing crunchy carrots and apples with ease? Learn more here!
Read More
Wisdom Teeth
How To Get Food Out Of Wisdom Teeth Holes
Getting food stuck in your wisdom teeth holes? Click here for all the information you need to keep your new wisdom teeth holes health & clean with Colgate ®.
Read More
Wisdom Teeth
Smoking After Wisdom Teeth Extraction
Smoking after getting a wisdom teeth extraction is a bad idea. Learn the complications smoking can cause after your wisdom teeth have been pulled.
Read More
Wisdom Teeth
Recovery After Wisdom Teeth Removal
How long is wisdom teeth recovery time? When will you be back to chewing crunchy carrots and apples with ease? Learn more here!
Read More
Wisdom Teeth
What Is Pericoronitis?
Your wisdom teeth (third molars) usually start to erupt (enter your mouth) during the late teen years. Sometimes, there's not enough room for them.
Read More
Wisdom Teeth
Should You Have Your Wisdom Teeth Removed?
For most people, it is a matter of when to get your wisdom teeth removed, not whether or not you should. However, for those who are unsure about whether they should, find your answers here.
Read More
Wisdom Teeth
Wisdom Tooth Extraction
A wisdom tooth extraction is a surgical procedure to remove one or more of your wisdom teeth. Learn what to expect, before during and after the surgery.
Read More
Mouth & Teeth Anatomy
3 Fun Facts About Teeth
People today know a lot about their oral health, but that wasn't always the case. Find out what our ancestors believed about teeth with these fun teeth facts.
Read MoreMouth & Teeth Anatomy
4 Possible Causes Of Salivary Gland Pain
You probably don't give your salivary glands much thought unless you're experiencing dryness in your mouth or pain involving one of your glands. Several health problems can cause salivary gland pain — some more serious than others. Should you ever experience this kind of pain, you'll want to be informed on the kinds of issues that can affect your glands, how these conditions can be treated and what you can do to keep your glands healthy.
Read MoreMouth & Teeth Anatomy
A Breakdown Of Tongue Anatomy
What are the different parts of the human tongue? Find a detailed breakdown of the anatomy of the human tongue and what each part does for you, here.
Read MoreMouth & Teeth Anatomy
About Cementoblastoma: Development & Treatment
A cementoblastoma is a benign growth that appears on the tooth root. Learn more about it, plus how dentists treat it here.
Read More
Mouth & Teeth Anatomy
About Cementum: Function, Types & Role In Tooth Sensitivity
Cementum is the connective tissue that forms along a tooth's root and helps solidify it by connecting to fibers that support the tooth's place in the jawbone.
Read More
Mouth & Teeth Anatomy
Adults with Baby Teeth: Causes and Treatment
Adults with baby teeth might not even know that their primary teeth are still in their mouth. Learn causes of retained teeth & when is treatment necessary.
Read More
Mouth & Teeth Anatomy
All About the Apical Foramen
What's an apical foramen? This junction between tooth pulp and the rest of the body is crucial for a successful root canal procedure. Learn more today.
Read More
Mouth & Teeth Anatomy
All About the Dental Arch
The shape of your dental arch helps determine whether your teeth are aligned or not. Learn about your options for correcting a misaligned bite.
Read More
Mouth & Teeth Anatomy
All About the Hard Palate
Your mouth is more than just the teeth, tongue and gums. Learn about diseases and conditions that can affect the hard palate.
Read More
Mouth & Teeth Anatomy
All About the Mandibular Nerve
The mandibular nerve helps you feel in many areas in your lower mouth. Your dentist may apply a nerve block to it before a dental procedure. Learn more.
Read More
Mouth & Teeth Anatomy
Alveolar Process: Anatomy, Features And Importance
The alveolar process is the bone that surrounds your teeth. Learn more about how it functions in your mouth and why it's important for your oral health.
Read More
Mouth & Teeth Anatomy
Anatomy Of The Occipitofrontalis And Its Role In Headaches
Many muscles control your facial expressions, but there is one that is responsible for raising your eyebrows: the occipitofrontalis. Learn how it works.
Read More
Mouth & Teeth Anatomy
Are Teeth Bones?
Teeth are strong and white, just like bones. They also store a lot of calcium, just like bones. But are teeth bones? Find out more, here.
Read More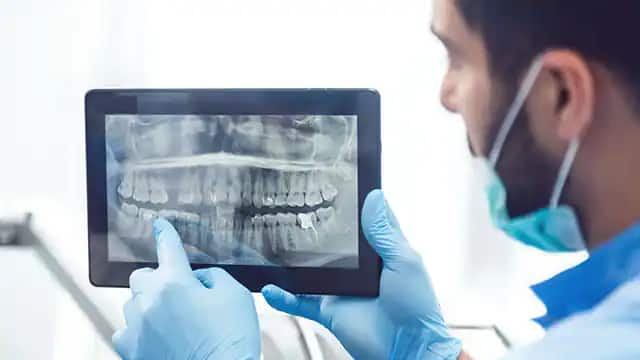
Mouth & Teeth Anatomy
Bone Resorption: Why It Happens And What To Do Next
Bone resorption is part of a complex biological process that can result in shrinkage or loss of bone. Here's how it may affect your mouth.
Read More
Mouth & Teeth Anatomy
Buccal Exostosis: Causes, Treatment And Care
A buccal exostosis is benign, but home care tips may ensure your mouth and gums stay healthy. Learn more.
Read More
Mouth & Teeth Anatomy
Can You Make a Cloverleaf Tongue?
Can you twist your tongue into a cloverleaf tongue? If so, you have a talent that many people don't have. Learn more about this unique talent.
Read More
Mouth & Teeth Anatomy
Can You Regrow Teeth With Coconut Oil?
Is it possible to regrow teeth with coconut oil? Learning how your enamel works can help you understand the answer and sort out fact from fiction.
Read More
Mouth & Teeth Anatomy
Circumvallate Papillae: Tastebuds, Function, and Complications
Circumvallate papillae are key to enjoying the taste of your favorite foods. Learn more about this extraordinary taste bud, here.
Read More
Mouth & Teeth Anatomy
Common Issues With Cryptic Tonsils And What To Do
When the folds in your tonsils gather debris, you can develop tonsil stones or tonsillitis. Here's what to do if you have issues with your cryptic tonsils.
Read More
Mouth & Teeth Anatomy
Congenitally Missing Teeth: What Are They and How to Treat Them
Congenitally missing teeth can affect the way your smile looks and how teeth work. A dentist can offer remedies to keep your mouth healthy. Learn more.
Read More
Mouth & Teeth Anatomy
Craze Lines on Your Teeth Making You Crazy? Here's What You Need to Know
Craze lines are tiny cracks that appear on the enamel or outside covering of the teeth. If you notice these cracks, should you be concerned?
Read More
Mouth & Teeth Anatomy
Diagnosing An Odontogenic Cyst And Getting Treatment
An odontogenic cyst is a cyst that occurs in the jaw during tooth development. Learn more about these cysts and how they're treated.
Read More
Mouth & Teeth Anatomy
Do You Have A Cusp Of Carabelli?
The cusp of carabelli is a non-functioning mini cusp that forms on some upper permanent first molars. Learn more about this here.
Read More
Mouth & Teeth Anatomy
Excessive Drooling: What's Normal?
Excessive drooling can be attributed to poor mouth and tongue control and inadequate swallowing due to many factors. Learn more here.
Read More
Mouth & Teeth Anatomy
Are Bony Growths in Your Mouth a Cause for Concern?
Exostosis mouth is a term used to describe an overgrowth of calcified bone in the oral cavity. The condition is not only benign, but also uncommon and very rarely requires any treatment.
Read More
Mouth & Teeth Anatomy
Extra Teeth? Tips To Smile More Confidently
In today's culture, you're bombarded with images of perfect smiles, but don't let your extra teeth get you down. Smile confidently with your extra teeth!
Read More
Mouth & Teeth Anatomy
Facial Nerve Anatomy
The facial nerve controls taste sensation and the muscles of expression. Here's how the nerve works and the problems that may affect it.
Read More
Mouth & Teeth Anatomy
4 Rare Teeth Conditions Parents Should Know About
Children should be screened early to see if they show signs of future teeth problems. Find out more about teeth problems, including unusual teeth problems, here.
Read More
Mouth & Teeth Anatomy
Frenums And Frenectomy
What happens if the tissue impairs oral function? A procedure called a frenectomy may be the answer. Click here to learn more about frenectomy with Colgate.
Read More
Mouth & Teeth Anatomy
Fungiform Papillae and Your Tongue
What are fungiform papillae? How do they help you taste your favorite flavors and what can hinder their important job? Learn more here.
Read More
Mouth & Teeth Anatomy
Granulation Tissue and Healing Oral Wounds
When wounds occur inside the mouth, the body begins healing. Granulation tissue plays an important role in this process. Find out more here.
Read More

Mouth & Teeth Anatomy
How Hypercementosis Affects A Tooth's Roots
Hypercementosis is a condition that affects the outer covering of a tooth's root. It results in a misshaped root and tends to develop in older patients.
Read More
Mouth & Teeth Anatomy
How To Build Strong Teeth
Strong teeth are healthy teeth, and the path to healthy teeth includes both eating the right foods and caring for your teeth. Learn more about strong teeth, here.
Read More
Mouth & Teeth Anatomy
How to Get Rid of a Dry Throat
Wondering how to get rid of a dry throat? Learn about some of the common causes, including allergies, dehydration, the common cold and more.
Read More
Mouth & Teeth Anatomy
How To Survive The 'Losing First Tooth' Milestone Healthily
After your child loses their first, however, be sure to include these steps in caring for the empty socket prior to the permanent tooth's eruption.
Read More
Mouth & Teeth Anatomy
How Your Levator Anguli Oris Helps You Form A Smile
The levator anguli oris is one of the keys to unlocking your smile. Learn how this muscle works and what conditions may affect its ability to function.
Read More
Mouth & Teeth Anatomy
How Your Palatine Tonsil Helps Guard Your Mouth
We are each born with a palatine tonsil in the back of our mouths. Here's what you need to know about this important structure.
Read More
Mouth & Teeth Anatomy
Inferior Alveolar Nerve (IAN): Causes and Symptoms of Damage
The inferior alveolar nerve (IAN) is very important to the mouth and its several functions. Here's all you need to know about this nerve.
Read More
Mouth & Teeth Anatomy
7 Amazing Facts You Didn't Know About Your Tongue
Your tongue helps in eating, digestion and speech. Check out these other facts about your tongue you probably didn't know.
Read More
Mouth & Teeth Anatomy
Jagged Teeth: Causes and Treatment
Wondering how to fix jagged teeth? Learn about what your dentist can do to fix chips, breaks and naturally uneven teeth. Learn more here.
Read More
Mouth & Teeth Anatomy
Let's Talk Tongue Muscles!
Bet you didn't know that your tongue muscles are similar to the tentacles of an octopus. Learn about this and more fun facts about the human tongue, here!
Read More
Mouth & Teeth Anatomy
Let's Think About The Mentalis Muscle
Muscles control every move you make. When you pout or stick out your lower lip, you have the mentalis muscle to thank.
Read More
Mouth & Teeth Anatomy
Lip Biting: Why It's Bad And How To Stop
Chronic lip biting is actually a bad habit for your oral health. You should discuss the issue with your dentist or here are several options that can help you eliminate lip biting.
Read More
Mouth & Teeth Anatomy
Maxillary Teeth: Characteristics And Evolution
Your maxillary teeth – which include your top incisors, canines, premolars and molars – can have a significant effect on your sinus cavities. Learn more.
Read More
Mouth & Teeth Anatomy
Mesial Tooth and Correcting Surface Gaps
What is a mesial tooth? What does it mean to have a mesial tooth gap? Should you leave it or talk to an orthodontist? Learn more about your options here.
Read More

Mouth & Teeth Anatomy
What Is Myofunctional Therapy?
When diagnosed, an abnormal tongue position can be corrected with myofunctional therapy, a special training process that ensures a future of good health.
Read More
Mouth & Teeth Anatomy
Occlusal Surface, Wear, Protecting Your Teeth
A tooth's occlusal surface plays a big role in your everyday life and is susceptible to wear and tear. Luckily there are ways to protect your teeth.
Read More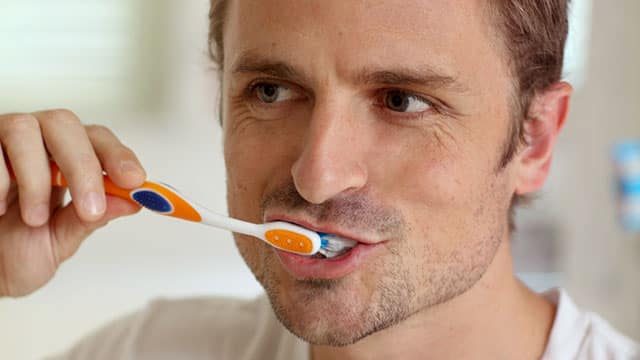
Mouth & Teeth Anatomy
Odontoblasts: What They Are And How To Keep Them Healthy
The odontoblast is a living specialized cell that forms the dentin, a hard component of the tooth that surrounds the dental pulp. Learn more here.
Read More
Mouth & Teeth Anatomy
Oral Bacteria: What Lives In Your Mouth?
You can't see them, feel them or taste them, but your mouth is home to entire colonies of microorganisms. Learn more about oral bacteria in your mouth, here.
Read More
Mouth & Teeth Anatomy
Orbicularis Oris: The Muscle For Puckering Up
The orbicularis oris is also referred to as the kissing muscle because of its role in puckering the lips. Learn more about its functions.
Read More
Mouth & Teeth Anatomy
Palatal Tori: Causes and Treatment
Palatal tori are benign growths that occur on the palate or roof of your mouth. Learn more here.
Read More
Mouth & Teeth Anatomy
Parotid Papilla Gland: Structure And Function
The parotid papilla is part of the papilla gland. It's important for producing saliva and keeping your mouth and teeth in good health. Learn more, here.
Read More
Mouth & Teeth Anatomy
Parts of the Mouth and Their Functions
The mouth, or oral cavity, is made up of several components that work together so you can breathe, speak, and eat. Learn more about the parts of your mouth.
Read More
Mouth & Teeth Anatomy
Periodontal Ligament: What Is It?
What is the periodontal ligament and why is it important to your overall oral health? Learn more, here.
Read More
Mouth & Teeth Anatomy
Pink Tongue? How Tongue Color Can Give Clues About Oral Health
A pink tongue may be an indicator of your oral health. Find out more about tongue colors, a pink tongue, and what it can say about your oral health.
Read More
Mouth & Teeth Anatomy
Preparing For Your Baby's First Molar
Watching your baby's teeth develop is an exciting milestone, but it can also be an overwhelming time for a parent. What can you expect from a first molar?
Read More
Mouth & Teeth Anatomy
Primary Molars Coming In? How To Help Your Child Through It
Molars coming in at this age might feel like a bigger hurdle in your child’s oral development. Luckily, there are things you can do to help them.
Read More
Mouth & Teeth Anatomy
Salivary Glands: How They Protect Your Oral Health
Probably one of the most overlooked parts of your digestive system are the salivary glands, but they play such an important role to your oral health.
Read More
Mouth & Teeth Anatomy
Submandibular Gland: Location, Function, and Complications
The submandibular gland is one of three types of gland that supply the mouth with saliva. Learn more about the submandibular gland, here.
Read More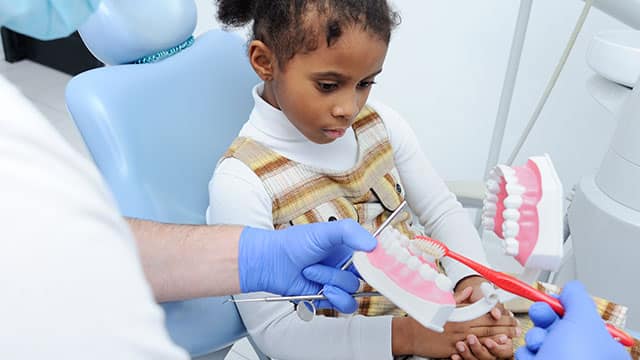
Mouth & Teeth Anatomy
Teeth And Tongue: Fun Ways To Teach Kids About Mouth Anatomy
Although teeth usually start the oral health show in your home, it doesn't do well to ignore the other parts of your child's mouth when learning how to stay healthy. After all, oral health also depends on keeping a healthy body, choosing the right foods and even ensuring the gums stay healthy as well.Mouth anatomy is about more than just teeth, and the more your child learns about the role his or her entire mouth plays on body health, the easier it is to promote good oral hygiene. Here are a few activities you can do together when talking about whole mouth health.
Read More
Mouth & Teeth Anatomy
The Glossopharyngeal Nerve Explained
For some cranial nerves, the name tells us the function. The prefix "glosso-" means relating to the tongue, and the suffix "-pharyngeal" means relating to the pharynx, or throat. Therefore, the glossopharyngeal nerve, also known as the ninth cranial nerve, has a role in both sensation and movement of the tongue and the throat. Learn what this important nerve does for your oral cavity.
Read More
Mouth & Teeth Anatomy
The Hypoglossal Nerve: The Brain Behind the Tongue
If you're concerned about a weakness or paralysis you've recently noticed in your tongue, or if you're just curious about the nerves that make up this unique muscular organ, you may come across the term "hypoglossal nerve."
Read More
Mouth & Teeth Anatomy
The Lingual Artery: The Tongue's Blood Supplier
If you've ever bitten or cut your tongue, you may have been surprised to see that it bled. Cuts inside the mouth, including on the tongue, can bleed due to the rich blood supply to these tissues. The tongue's blood supply comes from a large blood vessel called the lingual artery.
Read More
Mouth & Teeth Anatomy
The Role of Keratinized Tissue in Dental Implants and Healthy Teeth
Looking to address the gaps in your smile? Dental implants can provide both functional and cosmetic benefits.
Read More
Mouth & Teeth Anatomy
The Role of the Uvula
The mouth is one body part that receives constant attention. Breathing, eating and speaking would be impossible without every part working together. One of those mouth parts, the uvula, might not get as much attention as your teeth or tongue, but it's just as important.
Read More
Mouth & Teeth Anatomy
All About Premolars
Premolars, also called bicuspids, are the permanent teeth located between your molars in the back of your mouth and your canine teeth (cuspids) in the front. They are transitional teeth, displaying some of the features of both canines and molars, that help cut and move food from the front teeth to the molars for chewing. There are four premolar teeth in each dental arch - upper and lower.
Read More
Mouth & Teeth Anatomy
Tongue Coating: Too Much, Too Little And Just Right
Talking about your tongue coating might not be a popular topic of conversation in polite company, but it is a topic you should raise with your dentist. That coating is key to oral health as saliva helps wash away food particles and germs that could cause gingivitis and cavities, as well as initiating the digestive process by starting the breakdown of food. Saliva is great – that is, until you notice that you have too much or too little. Read on to learn what different amounts of coating on your tongue could mean for your overall health and wellness.
Read More
Mouth & Teeth Anatomy
Tongue Disease: 3 Conditions That May Affect Your Tongue
The tongue is an organ you may not give much thought to until it looks or feels funny. You may jump to a conclusion that you've contracted a tongue disease, though what you may have is an underlying condition that affects your tongue. If you exclude any form of trauma to the tongue, it still leaves a substantial number of congenital, acquired and autoimmune conditions that may cause potential tongue problems.
Read More
Mouth & Teeth Anatomy
Tongue Functions 101: Anatomy, Uses & Care
The mouth is a busy place: speaking, breathing, chewing, drinking. While the teeth might be the all-stars of the mouth (Let's face it, you notice when someone has a shiny white smile or, unfortunately, when they need some dental work.), don't forget about the tongue. The tongue does all the thankless grunt work. In fact, tongue function is involved in quite a few mouth maneuvers.
Read More
Mouth & Teeth Anatomy
Tooth Anatomy: Know The Parts Of Your Teeth
Have you ever wondered what makes up a tooth? Each part of a tooth has unique functions and properties. Aetna's Simple Steps to Better Dental Health lists major parts of tooth anatomy, including enamel, dentin, cementum, root(s) and the root canal chamber(s) inside the tooth. Damaged teeth, especially teeth with cracked or eroded enamel, are very susceptible to cavities. Advanced gum disease, another oral health condition that threatens tooth health, attacks the bone of the teeth and may cause tooth loss. Understanding the function of each part of a tooth and the steps required to keep teeth healthy with home care and regular checkups are important components of oral health education for you and your family.
Read More
Mouth & Teeth Anatomy
Torus Mouth: What's That Oral Growth?
If you can feel a bony protrusion on the roof of the mouth or on the inside of your lower jaw, you might be alarmed. However, a bony growth in the mouth, called a torus, is typically benign. According to the Cleveland Clinic, about 26 percent of the population have tori on the roof of their mouth, called palatal tori, or floor of their mouths, called mandibular tori.
Read More
Mouth & Teeth Anatomy
Torus Palatinus: Causes, Complications And Treatment
The palate or roof of your mouth is a bony structure overlaid with soft tissue. You use it to form certain sounds when speaking and to help chew and swallow. In most people, the palate is concave and smooth, and it remains that way all their lives. However, sometimes nodules (bony growths) may appear along the center line of the palate due to a condition called torus palatinus. While the nodules may look concerning, they are generally nothing to worry about.
Read More
Mouth & Teeth Anatomy
Treatment for Lingual Nerve Injury
What is your lingual nerve? Here's all you need to know about the lingual nerve, LN injury symptoms, and what you can do if it is injured.
Read More
Mouth & Teeth Anatomy
Treatment Options For Overjet
If your two front teeth extend out noticeably over your bottom ones, this is what is known as an overjet. You may be self-conscious about your appearance, particularly if you have endured any unwelcome descriptions of your front teeth, such as "buck teeth." If your child has the condition, you may be thinking about pursuing treatment so they can avoid social stigma in the future.Though the condition is not necessarily a health problem, and many people feel no need to fix it, there is a host of treatment options available. Here's what causes the condition and what your dentist or orthodontist may suggest to treat it.
Read More
Mouth & Teeth Anatomy
Types Of Abnormal Tongues And What They Look Like
The tongue might not be something you think about all that often, but what if you have an abnormal tongue? What does it look like? Find out more, here!
Read More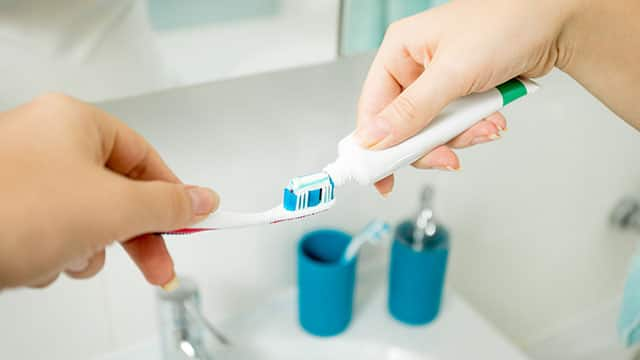
Mouth & Teeth Anatomy
Understanding Enamel Rods and Their Function
If you were to look at your teeth under a microscope, you'd see that their surface is covered by tiny enamel rods. Learn more about what they are.
Read More
Mouth & Teeth Anatomy
Understanding Teeth Structure
Teeth have lots of nicknames: pearly whites, chompers, chicklets. But no matter how you refer to them, don't forget their importance. Teeth perform several functions. In addition to chewing food for digestion, they also assist with word pronunciation while providing shape to the face. Learning about teeth structure is just as important when it comes to maintaining good oral care.
Read More
Mouth & Teeth Anatomy
Von Ebner Glands: What Do They Do?
Did you know that saliva helps us digest, taste, speak, and even protects our tooth enamel by breaking down acids from food?
Read More
Mouth & Teeth Anatomy
What's an Eye Tooth?
Without knowing exactly what "eye teeth" are, have you ever started a sentence exclaiming your wish for something valuable with "I'd give my eye teeth for …"?
Read More
Mouth & Teeth Anatomy
What Are Dentin Tubules?
Have you heard of the term dentin tubules? Well, now you have. Dentin tubules are a vital part of your teeth. As you may know, the teeth are made up of tissue layers, and each one serves a unique function. The dentin tubules are located in the dentin, one of the layers below the enamel surface. The role of dentin tubules is to help you feel sensations in your teeth. That's also why they're often blamed for hypersensitivity in people's teeth.
Read More
Mouth & Teeth Anatomy
What Are Filiform Papillae?
Look closely at your tongue. See all those little tiny dots? The majority of those dots are called filiform papillae. Learn more here.
Read More
Mouth & Teeth Anatomy
What Are Foliate Papillae?
Hundreds of tiny bumps called papillae cover your tongue, most of which contain taste buds with sensory cells. There are four types of papillae—filiform, fungiform, circumvallate, and foliate—and each has a role to play. This article looks into the foliate papillae, which are located on the sides of the tongue and contain taste buds.
Read More
Mouth & Teeth Anatomy
What Are Mandibular Tori?
Do you feel any hard bumps in your mouth? Those bumps are most likely harmless growths of extra bone called tori. Learn more about mandibular tori, here.
Read More
Mouth & Teeth Anatomy
What Are Primary Teeth?
The eruption of a baby's first tooth is a special moment. Young children develop 20 primary teeth altogether, and by adulthood 32 permanent teeth have taken their place. But why do you need two sets of teeth?
Read More
Mouth & Teeth Anatomy
What Causes A Tingling Tongue?
This tingling feeling, known as paresthesia, often occurs in the hands and feet. But did you know it can also occur in other body parts, including the tongue? Let's go over the potential causes of a tingling tongue and when you should see a medical or dental professional about your symptoms.
Read More
Mouth & Teeth Anatomy
What Causes Tongue Spasms?
You may never have heard of tongue spasms, but this little-known issue can occur at any age as part of a condition known as lingual dystonia. "Dystonia" refers to any involuntary muscle contraction, and "lingual" means having to do with the tongue. Read on to find out how spasms might occur, how they can be treated and how they are prevented from reoccurring.
Read More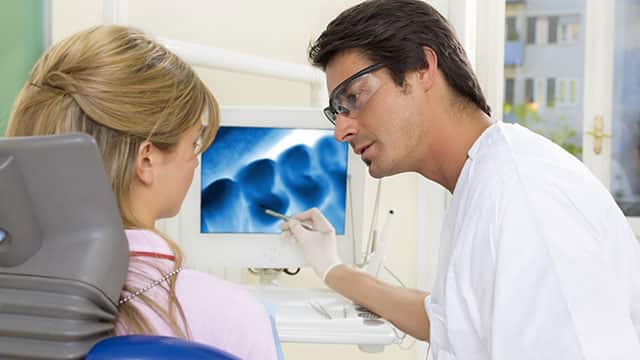
Mouth & Teeth Anatomy
What Does The Mandibular Nerve Do?
Receiving a local anesthetic injection is probably not an enjoyable part of undergoing dental work, but that shot is vital to numb the nerves around your teeth so you won't feel any pain. One major nerve in the lower part of the face and oral cavity is the mandibular nerve. Find out how this nerve affects your oral health and how it may come into play during certain dental procedures.
Read More
Mouth & Teeth Anatomy
What Does The Risorius Muscle Do?
When you smile and laugh or purse your lips, you're using a little-known muscle called the risorius. While most times it works effortlessly with other facial muscles to move your mouth into a smile, in rare instances, complications with the muscle can affect your appearance and ability to be animated.
Read More
Mouth & Teeth Anatomy
What Is a Canine Tooth?
Canine teeth are the slightly pointed teeth that sit on each side of the incisor teeth at the front of the mouth. Humans use them for biting and speaking as well as other important functions.
Read More
Mouth & Teeth Anatomy
What Is A Central Incisor?
When you flash a wide grin, the type of tooth that is front-and-center is the central incisor. Central incisors are the two upper and lower teeth at the very front of the mouth. On either side of them are the lateral incisors, making eight incisors in total in the adult dentition. Due to their position, incisors are the most noticeable teeth in the mouth, and they have various functions other than being the star of your smile.
Read More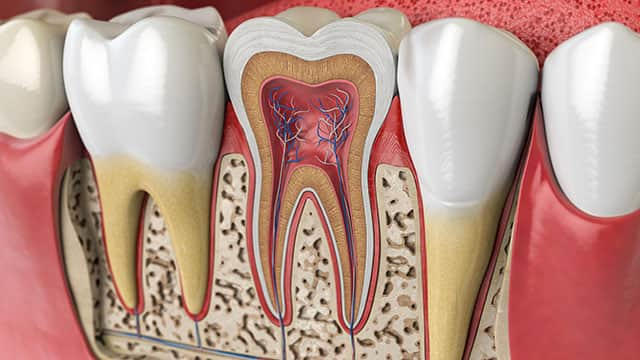
Mouth & Teeth Anatomy
What is the Pulp Chamber?
Your tooth's pulp chamber is the area within your tooth that houses the tooth pulp. Once your enamel is compromised, such as from a cavity, bacteria can enter the chamber and affect your sensitive tooth pulp. Here's how to protect the chamber area and pulp.
Read More
Mouth & Teeth Anatomy
What Is A Talon Cusp?
When you're inspecting your smile in the mirror, you most likely see two rows of smooth, rectangular teeth. Did you know that although your permanent teeth probably didn't come in for several years, they began developing before you were born? A baby begins to develop teeth in the womb, as early as twenty weeks! And while we all hope we'll end up with perfectly aligned, smooth adult teeth when they grow in, the tooth's development process can sometimes create anomalies. One such example is a talon cusp. Let's go over what a talon cusp is, how common it is, its causes, effects on oral health, and how to treat it if needed!
Read More
Mouth & Teeth Anatomy
What Is Centric Relation in Dentistry?
If you ever hear your dentist talking about centric relation, you might wonder what that term means. Centric relation (CR) has been a controversial and highly debated concept in dentistry for almost a century. Read on to find out what it means, how it's determined, and why it can be important for your oral health.
Read More
Mouth & Teeth Anatomy
What Is Concrescence?
Concrescence occurs when a tooth's cementum, the material covering the root of the tooth, is joined with another tooth's cementum. The teeth are connected at the roots. It isn't something that dental professionals see often, and it can go undetected if the teeth appear normal. It is only possible for your dental professional to make a proper diagnosis with an examination that includes X-rays.
Read More
Mouth & Teeth Anatomy
What Is Hyperdontia?
Have you ever met someone with a smile full of what looked like too many teeth? This oral health condition is defined as hyperdontia, which can mean a person has one or a dozen more teeth than the usual 32 permanent teeth.
Read More
Mouth & Teeth Anatomy
What Is Micrognathia?
Micrognathia is a big word for a condition meaning an undersized jaw. It's quite common in infants, and in many situations, it corrects itself. This condition isn't preventable and may occur when a child has another syndrome. Understanding what causes an undersized jaw and how the condition affects an individual can help you accommodate any special needs and additional care they might need.
Read More
Mouth & Teeth Anatomy
What Is Oligodontia?
If you have missing teeth from a condition or trait you were born with, you may have what's known as oligodontia.
Read More
Mouth & Teeth Anatomy
What Is Teeth Shaving?
No, it's not about hairy molars — teeth shaving is the process of intentionally recontouring or reshaping teeth to achieve a variety of restorative and cosmetic goals. This clinical procedure has been around for decades and presents an interesting option to help dentists achieve improved results for their patients.Shaving down tooth enamel is typically a painless procedure and does not normally require anesthesia. Read on for some of the more common reasons your dentist might suggest it.
Read More
Mouth & Teeth Anatomy
Face Muscles: What Are They and What Do They Do?
We use the buccinator muscle to chew, blow and suck air, whistle and form facial expressions. Learn how this important muscle works.
Read More
Mouth & Teeth Anatomy
What Is The Cementoenamel Junction (CEJ)?
Understanding the various parts of the tooth can help patients understand the many conditions that can affect the teeth and gums. One of these components, the cementoenamel junction (CEJ), is the source of tooth sensitivity for many people. Learning more about the CEJ and how to protect it from unnecessary wear can help you prevent dental sensitivity.
Read More
Mouth & Teeth Anatomy
What Is the Depressor Labii Inferioris?
It's time to learn about the depressor labii inferioris, which is the muscle that allows you to pull your lower lip down or to the side. Learning about the various muscles of the mouth facilitates a greater understanding of how your body systems work together to help you move and express your emotions.
Read More
Mouth & Teeth Anatomy
What Is the Distal Tooth Surface?
Have you ever heard of the distal tooth surface? "Distal" refers to the back surface of your tooth. In contrast, "mesial" means the front surface of your tooth. The distal surfaces of your back teeth are hard to see and can be challenging to clean. That means they're susceptible to tooth decay and other oral health concerns.
Read More
Mouth & Teeth Anatomy
What Is The Gingival Sulcus?
Much like the cuff of a sleeve fits snugly against the wrist, the gum tissue in your mouth fits tightly around each tooth. Think of the gingival sulcus as the space between the edge of the sleeve and the wrist, with the sleeve representing your gums and the wrist representing a tooth. Knowing how to keep this space clean and the role it plays in your oral health can help you avoid gum issues down the line.
Read More
Mouth & Teeth Anatomy
What Is The Medial Pterygoid Muscle?
While the chewing process is quite complicated, it's usually not something most people even think about unless they have a condition that makes moving the jaw uncomfortable. But behind the scenes of every bite of food you take, there are several muscles working together in your cheek and jaw to perform the task of breaking down your food before you swallow it. One of these is the medial pterygoid muscle.
Read More
Mouth & Teeth Anatomy
What Is The Parotid Gland?
Parotid glands are the largest salivary glands in the mouth, and they lie below and in front of the ears. A healthy parotid gland supplies saliva rich in digestive proteins to the mouth.
Read More
Mouth & Teeth Anatomy
What Is Tooth Dilaceration?
here are many ways that your teeth malformations can affect you or your child. What is tooth dilaceration? What causes curved tooth roots? We’ve got the answers to your top questions, so you know what’s going on with you or your child’s tooth.
Read More
Mouth & Teeth Anatomy
What Is Tooth Gemination?
Tooth gemination, also called double teeth, is a dental anomaly describing an oversized or abnormally shaped tooth that seems to be comprised of two teeth. If you've heard the phrase or noticed an irregularity in your smile, you may be curious to learn more about the condition and how it can be treated.
Read More
Mouth & Teeth Anatomy
What Teeth Are Baby Teeth?
IIt’s a cause for celebration when your baby’s first tooth appears. And it’s a rite of passage when your child loses their first tooth. At that point, you’ll keep the tooth fairy on standby for about six years.
Read More
Mouth & Teeth Anatomy
What To Know About The Mylohyoid Muscle
Have you ever noticed that the floor of your mouth moves when you swallow? This area is made up of several muscles, including one called the mylohyoid muscle. Here's what you need to know about this important muscle and how it helps your mouth function properly.
Read More
Mouth & Teeth Anatomy
Where Are The Anterior Teeth?
When you smile at yourself in the mirror, you can see some of your anterior teeth. There are twelve of these teeth in total: your top and bottom incisors (the two front central teeth, as well as the teeth directly next to them) and your top and bottom canine teeth. Together, the incisors and canines perform specialized functions when we eat, but these highly visible teeth are also prone to dental problems. Here's what you need to know to keep these teeth healthy and stay confident in your smile.
Read More
Mouth & Teeth Anatomy
Why Is Wharton's Duct Important?
Wharton's duct's, also known as the submandibular duct's, are the main transport channels under the tongue. Each Wharton's duct leads from the submandibular glands to the two small openings under the tongue where saliva enters the mouth. Wharton's ducts are small, but their influence on oral health is large.
Read More
Mouth & Teeth Anatomy
Your Baby's Labial Frenulum: What You Need To Know
Tucked inside your infant's gummy, toothless smile is a small piece of tissue under their upper lip called the labial frenulum.
Read More
Mouth & Teeth Anatomy
Your Zygomaticus Gives You Something To Smile About
The muscles of the face are able to perform many detailed movements, and the zygomaticus major is one of the most important muscles responsible for the creation of a smile. This facial muscle is also known as the musculus zygomaticus major or the greater zygomatic muscle, according to a study in the International Journal of Anatomy and Research (IJAR).
Read More
Mouth & Teeth Anatomy
How Many Teeth Do We Have?
How many teeth do we have? Have you ever wondered that? Well, the answer depends on a few factors, the biggest factor being age. Learn more, here.
Read More
Mouth & Teeth Anatomy
The Masseter Muscle And Its Role In Your Dental Health
Your masseter muscle is one of the strongest and most important muscles in your cheek. It helps you raise your lower jaw, which allows you to close your mouth and chew, as the textbook Illustrated Anatomy of the Head and Neck explains. When pain in this muscle arises, it can point to a number of conditions that could have an impact on your dental health. Find out how this large muscle functions, what conditions are associated with it and what treatment options are available.
Read More
Mouth & Teeth Anatomy
Tongue Laceration: Causes And Treatment
Your tongue is one of the most sensitive parts of your body and has a magnifying effect that helps you notice unwanted things in your food, like a hair or a spec of dirt.
Read More
Mouth & Teeth Anatomy
Tonsils And Adenoids: What's The Difference?
Say the words "immune system" and fighting off a pesky cold is probably the first thing that comes to mind for many people. You've heard all the standard advice, too: drink lots of fluids, get your sleep, and don't forget that vitamin C. But do you really know how your immune system works? From an oral care perspective, both the tonsils and adenoids play a key role in keeping you healthy.
Read More
Mouth & Teeth Anatomy
Interesting Facts About the Human Tongue
The tongue goes well beyond licking ice cream cones and sticking it out at your sibling. Here are ten human tongue facts, including some its functions.
Read More
Mouth & Teeth Anatomy
What Are The Different Parts Of A Tooth?
What are the different parts of a tooth? Learn about the types of teeth that make up your smile and the different parts of a tooth at Colgate® Oral Care.
Read More
Mouth & Teeth Anatomy
What Is Tooth Enamel?
Have you ever wondered about tooth enamel? What is it? How important is it? How can you protect it? Here are the answers to all of your enamel questions.
Read More
Mouth & Teeth Anatomy
3 Treatment Options For A Gummy Smile
If you have a gummy smile, it can affect your confidence. Luckily, there are several treatments available to get you the healthy smile you desire.
Read More
Mouth & Teeth Anatomy
Do You Know All the Human Teeth Names?
Get a better understanding of the human teeth names, each tooth's location in the mouth and how you use them in daily functions.
Read More
Mouth & Teeth Anatomy
Odontogenesis: 5 Stages Of Tooth Development
Odontogenesis is the medical term used to describe the complex biological process of tooth development. Here are the five stages that form your teeth.
Read More
Mouth & Teeth Anatomy
The Role Of The Platysma Muscle In Your Neck And Face
The platysma muscle is the long, flat muscle that spans from your collarbone to your lower face. Learn more about the role it plays in facial functions.
Read More
Mouth & Teeth Anatomy
What Is Hypodontia? Causes And Treatments For Missing Teeth
Hypodontia refers to the absence of one or more teeth. Learn how this condition is diagnosed and treated.
Read More
Mouth & Teeth Anatomy
What Is The Cingulum Of The Tooth?
The cingulum of the tooth is a component of dental anatomy that you can't really see, but you can feel with your tongue. Discover where it's located.
Read More
Mouth & Teeth Anatomy
What Is the Plica Fimbriata and Where Is It Located?
These small folds under the tongue are called the plica fimbriata, and they are just one of the many structures that make up the tongue and salivary glands. Learn more here!
Read More

Teeth Whitening
A Fast Way To Whiten Teeth At Home
A big event is approaching and you want to look your best for photos. What's a fast way to whiten teeth at home? Learn about fast whitening options!
Read More

Teeth Whitening
White Strips for Teeth Whitening: Do They Really Work and How to Use Them Effectively
Seeking a brighter smile? Colgate demystifies teeth whitening strips and offers proven alternatives. Discover your path to a radiant smile.
Read More
Teeth Whitening
Banana Peel Teeth Whitening: Will It Give You A Brighter Smile?
Some claim that banana peel teeth whitening works, but does the science support it? Learn more about bananas and what you can do for a whiter smile, here.
Read More
Teeth Whitening
What is the Best Over-the-Counter Teeth Whitening Option?
Whether you're on a budget or need results for a big event, here are the best over the counter teeth whitening options for any lifestyle. Learn more, here.
Read More
Teeth Whitening
Best Whitening Toothpaste: Five Signs You've Picked A Winner For A Perfect Smile
Read More
Teeth Whitening
Breaking Down Laser Teeth Whitening Cost
Laser teeth whitening is a highly effective way to whiten your teeth. It's becoming more popular among average people who are… Read more at Colgate.com
Read More

Teeth Whitening
How to Whiten a Crown
Can you whiten a crown when you've had dental work and want to brighten your smile? Before you proceed, it's best to speak with your dentist.
Read More
Teeth Whitening
Charcoal Teeth Whitening Dangers
Do charcoal teeth whitening dangers exist? Learn about the potential dangers you need to know before you give the trend a try.
Read More
Teeth Whitening
How to Choose a Teeth Whitening System
Many people want a whiter smile, so how do you choose the best teeth whitening system for you? Find out more about teeth whitening systems here.
Read More

Teeth Whitening
Does Baking Soda Whiten Teeth?
Considering teeth whitening with baking soda? Can it be combined with hydrogen peroxide? Get expert safety opinions for teeth whitening.
Read More
Teeth Whitening
Does Charcoal Teeth Whitening Work?
Charcoal toothpaste is a hot topic, and it might have you wondering if you should buy a tube of black toothpaste. But does charcoal teeth whitening work?
Read More
Teeth Whitening
Does Coconut Oil Whiten Teeth?
Does coconut oil whiten teeth? Instead of heading to a specialty food store, you should probably visit the toothpaste aisle instead. Here's why.
Read More
Teeth Whitening
Does Tea Stain Your Teeth?
We know that coffee can stain those pearly whites, but does tea stain teeth? The answer is yes. In fact, tea might be even more… Read more at Colgate.com
Read More
Teeth Whitening
Four Teeth Whitening Tips For A Whiter Smile
With the right teeth whitening tips and products, you can ensure that your investment in whiter, brighter teeth pays off with a permanently healthy smile.
Read More
Teeth Whitening
How Can I Keep My Teeth White After Whitening?
Whether you get an in-office bleaching treatment or spend weeks lightening your teeth at home, you have put a lot of effort into your beautiful smile....
Read More
Teeth Whitening
How Custom Whitening Trays Brighten Your Smile
If your teeth aren't as white as you'd like, there are safe and simple ways to improve it. One of them involves custom whitening trays.
Read More


Teeth Whitening
How Teeth Whitening Kits Create Brighter Smiles
Wanting a white smile is the top of everyone's oral hygiene list. Teeth whitening kits can help you do that at the dentist or at home. Learn more, here.
Read More
Teeth Whitening
How To Avoid Wine-Stained Teeth
How do you enjoy your favorite reds without the self-consciousness associated with red wine teeth? Here's the scoop on dental discoloration.
Read More
Teeth Whitening
How To Get A More Photogenic Smile
There are a few things you can do to get a more photogenic smile and to look more confident and composed in photos, no matter where or when they're taken.
Read More
Teeth Whitening
How To Get Whiter Teeth On The Go
Learn how to get whiter teeth before your commute or after your lunch break, and you'll always have time to build your naturally bright smile.
Read More
Teeth Whitening
What Foods Make Your Teeth Whiter?
Explore foods that make your teeth whiter. Boost your smile naturally with our top picks for teeth-whitening nutrition.
Read More
Teeth Whitening
How To Keep Your Teeth White While Sipping Warm Beverages This Winter
Coffee, tea and hot chocolate stain teeth. Here are ways to keep your teeth white while still enjoying delicious, hot beverages this winter.
Read More
Teeth Whitening
How To Keep White Teeth
Keep your teeth brilliantly white post-whitening treatment with our effective tips for a lasting, radiant smile.
Read More
Teeth Whitening
How To Make Teeth Whiter With A Whitening Toothpaste
Could your smile be brighter? Find out how to make teeth whiter by simply adding some brightening power to your regular oral care routine. Floss daily,...
Read More
Teeth Whitening
How To Smile in Pictures for a Genuine Result
Saying cheese doesn't always work. Here's how to smile properly in pictures so you appear natural, relaxed, and willing to show off your white teeth to the best effect.
Read More
Teeth Whitening
How To Whiten Teeth With Braces
Knowing how to whiten teeth with braces on isn't impossible, but special care must be taken to ensure treatment is successful. Here are three options.
Read More
Teeth Whitening
How to Whiten Your Teeth: 6 Methods for Whiter, Brighter Teeth
Discover effective techniques on how to whiten teeth with Colgate's dental tips. Enhance your confidence and whiten your teeth naturally.
Read More
Teeth Whitening
How White Can My Teeth Get?
A change of just two or three shades can make a noticeable difference in almost anyone's smile. So how white can your teeth get? Find out here.
Read More
Teeth Whitening
What are the best Instant Teeth Whitening Options?
Here are your options, including the fastest teeth whitening treatments, and the ones that take some time.
Read More
Teeth Whitening
Is Laser Teeth Whitening an Option For You?
Laser teeth whitening may be an option available at your dental office, but the treatment is not for everyone. Learn more about laser teeth whitening here.
Read More
Teeth Whitening
How Does LED Teeth Whitening Work And Is It Safe?
The process is minimally invasive and can offer great results. LED teeth whitening is a popular option for achieving a brighter smile, but is it the best at-home treatment for you?
Read More
Teeth Whitening
Is Professional Teeth Whitening Right For You?
Professional teeth whitening can seem like a miracle solution for stubborn stains and yellowing teeth, but is it the best option...
Read More
Teeth Whitening
Is Teeth Whitening Safe?
Learn about the safety of teeth whitening procedures. Discover tips and methods for safe teeth whitening to achieve a brighter and confident smile.
Read More
Teeth Whitening
How Much Does Teeth Whitening Treatment Cost?
Explore the factors influencing professional teeth whitening cost. Learn about options and considerations for achieving a brighter, more confident smile.
Read More
Teeth Whitening
Is Tooth Paint Effective For Whitening Teeth?
If you're looking to whiten your teeth, the idea of simply painting over stained or discolored tooth enamel is appealing. Does tooth paint work?
Read More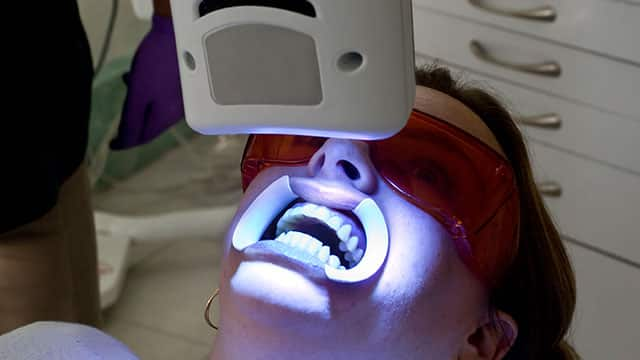
Teeth Whitening
Is UV Teeth Whitening Safe?
Is UV teeth whitening safe to do yourself at home? Find out more about UV teeth whitening including safety information and alternatives.
Read More
Teeth Whitening
Laser Teeth Whitening For A Beaming Smile
There are many cosmetic procedures to improve the color of your teeth. Laser teeth whitening is becoming one of the most popular. Here's why.
Read More
Teeth Whitening
Lipstick Color For Whiter Teeth: How Makeup Can Help Brighten Your Smile
Enhance your smile with the right lipstick color! Find out how the perfect shade can make your teeth look whiter and brighter.
Read More
Teeth Whitening
Make Your Teeth White The Right Way
Consumer demand for teeth-whitening products is high, and the options available are plentiful. Learn the best methods to make your teeth white.
Read More
Teeth Whitening
Professional Teeth Whitening: What To Ask Your Dentist
One of the most popular dental procedures now desired by patients is professional teeth whitening as it is known as. With patients retaining their teeth...
Read More
Teeth Whitening
Should You Try DIY Teeth Whitening Paste?
Tooth whitening is the process which lightens teeth, helps remove stains, and corrects tooth discoloration. Learn more on teeth whitening procedures, types, risks, and more.
Read More
Teeth Whitening
Do Strawberries Whiten Teeth and Do Other Weird Whitening Methods Really Work?
Wondering if strawberries can really whiten your teeth? Discover if this and other unconventional techniques truly work.
Read More
Teeth Whitening
Teeth Whitening For Summer
With plenty of fun outdoor opportunities, there has never been a better time to consider teeth whitening for summer. Here are your options:
Read More

Teeth Whitening
The Best Mouthwash for Teeth Whitening: What to Look For
What is the best whitening mouthwash out there and is using it going to help you get a brighter smile? Find out here!
Read More
Teeth Whitening
5 Cheap and Easy Tips for Whiter Teeth
Cheap teeth whitening is easier than you think. Try these cheap, simple steps to protect teeth from stains and to whiten teeth & brighten your smile.
Read More
Teeth Whitening
Three Proven Tips To Keep Teeth White
Thanks to advances in oral care, people no longer have to walk around with stained or yellow teeth. These days, brightening… Read more at Colgate.com
Read More
Teeth Whitening
Does Brushing Your Teeth Make Them Whiter?
Does brushing your teeth make them whiter? Everyone seeks a sparkling smile, but brushing alone may not remove gray or yellow stains.
Read More

Teeth Whitening
What Are the Benefits of Turmeric for Your Teeth?
Does turmeric for teeth whitening actually work? Read on to learn more about turmeric, if it whitens teeth and if there are other oral health benefits.
Read More
Teeth Whitening
Use Teeth Whitening Trays For A Brighter Smile
Whether you're a heavy smoker, you drink three cups of coffee each day or you've simply noticed that your teeth are becoming faded and yellow with age,...
Read More
Teeth Whitening
Wedding Photography: Get Your Smile Camera-Ready
Get your smile camera-ready for the wedding photography portion of your whirlwind day. But how do you achieve these whiter results?
Read More
Teeth Whitening
What Causes Green Tooth And Other Tooth Discoloration?
Green tooth discoloration, a rare condition, can be extrinsic or intrinsic, arising from various internal or external factors.
Read More
Teeth Whitening
What Tooth Whitening Method Is Best For Me?
Have you ever thought about tooth whitening? There are several different whitening products available for people thinking about whitening their teeth.
Read More
Teeth Whitening
Which Teeth Whitening Solution Is Best For You?
While our teeth are not, by nature, perfectly white, most people feel that they could improve their smile with brighter, whiter… Read more at Colgate.com
Read More
Teeth Whitening
White Spots on Teeth After Whitening Treatments
Teeth whitening can make existing white stains from hypocalcification more visible, rather than causing new stains. Learn more.
Read More
Teeth Whitening
Do Whitening Strips Damage Teeth? How to Use Them Safely
Are teeth whitening strips suitable for everyone? Discover the expert guidance from our professionals to make an informed decision about teeth whitening.
Read More
Teeth Whitening
Whitening Bonded Teeth: Perfect Your Smile
Restorations don't require a great deal of special care, but when it comes to whitening bonded teeth, there are some things you should keep in mind.
Read More
Teeth Whitening
Whitening Toothpaste 101: The Basics of Daily Whitening
Discover if whitening toothpaste is right for you: understand its effectiveness and safety to choose the best product for your dental health.
Read More
Teeth Whitening
What Works Best To Remove Coffee Stains From Your Teeth?
Most of us can't live without a daily dose of coffee to jump start the day, but could the beverage that puts morning smiles on… Read more at Colgate.com
Read More
Teeth Whitening
How To Make Your Own Teeth Whitening Paste
Tooth whitening is the process which lightens teeth, helps remove stains, and corrects tooth discoloration. Learn more on teeth whitening procedures, types, risks, and more.
Read More
Teeth Whitening
5 Tips For Preventing Teeth Stains From Braces
Learn about our top 5 tips for preventing teeth stains from braces and whitening your teeth evenly once they come off with Colgate.
Read More


Teeth Whitening
Teeth Whitening and Anti-Aging: Turning Back the Clock on Your Smile
As you age, your teeth age with you, often leading to yellowing. Here are some effective teeth whitening tips specifically for improving your aging, yellow teeth
Read More
Teeth Whitening
3 Types of Tooth Stains and How to Remove Them
Learn about the different types of stains and what whitening options are best for stain-removal for each type.
Read More
Teeth Whitening
What is Enamel Microabrasion?
A brighter smile can boost your confidence, consider a professional enamel microabrasion. Click here to learn more about enamel microabrasion with Colgate®.
Read More
Teeth Whitening
How to Smile on Camera
How to have a great smile on camera? Click here to learn the healthiest ways to have a beautiful smile on and off-camera with Colgate.
Read More


Teeth Whitening
12 Foods That Stain Your Teeth
Beverages, berries, curries, pasta sauce: identify foods that cause the most teeth stains and how to mitigate their effects for a healthier smile.
Read More
Teeth Whitening
Is a Teeth Whitening Light Effective?
Looking for a way to brighten your smile with teeth whitening? Learn more about both UV and blue light teeth whitening to decide which is the best option for you.
Read More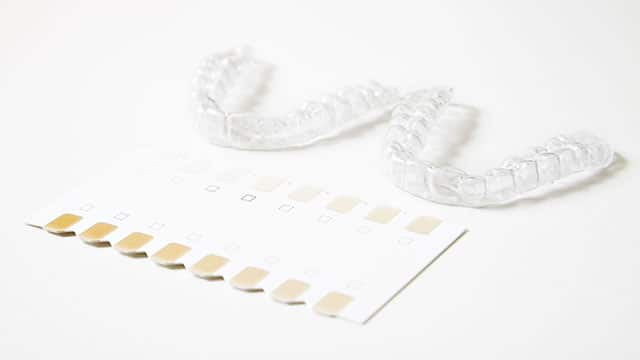
Teeth Whitening
How Do I Know What Shade My Teeth Are?
There's no one standard system in the dental field to measure and determine tooth color. Find out more here.
Read More
Teeth Whitening
Burned Gums from Teeth Whitening: What You Need to Know
If you've been whitening your teeth at home, you could have burned your gums from teeth whitening. Find out more about it, here from Colgate.
Read More
Teeth Whitening
How to Safely Use a Tooth Whitening Gel at Home
Find all our tips for brightening your smile at home with tooth whitening gel safely and effectively (with the guidance of a dentist).
Read More
Teeth Whitening
Tooth Whitening: Will it Work for Me and What are My Options?
Whiter teeth can be a confidence booster, so you might want to explore your options
Read More
Teeth Whitening
Whitening Toothpaste - Hydrogen Peroxide vs. Carbamide Peroxide
Hydrogen peroxide toothpaste is a great way to whiten teeth every day. Can you benefit from it? Here are four things people often wonder.
Read More
Teeth Whitening
How to Get Rid of Yellow Teeth: 5 Top Tips
Discover how to effectively get rid of yellow teeth, whether from stains or other causes, using over-the-counter products or professional dentist treatments.
Read More
Teeth Whitening
Whitening 101: Your Dental Hygienist Explains How Hydrogen Peroxide Works
Discover the science behind hydrogen peroxide in teeth whitening. A dental professional explains how it works, what to look for, and how to get a brighter smile.
Read More
Teeth Whitening
The Truth About a Whiter Smile After 35
By: Mandy Dennis
Registered Dental Hygienist
Read More
Teeth Whitening
Smile Brighter Every Day
Getting a truly bright smile shouldn't be a chore—it should be simple, effective, and backed by real results. This page is your guide to understanding what can stain teeth and how to build an easy, powerful routine with Colgate Optic White to keep your smile shining.
Read More
Teeth Grinding (Bruxism)
Using Botox as a Treatment for Grinding Teeth
Bruxism, more commonly known as teeth grinding, can result in jaw pain and persistent headaches. Learn more here.
Read More
Teeth Grinding (Bruxism)
Bruxism 101
Bruxism, or tooth grinding and clenching of the teeth is a common condition that affects up to 40 million adults. Learn more about bruxism and tooth grinding, here.
Read More
Teeth Grinding (Bruxism)
Bruxism Exercises To Reduce Teeth Grinding
Bruxism, can be damaging to the enamel and can even break your teeth. Find out more on reducing teeth grinding with bruxism exercises, here.
Read More
Teeth Grinding (Bruxism)
Bruxism: Signs And Symptoms
Other potential signs of bruxism include aching in the face, head and neck. Your dentist can make an accurate diagnosis and determine if the source of facial pain is a result from bruxism.
Read More
Teeth Grinding (Bruxism)
How to Treat and Prevent Pain from Grinding Teeth
Grinding teeth, also known as bruxism may cause facial pain. Find out more about teeth grinding, facial pain, and ways to combat this problem.
Read More
Teeth Grinding (Bruxism)
Trigger Point Injections for TMJ Disorders
If you suffer from TMD or myofascial pain, trigger-point injections may help you find relief, among other pain management treatments. Learn more here.
Read More
Teeth Grinding (Bruxism)
How Night Guards Help with Teeth Grinding
Regardless of where a night guard is purchased, its main function is to prevent the surfaces of your teeth from grinding together.
Read More
Teeth Grinding (Bruxism)
Bruxism Symptoms and Causes
The bruxism causes are varied, but you can watch for certain symptoms if you think you may have it. Learn more here.
Read More
Teeth Grinding (Bruxism)
Bruxism in Children: Signs, Symptoms, and Effects
Bruxism in children - believe it or not, is rather common. Here's what you need to know about bruxism and what you can do for your child.
Read More
Teeth Grinding (Bruxism)
Over the Counter vs. Custom Night Guard: Which Is Right for You?
Wearing a night guard protects against teeth grinding while you sleep, but which type is right for you? Learn about your custom night guard options.
Read More
Teeth Grinding (Bruxism)
How to Ease Symptoms of Teeth Clenching
Bruxism, a condition most often caused by stress, involves grinding your teeth, either at night or throughout the day, without realizing it. Learn how to stop clenching your teeth here.
Read More
Teeth Grinding (Bruxism)
The Temporalis Muscle, Jaw Pain, and Headaches
There are many different types of headaches. Surprisingly, some headaches can be traced to the jaw muscles, including the temporalis muscle. Learn more.
Read More
Teeth Grinding (Bruxism)
Sleep Bruxism: How to Stop Grinding Your Teeth at Night
Do you ever wake up from a night's sleep with sore teeth and jaws? You could be grinding your teeth. Learn more about bruxism here and why it occurs and how you can prevent it.
Read More


Oral Care: Kids (5-12)
Common Oral Health Questions Asked By New Parents
Many experts recommend breast-feeding over bottle-feeding for the overall health of your child. Learn more at Colgate.com.
Read More
Oral Care: Kids (5-12)
How To Practice Good Oral Hygiene With Braces
Having braces can be a real challenge when it comes to oral hygiene. Approximately 3 million teenagers and many adults wear braces.
Read More

Oral Care: Kids (5-12)
Oral Aversion & Oral Fixation Help
What is oral fixation or aversion? What causes each? Click here for your go-to information on oral fixations and aversions for babies with Colgate.
Read More
Oral Care: Kids (5-12)
10 Tips For Pacifier Weaning: Help Your Child Kick Their Pacifier Habit
Many babies get comfort and security from sucking on a pacifier. But eventually, it's time to stop the habit. Here are 10 tips for pacifier weaning.
Read More
Oral Care: Kids (5-12)
How Do I Know If My Baby Is Teething?
Struggling to determine if your baby is teething? Continue reading for the signs and symptoms for emerging teeth in your baby.
Read More

Oral Care: Kids (5-12)
Fun Dental Activities for Children
Enjoyable dental activities for children can teach kids about oral care. Since children learn through play, stimulate interest with these fun projects.
Read More
Oral Care: Kids (5-12)
4 Natural Teething Remedies For Babies: Are They Safe?
Teething is a fascinating time in a baby's life. Are there natural teething remedies that are safe for your baby? Learn more, here.
Read More
Oral Care: Kids (5-12)
6 Dentist Games For Kids To Ease Their Dental Phobia
Help ease your kid's fear of the dentist with these fun and effective dentist games, and get them empowered to form good oral care habits for life.
Read More
Oral Care: Kids (5-12)
9 Causes of Bad Breath in Children
Even healthy children can sometimes experience bad breath. If you've noticed that your little one's breath is not so pleasant, there is hope.
Read More
Oral Care: Kids (5-12)
A Guide To Your Teething Baby
Use this guide to understand the signs and symptoms of teething and to learn how to best soothe your teething baby's discomfort.
Read More
Oral Care: Kids (5-12)
A Morning And Evening Brushing Routine Helps Kids Improve Dental Care Habits
Did you know it only takes 21 days to make a routine a habit? Creating good oral health habits can start at a young age and carry through for life.
Read More
Oral Care: Kids (5-12)
Activities To Encourage Dental Health For Kids
From the time a child begins teething, dental health is something moms and dads think about. But sometimes brushing your child's teeth is harder than it sounds.
Read More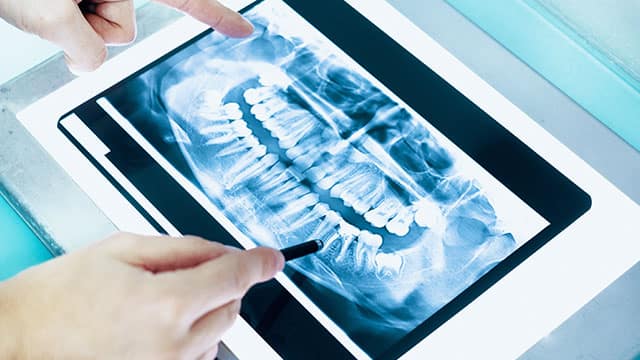
Oral Care: Kids (5-12)
An X-Ray of Baby Teeth: When, What, and How
An X-ray of baby teeth shows any underlying dental issues that may not be visible to the naked eye. Here's how to get your child ready.
Read More
Oral Care: Kids (5-12)
Ankyloglossia And Your Infant: Symptoms & Treatment
Ankyloglossia, commonly known as tongue-tie, is present at birth. How may tongue-tie affect infants and how does a doctor treat it? Learn more here.
Read More
Oral Care: Kids (5-12)
Are Infant Teething and Diarrhea Related?
It is a commonly held belief by parents that teething causes diarrhea. Current medical opinion, however, is that there is no direct correlation. Learn more here.
Read More
Oral Care: Kids (5-12)
Baby Bottle Tooth Decay: Shielding Your Baby's Teeth
What is Baby Bottle Tooth Decay? Tooth decay that occurs in infants or toddlers is also commonly referred to as early childhood caries (ECC).
Read More
Oral Care: Kids (5-12)
Baby Bottle Tooth Decay
In infants, tooth decay is commonly referred to as baby bottle tooth decay. This occurs when sugars from food & liquids attach to teeth for periods of time.
Read More
Oral Care: Kids (5-12)
Baby Teeth Chart: How It Can Help You During Teething
Many parents search for a baby teeth chart when their infant is teething. This period in a child's life can be difficult not only for the baby, but also for the parents.
Read More
Oral Care: Kids (5-12)
Baby Teething: Signs And Treatment
Learn about the primary dentition process so you can enjoy those special moments when baby's first teeth arrive. Learn more about eruption and more.
Read More
Oral Care: Kids (5-12)
Baby Teething Symptoms And How To Treat Them
Baby teething can be frustrating for you and your baby, but knowing what to expect can help you manage and overcome several baby teething symptoms.
Read More
Oral Care: Kids (5-12)
Baby Teething Timeline
Teething is a big part of your baby's first year of development. While every baby is different, here is a typical baby teething timeline that can help new parents.
Read More
Oral Care: Kids (5-12)
Back To School Health: A Checklist For Kids
Don't forget one of the most important items on your kid's back to school health checklist: a dental checkup. Find a back to school health checklist here.
Read More
Oral Care: Kids (5-12)
Best Teething Toys For Little Teeth
Once your baby starts teething, you’ll need toys to help ease pain. Find out more about the best teething toys for infants to alleviate teething pain.
Read More
Oral Care: Kids (5-12)
Best Toothpaste for Kids with Cavities
Discover the ideal toothpaste for children battling cavities on Colgate.com. Learn how to tackle tooth decay effectively for your kids' oral health needs.
Read More
Oral Care: Kids (5-12)
Bisphenol A In Dental Sealants: Is It Safe?
Dental sealants are protective coatings applied to the chewing surfaces of a child's molars, and they may contain bisphenol A (BPA). Here's what to know.
Read More
Oral Care: Kids (5-12)
Bleeding Gums In Children: Should You Be Worried?
Are bleeding gums in kids a cause for concern or nothing to worry about? For adults, gums that bleed during brushing or flossing may be a sign of gingivitis.
Read More
Oral Care: Kids (5-12)
Brushing Baby's Teeth: How To Get Started
Start your baby's oral care journey right by brushing their teeth as soon as they erupt, establishing a healthy habit that will benefit them for a lifetime.
Read More
Oral Care: Kids (5-12)
Step-by-Step Guide to Toddler Toothbrushing | Colgate
Learn with our new tutorial the importance of properly brushing your toddler's teeth early on, as it lays the foundation for lifelong oral hygiene habits.
Read More
Oral Care: Kids (5-12)
Can A Baby Sleep With A Pacifier? Know The Pros And Cons
Is it safe to let a baby sleep with a pacifier? Here are the pros and cons, as well as some best practices to follow when giving your child a pacifier.
Read More
Oral Care: Kids (5-12)
Can An Infant Ear Infection Affect Your Baby's Oral Health?
When your child gets fussy, how do you know if it's just teething or an infant ear infection? Consider these issues in this easy dental primer.
Read More
Oral Care: Kids (5-12)
Can Teething Cause Vomiting?
Teething causes sleepless nights for new parents, but can teething cause vomiting? Find out more about the side effects of teething, here.
Read More
Oral Care: Kids (5-12)
Caring For Baby Teeth
Our little guys are both under three years old, so we have a fair number of baby teeth around here. And as much pain as these teeth caused coming into the world, we still try to treat them well. Read more at Colgate.com
Read More
Oral Care: Kids (5-12)
Common Children's Dental Care Questions
Your children's teeth might be small, but they are important. Following good dental practices as a child is the only way to… Read more at Colgate.com
Read More

Oral Care: Kids (5-12)
Coping With The Toddler Teething Phase
Toddler teething is similar to baby teething: for some, it hurts. For others, it's a breeze. Looking for these signs may help you diagnose the distress.
Read More
Oral Care: Kids (5-12)
Crafts For the First Lost Tooth: Ideas and Fun Memories
Explore creative ways for pulling out your child's loose tooth with Colgate. Discover playful strategies and helpful tips to make this experience painless.
Read More
Oral Care: Kids (5-12)
Curing Gingivitis In Your Children
Curing gingivitis is usually straightforward, and a great opportunity for teaching your children about good oral health habits. Here are six treatments.
Read More
Oral Care: Kids (5-12)
Dental Activities For Kids Promote Oral Health Awareness
February is National Children's Dental Health Month, but learning about tooth care can be done anytime. Read more at Colgate.com
Read More
Oral Care: Kids (5-12)
Dental Care For Kids: The Best Secrets For Keeping Your Child's Smile Bright
When the first teeth begin to erupt in your child's mouth, you might feel concerned about giving her the right dental care. Read more at Colgate.com.
Read More
Oral Care: Kids (5-12)
Dental Care For Kids: The Importance Of Brushing Teeth At Child Care Centers
Good dental care for kids goes beyond home. Young children in preschool and daycare often eat two of their three meals a day and snacks without brushing.
Read More
Oral Care: Kids (5-12)
Dental Caries in Infants: Implications and Prevention
Explore the implications of dental caries in infants and learn effective prevention strategies with Colgate. Get insights to protect your kids oral health.
Read More
Oral Care: Kids (5-12)
Dental Health For Kids: A Parent's Guide
Dental health for kids is just as important as overall health. Understanding that your children's teeth need optimal care is the first step.
Read More
Oral Care: Kids (5-12)
Dental Hygiene For Kids: Make Mouth Care Fun!
When you tell your 4-year-old to brush his teeth before preschool, do you get the sense that he really hides in the bathroom for a few minutes?
Read More
Oral Care: Kids (5-12)
Dental Hygiene For Preschoolers
Dental hygiene for preschoolers should be a priority, even though baby teeth don't stick around for long.
Read More
Oral Care: Kids (5-12)
Dental Music: Songs About Teeth Your Kids Will Love
Have you ever thought about creating your own dental music that will encourage your children to engage in good oral care habits? Read more at Colgate.com
Read More
Oral Care: Kids (5-12)
Dental Trivia: Fun Teeth Facts for Kids
Discover fascinating dental trivia and fun teeth facts for kids at Colgate. Explore our top 10 most entertaining facts about children oral health.
Read More
Oral Care: Kids (5-12)
Dentist Appointment Anxiety: 3 Ways To Alleviate Your Child's Fears
Taking your child to the dentist can be a difficult experience if he is feeling anxious about the appointment. So what can you do to help ease his mind?
Read More
Oral Care: Kids (5-12)
What Is Dentofacial Orthopedics?
Dentofacial orthopedics is the field of study that concentrates on improving the position and dimensions of the bones that house the teeth. Learn more now!
Read More
Oral Care: Kids (5-12)
Do Baby Growth Spurts Affect the Development of Teeth?
Infant growth spurts are short periods when a baby quickly gains weight and height, and their side effects can have a close resemblance to teething.
Read More
Oral Care: Kids (5-12)
Do Baby Teeth Have Roots?
Do baby teeth have roots if they're just going to fall out? Understanding the structure of baby teeth allows you to properly care for your child's mouth.
Read More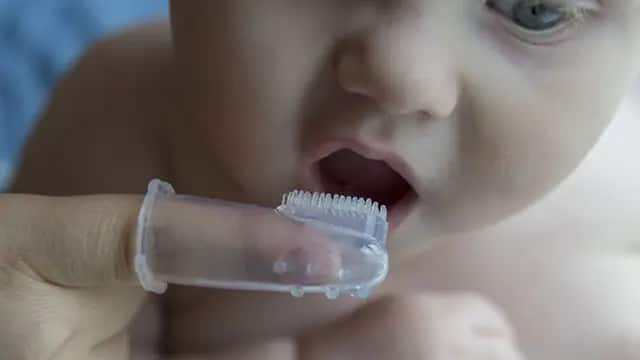
Oral Care: Kids (5-12)
How to Clean a Newborn’s Tongue: Do You Need a Tongue Cleaner?
A baby's mouth needs cleaning before the teeth erupt, and not necessarily with a baby tongue cleaner. Infant oral care is as easy as these steps.
Read More
Oral Care: Kids (5-12)
Does My Child Need a Thumb-Sucking Guard?
A thumb-sucking guard can help prevent children from putting their thumbs in their mouths, allowing teeth to grow in properly by a certain age.
Read More

Oral Care: Kids (5-12)
Early Childhood Caries: What Is It?
Learn about a common yet preventable oral health issue in children: early childhood caries. Find out what they are, risk factors, prevention, & treatment.
Read More

Oral Care: Kids (5-12)
Ease Discomfort When Your Child Is Teething
Teething can lead to an uncomfortable, cranky child and anxious, sleep deprived parents. So finding ways to alleviate the discomfort is important for both parent and child.
Read More
Oral Care: Kids (5-12)
Endodontic Treatment in Children
Endodontic treatment involves the pulp of a tooth. The pulp contains the tooth's nerve. It also contains blood vessels that give the tooth oxygen and nutrients.
Read More
Oral Care: Kids (5-12)
Exercises To Correct Tongue Thrust In A Growing Child
Doctors and speech therapists use tongue thrust exercises to help children pronounce words and swallow food properly. Try the following approaches at home.
Read More
Oral Care: Kids (5-12)
Extrusion Reflex: Why Your Baby Is Spitting Out Solids
An extrusion reflex could affect the way your baby experiences solids. Read on to learn the why and when behind giving your baby solid foods. Learn more.
Read More
Oral Care: Kids (5-12)
Fillings in Baby Teeth: Are They Really Necessary?
If primary teeth eventually fall out, is it really necessary to put fillings in baby teeth? Here's what you need to know about treating childhood cavities.
Read More
Oral Care: Kids (5-12)
Finding Relief for Your Baby’s Teething Fever
Learn how to provide relief for your baby's teething fever with Colgate's comprehensive guide. Discover symptoms, safe remedies, and expert tips here.
Read More
Oral Care: Kids (5-12)
First Dental Visit: What To Expect For Your Child
The day your child attends his or her first dental visit can be an anxious time for your child. But among other things, it's a time to get acquainted.
Read More
Oral Care: Kids (5-12)
Five Tips For Keeping Baby Gums Healthy
Oral care begins before primary teeth make their appearance. To this end, here are some simple tips to keep baby gums healthy during this first stage.
Read More
Oral Care: Kids (5-12)
Five Ways To Avoid Scary Treats For A Healthier Halloween
Not all candy is created equal. Items like candy teeth and gummies, which stay in the mouth longer, should be tossed for treats that are less damaging.
Read More
Oral Care: Kids (5-12)
Four Developmental Milestones In Your Child's Oral Health
We've all recorded our kids' big moments in the early years, but do you remember their dental developmental milestones? Here are the most important ones.
Read More
Oral Care: Kids (5-12)
4 Ways to Reduce Early Tooth Decay in Toddlers
Early tooth decay is damage on the tooth's enamel, and can happen anywhere on the tooth, and at any age. The good news is that it's very treatable.
Read More
Oral Care: Kids (5-12)
From Baby Teeth To Adult Teeth: Stages And Differences
Learn more about oral care for children, including how to properly brush kid's teeth, kids toothbrushes, and much more, from the Colgate Oral Care Center.
Read More
Oral Care: Kids (5-12)
Fun Ways To Teach Kids About Mouth Anatomy
Learn more about oral care for children, including how to properly brush kid's teeth, kids toothbrushes, and much more, from the Colgate Oral Care Center.
Read More
Oral Care: Kids (5-12)
Funny Games That Make Kids Smile
Kids laugh at pretty much anything, from mismatched socks to jokes that don't make sense. Engaging them in silly activities… Read more at Colgate.com
Read More
Oral Care: Kids (5-12)
Dental Care for Kids From Birth to 8 Years Old: When Should You Start Brushing Your Infant's Teeth?
Discover expert tips on when to start brushing your baby's teeth and how to get their toothbrush ready. Ensure your infant's oral health with Colgate.
Read More
Oral Care: Kids (5-12)
Glycerin in Dental Care
You may have heard of glycerin for baby's mouth and oral care, but dental experts recommend these tips for cleaning your little one's mouth. Learn more.
Read More
Oral Care: Kids (5-12)
Gum Abscess in Children: What Parents Need To Know
A gum abscess in children can be a concerning situation for parents. Luckily, it can be treated with a visit to the dentist.
Read More
Oral Care: Kids (5-12)
Hand, Foot and Mouth Disease (HFMD): Symptoms, Treatment, Prevention
Hand, foot and mouth disease is a common and communicable children's virus. Learn more about symptoms to watch for, how to treat and prevent HFMD.
Read More
Oral Care: Kids (5-12)
Healthy Kids Teeth: Surprising Facts Every Parent Should Know
Not every child develops cavities. What is the secret to healthy kids teeth? What are those super parents doing to protect their children from tooth decay?
Read More
Oral Care: Kids (5-12)
Healthy Teeth For Kids: Encourage Good Habits Early
Since your children's health is always high on your list of priorities, maintaining a healthy smile should be, too. Read more at Colgate.com
Read More
Oral Care: Kids (5-12)
Helping Your Child Break A Thumb Sucking Habit
Discover effective strategies to help your child break the thumb-sucking habit with Colgate. Find guidance and support to promote healthy oral habits for your little one.
Read More
Oral Care: Kids (5-12)
Herpangina And Children: Symptoms And Finding Relief
What is herpangina? How do you know if your child has it and how can you relieve their discomfort? Learn more about herpangina in children, here.
Read More
Oral Care: Kids (5-12)
How A Stainless Steel Crown Can Save A Baby Tooth
Baby teeth play a crucial role to the eventual adult set. If your child has a decayed primary tooth, a stainless steel crown may be the best solution.
Read More
Oral Care: Kids (5-12)
How Are Deciduous Teeth Different From Permanent Teeth?
Deciduous teeth, or primary teeth are different from your permanent teeth. Learn more about your deciduous teeth, from the Colgate® Oral Care Center.
Read More
Oral Care: Kids (5-12)
How Do I Care For My Infant's Teeth?
Learn the basics of infant tooth care including information about baby bottle decay, fluoride and teething at Colgate.com.
Read More
Oral Care: Kids (5-12)
How Do I Care For My Toddler's Teeth?
Passing on good oral habits to your child is one of the most important health lessons you can teach them. Start by teaching him or her to brush twice a day.
Read More
Oral Care: Kids (5-12)
How February Promotes Kids' Dental Care
Learn more about oral care for children, including how to properly brush kid's teeth, kids toothbrushes, and much more, from the Colgate Oral Care Center.
Read More
Oral Care: Kids (5-12)
How Long Should A Baby Use A Pacifier
As stated, pacifiers are used mainly to relax a child while also satisfying the sucking reflex. Learn more here about how often they should use them and when they should stop.
Read More
Oral Care: Kids (5-12)
How Teething Fits Into Infant Development
Many future responsibilities can run through your head as you hold your newborn in your arms, but teething is an important stage of infant development.
Read More
Oral Care: Kids (5-12)
How To Avoid Summer Dental Surprises When School's Out
While summer can breed lethargic children, it doesn't have to mean summer dental surprises. Get your kids to stick to oral hygiene with these four tips.
Read More

Oral Care: Kids (5-12)
How To Care For Your Child's Adult Teeth Right From The Start
You might try to keep your child's baby teeth clean, but once the permanent teeth start to come in, cleaning them needs to be a priority. Read more here.
Read More
Oral Care: Kids (5-12)
How To Clean A Baby Bottle Correctly In 5 Steps
Keeping your baby's bottle free of germs is paramount to their health. Check out these five steps outlining how to clean a baby bottle correctly.
Read More
Oral Care: Kids (5-12)
How To Clean A Pacifier Correctly: 3 Effective Methods
Knowing how to clean a pacifier can help you ensure that your child's mouth is free of harmful bacteria that can cause disease and tooth decay. Learn more.
Read More
Oral Care: Kids (5-12)
How To Clean Braces
Having braces can be a real challenge when it comes to oral hygiene. Approximately 3 million teenagers and many adults wear braces.
Read More
Oral Care: Kids (5-12)
How To Deal With Toddler Teething Pains
Few things are as upsetting as your child suffering from teething pains. Find out how you can help your child with relief from their teething pains, here.
Read More
Oral Care: Kids (5-12)
How To Encourage Oral Health Care For Kids
Oral health care for kids could be easy – that is, if you can get your children excited about it. Here are a few ideas to get them on track.
Read More
Oral Care: Kids (5-12)
How To Handle And Prevent Kids Biting
Biting is common in toddlers. Click here to find out why kids bite, how you should react to the biting, and what you can do to stop it with Colgate.
Read More
Oral Care: Kids (5-12)
How to Help a Child Who Won't Brush Their Teeth
Has your kid's oral care turned into a daily battle? Click here to learn more tips for making brushing and flossing fun with Colgate.
Read More
Oral Care: Kids (5-12)
How To Improve Oral Health
Many parents have experienced a child's noncompliance or even outright refusals when it comes to brushing teeth. Yet parents play a major role.
Read More
Oral Care: Kids (5-12)
How To Keep Kids Smiling With Braces
Smiling with braces can be difficult when your child feels self-conscious or less than thrilled about showing them. Here's how to give them confidence.
Read More
Oral Care: Kids (5-12)
How To Say Goodbye To Binky Bunny - Your Baby's Pacifier
Most parents allow their infants to use a pacifier, but that cute little binky bunny can damage your baby's teeth if it is used incorrectly.
Read More
Oral Care: Kids (5-12)
Importance of Caring for Natal Teeth
Caring for natal teeth is important as they affect the appearance of a child's adult teeth. Learn more about natal teeth and how to take care of them here.
Read More
Oral Care: Kids (5-12)
Is Bubble Gum Good Or Bad For Children's Teeth?
Bubble gum is a childhood favorite. The combination of sweetness, messiness and noise is irresistible to many kids. Parents, read more at Colgate.com.
Read More
Oral Care: Kids (5-12)
Is Your 3 Month Old Teething? What You Should Know
Most babies start teething between 6 and 12 months, but a 3 month old teething is a reality for some parents. Learn signs, symotoms, and treatment, here.
Read More
Oral Care: Kids (5-12)
Kid's First Cavity: What You Need to Know to Prevent Another One
One of the most powerful things that parents can do is model good oral hygiene for their children. So don't wait until you have the bathroom to yourself to brush your teeth.
Read More
Oral Care: Kids (5-12)
Kids' Teeth And Cavity Protection
Even if you had cavities when you were young, your child doesn't have to develop them. Find out how to protect kids' teeth from tooth decay.
Read More
Oral Care: Kids (5-12)
Kids Dental Care: Promoting Good At-School Habits
Here are a few simple ways in which to encourage good dental hygiene while kids are at school. Learn more at Colgate.com.
Read More
Oral Care: Kids (5-12)
Kids Mouthwash And Mouthwash Safety
An oral hygiene routine that includes mouthwash can help to keep teeth and gums healthy, but it's important that kids mouthwash is used safely. Learn more at Colgate.com.
Read More
Oral Care: Kids (5-12)
Kids With No Teeth: What Causes Delays In Tooth Eruption?
Although an eruption delay is not something to worry about for most kids with no teeth, there may be underlying causes for this condition in some infants.
Read More
Oral Care: Kids (5-12)
Learning To Brush: Teeth Cleaning Tips For Parents Of Toddlers
Is it time to teach your kids how to brush? Taking the time to teach your children to clean their own teeth at an early age will pay off in the long run.
Read More
Oral Care: Kids (5-12)
Losing Baby Teeth: A Sure Sign Of Growth
Losing baby teeth is a rite of passage for kids, and makes them feel like they're truly growing up. But good oral hygiene shouldn't stop at this time.
Read More
Oral Care: Kids (5-12)
Two Teeth-Shaped Treat Recipes For Fun and Education
Join the fun of baking teeth cookies with your family, a delightful activity that highlights the importance of dental hygiene tools and techniques.
Read More
Oral Care: Kids (5-12)
Managing The Teething And Sleep Habits Of Your Baby
Teething is one potential cause of your newborn not sleeping at night. As you'll come to understand, teething and sleep don't mix well. Find out more here.
Read More
Oral Care: Kids (5-12)
Missing-Tooth Smile? How To Restore Your Child's Confidence
Although a missing-tooth smile may give you plenty to grin at now, what should you do if your child loses a permanent tooth by accident?
Read More
Oral Care: Kids (5-12)
My Child Refuses To Brush And Floss!
Some children are very resistant to stopping their play or television time to brush and floss. Here are some ways to put an end to the fight.
Read More
Oral Care: Kids (5-12)
Natural And Safe Teething Remedies For Your Baby
What teething remedies are safe for babies? It is not easy watching your child deal with the discomfort that can come with the arrival of baby's first teeth.
Read More
Oral Care: Kids (5-12)
Oral Health And Safety For Children In The Winter
In the winter, oral health and safety for children means finding the right balance between the fun of a snow day and the requirements of mouth care.
Read More
Oral Care: Kids (5-12)
Oral Health Education: A Manual For Parents
Learn more about oral care for children, including how to properly brush kid's teeth, kids toothbrushes, and much more, from the Colgate Oral Care Center.
Read More
Oral Care: Kids (5-12)
Complete Guide to Children's Dental Health: Expert Tips for a Bright Smile
Teaching your child proper oral care at a young age is an investment in his or her health that will pay lifelong dividends. Learn more tips and tricks here!
Read More
Oral Care: Kids (5-12)
Oral Health Tips For Summer
Summer is fun, but a toothache on vacation isn't. Here are a few oral health tips for summer to keep a growing mouth healthy throughout the season.
Read More
Oral Care: Kids (5-12)
Oral Thrush in Babies: Causes, Symptoms, and Treatment
What is oral thrush in babies? How can you tell if your little one has it and how does a doctor treat it? Learn more here.
Read More
Oral Care: Kids (5-12)
Over-Retained Baby Teeth: A Guide to Treatment
When the eruption of the permanent tooth is delayed for more than a year from the expected date, it is considered over-retained.
Read More
Oral Care: Kids (5-12)
Pacifiers And Teeth: How To Protect Your Baby's Oral Health
When it comes to pacifiers and teeth, your baby can enjoy his or her pacifier without it interfering with early oral health, but use it wisely.
Read More
Oral Care: Kids (5-12)
Parent Guide To Children's Teeth: Who, What, When And How
We all wish kids came with a user manual, but good oral hygiene can actually consist in this handy parent guide to children's teeth.
Read More
Oral Care: Kids (5-12)
Pediatric Dentistry: What Makes It Different?
Pediatric dentistry is tailored to ensure infants, children and teens receive the best dental care possible. Learn more about pediatric dentistry, here.
Read More
Oral Care: Kids (5-12)
Pediatric Guidelines for Using Toothpaste in Young Children
Discover essential guidelines for using toothpaste in young children. Learn about fluoride toothpaste recommendations, supervision, and product selection.
Read More
Oral Care: Kids (5-12)
Posterior Tongue Tie: Complications and Treatment Options
A posterior tongue-tie may cause difficulty breastfeeding or eating. Learn what a medical professional can do to address this problem, here.
Read More
Oral Care: Kids (5-12)
Preventing Baby Bottle Syndrome
Learn how to prevent baby bottle syndrome and protect your child's teeth with simple tips from Colgate. Find expert advice on oral care for kids here.
Read More
Oral Care: Kids (5-12)
Primary Dentition: What To Expect Of Baby Teeth
Learn about the primary dentition process so you can enjoy those special moments when baby's first teeth arrive. Learn more about eruption and more.
Read More
Oral Care: Kids (5-12)
Pulpotomy In Primary Teeth
A pulpotomy in primary teeth may be performed if the tooth is still vital and the decay has extended to the pulp. Here's what you need to know.
Read More
Oral Care: Kids (5-12)
Reward System: Take Teeth Cleaning From Boring To Brilliant
Protecting your child's teeth from decay is important, but it can often be a struggle to get a child to clean his teeth or have his teeth cleaned every day.
Read More
Oral Care: Kids (5-12)
Signs Of A Teething Infant
Some parents will find themselves lucky enough to have children who sail through the teething process with relatively few signs, others are not as lucky. Learn more here about the signs of teething.
Read More
Oral Care: Kids (5-12)
Silver Diamine Fluoride: What Is It?
Unlock the power of silver diamine fluoride (SDF) with Colgate Oral Care. Learn its benefits, application methods, and safety for pediatric dental health.
Read More
Oral Care: Kids (5-12)
Space Maintainers Help With a Perfect Smile
Space maintainers are a dental device used for children as they lose teeth and wait for adult teeth to grow in. Read more information here, at Colgate.com.
Read More
Oral Care: Kids (5-12)
Oral Health Effects of Stress in Children
Stress is a common problem in today's society. Stress is a reaction to the demands placed on us and our ability to cope with them.
Read More
Oral Care: Kids (5-12)
Sugar Free Snacks For Your Child's Lunchbox
As a parent, it may be difficult caring for your child's teeth, but these sugar free snacks are here to help combat cavities and promote good oral health!
Read More
Oral Care: Kids (5-12)
Surprising Oral Health Facts About Children
As a parent, you do your best to educate yourself on the issues facing your kids. It's hard to keep up, but oral health facts can help you plan ahead.
Read More
Oral Care: Kids (5-12)
Taking Care Of Your Child's Molar Teeth
As a parent, taking care of your child's teeth is an important duty. Teaching them how to brush and floss properly is important from an early age.
Read More
Oral Care: Kids (5-12)
Teach Kids Dental Care: Easy And Fun Art Projects
Teach kids dental care by using these engaging art projects to show that taking care of their teeth is necessary for a great smile.
Read More
Oral Care: Kids (5-12)
Teaching Kids To Be Healthy: How To Prevent Tooth Decay
Tooth decay occurs as a result of interactions between the bacteria inside your mouth and the food you eat. Read more at Colgate.com
Read More
Oral Care: Kids (5-12)
Teeth Grinding In Children Effects
Children grind teeth for a number of reasons, but if the condition persists, it can have a number of effects on a child's mouth. Learn more, here.
Read More
Oral Care: Kids (5-12)
Teething And Your Baby's First Teeth
Teething may be occasionally uncomfortable for babies, but it's an exciting time for parents. Prepare for your baby's first teeth in the following ways.
Read More
Oral Care: Kids (5-12)
Teething: Is A Fever With Molars Normal?
Teething isn't a pleasant time for babies, so it's normal for them to be a bit uncomfortable. But it a fever with molars normal? Learn more here.
Read More
Oral Care: Kids (5-12)
Teething Rash: Symptoms And Treatment
Teething rash, sometimes called a drool rash, is the result of excessive drool irritating a baby's face while teeth are coming in.
Read More
Oral Care: Kids (5-12)
Teething Rashes: Symptoms And Treatment For Your Baby
Did you know that your baby's salivary glands start working between 2-3 months? Your baby may drool so much that it causes teething rashes. Learn more.
Read More
Oral Care: Kids (5-12)
Teething Ring Safety Tips
Teething is hard but teething rings can provide you baby with relief. Here’s how to safely use a teething ring with tips for parents. Learn more here.
Read More
Oral Care: Kids (5-12)
Ten Things Every Children's Dentist Needs
Sometimes you don't know where to start when looking for a family dentist. Here are the top ten things you should look for in a children's dentist.
Read More.jpeg)
Oral Care: Kids (5-12)
The Baby Teething Timeline: How To Help Your Child Cope
The baby teething timeline is different for every child, but the average first tooth eruption occurs between 5 and 7 months. Learn more here.
Read More
Oral Care: Kids (5-12)
The Best Teeth Games For Kids
Getting your kids to brush their teeth isn't always easy, but having fun is. These teeth games for kids will help parents avoid typical brushing battles.
Read More
Oral Care: Kids (5-12)
The Elmo Brushing Teeth Song And Other ToothBrushing Tips For Toddlers
If you have questions about caring for your preschooler's teeth, follow these tips to help keep your child's teeth healthy and pearly white.
Read More

Oral Care: Kids (5-12)
The Purpose Of A Tooth Chart For Children
Understanding how the dentist uses a tooth chart to track the health of your child's mouth is a great way to support good oral care as he or she grows.
Read More
Oral Care: Kids (5-12)
The Symptoms Of Teething Pain
When a baby is around six months old, most parents will begin to see their child's first teeth grow in during a process known as teething.
Read More
Oral Care: Kids (5-12)
Three Dental Health Activites For Toddlers
If your stubborn little ones insist on their independence, these dental health activities for toddlers can help teach oral health and proper technique.
Read More
Oral Care: Kids (5-12)
Three Ways To Prevent Bottle Rot
Oral care starts in your baby's first year. Even before the first tooth emerges, the following precautions to prevent bottle rot are very important.
Read More
Oral Care: Kids (5-12)
Thumb Sucking: The Good, The Bad, And The Normal
How concerned should a parent be about a thumb-sucking child? As long as it doesn't get excessive, it shouldn't be at the top of a parent's worry list.
Read More
Oral Care: Kids (5-12)
10 Tips To Help Your Child Sleep While Teething
Discover expert tips to help your child sleep peacefully during teething with Colgate Oral Care. Create a soothing bedtime routine for better rest.
Read More
Oral Care: Kids (5-12)
Toddler Dental Care Tips
Setting an early precedent for conscientious dental care & by making brushing a fun part of the day, parents can help to establish healthy oral care habits.
Read More
Oral Care: Kids (5-12)
Toddler Tooth Decay And How To Prevent It
Learn how to protect your toddler's smile from tooth decay with Colgate. Get expert advice and preventive strategies to safeguard your child's dental health.
Read More
Oral Care: Kids (5-12)
Toddlers and Bleeding Gums: What Should You Do?
Toddlers and bleeding gums don't have to be a cause for alarm, but they're definitely a warning sign that your little one's oral habits should be improved.
Read More
Oral Care: Kids (5-12)
Tooth Brushing Chart To Encourage Your Little Ones To Brush
It can be hard for children to remember to brush their teeth, but there are tools a parent can use to remind & encourage children to practice good dental care.
Read More
Oral Care: Kids (5-12)
Tooth Decay In Children: All Kids Are At Risk
Tooth decay in children is more common than you may think. More than one in every four preschool-aged child in the United States has a cavity.
Read More
Oral Care: Kids (5-12)
Top 7 Teething Remedies For Babies
When your baby's first tooth breaks through the gums, you have both reached an exciting milestone. But it's a painful one. These remedies can help.
Read More

Oral Care: Kids (5-12)
What Is Baby Bottle Tooth Decay?
Your dentist can provide treatment for baby bottle tooth decay, but the best way to avoid the issue is through early awareness and prevention.
Read More
Oral Care: Kids (5-12)
Types Of Pacifiers: How To Choose The One That's Right For Your Baby
Choosing between the many types of pacifiers can be difficult. Understanding their pros and cons can help you make an informed choice for your family.
Read More
Oral Care: Kids (5-12)
Typical Baby Teething Order
There are many milestones in your baby's first year. When does the first tooth erupt? What does the timeline look like and what is the teething order?
Read More
Oral Care: Kids (5-12)
Understanding Hutchinson's Teeth
Hutchinson teeth is a dental condition that can affect a child, and you might never have heard of it. Learn more about the signs, symptoms, and treatment.
Read More
Oral Care: Kids (5-12)
What Is Macrodontia?
Macrodontia is a condition where one or more teeth grow at a different rate from the others, and don't stop when they reach average size. Learn more here.
Read More
Oral Care: Kids (5-12)
What Are Pegged Teeth?
Discover the causes and treatment options for pegged teeth, a type of microdontia, in children. Learn from experts how to address this dental condition.
Read More
Oral Care: Kids (5-12)
Use Dental Cookie Cutters To Teach Healthy Habits
If your kids are having a hard time learning to brush properly, get creative and use dental cookie cutters to make the learning process fun.
Read More
Oral Care: Kids (5-12)
Use The Teething Timeline As A Guide For Your Baby's Tooth Care
The teething timeline is a great tool for parents who want to make sure their child's teeth are well cared for from the very beginning of life.
Read More
Oral Care: Kids (5-12)
What Age Do Babies Start Teething?
According to the American Dental Association (ADA), a baby's first tooth often appears anywhere from eight months to a year of age. Learn more here.
Read More
Oral Care: Kids (5-12)
What Are Mamelon Teeth?
Ever wonder about those bumps on your child's teeth? Mamelon teeth are completely normal and usually wear off by adulthood. Learn more here.
Read More
Oral Care: Kids (5-12)
What Are The Symptoms Of Teething?
The symptoms of teething are often unpleasant for your little one. Certain symptoms are common, and there are ways for you to ease your child's discomfort.
Read More.png)
Oral Care: Kids (5-12)
What Baby Teeth Come In First?
What baby teeth come in first, and what should a parent do when they come in? Here are a few tips by Colgate on practicing early oral care for your infant.
Read More.png)
Oral Care: Kids (5-12)
What Causes Tooth Decay In Toddlers?
One way you can prevent decay is by adopting a regular cleaning routine early on. When baby teeth first appear - usually when he's around 6 months old, it's time to start gently brushing them.
Read More
Oral Care: Kids (5-12)
What Causes White Spots on Baby Teeth?
Although you don't want to panic, you do want to take action if you see white spots on baby teeth. Here are two reasons these blemishes may develop.
Read More
Oral Care: Kids (5-12)
Baby’s First Solid Foods: Healthy Teeth and Gums From the Start
Most babies are ready for their first bite of solid food between four and seven months of age. Learn more here about the signs that your baby is ready to eat solid foods.
Read More
Oral Care: Kids (5-12)
What Is A Pulpectomy?
While the enamel and dentin on the outer layers of the teeth are tough and lifeless, the pulp inside is soft, living and very sensitive.
Read More
Oral Care: Kids (5-12)
What Is A Velopharyngeal Insufficiency?
Velopharyngeal insufficiency (VPI) describes a group of communication disorders that create a resonance disturbance during speech. Learn more, here.
Read More
Oral Care: Kids (5-12)
What Is Oral Health? Teaching Preschoolers About Dental Hygiene
A certain degree of independence is a big step in your child's development. This includes answering (and applying) the question: What is oral health?
Read More
Oral Care: Kids (5-12)
What Is Thrush In Babies?
Thrush, which is caused by overgrowth of yeast in the mouth, can be a common concern for new parents. What is thrush in babies? Find out more, here.
Read More
Oral Care: Kids (5-12)
What Parents Should Know About Mouthwash For Children
Toothpaste and mouthwash for children often feature kid-friendly flavors and graphics that make mouth care a bit more fun. Is your child ready to swish?
Read More
Oral Care: Kids (5-12)
What To Do For A Child With A Toothache?
Most of the time, a toothache is caused by injury to the tooth or a cavity. Here are some things that you can do to help your child when he has a toothache.
Read More
Oral Care: Kids (5-12)
What To Know About Your Smiling Baby
A smiling baby is the beginning of the end of the newborn stage, and it marks your child's first attempts at real social interaction. Learn more here about this exciting time.
Read More
Oral Care: Kids (5-12)
What To Look For In Toddler Toothpaste
When your child begins to get their first baby teeth, it's natural, to start thinking about the best way to care for them so they can have healthy teeth.
Read More
Oral Care: Kids (5-12)
What You Need To Know About Baby Tongue Thrust
Find out more about oral care and oral health for infants, including when to start brushing baby teeth, baby toothpaste, and more, from the Colgate Oral Care Center.
Read More
Oral Care: Kids (5-12)
When Do Babies First Smile? What Do Those Toothless Grins Really Mean?
Learn all about your baby's first smile: when your baby will start to smile, the various types of baby smile, and tips to encourage your baby to do it!
Read More.png)
Oral Care: Kids (5-12)
When Do Babies Get Their First Tooth?
Once your baby starts to show signs of teething, the biggest question on your mind will likely be. Learn more about a baby’s teething order, here.
Read More
Oral Care: Kids (5-12)
When Do Babies Start Teething & How Long Does It Last?
First-time parents who have heard the stories are probably wondering, when do babies start teething and how long does it last? Learn more.
Read More

Oral Care: Kids (5-12)
When Do Baby Teeth Fall Out?
Learn all about your child's baby teeth: when they'll lose their milk teeth and grow their adult teeth, what to do when it happens, and tips to support your child.
Read More
Oral Care: Kids (5-12)
When Little Ones Lose Baby Teeth: Six Special Ways To Celebrate
Go all out with celebrations when your little ones lose baby teeth, or keep it simple. Either way, the important thing is to make it special.
Read More
Oral Care: Kids (5-12)
When To Expect Your Baby's First Laugh And Other Milestones
What is more wonderful than hearing your baby's first laugh? Learn when they're supposed to start laughing, ways to make them laugh, and all the information you need.
Read More
Oral Care: Kids (5-12)
When To Take Your Child To The Dentist For The First Time
The American Dental Association and the American Academy of Pediatric Dentistry recommend that a child's first visit should be when the first tooth erupts in the mouth.
Read More
Oral Care: Kids (5-12)
When To Take Your Baby To The Dentist And Doctor: Dental Care, Teething Issues And More
Pediatric dentists and family dentists agree that you should take your baby to the dentist for the first time no later than the child's first birthday.
Read More
Oral Care: Kids (5-12)
Which Baby Teeth Fall Out First?
The first baby tooth is just as memorable as the first adult tooth. Knowing which baby teeth fall out first can help you and your kids enjoy the milestone.
Read More
Oral Care: Kids (5-12)
Using A Permanent Teeth Chart To Track Your Child's New Teeth
Learn to track your child's tooth eruption using a dental chart. Monitor your baby's emerging teeth and anticipate the arrival of your kid's next permanent tooth.
Read More
Oral Care: Kids (5-12)
Why Do Babies Suck Their Thumbs?
Find out more about oral care and oral health for infants, including when to start brushing baby teeth, baby toothpaste, and more, from the Colgate Oral Care Center.
Read More
Oral Care: Kids (5-12)
Why Do Kids Lose Their Teeth?
Losing a tooth is a big moment for any child. As a parent, you want to be able to make those moments memorable. When do kids lose their teeth?
Read More
Oral Care: Kids (5-12)
Why Teething Tablets Should Be Avoided
Some options for a teething baby are safer than others. Teething tablets, for example, are one solution parents shouldn’t rely on. Learn more, here.
Read More

Oral Care: Kids (5-12)
Will Tongue Thrust Treatment Benefit Your Child?
Babies naturally push their tongues forward when they're fed, but if this behavior doesn't dissipate with age, they may need tongue thrust treatment.
Read More
Oral Care: Kids (5-12)
Your Child Has a Mesiodens. Now What?
Discover everything about supernumerary teeth or mesiodens: why your child has extra teeth, how to manage mesiodens, and the solutions available for your child.
Read More
Oral Care: Kids (5-12)
When to Pull a Loose Tooth
Explore our method for fast and painless baby tooth removal at home! Get tips, precautions, and aftercare advice for an easy tooth extraction process for kids.
Read More
Oral Care: Kids (5-12)
Natural Toothache Pain Relief for Your Child
Discover reliable toothache relief for kids with natural remedies. Soothe your child's discomfort until you can visit with a dentist. Learn more here!
Read More

Oral Care: Kids (5-12)
Caring for Your Kid's Teeth
Whether you decide to introduce dental care to your child at the onset of the first tooth or wait a few months until he reaches his toddler years, caring for your kid's teeth is always filled with its share of challenges. Read more at Colgate.com
Read More
Oral Care: Kids (5-12)
Dental Hygiene for Kids
It is never too early to encourage healthy dental hygiene for kids. Your child's teeth are at risk of decay as soon as they first erupt.
Read More

Oral Care: Kids (5-12)
How to Get Kids to Eat Healthy Dinners
In households across America, Moms struggle to have their children eat healthy dinners. Chicken nuggets, pizza, and hamburgers… Read more at Colgate.com
Read More
Oral Care: Kids (5-12)
Is Swallowing a Tooth Dangerous?
Swallowing a tooth or a tooth fragment is not unusual. It can happen when your kid's tooth is loose, during a sporting event or in an injury. Learn more.
Read More
Oral Care: Kids (5-12)
Make Your Child's First Dental Visit Stress Free
Your child's first dental visit is an exciting milestone, and there's no reason it should be frightening. As long as you… Read more at Colgate.com
Read More
Oral Care: Kids (5-12)
National Children's Dental Health Month: Five Ways to Celebrate
With a focus on hygiene and health, National Children's Dental Health Month may be even more important than Valentine's Day this February.
Read More
Oral Care: Kids (5-12)
Personalized Pillow Cases to Commemorate Your Child's Lost Teeth
Personalized pillow cases are a fun way to commemorate milestones in your little one's life, such as lost teeth. You have many choices when it comes to...
Read More
Oral Care: Kids (5-12)
Preparing for Your Baby's First Molar
Watching your baby's teeth develop is an exciting milestone, but it can also be an overwhelming time for a parent. What can you expect from a first molar?
Read More
Oral Care: Kids (5-12)
How to Smile for School Pictures: Give Them the Perfect Smile
One of the most important elements in taking good school pictures has to be the smile. Children will feel more comfortable… Read more at Colgate.com
Read More
Oral Care: Kids (5-12)
Should You Use Baby Teeth Wipes?
Young children are especially vulnerable to cavities. Are baby tooth wipes the right option for preventing decay? Here's what to know about these products.
Read More
Oral Care: Kids (5-12)
Tiny Teeth
Elevate your child's oral care routine with expert tips tailored for tiny teeth. Get essential tips to ensure your child's dental health from Colgate.
Read More
Oral Care: Kids (5-12)
3 Things to Know: Taking Your Special-Needs Child to the Dentist
The dentist is a scary place for many children, and this is no different for children with special needs. Here are some tips on how to help your little one cope with their first dentist visit.
Read More
Oral Care: Kids (5-12)
Cold Sores in Children: Here's What to Know
If you're a parent, you may be concerned if your child develops a mouth sore. Here's what to know about cold sores in children and how to treat them.
Read More
Oral Care: Kids (5-12)
Fun Teeth Facts for Kids: Part II
Kids love learning about what happens inside of the human body. These teeth facts for kids can provide skills to maintain their health for a lifetime:
Read More
Oral Care: Kids (5-12)
Baby Bottle Tooth Decay: Shielding Your Baby's Teeth
What is baby bottle tooth decay? Learn more about tooth decay that occurs in infants or toddlers.
Read More
Oral Care: Kids (5-12)
Six Ways Healthy Kids Can Make Healthy Choices
Health hinges on kids' discovery of the daily choices that determine lifelong well-being. But they only make healthy choices if their parents promote them.
Read More
Oral Care: Kids (5-12)
Baby's First Teeth: Should You Use Toothpaste?
Learn about the optimal timing for introducing your baby to toothpaste brushing and nurturing proper oral care habits. Get valuable insights and guidance here.
Read More
Oral Care: Kids (5-12)
The "Candy Strategy" for a Cavity-Free Home
By: Dr. Natalie Carr-Bustillo, DDS, MS
Board Certified Pediatric Dentist
Read More
Tooth Extraction
12 Common Tooth Extraction Tools
The image of dental tools can conjure your fear of the dentist. Ease your concerns by learning more about the most common tooth extraction tools used.
Read More
Tooth Extraction
Alcohol After a Tooth Extraction: Is It OK To Have a Drink?
If you've recently had a tooth removed, you might want to know if you're allowed to drink alcohol after a tooth extraction. Here is your answer.
Read More
Tooth Extraction
Bone Infection After a Tooth Extraction: Symptoms, Treatment, and Prevention
While most extractions are safe and straightforward, in some cases, complications can arise, including a bone infection after a tooth extraction.
Read More
Tooth Extraction
Can I Drink Coffee After A Tooth Extraction?
It's important to take care of your mouth after an extraction. If you've ever wondered, Can I drink coffee after a tooth extraction? here is your answer.
Read More

Tooth Extraction
Dry Socket Prevention: Caring For Yourself After An Extraction
A tooth extraction should be uneventful, and if you follow a few dry socket prevention tips, your recovery will be just as smooth. Find out more, here.
Read More
Tooth Extraction
Finding A Bone Spur In Gum Tissue? Here's What To Do
Feeling a bone fragment in your gums? You may have a bone spur in gum tissue, but the condition is common and treatable through a visit to your dentist.
Read More
Tooth Extraction
How Socket Preservation Helps After A Tooth Extraction
Socket preservation is very important after you get a tooth removed, but whether or not you need it depends on the nature of your procedure. Learn more.
Read More
Tooth Extraction
What's the Best Pain Relief after a Tooth Extraction?
Ibuprofen and Acetaminophen Together May Give Profound Pain Relief With Fewer Side Effects After Dental Surgery. Learn more about the benefits of these two pain medicines.
Read More
Tooth Extraction
Pain After Having A Tooth Removed: 3 Tips To Help Your Kids Keep Brushing
If a tooth does not fall out on its on and has to be pulled, it can be tender and cause pain for several days. Find out more about pain after having a tooth removed, here.
Read More
Tooth Extraction
Use Caution When Taking Prescription Medications
Sometimes dentists prescribe opioids to patients for pain relief after a dental procedure. Here is a brief description of opioids and some questions to ask your dentist before taking these medications.
Read More
Tooth Extraction
When Surgical Extraction Of Teeth Is Necessary
Although many of your teeth are easily removable, it's occasionally more complicated. Here's why the surgical extraction of teeth may become necessary.
Read More
Tooth Extraction
Serious Tooth Infections
Oral and maxillofacial surgeons are trained to treat infections in the head and neck region, as some infections may spread beyond teeth. Learn more here.
Read More
Tooth Extraction
Tooth Removal 101
Learn more about tooth extractions and the removal of wisdom teeth. Find out more about what will cause tooth extractions, the procedures, infections, and recovery.
Read More
Tooth Extraction
Tooth Extraction: What You Need To Know
Tooth extraction is the removal of a tooth from its socket in the bone. If you are facing a tooth extraction, it can seem a little daunting and nerve-wracking.
Read More
Tooth Extraction
Pulling A Tooth At Home: When It's OK And When It's Not
The loss of baby teeth can be an exciting time for both parents and children. Learn about the dos and don'ts of pulling a baby tooth.
Read More
Tooth Extraction
Tooth Extraction Healing Time: What's Normal?
Sometimes, it's necessary to have a tooth pulled. Here are guidelines on typical tooth extraction healing time and tips for a speedy recovery.
Read More
Dental Product Guidance
5 Benefits Of Chewing Gum
Did you know that there are benefits of chewing gum? Learn more on how gum may improve your oral health.
Read More
Dental Product Guidance
5 Places To Donate Your Extra Toothbrushes & Toothpaste
If you have extra unused, unopened, and unexpired personal care items and toiletries, you can donate to these 5 organizations to benefit those in need.
Read More
Dental Product Guidance
A Toothpaste Holder Contains The Mess
If you have little kids, you've probably gone into the bathroom and found toothpaste everywhere. It's sticky and hard to clean… Read more at Colgate.com
Read More
Dental Product Guidance
Basics Of Brushing For Kids: What Toothpaste Is Right For Your Toddler?
By knowing the basics of brushing for kids of every age, you can take excellent care of your child's mouth and set him up for healthy smile success.
Read More
Dental Product Guidance
The Benefits of Alcohol-Free Mouthwash
Mouthwash may appeal to those who need a quick on-the-go clean. Alcohol free mouthwash, however, is a product whose value depends on the individual.
Read More
Dental Product Guidance
Best Toothpaste To Use For Safe And Fast Whitening
The best toothpaste to use for fast results depends on your oral care needs. Here are four things to keep in mind when making a selection.
Read More
Dental Product Guidance
Charcoal Toothpaste: What Is It?
Charcoal toothpaste is gaining popularity as a new whitening method. Learn more here.
Read More
Dental Product Guidance
Choosing The Best Toothbrush For You
The best toothbrush for the job depends on a variety of things that are unique to you. Here are three things to look for in a product that does this.
Read More
Dental Product Guidance
Dental Technology: 3D Printed Teeth And More
Its exciting applications for dental care include custom 3D printed teeth, dentures and a variety or other tools for patients and practitioners
Read More
Dental Product Guidance
Should You Choose a Mouthguard That Includes a Lip Guard?
Mouth guards come in a variety of styles and shapes. Should you choose one with a lip guard mouthpiece? Find out more, here.
Read More
Dental Product Guidance
Does Mouthwash Expire?
Does mouthwash expire? Nothing lasts forever, including that bottle of mouthwash you have stashed away. Learn more about the shelf life of mouthwash.
Read More
Dental Product Guidance
Finding The Best Tongue Cleaner
A tongue scraper is the best tongue cleaner out there. Here's why you should invest in one, how to use it and what to consider when buying one. Learn more.
Read More
Dental Product Guidance
5 Types Of Dentist Recommended Toothpaste
If you're confused as to which toothpaste is right for your family, talk to your dentist and consider a few forms of dentist recommended toothpaste.
Read More

Dental Product Guidance
How Gluten-Free Toothpaste Keeps You Clean and Healthy
There are many types of toothpastes available today, but it may not have occurred to some to consider gluten free toothpaste. Here's how it works:
Read More.png)
Dental Product Guidance
How Long Will A Travel Size Toothpaste Last?
The amount of toothpaste you use makes a huge difference in the length of time a travel size toothpaste will last you, so we did some calculations.
Read More
Dental Product Guidance
Is a Bamboo Toothbrush Right for You?
To reduce the use of plastic at home, some people are switching to bamboo toothbrushes. Learn if a bamboo toothbrush is an eco-friendly and healthy choice.
Read More
Dental Product Guidance
Is An Electric Toothbrush Right For My Child?
Anything that boosts your child's interest in oral care can be helpful in preventing plaque and cavities. An electric toothbrush for kids may be the answer for a child who doesn't like to brush.
Read More
Dental Product Guidance
Is Baking Soda Mouthrinse Safe And Effective?
While there are many mouthwashes on the market today, would a baking soda mouthrinse be safe and effective for daily use?
Read More
Dental Product Guidance
Is Flossing Hard? Interdental Brushes May Be The Answer
Cleaning in between teeth and around gums is important if you want to maintain a healthy mouth. Many people use floss to clean
Read More
Dental Product Guidance
Is There a Special Toothbrush for Braces?
While you might not need to use a special toothbrush for braces, you may need to increase how frequently you brush. Learn about toothbrushes for braces.
Read More
Dental Product Guidance
Is Woven Dental Floss Best? Finding The Right Floss For You
The rows of choices at the drugstore could turn this daily routine into a head-scratcher. How does woven dental floss stack up to other varieties?
Read More

Dental Product Guidance
Kids Toothbrushes: What To Buy For Your Child
Following a few simple guidelines can help you choose a toothbrush that cleans your child's teeth effectively and encourages good dental care habits in the process.
Read More
Dental Product Guidance
Making A Natural Mouthwash Recipe With Essential Oils
Although many people are OK with the average commercial mouthwash, some prefer a natural mouthwash recipe to prepare themselves. Here are the essentials.
Read More

Dental Product Guidance
Mouth Guards: Everything You Need To Know
Dentists might recommend mouth guards for their patients who grind their teeth at night, play contact sports, or have TMJ problems or sleep disorders.
Read More
Dental Product Guidance
Natural Toothache Relief
Most toothaches are caused by sensitivity to the nerve (pulp) of the tooth due to decay, injury to the tooth, and infection.… Read more at Colgate.com
Read More
Dental Product Guidance
Personalized Toothbrushes: Fun For Kids And Sanity-Saving For Parents
If you, like many parents, struggle to get your children to brush their teeth, you may be at your wit's end. In fact, you might… Read more at Colgate.com
Read More
Dental Product Guidance
Selecting Dental Products 101
Learn more about selecting dental products to find the right toothbrushes, toothpaste, and mouthwashes for you and your family. A healthy smile starts today, with Colgate!
Read More
Dental Product Guidance
Should You Consider A Water Flosser?
Flossing is important for good oral health. If you have difficulty using string floss, talk to your dentist about alternatives, like a water flosser.
Read More
Dental Product Guidance
Should You Try Coconut Toothpaste?
Should you seek oral care products that contain coconut? Visit Colgate IN and learn more about the health benefits of coconut for your oral health.
Read More
Dental Product Guidance
Should You Use Homemade Toothpaste?
Is it a good idea to make your own toothpaste? Here's what you need to know before you decide to make homemade toothpaste and how it compares.
Read More
Dental Product Guidance
5 Natural Ingredients in Fluoride-Free Toothpaste
Non fluoride toothpaste is an effective alternate for those who are sensitive to fluoride. Here are six natural ingredients that still protect your teeth.
Read More
Dental Product Guidance
Soft vs. Hard Toothbrushes: What's Right For You
As a general rule, however, dentists recommend choosing a toothbrush with soft bristles, instead of one considered hard or even medium.
Read More
Dental Product Guidance
Teeth Whitening Toothpaste: Does It Work?
If surface stains are contributing to your teeth's discoloration, you can try using a teeth whitening toothpaste to improve their appearance.
Read More

Dental Product Guidance
The Facts About Abrasive Toothpaste
Abrasive toothpaste can damage tooth enamel. Here's how you can keep your enamel safe from abrasive toothpaste ingredients.
Read More
Dental Product Guidance
Tooth Powder vs. Toothpaste: What's Right For You?
Tooth powder vs. toothpaste: which is better? Find out more about usage and the advantages of commercial toothpastes in comparison to tooth powders, here.
Read More
Dental Product Guidance
Do You Have a Toothpaste Allergy?
While you might not hear about toothpaste allergy too often, it still can occur. Here's some important information to know and what to look for.
Read More
Dental Product Guidance
Transcutaneous Electrical Nerve Stimulation (TENS) Therapy in Dentistry
Can transcutaneous electrical nerve stimulation help relieve pain and discomfort caused by certain dental problems? Fin dout more here.
Read More
Dental Product Guidance
Using Tartar Control Toothpaste For Healthy Teeth And Gums
Brushing your teeth properly using tartar control toothpaste regularly is an important part of establishing and maintaining good oral health.
Read More
Dental Product Guidance
Should You Use An Electric Toothbrush?
There are many types of toothbrushes on the market, including electric toothbrushes. Find out how they help boost your oral hygiene with Colgate®. Click here!
Read More
Dental Product Guidance
5 Most Common Toothpaste Ingredients
Every morning and night, you squeeze a small amount of toothpaste onto your toothbrush. Have you ever wondered what is in toothpaste?
Read More
Dental Product Guidance
Whitening Products Available from Dentists
The best way to ensure teeth whitening at home is to seek the whitening products that are available from dentist. Consult with professionals to know exactly what to use and how to use at-home whitening products.
Read More
Dental Product Guidance
What is Sodium Lauryl Sulfate and Is It Safe?
Many household cleaners, detergents and even cosmetics and toothpastes you commonly use contain sodium lauryl sulfate, or SLS. Learn about it, here.
Read More
Dental Product Guidance
How to Choose the Best Teeth Whiteners
Daily brushing and flossing keep teeth clean and free of decay – but if they've lost their sparkle or are looking yellow, don't worry! We've rounded up the best teeth whitening options so that you can select the best ones for you – and smile even wider.
Read More
Dental Product Guidance
Choosing The Right Toothbrush
Selecting the right toothbrush is the first step to optimize a healthy oral care routine. Click here to find the right toothbrush for your oral care need with Colgate.
Read More
Dental Product Guidance
Antiseptic Vs. Antibacterial Mouthwash: What's The Difference?
Mouthwash can freshen your breath and protect against cavities. When it comes to antiseptic vs. antibacterial mouthwash, is one better than the other?
Read More
Dental Product Guidance
Benefits Of Cetylpyridinium Chloride Mouthrinse
Mouthrinse can be a good addition to your oral care routine. Here's why your dentist may recommend one containing cetylpyridinium chloride.
Read More
Dental Product Guidance
Is Oxygenated Toothpaste Right For You?
If you want to reduce oral bacteria or you want whiter and brighter teeth, an oxygenated toothpaste may be the answer. Here's why.
Read More

Dental Product Guidance
What's The Difference Between A Retainer And A Night Guard?
What's the difference between a retainer and a night guard? Although they may look similar, these devices serve different functions. Here's what to know.
Read More
Dental Product Guidance
Why Does Mouthwash Burn? Tips on Finding the Product for You
Mouthwash can be a great addition to your oral care routine, but it can cause irritation for some patients. Why does mouthwash burn? Find out more.
Read More
Dental Product Guidance
Aloe Vera Toothpaste: What are the Benefits?
Why use Aloe Vera Toothpaste? Aloe Vera is known for its benefits in controlling bacteria that causes cavities than other commercial toothpaste.
Read More
Dental Product Guidance
CBD and Oral Care. Are There Benefits?
If you're interested in incorporating CBD charcoal toothpaste & CBD mouthwash into your oral care routine read this article from Colgate.
Read More
Dental Product Guidance
What are Toothpaste Tablets?
How can you incorporate toothpaste tablets into your oral care routine? Not only are they convenient, travel-easy, but they are also environmentally friendly.
Read More
Dental Product Guidance
How Does Enzymatic Toothpaste Work?
What is enzyme-powered toothpaste? Click here to learn more about enzyme toothpaste, as well as the benefits for your teeth and gums with Colgate.
Read More
Dental Product Guidance
Oral Health Tips for College Students
There are different ways to keep up oral health while in college. Click here to learn more on how to care for your oral health with Colgate®.
Read More
Dental Product Guidance
What is a Toothpaste Color Code?
One popular hoax in recent years had to do with a toothpaste color code on the bottom of the tubes. Find out what the toothpaste color code really means.
Read More
Dental Product Guidance
4 Questions You Might Have About Chlorhexidine Gluconate Mouthwash
Chlorhexidine gluconate is used to treat gingivitis, another name for mild gum disease. Learn more about the benefits of using this mouthwash here.
Read More
Dental Product Guidance
Teeth Whitening Pens 101
If you're looking for a last-minute touch-up to your smile, a teeth whitening pen might be just the thing. Here's what makes it work, and how to use it.
Read More
Mouth Sores and Infections
All About Herpes in the Mouth
Of all the possible sores found in the mouth and on the lips, one of the most common is herpes in the mouth. Read on to learn about how herpes in the mouth is contracted, how prevalent it is among Americans, how it is caused, and treatments that can relieve the symptoms.
Read More
Mouth Sores and Infections
Antibiotic Names And Their Use In Dentistry
Dentists routinely prescribe antibiotics. They may do this prior to treatment when a patient has a medical condition that could be made worse by dental treatment from the normal bacteria found in the mouth. Some procedures also require antibiotics as part of aftercare.
Read More
Mouth Sores and Infections
Bad Taste in Mouth: Causes and Treatment
A strange or nasty taste in your mouth is an annoyance at best, and at worst it could be a symptom of a serious medical condition. If you have a bad taste that never goes away or returns regularly, you should talk to your dentist or physician. The condition could be due to a problem in your mouth or another part of your body or due to medications or supplements that you're taking.
Read More
Mouth Sores and Infections
Black Spots On Tongue: Causes & Treatment Options
The spots, patches and discoloration that tongues can develop may be harmless, but occasionally they're a sign of something serious. Black spots on tongue could range from tiny dots to conspicuous black areas, which look especially alarming. If you notice black dots, tell a dentist or physician about them and get a proper diagnosis.
Read More
Mouth Sores and Infections
Can Stress and Other Risk Factors Lead to Canker Sores?
Of all the different types of mouth sores, canker sores might be the most mysterious. It isn't well understood why people get them. Canker sores develop on the inside of the mouth, cheeks and lips and on the tongue and gums. Although they aren't contagious, the tingling pain can be unpleasant. If you have a canker sore, stress or anxiety could be a potential influence.If you think your canker sores are connected to stress levels, learning to recognize and manage your triggers might help you avoid a flare-up.
Read More
Mouth Sores and Infections
Canker Sore on Tonsil? Here's How To Deal
It feels like a sore throat, but you're not sick: What could it be? If you grab a mirror and peer into the back of your throat, you might find that what feels like a sore throat or swollen tonsils is actually a canker sore. Canker sores can affect any part of the mouth, including the gums, teeth, and yes, your tonsils. The good news is that it likely won't merit a trip to the doctor, but the bad news is that canker sore on tonsil pain can really disrupt your daily activities. Learn how to deal and how to avoid canker sores in the future so you can continue to eat, drink, and enjoy life without the pain.
Read More
Mouth Sores and Infections
Complex Canker Sores: What They Are And How They're Treated
Almost everyone's had a canker sore before: those annoying, painful little sores that sometimes result from eating too much acidic food or accidentally biting the inside of your cheek. But for some people, canker sores are a serious problem. Complex canker sores can last for weeks and even leave scars. If you have a canker sore that's more than just a minor annoyance, it's best to educate yourself before seeing your health care provider about treatment and prevention options.
Read More
Mouth Sores and Infections
Dental Abscesses And Infection In Gums: What You Need To Know
You're relaxing after a day at work or spending time with your family when you feel a sharp pain in your mouth. If you have a history of dental problems – such as infection in gums, teeth or even cavities – the pain could be related to a dental abscess.There are two types of dental abscess: A periapical, or tooth abscess, affects the root of the tooth. The other type, a periodontal (gum) abscess, affects the gums. The latter usually occurs in severe cases of periodontal disease, when the gums have pulled away from the teeth, causing pockets to form. Both types of abscess consist of small pockets that fill with bacterial pus. With the right treatment, you can recover from either type and regain control of your oral health.
Read More
Mouth Sores and Infections
Dental Fistula: Identify, Treat, and Prevent
If you notice discomfort or swelling on the side of your face, it can be many things. It may be a parotid gland infection. Read on to learn the signs and symptoms to get the care you need and learn about preventing parotid gland swelling in the future.
Read More
Mouth Sores and Infections
8 Common Oral Infections
Oral bacteria can cause viruses, tooth decay, gum disease and other common mouth infections in both children and adults.
Read More
Mouth Sores and Infections
Enlarged Papillae: Causes, Symptoms, and Treatment of Tongue Bumps
Did you ever have one of those little tongue bumps that just showed up out of nowhere? The kind that drives you crazy, sometimes to the point where you try to remove it just to get rid of it? These tongue bumps (enlarged papillae) may appear for one of many reasons.
Read More
Mouth Sores and Infections
Everything You Need To Know About MRSA
MRSA, or Methicillin-resistant Staphylococcus aureus, is a serious type of bacteria resistant to antibiotics in the penicillin family.
Read More
Mouth Sores and Infections
Fibroma Treatment
Fibromas are commonly found at the oral cavity – essentially outgrowths of tissue that can come hard or soft and white or pink, depending on its makeup. Rest assured they're usually benign. Here's what causes one to develop and what types are often found in and around the mouth. You should also know how and where they develop, as well as which treatment is recommended for those who may have one.
Read More
Mouth Sores and Infections
Five Approaches To Burning Mouth Syndrome Treatment
Burning mouth syndrome (BMS) is an irritating condition that affects about 1 percent of the adult population, and the cause can be very difficult to pinpoint. Therefore, it's often difficult to treat as well. But with the right combination of diet, medication and physician consultation, burning mouth syndrome treatment can successfully target the things that aggravate the structures in and around the mouth and tongue.The pain and burning of BMS can involve the tongue, cheeks, the back of your palate and throat and even possibly your gums. It can also give way to other symptoms, such as tingling and numbness, a bitter or metallic taste and a dry mouth. Here's what treatment may look like per some of these symptoms:
Read More
Mouth Sores and Infections
Five Common Oral Diseases and How They're Treated
Oral care doesn't just keep your teeth strong; it can have a significant effect on your general wellness, too. Nearly one in 10 people have some sign of poor dental health, and in some instances that number goes up to almost 100 percent. The most common oral diseases are:
Read More
Mouth Sores and Infections
Five Burning Tongue Causes and Solutions
If you're experiencing a burning sensation from your tongue or in your mouth, it may indicate a condition known as Burning Mouth Syndrome, also known as BMS. What exactly does this indicate about your health? What are the potential causes, and how do they result in discomfort? We're here with answers to your top questions and guidance on what you can do for relief.
Read More
Mouth Sores and Infections
Geographic Tongue: Causes, Symptoms And Care
Have you ever looked at your tongue in the mirror and thought you were looking at a road map of Florida? Or maybe on another day it looked more like Pennsylvania. You may have a condition called geographic tongue. Don't be alarmed, though. This benign condition is not a threat to your health.Here are some interesting facts about this disorder (also referred to as migratory glossitis or wandering rash of the tongue) that you should know.
Read More
Mouth Sores and Infections
Glossitis: Symptoms, Causes And Treatment
Has your tongue ever been swollen or inflamed, and you’re not sure why? You might have been experiencing glossitis, which is the inflammation of the tongue.
Read More
Mouth Sores and Infections
Herpes Esophagitis: Symptoms, Treatment Options, and Prevention
If you've ever had a cold sore on your lip or mouth, you most likely have herpes simplex virus type 1 (HSV-1). While the name might sound intimidating at first, this is a widespread virus that affects people worldwide.
Read More
Mouth Sores and Infections
Herpes On The Tongue
How does herpes on the tongue happen? Better yet, how can you prevent herpes from infecting your tongue? We'll give the lowdown on oral herpes on the tongue, ways to avoid an outbreak, and how to treat the condition.
Read More
Mouth Sores and Infections
Herpetic Lesions: Symptoms, Treatment And Prevention
According to the World Health Organization (WHO), 67 percent of the world's population younger than 50 years old has herpes simplex virus type 1 (HSV-1). HSV-1 is generally spread through oral-to-oral contact and is commonly known as cold sores or fever blisters. These blister-like herpetic lesions can be spread from the mouth to other parts of the body. Since approximately 3.7 billion people carry this virus, it is very important to understand the symptoms and management of the condition.
Read More
Mouth Sores and Infections
How Blisters in Mouth Tissue Occur and How to Treat Them
Finding blisters in mouth tissue isn't unusual; it can occur in all age groups and for a variety of reasons. It is therefore important for you to identify the contributing factors for your specific condition. In certain instances, these lesions can be contagious or pose a greater risk for infection.These ulcers can occur on the lips, tongue, gums, inner cheeks, roof or floor of the mouth, and they can arise from tissue trauma, non-communicable illness or something very often transmitted.
Read More
Mouth Sores and Infections
How Salt Water Mouth Rinse Benefits Oral Health
A salt water mouth rinse is useful for a number of different reasons. It's a great option for anyone who has a sore throat, gum sores or recently underwent dental procedures. It doesn't take the place of modern dental hygiene, but is used as a supportive measure for adults and children alike.
Read More
Mouth Sores and Infections
How to Kill Mouth Bacteria and Keep It Away
Did you know there’s a party going on in your mouth? That’s right, according to News in Health, your mouth is home to over 700 species of microbes, including bacteria, fungus, and more. Some bacteria can be helpful, while others can be associated with tooth decay and bad breath. Luckily, figuring out how to get rid of harmful bacteria isn’t that hard. It all comes down to a good oral care routine. Find out what that looks like!
Read More
Mouth Sores and Infections
How To Manage Chemotherapy Mouth Sores
The drugs used to fight cancer may potentially affect an oncology patient's oral health. Chemotherapy mouth sores are a common side effect of treatment that can affect the lips and mucous membranes of the mouth. Drugs affect people in different ways, and there is no way to predict who will experience side effects, but knowing what to look out for and how to relieve discomfort may help you reduce chemotherapy's impact on your oral health.
Read More
Mouth Sores and Infections
How to Prevent a Cold Sore Scab
Cold sores are no fun. Besides being painful, they can make the most confident person self-conscious. Ideally, you want them to go away as quickly as they happen. And you don’t want them to leave a scar. Here’s what to do and not do if you suffer from cold sores.
Read More
Mouth Sores and Infections
How To Prevent Canker Sores
Canker sores can seem to suddenly appear for no reason. One minute your mouth is fine, and the next you have an annoying, sometimes painful lesion on your gums or cheek. While canker sores usually heal without treatment from a dentist or doctor, taking steps to help prevent them from developing can save you from the lingering discomfort they often cause. The key to stopping canker sores is to figure out what triggers them in your mouth.
Read More
Mouth Sores and Infections
How To Improve an Oral Cancer Prognosis
While oral cancer makes up only three percent of all cancer diagnoses in the United States, it’s important to be aware of the symptoms and risks.
Read More
Mouth Sores and Infections
Infection Control Information and Tips: More Than Just Toothbrushing
Infection control is important both in the home and when you visit your dentist. It's about far more than just toothbrushing. In fact, it's about keeping any bacteria at bay that can harm your teeth and your overall health.
Read More
Mouth Sores and Infections
Lesion In Mouth: Symptoms, Causes And Treatments
Read on to learn about the common conditions that can cause mouth lesions along with their symptoms and treatment options.
Read More
Mouth Sores and Infections
Lingual Tonsils And Your Immune System
You probably only notice your lingual tonsils — more simply known as just tonsils — when they're infected. Suddenly, swallowing is painful and you notice that the lumps in the back of your throat are red, swollen and might also be covered in white patches.Your tonsils are the first line of defense in your immune system, and the antibodies they produce fight the viruses or bacteria that invade your throat. However, sometimes the tonsils themselves become infected, and if you suffer from repeated bouts, it may be better to have your tonsils removed. Learning about how the tonsils function in relation to the immune system and speaking with your doctor about your experience with infections can help you be more informed about tonsil removal.
Read More
Mouth Sores and Infections
Managing A Blood Blister In The Mouth
If you've ever had the displeasure of accidentally biting your cheek while chewing food, you might recall a sore forming in the area. While mouth sores caused by cheek biting are usually no cause for concern, what if you notice a sore in the mouth that's filled with blood?
Read More
Mouth Sores and Infections
Managing Burning Mouth Syndrome
Burning mouth syndrome, or BMS, is a chronic dental condition that is often described as a burning sensation felt on the tongue, cheeks, lips or entire mouth. For those who deal with this issue, its symptoms can be both frustrating and painful, impacting the way in which they are able to live their lives--the condition generally appears suddenly and without warning. For most people diagnosed with this syndrome, its sudden onset can be likened to the sensation felt when your mouth is scolded by an extremely hot food or drink. Consequently, speaking with a dental health professional for prompt diagnosis is the first step in managing symptoms.
Read More
Mouth Sores and Infections
Is There Good Bacteria In Your Mouth?
Learn more about the good bacteria in your mouth and how it is responsible for keeping your mouth healthy with this article from Colgate.
Read More
Mouth Sores and Infections
Mouth Piercings Aftercare
Body piercings, including mouth piercings, are a well-known form of self-expression. A tongue piercing, also known as an oral piercing, penetrates the tongue from one side to another, usually directly through the center of the tongue. Here are a few options for other oral piercings you can consider:
- Midline: Along the midline of the tongue (one of the most common sites)
- Frenulum: Underneath the tongue
- Tongue web: Two tongue piercings placed side-by-side
- Horizontal: Placed horizontally on the tongue
- Side tongue: Placed on the side of the tongue

Mouth Sores and Infections
Mouth Rash: Treatment And Prevention
Do you have a rash around your mouth, and you're wondering what it's from? First off, it's a great question. Why? Because when it comes to mouth rash, prevention is the key. It's important to know what's causing your mouth rash so that you can stay clear of any triggers. As you read on, we'll go into the signs, symptoms, and causes associated with mouth rash in adults, as well as how to treat and prevent it. That way, you can stay comfortable, healthy, and rash free.
Read More
Mouth Sores and Infections
Oral Care For Kids With Canker Sores
If your child suffers from painful canker sores, don't neglect his routine oral care. Keeping your child's mouth clean will prevent more sores from appearing and will reduce the healing time.
Read More
Mouth Sores and Infections
Oral Fungus Causes Common Mouth Infection
Oral thrush, also called candidiasis, is a fungal infection that creates painful white sores in your mouth. However, in some cases, the mouth will not produce white spots but look red and sore instead. Oral thrush can be a bit unsightly, but there’s no need to worry! The gum fungus this infection causes can be treated and, even better, prevented. Here’s what you need to know about treating your oral thrush.
Read More
Mouth Sores and Infections
Oral Hairy Leukoplakia and Its Effects
Oral hairy leukoplakia may sound like some weird disease that causes hair to grow on your tongue, but hair growth in your mouth luckily isn't a symptom at all.
Read More
Mouth Sores and Infections
Oral Mucositis Treatment Advancements May Provide Relief
Oral mucositis is a condition involving painful sores in the mouth, which can range from inflammation of the mouth tissue to severe ulcers. The inflammation will appear as a red, painful surface. Ulcers may occur on the tongue, the floor of the mouth, the insides of the cheeks, the roof of mouth or the gums. These lesions can extend from the oral cavity through the gastrointestinal tract, the organ system including the esophagus and stomach.
Read More
Mouth Sores and Infections
Parotid Gland Swelling: Symptoms, Treatment, and Prevention
If you notice discomfort or swelling on the side of your face, it can be many things. It may be a parotid gland infection. Read on to learn the signs and symptoms to get the care you need and learn about preventing parotid gland swelling in the future.
Read More
Mouth Sores and Infections
Popping A Cold Sore: A Good Or A Bad Idea?
A cold sore is a nuisance, and it can be a great temptation to pop the blisters. However, popping a cold sore doesn't speed up the healing process and can lead to scarring. To prevent a cold sore from lingering, keep your hands off it and stick to gentle, safe treatments and medications.
Read More
Mouth Sores and Infections
Purple Spot On Lip: What Causes It?
Discovering a purple spot on your lip that was never there before can be scary, and you may be curious to know what it is and where it came from. While there are a number of reasons you might see a purple spot on lip tissue, it may be a case of purpura. Here's what you should know about this condition.
Read More
Mouth Sores and Infections
Rash Around the Mouth? Perioral Dermatitis and What It Means for You
You try to take care of your skin, but despite applying sunscreen and regularly cleansing and moisturising your face, you may still notice a rash around your mouth. As far as skin conditions go, MedlinePlus notes that rashes around the mouth are most likely to affect young women and children, but can ultimately affect anyone. This condition is called perioral dermatitis, and its causes might surprise you. By understanding what it is and how to treat it, you can soothe your rash to reveal healthy, glowing skin once again.
Read More
Mouth Sores and Infections
Reversible And Irreversible Pulpitis: Causes And Treatment
If you notice a tingling sensation in one of your teeth or sharp pain when eating something hot or cold that goes beyond regular tooth sensitivity, you may be dealing with pulpitis.
Read More
Mouth Sores and Infections
Salivary Gland Infection Symptoms and Treatment
Your salivary glands do a lot more than just make your mouth water at the sight of your favorite snack. These hard-working glands found in the lower arch and sides of your mouth produce saliva to keep your mouth clean and aid in the breakdown and digestion of food. But sometimes, infection can cause your salivary glands to malfunction and even cause you pain. What could feel like the usual sore throat and fever might actually be a salivary gland infection. Know the signs and symptoms so you can get the necessary care you need, and then care for your glands so it doesn't happen again. Here's how.
Read More
Mouth Sores and Infections
Scarlet Fever on the Tongue: Symptoms, Risks, and Complications
As a parent, you work hard to ensure your child stays healthy and happy. But the fact is, millions of children will develop strep throat annually, notes the Centers for Disease Control and Prevention (CDC). A certain strain of strep throat, known as a group A streptococcal infection, may develop into scarlet fever, according to the CDC. While it's most known for its telltale skin rash, scarlet fever tongue symptoms may occur.Find out more about what to look out for in your child's mouth and how to get your little one feeling their best again.
Read More
Mouth Sores and Infections
6 Uncommon Oral Health Problems
Tooth decay and periodontal (gum) disease are two of the most common oral diseases you and your family may experience at some point in your lives. Injuries to the face and head can also compromise the health of your teeth. However, here are a few less common oral health problems that may be worth seeking help with from your dentist or doctor.
Read More
Mouth Sores and Infections
Soothing Mouth Ulcer Treatment Tips
Have you ever developed a white painful sore with red borders inside of your mouth? These are called aphthous ulcers, better known as canker sores. These lesions are somewhat of a mystery as to why some people get them, but usually the cause could be related to stress, a slight injury to the soft tissues in the mouth, dentures that don't fit properly, braces can contribute to this, as well as eating highly acidic foods such as oranges, strawberries and tomatoes and nutritional deficiencies.
Read More
Mouth Sores and Infections
Stomatitis Treatment For 3 Types Of Mouth Sores
Stomatitis is a common problem many people deal with at some point, and there are different types. Here's what you need to know about stomatitis.
Read More
Mouth Sores and Infections
Strawberry Tongue And Related Conditions: Causes & Treatments
Parenting is full of all sorts of challenges, including figuring out what's wrong with your children when they're sick. That difficulty is compounded when very young children aren't able to communicate what's wrong or don't understand what being sick means. So you have to look for symptoms. But some oral symptoms might not be so obvious, such as bumps on a tongue.
Read More
Mouth Sores and Infections
The Sublingual Papilla and Your Salivary Structures
If you've ever been confused about words like “sublingual papilla” or “Wharton's duct,” you are not alone. Here's what you need to know about your sublingual papilla, salivary structures, and salivary stones.
Read More
Mouth Sores and Infections
Toddler Mouth Sores: Causes And Treatments
Diagnosing your toddler's mouth sores is ultimately your dentist's or your child's pediatrician's job, but it helps to have some knowledge about mouth sores and the types of treatments available for your child.Here's how to determine whether that mouth sore your poor tot is nursing is a common malady or a cause for concern, as well as some tips for soothing your irritable child's discomfort.
Read More
Mouth Sores and Infections
Toothpaste on Cold Sore: Does It Work?
Tingling or itching around the lips is a distressing signal that a cold sore is on its way for sufferers of this chronic, recurring condition. The cluster of tiny blisters that soon appears is painful and can be embarrassing. Is it possible to stop a cold sore in its tracks? Toothpaste is one home remedy that's sometimes recommended as a cold sore preventative, but the jury is still out on its effectiveness.
Read More
Mouth Sores and Infections
Ulcerative Colitis Mouth Sores
Are you one of the three million adults diagnosed with inflammatory bowel disease (IBD) in the United States?
Read More
Mouth Sores and Infections
What A Gum Boil Could Mean For Your Dental Health
If you notice anything strange in your mouth, such as a gum boil or a bump that looks like a pimple, it's a good idea to have it checked out by a dentist.
Read More
Mouth Sores and Infections
What a Sore Throat and Tongue Can Mean
Having a sore throat is uncomfortable and inconvenient, and even more so when accompanied by a sore tongue. The combination of a sore throat and tongue isn't a rare symptom of certain conditions, but your diagnosis depends on the other signs and symptoms you experience.
Read More
Mouth Sores and Infections
What Are Canker And Mouth Sores?
Probably one of the most overlooked parts of your digestive system are the salivary glands, but they play such an important role to your oral health.
Read More
Mouth Sores and Infections
What Are Lie Bumps?
TLP affects the fungiform papillae of your tongue, which are the small round projections that cover the top of the tongue.
Read More
Mouth Sores and Infections
What Are Tonsil Stones?
Tonsil stones, clinically called tonsilloliths, are small, white discharges that form in the crevices of the tonsils. They are typically found on the surfaces of the pharyngeal tonsils on either side at the back of the throat. They can be as small as a grain of rice or as large as a pea. They are quite common and usually harmless, but they may spark alarm in patients when noticed for the first time.
Read More
Mouth Sores and Infections
What Causes a Black Spot on Your Gums?
We’re here to help walk you through the causes of dark spots in your mouth and what they mean.
Read More
Mouth Sores and Infections
What Causes a Scab on the Lip?
Discovering a scab on your lip can be distressing. Scabs in this area can make daily activities like eating and drinking difficult, and since they're so visible, they may reduce your self-confidence. There are many possible causes for a scab on the lip, but rest assured, there are ways you can help it heal.
Read More
Mouth Sores and Infections
What Causes Red Spots On The Roof Of Your Mouth?
Red spots on the roof of your mouth can be caused by a variety of different reasons. Some are just a minor inconvenience, while others could be a sign of a more serious health issue that may require further investigation. Here are some common possibilities:
Read More
Mouth Sores and Infections
What Does a Black Tongue Say About Your Health?
When these papillae grow longer instead of shedding and start to trap food remnants and bacteria, it may lead to a black tongue, according to the Mayo Clinic.
Read More
Mouth Sores and Infections
What Is A Dentigerous Cyst?
If you have a permanent tooth that's coming in and a clear sack of fluid has formed around it, you may have what's called a dentigerous cyst. We'll give you all the info you need to know about these growths so you can feel confident about your health, treat your cyst, and get your gums back to a condition you can smile about.
Read More
Mouth Sores and Infections
What Is A Mouth Cyst?
A mouth cyst is a thin, fluid-filled sac on the inside of your mouth. Also called a mucous cyst or mucocele, the sac is harmless and painless, says the National Institutes of Health (NIH). It may annoy you though, because you feel a bump inside your mouth.These cysts commonly occur on the inside of the lips but can also form on your tongue, palate, inside of the cheeks, floor of the mouth or around piercings on the tongue or lips. A cyst on the floor of your mouth is called a ranula, and a cyst on the gum is called an epulis. The mucocele sac is bluish and clear and contains clear fluid. Your dentist can usually diagnose a mucous cyst just by looking at it.
Read More
Mouth Sores and Infections
Herpangina 101: Signs, Symptoms, and Treatment
You’re likely familiar with contagious illnesses that children transmit like the flu or a cold—but there’s another common viral infection to be aware of: herpangina.
Read More
Mouth Sores and Infections
What Is Linea Alba on the Cheek?
Linea alba on the cheek is an oral condition that doesn't cause any discomfort or pain. It is usually diagnosed during routine dental exams.
Read More
Mouth Sores and Infections
Oral Warts: What to Do About Warts on Your Tongue
Warts on the tongue can be an uncomfortable condition. Here's what you need to know about how these warts are caused, how they can be treated, and more.
Read More
Mouth Sores and Infections
White Gums: Causes And Symptoms
People know tooth pain or bleeding gums are reasons to seek dental care. But what if your gums are white? Read on to learn what it means and what you should do if you have white gums.
Read More
Mouth Sores and Infections
White Spot on the Tongue: Is It Serious?
You might notice white spot on the tongue after experiencing discomfort or when checking inside your mouth. Most are harmless. Here's what it could be...
Read More
Mouth Sores and Infections
Why Do Tongue Lesions Occur and How Are They Treated?
Tongue lesions can be the result of several different etiologies. Find out what they are and what you and your dentist can do about them, here.
Read More
Mouth Sores and Infections
Winter Tips For A Healthy Mouth: Dealing With Common Winter Mouth Woes
Skin isn't the only part of your body that suffers from a dryer climate. Embrace these winter tips for a healthy mouth by Colgate.
Read More
Mouth Sores and Infections
Yeast Infection In Your Throat: Everything You Need To Know
Understanding the causes and symptoms of yeast infection in throat can help you get the right diagnosis and treatment. Learn more, here.
Read More
Mouth Sores and Infections
What's A Ranula? A "Frog" In Your Mouth
According to Latin translation, a ranula is a little frog. In dentistry, it's a large swelling in the floor of the mouth. Learn how it can be treated.
Read More
Mouth Sores and Infections
When Is A Cold Sore No Longer Contagious?
It starts as a tingling, burning or itching sensation, soon followed by blisters that begin to ooze: another cold sore has arrived. Unfortunately, the virus that causes cold sores is highly infectious. But when is a cold sore no longer contagious? Once the sore has scabbed over, your chances of passing on the virus decrease significantly.
Read More
Mouth Sores and Infections
Mouth Sores and Other Causes for Roof of Your Mouth Discomfort
Mouth ulcers are not uncommon, but developing a sore on the roof of your mouth can still have you concerned. The sore on the roof of your mouth may be from one of these four conditions.
Read More
Mouth Sores and Infections
3 Types of Tongue Blisters
Your tongue is also remarkably uncomfortable when indisposed, and sores or tongue blisters can inconvenience you more than you might expect. Learn about 3 types of tongue blisters here.
Read More
Mouth Sores and Infections
How to Spot Lip Fungus and What to Do About It
Lip fungus is due to a yeast called Candida that occurs naturally in your body. Learn what causes the overgrowth infection and what you can do about it.
Read More
Mouth Sores and Infections
Angular Cheilitis: Symptoms, Causes and Treatments
Angular cheilitis may look like a simple mouth sore, but these painful patches at the corners of your lips may point to a serious condition. Learn more.
Read More
Mouth Sores and Infections
What to do about Mouth Shingles
Herpes Zoster is a member of the Herpes family of viruses. In some instances, this can cause shingles in mouth that require specialized treatment.
Read More
Mouth Sores and Infections
Foods To Think About If You Have Cold Sores
A cold sore outbreak can be uncomfortable, but knowing what foods to avoid with cold sores can help you feel better until they go away.
Read More
Mouth Sores and Infections
Apical Abscess: Symptoms, Diagnosis And Treatment
An apical abscess is one of the most common types of dental abscesses. Find out more about the symptoms, diagnosis, and treatment of apical abscess, here.
Read More
Mouth Sores and Infections
Can You Get a Cold Sore From Sun Exposure?
Cold sores are common, and they can be triggered by certain factors. Here's what to know about getting cold sores from sun exposure.
Read More
Mouth Sores and Infections
Can You Use Hydrogen Peroxide On A Canker Sore?
Learn how canker sores form and whether you can use hydrogen peroxide on a canker sore. Read on for additional ways to heal a canker sore.
Read More
Mouth Sores and Infections
Canker Sore Vs. Cold Sore: Spot These 3 Differences
It can be hard to differentiate between a canker sore vs. cold sore. Here are the differences between the two and learn how to treat and prevent them.
Read More
Mouth Sores and Infections
Eruption Cyst: Causes, Symptoms, and Treatments
Hearing that your child has an eruption cyst can be alarming. But dental professionals can help to treat this oral issue. Here's what to know.
Read More
Mouth Sores and Infections
Globus Sensation Causes, Symptoms, and Treatments
Have you ever felt like you had a lump in your throat? This is called globus sensation, and it may have a variety of causes, symptoms, and treatments.
Read More
Mouth Sores and Infections
Identifying Koplik Spots and Other Symptoms of Measles
Koplik spots are one of the signs of measles. Look for any lumps or bumps, along with any variations of color. Here's what to know.
Read More
Mouth Sores and Infections
Leukoplakia: Symptoms, Causes and Treatments
Leukoplakia is a condition where white patches or lesions appear in the mouth. Learn more about signs and symptoms, when to see a doctor for treatment, and more.
Read More
Mouth Sores and Infections
Leukoplakia Treatment Considerations and Causes
Leukoplakia defines all white patches found in the inner lining of the mouth. They can be benign or a sign of something more dangerous. Learn more, here.
Read More
Mouth Sores and Infections
Lysine For Cold Sores: Does It Work?
Cold sores are a drag, especially when they keep coming back. Here's what you need to know about lysine for cold sores.
Read More
Mouth Sores and Infections
Oral Mucocele: Causes, Prevention & Treatment
What are mucoceles, why do they occur and how many people experience one in their lifetime? Find out more about mucoceles, here.
Read More
Mouth Sores and Infections
Oral Lichen Planus: Symptoms, Causes, & Treatment
Oral lichen planus is a non-infectious, inflammatory condition that affects the membranes inside the mouth. What are the symptoms? Learn more.
Read More
Mouth Sores and Infections
Pimple vs. Cold Sore: How to Spot the Difference
At the onset, they can look similar, but these key differences between a pimple vs. cold sore will help you determine the right treatment from the start.
Read More
Mouth Sores and Infections
Purple Tongue: Possible Causes And Treatment Options
If you looked in the mirror and notice that your tongue is looking purplish, don't fret just yet. Here are some of the possible causes of a purple tongue.
Read More
Mouth Sores and Infections
Scalloped Tongue: Causes and Treatment Options
If you notice indentations on the sides of your tongue, you may be wondering if it is something to worry about. Here are the causes and treatment options.
Read More
Mouth Sores and Infections
Swollen Uvula: Causes, Symptoms And Treatments
If you have a swollen uvula, you may be experiencing allergies or an infection. Learn more about the causes, symptoms and treatment options.
Read More
Mouth Sores and Infections
The Signs of an Infected Tongue Piercing
Find out more about infections of the mouth, including canker sores or mouth ulcers, cold sores, oral thrush, and more. Learn about signs, symptoms, and treatment options.
Read More
Mouth Sores and Infections
Tooth Abscess
A tooth abscess is a bacterial infection found in the inner part of the tooth. Learn more about common causes, symptoms and how to prevent a tooth abscess.
Read More
Mouth Sores and Infections
What You Need To Know About Impetigo
If your child comes home from school with red sores around their nose and mouth, they may have an infection called impetigo. Here's what to know.
Read More
Mouth Sores and Infections
What Is Orbital Cellulitis And What Does It Have To Do With Dental Health?
Orbital cellulitis is an infection that can sometimes be caused by dental issues. Learn more about this condition and how it's treated.
Read More
Mouth Sores and Infections
What You Should Know About Benzocaine
Benzocaine is an over-the-counter local anesthetic that temporarily numbs sores, but it can have negative health effects. Learn more about its safety.
Read More
Mouth Sores and Infections
Why Your Dentist Might Recommend Amoxicillin For Abscessed Tooth
Amoxicillin is a widely prescribed antibiotic used to treat dental infections. Here's why your dentist may recommend amoxicillin for abscessed tooth.
Read More
Mouth Sores and Infections
Oral Fungus Causes Common Mouth Infection
Also called candidiasis, the fungal infection causes painful white spots on the tongue or inner cheeks. Learn more about this infection and how to both treat & prevent it.
Read More
Mouth Sores and Infections
What Are Canker And Mouth Sores?
Mouth sores, also including canker sours, are common conditions that can affect your daily life due to the pain. These sores can appear inside of the mouth, lips, tongue, and cheeks. Learn more about what causes mouth sores and how they can be treated.
Read More
Mouth Sores and Infections
What Are Cold Sores and Fever Blisters?
What is a cold sore? Fever blisters, also known as cold sores, present as tiny, fluid-filled blisters on lips, under the nose, or around the chin. Learn about what causes them here.
Read More
Mouth Sores and Infections
Mouth Sores and Other Causes for Roof of Your Mouth Discomfort
Mouth ulcers are not uncommon, but developing a sore on the roof of your mouth can still have you concerned. The sore on the roof of your mouth may be from one of these four conditions.
Read More

Mouth Sores and Infections
5 Ways To Get Rid of Canker Sores Naturally
When you're looking for how to get rid of canker sores naturally, you'll see there are a variety of treatments available. Learn more here.
Read More
Mouth Sores and Infections
How to Get Rid of a Cold Sore Fast
These sores are common and will go away on their own, but if you have a major event coming up, you might be wondering how to get rid of a cold sore fast.
Read More
Mouth Sores and Infections
What Is Herpetic Gingivostomatitis?
Gingivostomatitis, or primary herpetic gingivostomatitis, is a highly contagious infection of the mouth. Here's what to know about this oral issue.
Read More
Dental Health Threats
Q&A ON COLGATE-PALMOLIVE LABORATORY AND CLINICAL RESULTS ON EFFECTS OF TOOTHPASTE AND MOUTHWASH ON COVID-19 VIRUS
Can toothpaste and mouthwash neutralize and reduce the virus that can cause COVID-19 in your mouth? Read more on this new Colgate-Palmolive research for toothpaste and mouthwash effects on the COVID-19 virus.
Read More
Dental Health Threats
Is Open Mouth Breathing Bad for Your Teeth?
If your mouth often feels dry when you wake up, you may be sleeping with your mouth open. Here's how this can affect your teeth and what you can do.
Read More
Dental Health Threats
10 Possible Causes Of A Numb Mouth
If your mouth has become numb for no apparent reason, it can be concerning, but treatments are available. Here are some possible causes for a numb mouth.
Read More
Dental Health Threats
A Gum Piercing: What You Need To Know
Gum piercings are 2018's hot body trend. Learn more about gum piercings, and how to care and preserve your piercing while maintaining your oral health.
Read More
Dental Health Threats
A Lip Tattoo: Should You Get Ink On Your Lips?
A lip tattoo is different than other forms of tattooing. Why wait? Learn more about getting inked on the inside of your mouth and what you need to know.
Read More
Dental Health Threats
Abfraction Lesion: Causes And Treatment
An abfraction isn't a cavity, but it may cause tooth sensitivity and decay. Learn what to watch for and how a dentist may treat one here.
Read More
Dental Health Threats
Abscessed Tooth Dangers
Teeth can develop an abscess when bacteria enter the pulp canal. Knowing abscessed tooth dangers can help you keep your mouth happy and healthy.
Read More
Dental Health Threats
Anemia Gums And Your Oral Health
Anemia can lead to a variety of symptoms, and problems affecting your oral health. Learn more about the symptoms, treatment, and prevention of anemia gums.
Read More
Dental Health Threats
Anemia Tongue: Symptoms, Causes, And Treatments
If you have anemia, tongue function and appearance can feel the effects almost as much as your energy level. Here's how to identify it & treatment options.
Read More
Dental Health Threats
Are Teeth Grills Safe For Your Mouth?
Teeth grills are a popular cosmetic dental treatment that musicians, celebrities and many others use to make fashion statements. Learn more, here.
Read More
Dental Health Threats
Biofilms and Oral Health
The role of biofilms in the oral health of patients has been known for several years, but only recently has the public been made aware. Learn more here.
Read More
Dental Health Threats
Black Hairy Tongue Causes And Treatment
Black hairy tongue is caused by bacteria overgrowth on the tongue. Luckily, this condition is harmless and can be easily treated by your dentist or doctor.
Read More
Dental Health Threats
Can Bad Teeth Make You Sick?
Can bad teeth make you sick? Yes, eventually. Poor oral health can cause dental issues like abscesses, and they can impact your health. Here's how.
Read More
Dental Health Threats
Can You Remove Tartar At Home?
Tartar can have negative effects on your oral health, so it shouldn't be allowed to build up. No matter what you may hear or read, it's not a good idea to remove tartar at home.
Read More
Dental Health Threats
Causes Of A Black Spot Inside The Cheek
A black spot inside the cheek could result from an amalgam tattoo, smoking or, very rarely, oral cancer. Learn when to seek advice from your dentist.
Read More
Dental Health Threats
Dental Ankylosis: A Rare Concern For Baby Teeth
What is dental ankylosis? Learn how to watch out for this rare issue that can happen during the transition from baby teeth to adult teeth.
Read More
Dental Health Threats
Dental Grill: The New Trend Affecting Dentistry And The Health Of Your Teeth
Grills, also called fronts, are removable and fit over the front teeth. Dental grills are made of gold, silver or jewel encrusted metals that run as little as $20 and well into the thousands for more elaborate designs.
Read More
Dental Health Threats
Do You Know Your Saliva PH? Here's Why It's Important
Dental and medical professionals use many measurements as indicators of your health. Saliva pH is one of them. Here's why it's important.
Read More
Dental Health Threats
Do You Need A Mercury Detox? The Facts About Amalgam And Mercury Exposure
If you have silver fillings, also known as amalgam fillings, they may contain mercury. Does this mean you need a mercury detox? Here are the facts.
Read More
Dental Health Threats
The Effects Of Smoking On Teeth
Although they aren't addressed very often, the effects of smoking on teeth and the oral cavity are important in the process of quitting.
Read More
Dental Health Threats
Are Tongue Piercings Bad for Your Teeth?
Tongue piercing rings and similar body jewelry can affect your oral health depending on the location. Here's what to look for in these items.
Read More
Dental Health Threats
Erythroplakia: What This Red Spot May Mean
Erythroplakia is a precancerous red spot in the mouth. Find out how to seek treatment from your dentist. Learn more, here.
Read More
Dental Health Threats
Five Classifications of Hypophosphatasia
What is hypophosphatasia? Read on to learn more about this condition and the effects it has on bones, teeth and your health.
Read More
Dental Health Threats
Hookah vs. Cigarettes: Is Smoking Hookah Safer for Your Mouth?
When it comes to hookah vs. cigarettes, people often think of smoking hookah as a safer option. But is it? Learn more about how it can affect your health.
Read More
Dental Health Threats
How A Fractured Jaw Is Identified And Treated
A fractured jaw can change the functions of your breathing, eating, and speaking. Learn more on how to identified and treat fractured jaw by reading more, here.
Read More
Dental Health Threats
How Acidic Drinks Affect Your Teeth
Acidic drinks are very damaging to tooth enamel, no matter how long you've held the habit, so be sure to consume the following in moderation... Learn more.
Read More
Dental Health Threats
How Mouth Spray Helps Dry Mouth
A mouth spray may be good option if you need short-term relief of dry mouth. Learn how sprays work and what you can do for longer-term solutions, here.
Read More
Dental Health Threats
What To Do With A Blocked Salivary Duct
What is a blocked salivary duct? How do you deal with it? Click here to learn all you need to know to care for a blocked salivary duct with Colgate.
Read More
Dental Health Threats
How To Fix Smokers Teeth Before Wedding Season
Whether it's your own wedding of you're just a guest, one thing is for sure: You want to look great in the photos. The problem is your smokers teeth.
Read More
Dental Health Threats
How To Keep Your Lips Safe In The Sun
Being out in the sun usually means applying sunscreen. This is no different when it comes to your lips. Read more on the importance of lip sunscreen here.
Read More
Dental Health Threats
How to Manage Brittle Teeth
Brittle teeth result in chips, fractures and discolored enamel. What causes brittle teeth and how can your dentist strengthen your smile?
Read More
Dental Health Threats
How to Manage Orofacial Pain
Orofacial pain or discomfort can be due to dental conditions, TMD, trauma to the orofacial area, inflammation or disease. Learn more, here.
Read More
Dental Health Threats
How to Quit Smoking and Protect Your Oral Health
Quitting smoking can really help save your teeth, and overall oral health. Click on this article from Colgate to find out smoking affects your oral health.
Read More
Dental Health Threats
Hydrated Silica in Toothpaste
Hydrated silica is an abrasive ingredient used in toothpaste to provide a dental office-like clean feeling, but for some people it can be too harsh.
Read More
Dental Health Threats
Is One Sensitive Tooth A Serious Issue?
Knowing how to clean braces properly is essential. Click here for more information that will help you plan to keep your mouth healthy!
Read More
Dental Health Threats
Macroglossia: Causes, Symptoms, Diagnosis, And Treatment
Macroglossia refers to an enlarged tongue stemming from various conditions. It can cause problems with eating and breathing. Learn more, here.
Read More
Dental Health Threats
Mandibular Advancement Devices (MAD) And Sleep Apnea
Up to 25 million American adults have sleep apnea. Could a mandibular advancement device help their condition? Learn more.
Read More
Dental Health Threats
On World No Tobacco Day, Think About These Five Effects On Oral Health
Read More
Dental Health Threats
Oral Pathology And 4 Common Oral Diseases
Oral pathology is the dental specialty that studies the causes and effects of conditions affecting the mouth and other oral structures. Learn more here.
Read More
Dental Health Threats
Oral Piercing Aftercare: Maintenance Is Required!
Oral piercings are popular but require a good amount of maintenance. If you have one, make sure to follow this dentist recommended piercing aftercare.
Read More
Dental Health Threats
Oral Piercing Risks & Proper Oral Hygiene
What exactly is the relationship between oral piercings & oral health? Click here to discover helpful tips to keep your piercing and oral health safe.
Read More
Dental Health Threats
Anemia Tongue: Symptoms, Causes, And Treatments
Pernicious anemia, a condition arising from a vitamin B12 deficiency, can affect the oral cavity and other parts of the body. Here's what you should know.
Read More
Dental Health Threats
Reusable Straws: Protect Your Teeth And The Environment
Caring for your teeth is a vital key to overall good health. Here is what you need to know about different straws and their effects on teeth.
Read More
Dental Health Threats
Treating and Reversing Smoker's Mouth
Smoking causes a lot of damage inside your oral cavity. Here are four ways to control the odorous smokers mouth while or after quitting.
Read More
Dental Health Threats
Smoking Side Effects And How Quitting Stops Them
Numerous smoking side effects can influence your mouth's health. Consider the following in the process of extinguishing the habit for good.
Read More
Dental Health Threats
Strep Throat and Tonsils: What's the Connection?
The connection between strep throat and tonsils is a close one. But does having your tonsils removed curb the infection? Here's what to know.
Read More
Dental Health Threats
Sugar Habit? How to Curb It and Prevent Tooth Decay Symptoms
Sugar exacerbates tooth decay symptoms, and it's common knowledge that large amounts are bad for your dental health. Here's how to start avoiding it.
Read More
Dental Health Threats
Teeth Without Enamel: Causes, Treatment And Care
Although enamel is the hardest substance in your body, not everyone's is the strongest. Still others have teeth without enamel at all. Learn more, here.
Read More
Dental Health Threats
The Effects Of Chlorine On Your Teeth
Although it's a necessary disinfectant, the effects of chlorine on your teeth can be a cause for concern. Consider the following to protect teeth enamel.
Read More
Dental Health Threats
The Many Causes of Loose Teeth
As children, wiggly, loose teeth meant that we would soon be richer, thanks to the tooth fairy. As adults, we want to keep our teeth for a lifetime.
Read More
Dental Health Threats
The Telltale Signs You're Suffering From Dental Erosion
Dental erosion may be invisible to the naked eye. Learn more about dental erosion and some tell-tale signs if you may have it.
Read More
Dental Health Threats
The Two Types Of Dentin Dysplasia
A rare condition, dentin dysplasia causes abnormal tooth development that can result in tooth loss. Learn more about the causes, effects and treatments.
Read More
Dental Health Threats
Threats to Dental Health 101
Learn more about how other diseases and conditions can pose a threat to your overall dental health. Learn more about your oral health, at Colgate.com
Read More.png)
Dental Health Threats
Three Cosmetic Effects Of Dental Erosion
Dental erosion can affect the look of your smile, but luckily it is treatable and preventable. Find out more about the effects of dental erosion here.
Read More
Dental Health Threats
Three Types Of Bacteria In The Mouth And What They Do
There are about 300 types of bacteria in the mouth. Here's background on where they're found, which ones cause decay and which result in gum disease.
Read More
Dental Health Threats
Tongue Piercings: Wear With Care
Teenagers love setting themselves apart from their peers. In recent years, that means a tongue piercing. But without proper care, it poses several risks.
Read More
Dental Health Threats
Tongue Piercings: What To Expect
Tongue piercings are an ancient form of body modification and self-expression that still interest people today. Here's what you should know.
Read More
Dental Health Threats
Tooth Enamel Loss Prevention Tips
Although it's the hardest substance in your body, enamel is actually pretty fragile. Here's what you can do to prevent tooth enamel loss in your everyday.
Read More
Dental Health Threats
Tooth Enamel Repair Approaches
When your teeth's surfaces wear away, your teeth can become discolored or sensitive. But with the help of your dentist, tooth enamel repair is possible.
Read More
Dental Health Threats
Torus Mandibularis: What You Need To Know
Torus mandibularis is a bony growth that develops on the lower jaw, underneath the tongue. Find out more about causes, symptoms, treatments, and more.
Read More
Dental Health Threats
Translucent Teeth: Three Things To Know
Teeth should be opaque, but some may notice the edges of their enamel are a bit thinner. Here are three things to know about translucent teeth.
Read More
Dental Health Threats
Treating Meth Mouth
Being aware of the dangers of meth use and the treatment options available for those who may be addicted can help individuals make informed choices that lead to a healthier mouth and body.
Read More
Dental Health Threats
What Are The Signs Of Meth Teeth?
Dental problems associated with meth use are known as 'meth teeth.' If you're concerned a loved one may be using, their teeth can provide clues. Learn more.
Read More
Dental Health Threats
What Causes Cheek Swelling?
Noticing that your cheeks are swollen can be distressing. There are many possible causes of cheek swelling, and a doctor or dentist can diagnose the issue.
Read More
Dental Health Threats
What Causes Submandibular Gland Swelling?
Submandibular gland swelling often occurs due to small, calcified stones blocking the salivary glands. Learn how to treat and prevent this condition.
Read More
Dental Health Threats
What Causes Tongue Bumps?
Most tongue bumps are harmless and disappear without any treatment. See a medical professional if you have a bump on your tongue that doesn't go away.
Read More
Dental Health Threats
What Is A Vertical Root Fracture?
If you're experiencing pain in a tooth that previously had a root canal, it's possible that you have a vertical root fracture. Here's what to know.
Read More
Dental Health Threats
What Is An Odontoma And How Is It Treated?
An odontoma is one of the more common types of benign oral tumors. Here's what you need to know.
Read More
Dental Health Threats
Ossifying Fibroma: Causes, Symptoms, and Treatment
An ossifying fibroma (sometimes called a cemento-ossifying fibroma) is one of the rare, benign tumors that can occur in the jaws. Learn more.
Read More
Dental Health Threats
What Is Dental Tourism?
There's another kind of tourism that people are talking about: dental tourism. Learn more about popular destinations, dangers and safe ways to save money.
Read More
Dental Health Threats
What Is Ludwig's Angina?
Untreated dental decay can unfortunately lead to severe complications. One life-threatening condition is called Ludwig's angina. Learn more.
Read More
Dental Health Threats
Apical Periodontitis: Causes, Symptoms, and Treatments
Periapical periodontitis means inflammation near the tip of your tooth's root. Learn about the different types, common causes and treatment options.
Read More
Dental Health Threats
What Is Tartar Buildup On Teeth?
When plaque mineralizes, it becomes tartar buildup on teeth. Clean regularly to prevent it.
Read More
Dental Health Threats
What Is The Worst Drink For Your Teeth? Avoid These Five
Certain liquids do a number of your mouth health. What is the worst drink for your teeth, though? Nothing tops the list. Here are five to avoid and why.
Read More
Dental Health Threats
What To Do With An Infected Oral Piercing
An infected piercing sounds gross, but it happens, especially with piercings in and near the oral cavity. Here's how to avoid and treat them.
Read More

Dental Health Threats
When Is Lip Biting A Sign Of Other Conditions?
Lip biting is just an occasional nervous habit for some people, but sometimes, it can be a sign of an underlying dental or medical condition.
Read More
Dental Health Threats
When Sick Teeth Hurt: Three Illnesses That Cause Tooth Pain
If you feel sick, teeth hurt and you can't figure out what's wrong, you may be experiencing an ear infection, sinus troubles or a side effect of angina.
Read More

Dental Health Threats
Do You Have Acid Erosion on Your Teeth?
Do you have acid erosion on your teeth? What causes acid erosion on your teeth? Click here for more information on all things acid erosion with Colgate.
Read More
Dental Health Threats
Your Baby Has A White Tongue: Is It Thrush?
If your baby has a white tongue, don't panic. Learn the common causes of a white tongue and how to prevent a possible case of thrush.
Read More
Dental Health Threats
Eagle Syndrome: Signs And Treatment Options
If you have painful chewing and swallowing, it may be related to Eagle syndrome. Here's what you should know about the condition.
Read More
Dental Health Threats
Rotten Teeth: Causes, Symptoms, and Treatment for Tooth Decay
How can you tell if you have rotten teeth? Can a dentist save them and make your mouth healthy again? Learn the signs and treatments for rotten teeth.
Read More
Dental Health Threats
What Is Mask Mouth?
Wearing a face mask can help prevent you from the spread of viruses. However, wearing a mask for an extended period of time can cause some side effects like mask mouth. Read on to learn more about the causes and symptoms of mask mouth and how to prevent it and make wearing a mask more comfortable.
Read More
Dental Health Threats
How Do I Care For My Teeth During The Coronavirus Pandemic?
Due to the COVID-19 outbreak, questions surrounding dental health have arose. Find your at-home treatments, & when you should see a dentist here.
Read More
Dental Health Threats
Tongue Piercing Aftercare: Healing and Risks
The practice doesn't appear to be any more risky than getting an ear pierced. However, if you're going for a hole in your tongue, you might want to be aware of what can go wrong.
Read More
Dental Health Threats
11 Habits That Damage Teeth
You know that brushing and flossing are good oral care habits, but what about habits that can damage teeth? Here are 11 harmful habits to watch out for.
Read More
Dental Health Threats
Managing Epilepsy And Oral Health
Epilepsy is a neurological condition in which a person experiences unpredictable seizures. Here are the important facts regarding epilepsy and oral health.
Read More
Dental Health Threats
Teeth And Medication: How Are They Connected?
Certain drugs that treat health issues may cause oral side effects. Here's how teeth and medication are connected and some of the symptoms to look for.
Read More
Dental Health Threats
Celebrate The Great American Smokeout Nov. 15th
Celebrate The Great American Smokeout on November 15th! This is an annual event sponsored by the American Cancer Society. Find out more details, here.
Read More
Dental Health Threats
The Connection Between Oral Health And Strokes
You might not think that oral health and strokes are related, but they are connected in important ways. Here's what you need to know and how to prevent it.
Read More
Dental Health Threats
What Causes Pale Gums? 3 Possibilities to Discuss With Your Dentist
If your gums appear paler than usual, it may indicate that you have a health problem. Here are three possibilities to discuss with a doctor or dentist.
Read More
Dental Health Threats
What Is A Dental Black Triangle? Causes And Treatments
A dental black triangle is empty space between your teeth where gum tissue should be. Learn more about the oral health risks, causes and treatments.
Read More
Dental Health Threats
What Is Phossy Jaw?
In the 19th century, some workers in match factories developed a condition called phossy jaw after being exposed to a chemical used in the match manufacturing process. This condition, clinically known as osteonecrosis of the jaw, vanished until it recently reappeared in the 21st century.
Read More
Dental Health Threats
What Is Proper Tongue Posture And Why Does It Matter?
Proper tongue posture becomes important because it links to your overall health. Find out warning signs of your poor tongue posture and how to treat it.
Read More
Dental Health Threats
Is Ayurvedic Treatment for Dental Bone Loss Effective?
Alternative forms of medical and dental treatment, such as Ayurveda, may sound appealing, but does Ayurvedic treatment for dental bone loss really work?
Read More
Dental Health Threats
How Better Oral Care Routines Can Save Our Oceans
Plastics are affecting our ecosystem and polluting our oceans. Learn more about how you can do your part to reduce oral care products waste.
Read More
Dental Health Threats
De-Stress: Its good for your teeth
Stress can cause negative effects on our teeth. From TMJ disorder, canker sores, and gum disease. Learn more from Colgate on how to de-stress.
Read More
Dental Health Threats
The Benefits of Vitamin D for Your Teeth and Overall Oral Health
How does vitamin D help your teeth? Learn more of the benefits of Vitamin D for Your Mouth from Colgate.
Read More
Dental Health Threats
What is Oral Thrush & What Causes It?
What is oral thrush? What are the signs & symptoms? Click here to read more about oral thrush and what causes it with Colgate.
Read More
Dental Health Threats
Does Seltzer Damage Your Teeth?
Does seltzer damage your teeth? Click here to find out about the effects of seltzer and carbonated water on teeth with Colgate®.
Read More
Pain Management (Anesthesia)
4 Conscious Sedation Drugs Used In Dentistry
For patients with dental phobia or those going through an extensive dental procedure, conscious sedation drugs can help. Here are four commonly used drugs.
Read More
Pain Management (Anesthesia)
A Guide To Sedation Dentistry
Find out more about sedation dentistry, including if you're a candidate for sedation, the types of dental sedation, and the ADA's role in guidelines and training.
Read More
Pain Management (Anesthesia)
The 411 On Dental Anesthesia
When in surgery, some people suffer from dental anesthesia side effects. Learn more about anesthesia and why some patients don't respond as well to it.
Read More
Pain Management (Anesthesia)
How Long Does Novocaine Last?
How long does novocaine last? Learn what anesthesia options are available for your dental treatment and how long the numbing effects will last.
Read More
Pain Management (Anesthesia)
Inferior Alveolar Nerve Block and Dental Pain Control
Local anesthesia — often referred to as Novocaine, which is a brand name — is achieved by injecting anesthetic agents in targeted areas of the mouth with a needle.
Read More
Pain Management (Anesthesia)
Is Dental Sedation Safe For Kids?
Sedating a patient is normally a very safe procedure, and parents can help reduce the risks and stress level for their child before, during and after the treatment.
Read More
Pain Management (Anesthesia)
Is IV Sedation Dentistry Right For You?
The type of sedation that you receive at a dentist's office varies based on your level of anxiety and the type of exam or procedure you are having.
Read More
Pain Management (Anesthesia)
Lidocaine Without Epinephrine: Pros And Cons
How does a dentist determine if lidocaine without epinephrine is the right anesthetic for you? Find out more about the pros and cons of this anesthetic.
Read More
Pain Management (Anesthesia)
What's A Dental Block? 5 Things You Should Know
If you're in for a major dental procedure, your dentist may administer a dental block. Here are four things to know about dental blocks.
Read More
Pain Management (Anesthesia)
What Is Laughing Gas?
What does laughing gas do when you go to the dentist? Find out more about laughing gas, what it does, and what the side effects are, here.
Read More
Pain Management (Anesthesia)
What Is The Buccal Nerve?
The buccal nerve provides feeling to your cheeks. Learn more about this important nerve and why your dentist might need to numb it during treatment.
Read More
Pain Management (Anesthesia)
Articaine: A Local Anesthetic
Articaine is one of the medications that has replaced Novocaine for many dental procedures that require injectable anesthesia.
Read More
Pain Management (Anesthesia)
Types of Local Anesthesia
If you’re new to having local anesthesia or you just want some more information on what to expect, you’ve come to the right place. Read on for a simple guide on local anesthesia.
Read More
Pain Management (Anesthesia)
Sedation vs. Anesthesia at the Dentist: What's the Difference?
Are you weighing the options of sedation vs. anesthesia for your next dental procedure? Here's what to discuss with your dentist to make your decision.
Read More
Pain Management (Anesthesia)
Techniques for Pain-Free Dentistry
For many, the prospect of visiting a dentist can invoke fear and anxiety. Thankfully, pain-free dentistry is possible for everyone. Here's what to know.
Read More
Pain Management (Anesthesia)
What Does a Dental Anesthesiologist Do?
A dental anesthesiologist is an expert at administering and monitoring anesthesia during a dental procedure. Here's more about what they do.
Read More
Dental Visits
Five Organizations Furthering Oral Health Education
Dental health organizations provide information and resources dedicated to further your oral health education. Learn more about the five organizations here with Colgate.
Read MoreDental Visits
4 Things To Know Before You Go — And 4 More Dental Tips For While Traveling Internationally
Any dental emergency can be a traveler's nightmare. Here are tips on what to do and prepare when you are on your trip and your teeth need treatments.
Read More
Dental Visits
6 Answers to Your Questions about How Dental Insurance Works
Dental work can be costly even with insurance, which can leave you at a crossroad. Read up here on primary and secondary dental insurance to see your options.
Read More
Dental Visits
A Day In The Life Of A Dental Hygienist
Considering a career as a dental hygienist? Learn all about their day-to-day here and what to expect in this profession.
Read More
Dental Visits
How to Find a Dentist for Your Kids
A fun dentist can make a dental visit much easier for your kids. Find out what to look for in a dentist office and how to find a fun dentist, here.
Read More
Dental Visits
All About Dental Lasers
Dental lasers are quickly becoming another tool dentists can use to treat their patients. Learn more about laser uses and safety for dental treatment, here.
Read More
Dental Visits
Dental Anxiety Tips for Kids
Anxiety over a dental appointment? Find more on how to ease your child's worries to make their dentist appointments comfortable.
Read More
Dental Visits
Be Your Own Health Advocate And Speak Up to Your Dentist
Learning to be an advocate for yourself is a crucial step to building a great relationship with your dentist and making sure you are on the road to success for your oral care journey.
Read More
Dental Visits
What is CAD/CAM Dentistry?
Digital technology is improving the quality and speed of dental restorations. Could CAD CAM dentistry be part of your appointment? Learn more.
Read More
Dental Visits
Can Dentists Use Stem Cells To Grow Teeth? Exploring The Future Possibilities
Stem cells show promising potential in dentistry. Here's where the research stands regarding the possibility of using stem cells to grow teeth.
Read More
Dental Visits
Can Your Dental Hygienist Be An Oral Health Therapist?
Learn more about oral care for adults, including how to properly brush and floss, adult toothbrushes, and much more, from the Colgate Oral Care Center.
Read More
Dental Visits
Common Dental Fears and How to Overcome Them
Suffering from oral care issues, but nervous about going to the dentist. Here are some common misconceptions to ease your worries.
Read More
Dental Visits
DDS Vs DMD: What Is The Difference?
DDS means Doctor of Dental Surgery. DMD means Doctor of Medicine in Dentistry. Is there a difference between a DDS vs DMD? Read more, here.
Read More
Dental Visits
Deep Cleaning Your Teeth: When to Do It
Deep cleaning your teeth is a specific procedure performed by your dentist to treat periodontal disease.
Read More
Dental Visits
Dental Crafts That Will Prepare Your Child For A Trip To The Dentist
Trying a few dental crafts can make talking about a child's first trip to the dentist fun. Find out more about dental crafts for kids to prepare for the dentist.
Read More
Dental Visits
Dental Fear Of The Pediatric Dentist: The Parent's Role
Dental fear is a frequent problem in pediatric dentistry or for any dentist that specializes in working with children. Find out more about alleviating fears.
Read More
Dental Visits
Dental Insurance For Students: Helpful Or A Money-Waster?
Is dental insurance or students worth it or a waste of money? Find out more on dental insurance for students here and if its worth the investment.
Read More
Dental Visits
Dental Plans To Fit Your Needs
Dental plans that cover all phases of clinical dentistry are very popular with patients, and help cover the cost of their dentistry. Learn more, here.
Read More
Dental Visits
Dental Procedures: How To Prepare
Whether it's tooth extraction or a root canal, few people look forward to dental procedures. Here are four things you can do in advance to feel ready.
Read More
Dental Visits
Dental Tourism: 5 Risks Of Traveling For A Dental Procedure
Before you try to combine cheap dental care with a vacation, you should understand the risks of dental tourism, or going outside the U.S. for your care.
Read More
Dental Visits
Dental Treatment Plan: Your Oral Health Strategy
Your dentist personalizes your dental treatment plan to restore or maintain your oral health. Here's their process.
Read More
Dental Visits
Dental Visits 101
Learn how you should go about finding a dentist, including what to look for, the type of dentist to seek and more, courtesy of Colgate Oral Care.
Read More.png)
Dental Visits
Dental Visits – The Dentist Visit And What To Expect
What happens during a dental visit? Find out more about what to expect when you visit the dentist, from the cleaning to the x-rays and the examination.
Read More
Dental Visits
Dentist Requirements: What It Takes To Become A Dentist
Dentist requirements extend beyond an additional education, though. Your dentist needed to pass a number of tests and more. Find out additional information here.
Read More
Dental Visits
Dentist Specialist: Which Professional Treats What?
You may have to visit a dentist specialist if you have a specific oral condition. Which highly specialized professional is best suited to treat you?
Read More
Dental Visits
Dentistry For Kids: Focus On Fun, Not Fear
When it comes to dentistry for kids, focus on fun, not the fear. Find out more on taking the fear out of visiting the dentist for kids.
Read More.png)
Dental Visits
Dentistry For Kids: Rise Of The Kid-Friendly Dentist
Over the years, dentistry for kids has grown to help parents and children experience less anxiety brought on by oral health issues. Learn more, here.
Read More
Dental Visits
Discount Dental Work Through a Dental School
It's important to get dental care when you need it, so what's a patient to do with a tight budget? You might consider treatment through a dental school.
Read More
Dental Visits
Overcoming Fear and Anxiety At the Dentist's Office
Keep in mind the apprehension of going to the dentist can also be learned and passed down from parent to child. Learn more here.
Read More
Dental Visits
Does My Child Need Infant Dental Care
As you cradle your infant in your arms and gaze into his cherubic smile, you might naturally wonder when your child will need to see a pediatric dentist.
Read More
Dental Visits
Exodontia: What You Need To Know About Tooth Extraction
Tooth extraction, or exodontia, is a common procedure. Occasionally, complications can occur after tooth extraction. Here's what you need to know.
Read More
Dental Visits
Family Dental Practice: What It Is And The Best Way To Find One
Busy parents know scheduling appointments for everyone in your family can take time. Finding a family dental group can mean fewer individual office visits, if you know where to look.
Read More
Dental Visits
Finding A Family Dentist That You And Your Kids Love
Find out more about what's important for kids and parents alike when choosing a dentist. Find a family dentist you and your kids love today!
Read More
Dental Visits
5 Helpful Cosmetic Dentistry Procedures You Should Know About
Learn more about oral care for adults, including how to properly brush and floss, adult toothbrushes, and much more, from the Colgate Oral Care Center.
Read More
Dental Visits
Getting a Dental Impression: How To Cope With Your Gag Reflex
Dental impressions are never comfortable, but for those with a gag reflex, is a nightmare. Learn to cope with your gag reflex when getting a dental impression.
Read More
Dental Visits
How A Dental Hygienist Education Benefits A Dental Practice
A dental hygienist education not only spans at least two years, but it also requires one to become licensed before they can practice. Learn more, here.
Read More
Dental Visits
How a Strong Doctor-Patient Relationship Can Improve Your Smile
By learning more about what your dentist does to make you feel comfortable in their office, you can build a strong, lifelong doctor-patient relationship.
Read More
Dental Visits
How Does A Tooth Polishing Procedure Work?
Many dental practices offer polishing after a dental treatment or as the final stage of a routine dental visit. Learn more about tooth polishing here.
Read More
Dental Visits
When Should Kids Go to The Dentist
How often should you go to the dentist after a first appointment? Six months? A year? Ideally, you should take your child to the dentist every six months.
Read More
Dental Visits
How Preventive Dentistry Keeps Teeth Clean at Any Age
From daily brushing to annual dental cleanings, preventive dentistry is designed to avoid gum disease, cavities, enamel wear and more. Here's how.
Read More
Dental Visits
How To Find A 'Kid-Friendly' Dental Health Center
Tooth decay can start when a child's first tooth appears. Finding a dental health center that is compatible with kids is vital. Here's how to choose.
Read More.png)
Dental Visits
How To Find A Good Pediatric Dentistry Practice
Find out everything you need to know about how to find a good pediatric dentistry practice in your area, courtesy of the Colgate Oral Care Center.
Read More
Dental Visits
How to Find an Affordable Dentist
Those without insurance believe an affordable dentist is out of reach, but these regular dental visits are a must. Here's how to find care in your budget.
Read More
Dental Visits
How To Get Your Teeth Clean Before The Dentist
Brushing your teeth is one thing, but brushing them properly gives you completely different results and clean teeth for your checkup.
Read More
Dental Visits
Individual Dental Insurance 101: Your Guide To Choosing A Plan
Dental insurance helps you get the oral care you need. Learn if individual dental insurance could be right for you and, if it is, how to choose a plan.
Read More
Dental Visits
Medical Identity Theft: How to Ensure Your Safety
Learn how medical identity theft works, who's most at risk and how you can ensure your family stays safe.
Read More
Dental Visits
Men's Guide To Dental Care
When it comes to dental care, men and women aren't the same. Men are often at higher risk for common issues, and should do the following to stay healthy.
Read More
Dental Visits
Moving Checklist For Your Dental Needs
One thing to add to your moving checklist is finding a new dental care professional once you arrive at your new home. Find your moving checklist, here.
Read More
Dental Visits
Moving Tips: How To Find A New Dentist
One of the most important moving tips isn't how you pack your china, but when and how you choose a new dentist. Learn more on moving tips, here.
Read More
Dental Visits
National Dentist Day: Ten Ways Your Dentist Protects Your Health
National Dentist Day is a great time to celebrate everything your dentist does for your health. Here are 10 things your dentist does that you should honor.
Read More.png)
Dental Visits
Oral Health America And Seven Things It Believes In
Oral Health America is a not-for-profit, founded in 1955 and based in Chicago. The company hosts numerous programs in the name of oral health.
Read More.png)
Dental Visits
Oral Health In America: Are Americans Seeing The Dentist?
Nearly one in three Americans are not visiting the dentist — a poor reflection on oral health in America. Find out more about oral health in America, here.
Read More
Dental Visits
Pedodontist: A Dentist For Children
Sometimes known by the archaic term pedodontist, a pediatric dentists specialize in working with kids. Find out if one is right for your family.
Read More.png)

Dental Visits
10 Signs You Have the Best Dentist
If you're wondering whether or not yours is top of the line, consider these 10 things all good dentists do for their clients.
Read More
Dental Visits
The Changing World of Digital Dentistry
Dental technology is an exciting field that is constantly changing. Learn how your dentist uses digital dentistry to help give you the best care possible.
Read More
Dental Visits
The History Of Dentistry
A look at the history of dentistry will help you understand where the conveniences of modern dentistry came from and how they led to today's practices.
Read More
Dental Visits
The Role Of A Sedative Filling In A Pulp Cap Procedure
A sedative filling is placed into a decayed tooth as part of a pulp cap procedure. Here's how it can help save your tooth.
Read More

Dental Visits
10 Common Questions To Ask Your Dentist
At each appointment, asking dental questions is an important part of your long-term healthcare. Here are 10 you should get the answers to.
Read More
Dental Visits
Understanding Deep Sedation At The Dentist's Office
With some types of dental work, your dentist might recommend a type of anesthetic like deep sedation. Learn all about deep sedation and what it's used for.
Read More
Dental Visits
What a Dental Clinic Can Do for You
A dental clinic can house all of your dental needs under one roof. But there is more than one kind of specialist in this type of facility. Learn more here.
Read More
Dental Visits
What Does a Dentist Do?
You might be thinking, \"I brush my teeth and I floss, so why do I need to visit the dentist? What does a dentist actually do?\" The truth is that brushing and flossing aren't enough! Beyond good oral hygiene, regular dental examinations prevent most dental diseases.
Read More
Dental Visits
What Happens at a Dental Prophylaxis Appointment?
Has your doctor or dentist recommended a dental prophylaxis appointment? Find out what you can expect during your dental prophylaxis appointment, here.
Read More
Dental Visits
What Is A Holistic Dentist And Should You See One?
If you're interested in alternative medical treatments, you might have considered seeing a holistic dentist. Here's what to know and expect.
Read More
Dental Visits
What Is A Pediatric Dentist?
Pediatric dentists fill a vital role in oral medicine; here are some answers to a few questions you may have about them.
Read More
Dental Visits
What Is An Alginate Impression?
Alginate impression material helps dentists take accurate impressions of the teeth for a variety of devices and treatments. Learn more.
Read More
Dental Visits
What Is an Odontoplasty?
Dental patients have more ways than ever to perfect their smile. Here's a closer look at one option: odontoplasty, or tooth recontouring. Learn more, here.
Read More
Dental Visits
What Is CEREC in Dentistry?
The term CEREC as used in dentistry stands for Chairside Economical Restoration of Esthetic Ceramic. This is a system that uses CAD/CAM to fabricate dental restorations.
Read More
Dental Visits
What Is Laser Dentistry?
In laser dentistry, lasers are used to remove or alter hard and soft tissues in a variety of dental procedures. Consult your dentist to learn more.
Read More
Dental Visits
What To Ask A Dentist At Your First Appointment
Find out more about what you should ask your dentist on your first dentist appointment. Learn more, here.
Read More
Dental Visits
Why Your Dentist Might Use A Rubber Dam
A rubber dam — also called a dental dam — is a protective sheet that a dentist places over a tooth during dental treatment. Here's why it is important.
Read More
Dental Visits
Your Child's First Dentist Appointment: Calming Their Fears
The day your child has their first dentist appointment is a landmark occasion. Find out what you need to know about your child's first dentist appointment.
Read More
Dental Visits
How Often Should You Go To The Dentist?
While it’s true that a twice-yearly cleaning schedule is a good rule of thumb for many people, scheduling dental visits should be based on each person’s oral hygiene, habits and medical conditions.
Read More
Dental Visits
How to Prepare for Your Child's First Dental Visit
The arrival of baby teeth is momentous for kids. Learn more about your child's first dental visit and what you can expect.
Read More
Dental Visits
Coronal Polishing: What It Is and When You Might Need It
Coronal Polishing: what it is and when you might need it. Click here to learn more here on how coronal polishing differs from a routine dental cleaning.
Read More
Dental Visits
What's Included in Dental Records and How Can You Access Yours?
Your dentist takes detailed notes on your oral health history and treatments. Here is what's included in your dental records and how you can access yours.
Read More
Dental Visits
When to See an Endodontist vs. Periodontist
Here's how to determine which specially trained dentist — an endodontist vs. periodontist — you should see for certain dental care needs.
Read More
Dental Visits
What is CBD? Can CBD Reduce Anxiety Around Going to the Dentist?
How CBD oil can help reduce anxiety before your next trip to the dentist? Colgate is here to provide information on what CBD can do & research.
Read More
Diabetes & Other Endocrine Disorders
Can You Get Diabetes from Eating Too Much Sugar?
Can you get diabetes from eating too much sugar? The answer is complicated, but diets and lifestyles can lead to this disease. Learn more, here.
Read More
Diabetes & Other Endocrine Disorders
Dental Care For Diabetics: Five Conditions To Watch For
Uncontrolled diabetes, diabetic medications and high blood sugar levels can cause decreased saliva flow and a dry mouth, according to the American Diabetes Association.
Read More
Diabetes & Other Endocrine Disorders
Diabetes and Oral Health: What You Should Know
Diabetes conditions can result in a greater risk of oral infection. Find out more on how to avoid complications and maintain your oral health here.
Read More.png)
Diabetes & Other Endocrine Disorders
Diabetes And Dental Treatment: What You Should Know
Dealing with diabetes and dental treatment can be tricky. Diabetes can lead to oral health complications, and it's important to balance both health areas
Read More.png)
Diabetes & Other Endocrine Disorders
Diabetes And Teeth: Brushing Up On Oral Health
Diabetics are at extra risk of gum disease. Let's take a look at the connection between diabetes and teeth to see how you can protect yourself.
Read More
Diabetes & Other Endocrine Disorders
Diabetes And Dry Mouth
Why do diabetes and dry mouth often occur in the same patients? Two of the main causes of dry mouth for people with diabetes are medication side effects and high blood sugar levels.
Read More
Diabetes & Other Endocrine Disorders
Can Diabetes Cause Gum Disease?
How diabetes can potentially lead to problems with teeth and gums. Learn more on how to detect and treat Gum Disease caused by diabetes.
Read More
Diabetes & Other Endocrine Disorders
Prevent Diabetes Problems, Keep Your Teeth And Gums Healthy
Use this page to learn about tooth and gum problems caused by diabetes. You will learn the things you can do each day and during each year to stay healthy and prevent diabetes problems.
Read More
Diabetes & Other Endocrine Disorders
Salty Taste in Mouth & Diabetes: Complications and Remedies
People with diabetes may suffer from a taste disorder that causes a salty, bad or sour taste in the mouth. Learn more about this here.
Read More
Diabetes & Other Endocrine Disorders
What Causes Diabetes?
A description of what causes diabetes depends on whether you have type 1, type 2 or the version brought on by pregnancy. Learn more with Colgate.
Read More
Diabetes & Other Endocrine Disorders
What Causes Hypoglycemia And How Does It Affect Diabetics?
According to the American Diabetes Association and the Endocrine Society , new guidelines have been developed to make clinicians aware of the effects...
Read More
Diabetes & Other Endocrine Disorders
How Does Type 1 Diabetes Affect Your Teeth?
What is type 1 diabetes? It's a disease in which the pancreas is unable to produce insulin. Insulin is a hormone that controls the amount of glucose (sugar) in the blood.
Read More
Diabetes & Other Endocrine Disorders
Diabetes Patients Should Pay Close Attention to Oral Health
Diabetes can lower the body's resistance to infection, and periodontal abscesses can develop. Learn more about the signs of periodontal disease, here.
Read More
Veneers
3D Printed Dental Veneers: What You Need To Know
3D printing technology is increasingly used in dental service industry. If you are interested in getting dental veneers, find out if 3D printed veneers are right for you.
Read More
Veneers
Are Removable Veneers Possible?
Removable veneers are much less expensive, but they don't offer many of the advantages of permanent veneers. Learn the difference here.
Read More
Veneers
Can You Whiten Veneers?
After a few years your once-bright veneers may look discolored. Can you whiten veneers? Find out more about caring for your veneers and keeping them white.
Read More
Veneers
All About Veneers: How Long They Last and How To Care For Them
How long do veneers last? The answer depends heavily upon how you care for them. Learn how to care for them and more, here.
Read More
Veneers
How Porcelain Dental Veneers Can Rebuild Your Smile
If unattractive teeth make you hide your smile, it may be time for an oral makeover. Here's how porcelain dental veneers can help.
Read More
Veneers
Porcelain vs Composite Veneers: Which Are Better for You?
What type of veneer would be a good fit for you: porcelain or composite? Learn more about veneers before booking your appointment.
Read More
Veneers
Porcelain Vs. Prepless Veneers
How are porcelain and prepless veneers different? These veneers are intended to strengthen teeth and improve the appearance of your smile. Learn more here.
Read More
Veneers
What Are Snap on Veneers?
You may already be familiar with traditional veneers, but there is a less-permanent option: snap on veneers. Learn more about snap on veneers here.
Read More
Veneers
Will a Gum Veneer Help Your Receding Gums?
When the gums recede, the roots of the teeth become exposed, so the teeth look longer. A gum veneer can help improve the look of receding gums.
Read More
Veneers
Dental Veneers: Pros And Cons
Your smile is one of the first features that most people will notice. Click here to find out the pros and cons of dental for your teeth with Colgate.
Read More
Tooth Fairy
A Fun Tooth Fairy Poem To Share With Your Child
Find this fun tooth fairy poem to share with your child. It's a fun way to add a touch of magic to your little one's special day. Find out more, here.
Read More
Tooth Fairy
A Tooth Fairy Story To Encourage Children To Brush And Floss
Sarah, a mom in New York, shared a charming and unique tooth fairy story. She told her children there are several tooth fairies because it's way too much work for just one fairy.
Read More
Tooth Fairy
Oral Hygiene Tips To Make The Tooth Fairy Happy
It's not always easy to convince kids to take proper care of their teeth, especially when they're still young. Find these dental tips to make the tooth fairy happy.
Read More
Tooth Fairy
Designing A Tooth Fairy Letter Template
Find this tooth fairy letter template and more information on designing a your own tooth fairy letter template, for when your child loses their tooth.
Read More
Tooth Fairy
Goodbye Baby Teeth: Celebrating The Tooth Fairy's Last Visit
Say goodbye to your child's last baby tooth. Celebrate the tooth fairy's last visit and make the last baby tooth a special occasion. Find out more, here.
Read More
Tooth Fairy
How Much Money Does The Tooth Fairy Leave Under The Pillow?
No matter what your family's preferred fairy looks like, tooth fairies all leave behind a gift when they collect a tooth, so how much do you leave. Find the most popular answer here!
Read More
Tooth Fairy
How The Tooth Fairy Movie Can Inspire Your Kids
Find out more about how the tooth fairy movie can inspire your kids to achieve better dental health. Learn more, from the Colgate® Oral Care Center.
Read More.png)
.png)
Tooth Fairy
Is The Tooth Fairy Real? Tips For Answering That Question
What should you do when a child asks 'Is the tooth fairy real?' What you do as a parent is up to you, but keep this in mind when answering the tooth fairy question.
Read More
Tooth Fairy
4 Tips on How to Be the Tooth Fairy
An encouraging letter from the tooth fairy, accompanied by a treat, can be sent to praise the child's bravery at the dentist office.
Read More
Tooth Fairy
Tooth Fairy 101
Tooth fairy plays an important role in childhood. Although there are many unique traditions around the world, parents always look for creative ideas to celebrate the loss of their child's baby teeth.
Read More
Tooth Fairy
How to Write a Letter From the Tooth Fairy
A tooth fairy letter can help children answer questions about their teeth as well as encourage kids to take care of their teeth. Find out more, here.
Read More.png)
Tooth Fairy
Top Tooth Fairy Ideas To Make Your Child's Fantasies Real
Losing your first tooth is a memory your child will hold dear. Find these tooth fairy ideas to make your child's fantasies real, courtesy of Colgate® Oral Care.
Read More
Tooth Fairy
Use A Tooth Fairy Certificate To Make Your Child Smile
A tooth fairy certificate not only helps your child take pride in the fact that he lost a tooth, but it serves as a keepsake that documents when and how the milestone took place.
Read More
Tooth Fairy
How to Answer the Question "Is the Tooth Fairy Real?"
Every parent gets hit with a few dreaded questions at some point. Is the Tooth Fairy real? is one of them. Find out how to answer this question, here.
Read More
Developmental Conditions
Amelogenesis Imperfecta: No Enamel on Teeth
What Is Amelogenesis Imperfecta? Click here to find out everything you need to know with this article from Colgate.
Read More
Developmental Conditions
Developmental Disabilities 101
Approximately 52 million Americans suffer from some type of developmental disability. These disabilities can affect the brain, body, and can make everyday dental care a challenge. Learn more, here.
Read More
Developmental Conditions
How Cleidocranial Dysplasia Affects The Teeth
Cleidocranial dysplasia is an extremely rare genetic condition that involves a number of distinctive features, including dental abnormalities. Here's more.
Read More
Developmental Conditions
How to Get Rid of White Spot Lesions on Teeth
Don't let discoloration keep you from smiling. Like most oral issues, figuring out how to get rid of white spots on teeth may be easier than you thought.
Read More
Developmental Conditions
How To Identify And Treat A Lip Tie
Lip tie occurs when the soft tissue that attaches the upper lip to the upper gum interferes with breastfeeding. Learn how to spot and treat lip tie.
Read More


Developmental Conditions
Treating Prognathism: Ways To Correct Abnormal Jaw Alignment
Prognathism is defined as the overdevelopment of either jaw in relation to the other jaw and to the skull. Here's how this condition may be treated.
Read More
Developmental Conditions
What's an Enamel Pearl? Causes, Diagnosis, and Treatment
An enamel pearl is a developmental defect that results in a nodule of enamel developing on the root of a tooth — where it doesn't belong! Learn more here.
Read More
Developmental Conditions
What Is a Bifid Uvula?
Present in some infants at birth, a bifid uvula is a developmental condition, and it is the less serious form of a group of conditions found at birth, such as cleft lip and cleft palate. Learn more here.
Read More
Developmental Conditions
What Is Dentinogenesis Imperfecta?
Dentinogenesis imperfecta is a rare genetic disorder affecting the teeth. What symptoms may point to this diagnosis? How is it treated? Learn more, here.
Read More
Developmental Conditions
What Is Oromandibular Dystonia (OMD)?
You may not have heard of oromandibular dystonia before, perhaps because it's a very rare condition. Learn more about it.
Read More
Developmental Conditions
What Is Regional Odontodysplasia?
Regional odontodysplasia is a rare developmental disorder of the teeth that is characterized by a ghostlike appearance of affected teeth. Learn more here.
Read More
Developmental Conditions
What Is Taurodontism?
Taurodontism is an unusual developmental phenomenon that most often affects the permanent teeth. Learn more about this rare condition and how it's treated.
Read More
Developmental Conditions
Are Oral Health Issues Genetic? 10 Conditions to Know
You inherit many things from your parents. But are oral health issues genetic? The short answer is, some are and some aren't. Learn more.
Read More
Developmental Conditions
What Is a Lisp and What Causes It?
A lisp is a common type of speech impediment. Here's why someone may have trouble making phonetic sounds correctly and what can be done about it.
Read More
Respiratory Conditions
Chronic Sinusitis Symptoms and the Effects on Oral Health
Your sinuses can become inflamed from more than just an infection. For this reason, chronic sinusitis symptoms can have a number of effects on oral health.
Read More
Respiratory Conditions
Do You Need Oral Appliance Therapy?
The answer to a sound night's sleep and improved quality of life may come from a surprising place: oral appliance therapy or a removable oral appliance.
Read More
Respiratory Conditions
The Truth About Post Nasal Drip and Bad Breath
Learn about the relationship between postnasal drip and your dental health and does it cause bad breath?
Read More
Respiratory Conditions
Good Dental Health Can Prevent Respiratory Illnesses
White teeth and pink gums aren't the only benefit of a good dental health. Youcan also reduce the risks of a few common respiratory illnesses. Learn more.
Read More
Respiratory Conditions
The Link Between Lung Conditions and Your Oral Health
Some of the most common lung ailments that can affect your mouth are asthma, chronic obstructive pulmonary disease (COPD), tuberculosis and sleep apnea.
Read More
Respiratory Conditions
How Oral Bacteria Affect Your Lungs
Tooth decay, tender gums and periodontal disease are signs of poor oral health, but did you know oral bacteria also increase the risk of lung infection?
Read More
Respiratory Conditions
Improve Lung Health Through Oral Care
Oral bacteria can cause respiratory problems over time. But with these healthy habits and breathing exercises, you can reduce your risk of poor lung health
Read More
Respiratory Conditions
Is A MouthGuard Necessary For Sleep Apnea?
Sleep apnea is a condition that occurs when you stop breathing while you're sleeping. Your breathing generally resumes on its own after a few seconds or a few minutes.
Read More
Respiratory Conditions
Is It A Teething Cough Or A Cold? Identifying The Source Of Your Baby's Cough
With these tips on identifying the source of the cough, along with your pediatrician's advice, you can get the care your baby needs.
Read More
Respiratory Conditions
The Connection Between Sleep Apnea and Oral Health
People of all ages and both genders are affected by this affliction. Learn more about sleep apena & it's relation to dental issues here.
Read More
Respiratory Conditions
Post Nasal Drip And Bad Breath
A common cause of bad breath is post nasal drip, which involves mucus secretions from your nose and throat
Read More
Respiratory Conditions
Recurring Strep Throat: Causes, Treatment Options and Prevention
If you've beaten strep throat once, you certainly don't want to deal with it again. Yet, some unlucky individuals develop recurring strep throat. Here's what to know about this condition.
Read More
Respiratory Conditions
Respiratory Conditions
Asthma, COPD, Tuberculosis, and other respiratory diseases or conditions can have a significant affect on your oral health, ranging from dry mouth to infections and more.
Read More
Respiratory Conditions
Snoring Aids: Do They Really Work?
Do they actually work? By knowing which snoring aids to use and which to avoid, you might be able to stop snoring once and for all.
Read More

Respiratory Conditions
What Causes Snoring: Its Effect On Oral Health
Snoring is an unmistakable hoarse sound that occurs when a person's airway is partially blocked while sleeping. Learn more here.
Read More
Respiratory Conditions
Respiratory Infections and Oral Health
When you catch a cold or flu, it's usually considered a respiratory infection – something that attacks the respiratory tract but has roots in oral health.
Read More
Respiratory Conditions
Why Does My Tooth Hurt?
If you have symptoms of a cold, the flu or a sinus infection, particularly congestion and pressure in the sinuses, your tooth pain could be related.
Read More
Respiratory Conditions
5 Reasons You Might Experience Pain When Swallowing
Pain when swallowing can be uncomfortable and make it difficult to eat or talk. Here are five possible causes to discuss with your doctor or dentist.
Read More
Respiratory Conditions
How to Manage a Sore Throat From Allergies
For many Americans, allergy season means runny noses and sneezing. If you experience a sore throat from allergies, here's how to find relief.
Read More
Respiratory Conditions
How To Use A Salt Water Gargle For A Sore Throat
Sore throats can be very unpleasant. Using a salt water gargle for a sore throat may help to relieve your discomfort. Here's how.
Read More
Respiratory Conditions
Sore Throat at Night: Causes and Home Treatments
A sore throat at night can disturb your sleep and leave you feeling tired the next day. Here are the possible causes and some home remedies you can try.
Read More
Respiratory Conditions
What's An Oral Appliance For Sleep Apnea And How Does It Work?
An oral appliance for sleep apnea is one common treatment for the condition. Learn about what this oral device does and if it might be a good fit for you.
Read More
Respiratory Conditions
Mouth Taping for Sleep
Waking up with a dry mouth? It can have adverse effects on your oral health. Click here to learn more about mouth taping for sleep with Colgate®
Read More.png)
Early Orthodontics (Braces)
5 Most Common Questions Kids Have About Braces
Getting braces can be a stressful endeavor for parents and children. Take a look at some of the best ways to combat the fear.
Read More
Early Orthodontics (Braces)
All About Fiberotomy
A fiberotomy is a procedure that helps the teeth to stay in their new positions after braces come off. Learn about what a fiberotomy entails.
Read More
Early Orthodontics (Braces)
An Overbite - Braces For Your Child's Best Smile
According to the Mayo Clinic, an overbite is a condition that occurs when your child's top teeth vertically overlap his bottom teeth.
Read More
Early Orthodontics (Braces)
Are Gold Braces Right For You?
These days, braces can be a fun fashion statement. Here's what to know about gold braces versus other options before you visit the orthodontist.
Read More
Early Orthodontics (Braces)
Braces Colors: How To Choose Your Perfect Shade
Braces colors abound! How can you pick the right color for your braces? Learn more here.
Read More
Early Orthodontics (Braces)
Braces Pain: The Gain Is A Beautiful Smile!
Experiencing braces pain? Learn about what causes this discomfort and how to relieve it. Learn more.
Read More
Early Orthodontics (Braces)
Bringing Teeth Into Alignment With Orthodontic Treatment
Advances in Orthodontics technology make appliances such as Braces and Retainers more comfortable and less visible than ever before.
Read More
Early Orthodontics (Braces)
Causes and Remedies of an Underbite in Children
An underbite, also called a Class III malocclusion or prognathism, is a condition in which the lower teeth and jaw protrude in… Read more at Colgate.com
Read More
Early Orthodontics (Braces)
Crossbite: Effects And Treatments
Crossbite is a type of oral misalignment. When the upper and lower teeth close in a bite, the two sets of teeth don't meet correctly. Learn more here.
Read More
Early Orthodontics (Braces)
Early Orthodontics
Learn more about common orthodontic issues in children and orthodontic treatments, including alignment, kids braces, and much more, from the Colgate Oral Care Center.
Read More
Early Orthodontics (Braces)
Five Signs You May Have Enamel Dysplasia
Enamel dysplasia is a condition that affects the normal levels of one's tooth enamel. Those suffering from this deficiency may produce these symptoms.
Read More
Early Orthodontics (Braces)
Foods You Can Eat With Braces
You know to avoid taffy, but what foods are safe and comfortable to eat? Here's a rundown of foods you can eat with braces to keep them intact.
Read More

Early Orthodontics (Braces)
5 Questions to Ask Before Getting Braces Removed
Here are a few common questions and answers about the process of getting braces off. Find out more about getting your braces off and how to prepare.
Read More
Early Orthodontics (Braces)
Getting Braces: What You Need to Know
What to know before getting braces? Learn more about the preparation and procedure of getting braces with this article from Colgate.
Read More
Early Orthodontics (Braces)
Good Dental Hygiene Is Critical For Kids With Braces
Good dental hygiene is crucial for kids with braces. You've seen how excited your child has been anticipating that happy day in… Read more at Colgate.com
Read More
Early Orthodontics (Braces)
Hawley Retainer: Proven To Maintain Your Straight Smile
Once braces treatment has ended, your new smile needs to be maintained by a retainer, the most common of which is the hawley retainer. Learn more, here.
Read More
Early Orthodontics (Braces)
How Long Do You Have to Wear a Retainer After Your Braces Come Off?
How long do you have to wear a retainer? That depends on a variety of things – here's what you need to know when it comes to this varied appliance.
Read More
Early Orthodontics (Braces)
How to Clean Teeth with Braces
Before you brush, rinse with water. This can help loosen any food lodged in and around the braces. When you're ready to brush, start by brushing at the gumline at a 45-degree angle.
Read More
Early Orthodontics (Braces)
How To Choose A Family Orthodontics Practice For Your Kids
Learn more about oral care for children, including how to properly brush kid's teeth, kids toothbrushes, and much more, from the Colgate Oral Care Center.
Read More
Early Orthodontics (Braces)
How To Straighten Teeth Without Braces
Not all conditions require braces. Here's how to straighten teeth without braces, all depending on your condition or what you'd like to see change.
Read More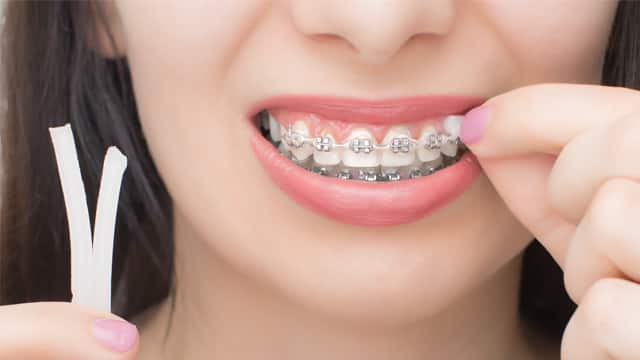
Early Orthodontics (Braces)
How To Use Wax for Braces
What is wax for braces? Dental wax can help you through a rough patch, from irritating brackets to loose wires. Learn more.
Read More
Early Orthodontics (Braces)
How Tongue Thrust Occurs
Here's why tongue thrust can occur, who can be affected, what complications tongue thrusting can cause and how certain retreatment regimens can be used.
Read More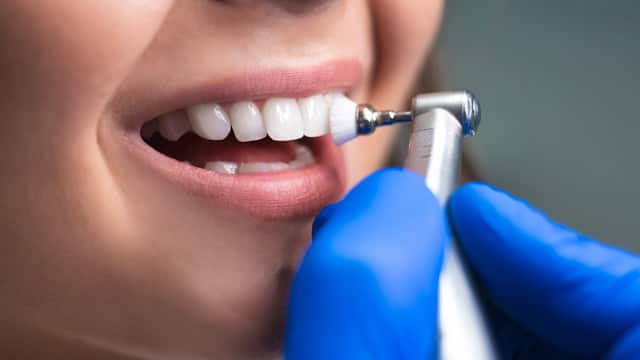
Early Orthodontics (Braces)
How Wearing Braces Headgear Affects Your Teeth Cleaning
Braces headgear isn't a reason for poor oral hygiene provided your child follows the orthodontist's advice and uses the right products and equipment.
Read More
Early Orthodontics (Braces)
Interesting Facts From the History of Orthodontics
Poorly aligned teeth have been a cause for concern as far back as Ancient Egypt. Here's a history of orthodontics through four different time periods.
Read More
Early Orthodontics (Braces)
Kids' Braces Have Come A Long Way
Does the thought of getting your kids braces bring back painful
Read More
Early Orthodontics (Braces)
Overjet vs. Overbite: What's the Difference?
What's the difference between overjet vs. overbite? These conditions describe misalignment of the upper and lower teeth. Here's how they might be treated.
Read More
Early Orthodontics (Braces)
Picking the Best Toothbrush for Braces
Finding the best toothbrush for braces is ideal to keeping the teeth and gums healthy during treatment. Here are a few things you can look for.
Read More
Early Orthodontics (Braces)
Preventing Tooth Decay With Braces
How can you prevent tooth decay with braces? Learn about what causes tooth decay and how you can take care of your smile during orthodontic treatment here.
Read More
Early Orthodontics (Braces)
Protect Your Investment: How to Clean Braces
Knowing how to clean braces properly is essential to ensuring a cavity-free mouth. Click to learn how to clean your braces with Colgate.
Read More
Early Orthodontics (Braces)
Risks Of Fake Braces For Kids
Learn more about common orthodontic issues in children and orthodontic treatments, including alignment, kids braces, and much more, from the Colgate Oral Care Center.
Read More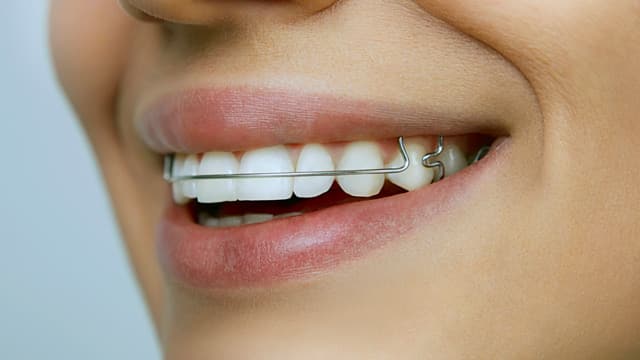
Early Orthodontics (Braces)
Temporary Retainer: A Guide for Wear and Care
Your braces are finally off! Before you get a permanent set, you may be given a temporary retainer. Here's how to wear and care for one.
Read More
Early Orthodontics (Braces)
The Mechanics Of An Upper And Lower Jaw Expander
Not every child's jaw is big enough to accommodate his or her adult teeth. Luckily, upper and lower jaw expanders help make room without extraction.
Read More
Early Orthodontics (Braces)
Types of Underbite Correction Treatments
Doctors can make incredible improvements these days, and an underbite correction is no longer as tedious as it often used to be. Here are your options.
Read More
Early Orthodontics (Braces)
Upper Jaw Expansion For Orthodontic Correction
In some cases, teeth produce crowding and there's simply not enough room for all of them to fit properly. This is where upper jaw expansion comes in.
Read More
Early Orthodontics (Braces)
What Are Gap Bands and Will They Fix Your Teen's Teeth?
Talk to your teen about the dangers of the newest orthodontic trend: trying to close the spaces between their teeth using what's known as a gap band.
Read More
Early Orthodontics (Braces)
What Color Braces Should I Get?
What color braces should I get? In this article, please list some things to consider when someone is trying to decide what color to get for their braces. How can they consider things like their personality, their face structure, etc.?
Read More
Early Orthodontics (Braces)
What Is An Open Bite?
If your child's teeth aren't lining up quite right, he or she may have an open bite.
Read More
Early Orthodontics (Braces)
What Is Orthodontics?
Learn more about common orthodontic issues in children and orthodontic treatments, including alignment, kids braces, and much more, from the Colgate Oral Care Center.
Read More
Early Orthodontics (Braces)
What Is The Best Age For Braces?
While the best age for braces tends to be during the childhood years when teeth are developing, it's never too late to pursue a healthier smile.
Read More
Early Orthodontics (Braces)
When Overbite Correction Can Be Beneficial
Not everyone's teeth are perfectly aligned. Before considering overbite correction, let's define what the condition is and the reasons it may form.
Read More
Early Orthodontics (Braces)
When Upper Jaw Expansion Benefits Your Child
Upper jaw expansion is a form of orthodontic treatment that is used in specific cases. There are numerous benefits depending on a patient's age and need.
Read More
Early Orthodontics (Braces)
Why Does My Child Need A Palate Expander?
Is a palate expander necessary? Is it painful? What does it do? Find out more about how this treatment can help guide the growth of your child's mouth.
Read More
Early Orthodontics (Braces)
How Much Do Braces Cost?
So how much do braces cost for kids? First, it's necessary to identify the type of braces for your child and the duration of the treatment.
Read More
Early Orthodontics (Braces)
Retainers After Braces: Types And Maintenance
Once orthodontic treatment has been completed, the use of retainers after braces is a very important part of the continuing maintenance of teeth. Learn more here about the benefits of retainers after braces.
Read More
Early Orthodontics (Braces)
Broken Braces Or Wires
Braces, bands or wires sometimes break or fall off. Usually this is caused by chewing hard or sticky foods. More often, one of the parts will come loose. This can cause some discomfort. Here are a few possible problems
Read More
Early Orthodontics (Braces)
Bracing Yourself For Their Braces
Learn more about common orthodontic issues in children and orthodontic treatments, including alignment, kids braces, and much more.
Read More
Early Orthodontics (Braces)
Diastema (Gap Between Teeth)
What Is Diastema? A diastema is a space or gap between two teeth. It appears most often between the two upper front teeth. Learn more here.
Read More
Early Orthodontics (Braces)
Do I Need Braces Quiz: Discover If Orthodontics Might Be in Your Future
Are braces in your future? Take this Do I Need Braces quiz to kick-start a conversation with an orthodontist about straightening your smile.
Read More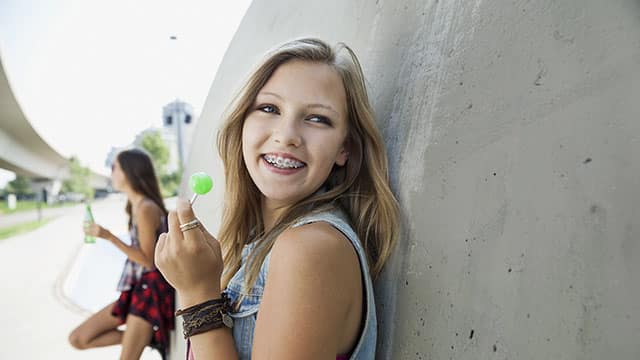

Early Orthodontics (Braces)
Yellow Teeth in Kids: Causes and Treatments
The arrival of permanent teeth is an exciting time for kids and parents. But what if they appear discolored when they come in? Here's what to know.
Read More
Early Orthodontics (Braces)
Why More Adults Are Choosing to Straighten Their Smiles
By: Mandy Dennis
Registered Dental Hygienist
Read More

Heart Disease
How Oral Health and Heart Disease Are Connected
First, recent studies show that if you have gum disease in a moderate or advanced stage, you're at greater risk for heart disease than someone with healthy gums.
Read More
Heart Disease
Periodontal Disease And Cardiovascular Disease
Gum disease is the leading cause of tooth loss, learn ways to identify and treat gum diseases that include Gingivitis and Periodontitis.
Read More
Heart Disease
How Oral Care Can Prevent Heart Disease
Can oral care help prevent heart disease? Click here to learn more about preventing heart disease with good dental hygiene with Colgate ®.
Read More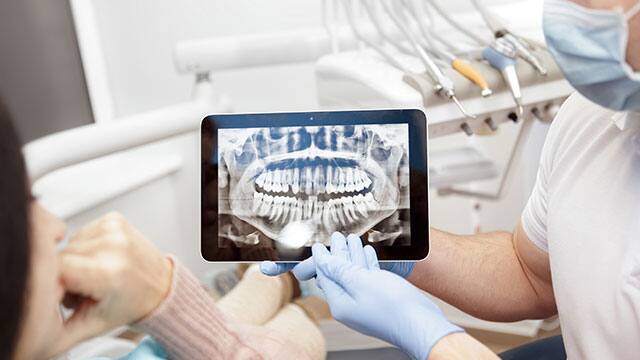
Dental Emergencies & Sports Safety
4 Longitudinal Fracture Issues And How They're Treated
Damaging a tooth, whether it be from a cavity or a traumatic injury, can be troubling. Learn more about these four types of longitudinal fracture issues.
Read More
Dental Emergencies & Sports Safety
Broken Wisdom Tooth: Adverse Side Effects If Left Untreated
Wisdom teeth are the very last of your permanent teeth to come in, and they usually erupt in your late teens or early twenties. Read more at Colgate.com
Read More
Dental Emergencies & Sports Safety
Can I Use Clove Oil for Toothache Pain?
Using clove oil for toothache pain can provide you with relief now, but it doesn't last as long as treatment from your dentist. Here's why.
Read More
Dental Emergencies & Sports Safety
Choose A Custom-Designed Mouth Guard For Sports
When you're shopping for helmets and kneepads before the start of the sports season, don't forget another, often-neglected type… Read more at Colgate.com
Read More
Dental Emergencies & Sports Safety
Cleaning A Mouth Guard
In many sports, a mouth guard is an important piece of equipment for safeguarding your teeth, protecting them from breaking or… Read more at Colgate.com
Read More
Dental Emergencies & Sports Safety
Cut on Gums: Causes, Treatment & Prevention
When a cut on gums ruins your day, here are the signs that you should visit a doctor. Learn more here.
Read More
Dental Emergencies & Sports Safety
Dental Emergencies and Sports Safety 101
Learn more about what you should do in case of a dental emergency and how to prevent dental emergencies from happening. Learn more about preventable measures, here.
Read More
Dental Emergencies & Sports Safety
Dental Emergency First Steps: Do You Know What To Do?
When your little one injures his mouth, keep your composure. Staying calm and collected during a dental emergency reduces your child's anxiety during...
Read More

Dental Emergencies & Sports Safety
Dental Fistula: What Is It?
What is a dental fistula and how can your dentist help make your mouth healthy again? Learn more, here.
Read More
Dental Emergencies & Sports Safety
Do You Need Emergency Dental Care?
Dental emergencies require immediate attention to relieve severe pain, treat high risk of infection or save a tooth that is at risk.
Read More
Dental Emergencies & Sports Safety
Dry Socket: Symptoms and Treatment
Probably one of the most painful, but easy-to-treat dental emergencies is dry socket. Learn more about the symptoms of dry socket and how it happens.
Read More
Dental Emergencies & Sports Safety
Emergency Tooth Extraction: Five Signs To Help You Decide
Knowing whether you need an emergency tooth extraction can be a hard call given advancements in dental and endodontic treatment of late.
Read More
Dental Emergencies & Sports Safety
4 Tips to a Soothe a Burnt Tongue
Oral burns call for a swift response if you want to ease the pain. Fortunately, there are several burning tongue remedies that can help. Learn more here.
Read More
Dental Emergencies & Sports Safety
Four Options For Fixing A Chipped Tooth Fast
Fixing a chipped tooth as soon as it happens ensures your mishap doesn't cause further problems, but what are your options? Find out more, here.
Read More
Dental Emergencies & Sports Safety
Front Tooth Replacement: What's The Best Option For You?
When you were a child, losing your front teeth was an exciting rite of passage. As an adult, a chipped or missing front tooth isn't as cute. Usually the result of some type of trauma, a chipped, cracked or accidental removal of your front tooth can leave you in pain and feeling self-conscious. With proper care, however, you won't have to deal with pain and embarrassment for long. Front tooth replacement options depend on the condition of remaining teeth, and your dentist can help you choose one of the following ways to fix your teeth and restore your smile.
Read More
Dental Emergencies & Sports Safety
Getting A Mouthguard For Braces
Getting braces can be big transition in the life of your pre-teen or teenager. Becoming accustomed to having foreign objects on… Read more at Colgate.com
Read More
Dental Emergencies & Sports Safety
Handling A Medical Emergency: What Your Dental Professional Should Do
Did you ever wonder what would happen if you developed a serious medical emergency in your dentist office? Maybe not but are their office or staff...
Read More
Dental Emergencies & Sports Safety
Helmets And Mouth Guards
Safety equipment protects faces from harm. More than 200,000 oral injuries are prevented by mouth guard use. Learn more here.
Read More
Dental Emergencies & Sports Safety
How A Moldable Mouth Guard Protects Teeth In Sports
Many physical activities carry a risk of injury to the mouth, jaw or teeth. A moldable mouth guard provides protection in these situations.
Read More
Dental Emergencies & Sports Safety
How an Alveolar Fracture Can Occur in Sports
A mouth injury doesn't often receive much thought, but an alveolar fracture can be a true cause for concern. Here's how they typically occur.
Read More
Dental Emergencies & Sports Safety
Tips for Emergency Dental Care For Kids
Kids fall a lot, and mouth injuries are therefore very common. Knowledge of emergency dental care for kids can keep them from accidentally losing a tooth.
Read More
Dental Emergencies & Sports Safety
How To Deal With Your Child's Chipped Tooth
Every parent knows it's hard to keep children still for too long. Kids today love to run round the house, jump on furniture and… Read more at Colgate.com
Read More
Dental Emergencies & Sports Safety
How To Find An Emergency Dentist When You Need One
If you're faced with a dental issue, it can be hard to tell if you should go to an emergency dentist. Here's how to get the care you need.
Read More.png)
Dental Emergencies & Sports Safety
How To Keep An Athletic Mouth Guard Clean
One of the greatest inventions in safety equipment for athletes is the athletic mouth guard. These devices help to safeguard… Read more at Colgate.com
Read More
Dental Emergencies & Sports Safety
How to Prevent a Tooth Root Fracture During Sports Activities
One sports-related injury that is not so easily visible is a tooth root fracture. Here's how to safeguard your teeth during your favorite athletic events.
Read More
Dental Emergencies & Sports Safety
How To Protect Your Teeth During Sports
Learning how to protect your teeth when playing a sport or similar close-contact activity isn't as difficult as the frequency of these incidents suggests.
Read More
Dental Emergencies & Sports Safety
I Bit My Tongue. What Now?
Oh no, I bit my tongue! Biting your tongue is upsetting and uncomfortable, but tongue injuries are rarely serious and you can often treat them at home.
Read More
Dental Emergencies & Sports Safety
Identifying A Bruised Tooth
Hearing about a bruised tooth can be alarming. Will the tooth heal? Will it actually turn black & blue? Find out more about identifying and treatment here.
Read More.png)

Dental Emergencies & Sports Safety
Injured Tooth: What Should I Do?
If a tooth is completely knocked out of the mouth by an injury, take the tooth to your dentist as soon as possible. Learn more here.
Read More
Dental Emergencies & Sports Safety
Lip Injury From Sports: Types And Treatments
A lip injury is one of the most common oral lacerations. Here are the common sports-related lip wounds than can occur, and how to respond accordingly.
Read More
Dental Emergencies & Sports Safety
Mandible Fracture: Symptoms and Treatment
A jawbone or mandible fracture is serious, but an oral surgeon can set the bone back in place. Learn more about symptoms and treatment here.
Read More.png)
.png)
Dental Emergencies & Sports Safety
Mouth Guards: Every Mom's Oral Health Insurance Policy
When your kids play sports, you do everything you can to keep them safe. You invest in protective gear and footwear and get approval from your pediatrician
Read More
Dental Emergencies & Sports Safety
My Child Has A Knocked Out Tooth: What Should I Do?
A knocked out tooth is a manageable emergency for parents who know what to do.
Read More
Dental Emergencies & Sports Safety
Oral First Aid At Home
You probably have a first aid kit in your home to handle life's minor bumps and bruises. But are you prepared for a dental emergency?
Read More
Dental Emergencies & Sports Safety
Safety Chart
Dental injuries can often be prevented — especially if you know what to watch out for. In this article you will find a chart that can help you do just that.
Read More.png)
Dental Emergencies & Sports Safety
Seeking Treatment For Oral Care Problems In Emergency Rooms
Hospital emergency rooms are seeing an increase in people visiting with routine oral care problems.
Read More
Dental Emergencies & Sports Safety
Sports Dentistry: Athletes Need Dentists?
How does the branch of sports dentistry differ than primary dentistry? Find out more about sports dentists and how their specialty helps athletes, here.
Read More
Dental Emergencies & Sports Safety
Swollen Lip Causes And Treatments
Trauma, allergic reaction, infection, and additional blood flow are swollen lip causes. When should you visit your doctor? Learn more, here.
Read More
Dental Emergencies & Sports Safety
Swollen Tongue: Causes And Treatments
A swollen tongue may be due to an injury, infection or irritation, but a common cause is a food allergy. Breathing problems require emergency treatment.
Read More
Dental Emergencies & Sports Safety
The Three Most Common Dental Injuries in Sports and How to Prevent Them
Every year, 5 million Americans lose teeth in a sports-related tooth injury. Luckily, dentists can repair almost any of the most common three types.
Read More
Dental Emergencies & Sports Safety
The 5 Classifications of Tooth Luxation
Tooth luxation is the dislodgement of a tooth, sometimes invisibly, from an injury to the ligaments and tissues holding the tooth in place. Learn more.
Read More

Dental Emergencies & Sports Safety
Can A Tooth Crack In Half And Be Fixed?
One moment you're biting into a crisp, flatbread pizza, and the next, you've got a tooth cracked in half. There are a few reasons why this can happen.
Read More
Dental Emergencies & Sports Safety
Treating A Tongue Injury From Sports
Incidents such as spraining your ankle during basketball are to be expected, but a tongue injury can still result from the unexpected. Here's how.
Read More
Dental Emergencies & Sports Safety
Use Football Mouthguards And Stay In The Game
Between tackles, blocks and personal fouls, football is filled with physical contact that can result in serious injuries to play...
Read More
Dental Emergencies & Sports Safety
Using A Braces Mouth Guard In Sports
A braces mouth guard protects braces as well as the teeth, gums and jaw, and options are available to suit most needs and budgets
Read More
Dental Emergencies & Sports Safety
Here’s What You Need To Know About Sports Mouthguards
Learn about various sports mouth guards and how these different types of dental mouth guards are created.
Read More.png)
Dental Emergencies & Sports Safety
What Is A Mouthpiece For Braces?
There are a few different types of mouth guards available from your orthodontist and some specialty retailers. Learn more about them here.
Read More
Dental Emergencies & Sports Safety
What To Do If Your Filling Falls Out: Don't Panic, Just Call The Dentist
Wondering what to do if your filling falls out? A phone call to the dentist is your first step. At the dental office, the dentist will determine the necessary treatment.
Read More
Dental Emergencies & Sports Safety
What To Do With A Broken Tooth
Breaking a tooth is traumatic, but quick action and a visit to the dentist can fix and prevent long-term problems. Find out what to do with a broken tooth here with Colgate.
Read More.png)
Dental Emergencies & Sports Safety
What To Do With A Knocked-Out Tooth
Do you know what to do with a knocked-out tooth? Whether the cause is sports, an accident, or assault, it is important to know… Read more at Colgate.com
Read More
Dental Emergencies & Sports Safety
Why Do You Need a Mouthguard?
According to the ADA, more than 200,000 oral injuries are prevented each year by wearing a mouth guard. This is why you need a mouth guard while playing a sport.
Read More

Dental Emergencies & Sports Safety
What To Do If Your Filling or Crown Falls Out: Don't Panic, Just Call The Dentist
If you have fillings or crowns on your teeth, it can be scary when you feel them floating in your mouth and you know that they have fallen out. Read more here about what to do.
Read More
Dental Emergencies & Sports Safety
Tooth Abscess & Gum Abscess
When the inside of your mouth gets hurt or irritated, bacteria may enter and cause an infection. This is known as an abscess. The abscess forms a barrier around the infection. This is one way that your body tries to keep a bacterial infection from spreading.
Read More
Dental Emergencies & Sports Safety
How to Deal with Wounds or Cuts in Your Mouth
How can something so tiny be so annoying and painful? Cuts inside your mouth can happen to anyone. Find out how to treat inner lip or mouth wounds here.
Read More
Dental Emergencies & Sports Safety
Knocked-Out Tooth? Tips on Handling an Avulsed Tooth
Dentists refer to a knocked-out tooth as an 'avulsed' tooth. Though this is one of the most serious dental emergencies, the damage isn't necessarily permanent. Read more information regarding knocked out teeth at Colgate.com.
Read More

Dental Emergencies & Sports Safety
Fractured And Broken Teeth
Present in some infants at birth, a bifid uvula is a developmental condition, and it is the less serious form of a group of conditions found at birth, such as cleft lip and cleft palate. Learn more here.
Read More
Adult Orthodontics (Braces)
A Quick Guide to Getting Braces
Braces are a common orthodontic option used to straighten teeth for people who have crooked teeth or a misaligned bite. They… Read more at Colgate.com
Read More
Adult Orthodontics (Braces)
Adult Braces Before And After: What To Expect When They Come Off
Read More
Adult Orthodontics (Braces)
Adult Orthodontics 101
Find information on orthodontics for adults, including alignment, preventative treatments and maintenance of braces, here.
Read More
Adult Orthodontics (Braces)
Are Ceramic Braces Right For You?
Ceramic braces are well-suited for many patients without severe misalignments. Your orthodontist will let you know if you're a good candidate for these braces after they examine your teeth.
Read More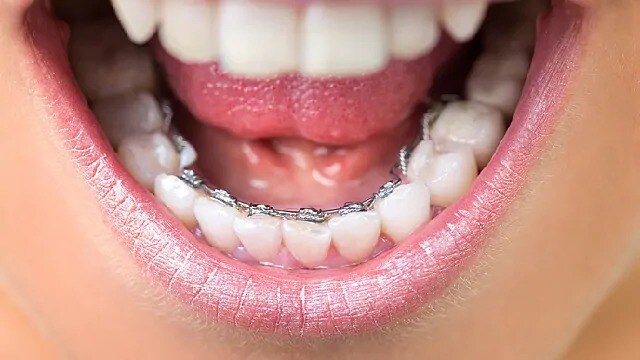
Adult Orthodontics (Braces)
Are Lingual Braces Right for Me?
There are so many options available to those who want to get their teeth straightened today, including lingual braces. But what are lingual braces? Find your answers here.
Read More
Adult Orthodontics (Braces)
Benefits Of Clear Braces For Adults
Are you or your friends considering clear braces for adults? Have you ever wondered about the
Read More
Adult Orthodontics (Braces)
Braces For All Ages: Orthodontic Appliances For Adults
Find information on orthodontics for adults, including alignment, preventative treatments and maintenance of braces, from the Colgate Oral Care Center.
Read More
Adult Orthodontics (Braces)
Broken Retainer? Here's What You Can Do
If you've made the investment in orthodontic treatment to achieve a beautiful smile, don't let a broken retainer undo all that hard work. Find out what you need to do to fix it here.
Read More
Adult Orthodontics (Braces)
Buck Teeth? Three Ways To Minimize Them Without Braces
Whether you feel like your buck teeth are an asset or something that makes you uncomfortable, remember that confidence is key. Find out more here.
Read More
Adult Orthodontics (Braces)
Buying Teeth Aligners Over The Counter And What To Consider
Many people want straighter teeth, and numerous methods are available. Learn if buying teeth aligners over the counter is a good way to improve your smile.
Read More
Adult Orthodontics (Braces)
Can Retainers Realign Your Teeth?
Can retainers realign teeth if you forget to wear yours for a while? It depends... but understanding how retainers work can give you a clearer answer.
Read More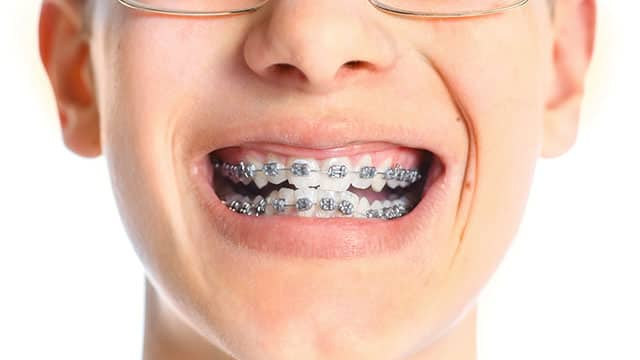
Adult Orthodontics (Braces)
Caring for Braces: You're on Your Way to a Healthy Smile
Caring for braces is an important part of the experience: The better care you take of your braces, the more comfortable and effective they'll be, and the quicker you'll have them taken off.
Read More
Adult Orthodontics (Braces)
Caring For Braces
Orthodontic treatment can be a large financial investment, and the last thing your family needs is a repair cost. Therefore, caring for braces is crucial.
Read More
Adult Orthodontics (Braces)
Clear Aligners Or Metal Braces? Here's How To Choose
Both clear aligners and metal braces are great options for adults. Learn more about options that will turn a crooked smile straight here.
Read More
Adult Orthodontics (Braces)
Clear Braces: A Less Noticeable Way To A Straighter Smile
When a teen finds out he needs braces to correct crooked teeth or a misaligned bite, one of the first concerns he will have is… Read more at Colgate.com
Read More
Adult Orthodontics (Braces)
Clear Retainers: About, Keeping Them Fresh And In Good Shape
With care, clear retainers should last as long as your orthodontist prescribes you to wear it. Find out more about clear retainers and maintenance.
Read More
Adult Orthodontics (Braces)
How to Correct a Crossbite
Dental, orthodontic and surgical treatments are available to correct crossbite. Learn more about crossbite and options for correction, here.
Read More
Adult Orthodontics (Braces)
Do Braces Hurt?
Are you feeling anxious about getting braces? You may be wondering,
Read More
Adult Orthodontics (Braces)
Exploring An Alternative To Braces For Adults
If you aren't eligible for or interested in braces, your orthodontist may recommend an alternative to braces for adults who want to realign their smile.
Read More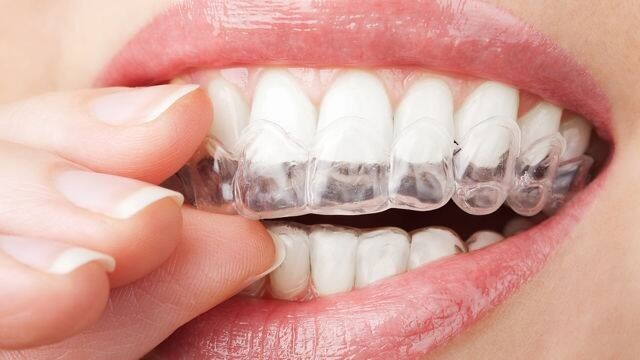
Adult Orthodontics (Braces)
Five Questions To Ask Orthodontic Care Specialists
A general dentist is fine for many people, but some issues require orthodontic care specialists. Ask these questions when looking for an orthodontist.
Read More
Adult Orthodontics (Braces)
4 Reasons You May Have Your Permanent Retainer Removed
If you have a permanent retainer on the back of your teeth, you may consider one of these reasons for a permanent retainer removal in the future:
Read More
Adult Orthodontics (Braces)
How Are Braces Put On? Learn The Basics Of The Brackets
How are braces put on? Knowing what to expect during the process may help you feel more confident about your decision to get braces. Learn more, here.
Read More
Adult Orthodontics (Braces)
How Does A Retainer Work?
Retainers are commonplace in oral care, regardless of age. But how does a retainer work to keep your teeth in position following orthodontia?
Read More
Adult Orthodontics (Braces)
How Headgear Braces Perfect A Misaligned Smile
Find information on orthodontics for adults, including alignment, preventative treatments and maintenance of braces, from the Colgate Oral Care Center.
Read More
Adult Orthodontics (Braces)
How Much Are Braces With Insurance?
When you learn that your child needs orthodontic treatment, cost is one of the first thoughts to cross your mind. So, how much are braces with insurance?
Read More
Adult Orthodontics (Braces)
How To Become An Orthodontist
So, you're wondering how to become an orthodontist? Here's the training and education you would need and what specialties orthodontists focus on.
Read More
Adult Orthodontics (Braces)
Key Differences Between Adult Orthodontics And Kids' Orthodontics
Find information on orthodontics for adults, including alignment, preventative treatments and maintenance of braces, from the Colgate Oral Care Center.
Read More
Adult Orthodontics (Braces)
Lingual Braces Vs. Clear Aligners: How to Choose the Best System for You
A patient needs the facts concerning all types of orthodontic methods before deciding which system suits their needs. Today: lingual braces vs. Invisalign.
Read More
Adult Orthodontics (Braces)
Malocclusion: Getting The Bite Right
One in five people have some sort of malocclusion where their teeth don't line up correctly. Some misalignments are minor and do not need correcting, but
Read More
Adult Orthodontics (Braces)
Misaligned Jaw and Treatment Options
When the upper and lower teeth don't meet comfortably the cause is often a misaligned jaw. Learn more about misaligned jaws as well as treatment options.
Read More
Adult Orthodontics (Braces)
Orthodontic Treatment Advances: Braces Then And Now
Find information on orthodontics for adults, including alignment, preventative treatments and maintenance of braces, from the Colgate Oral Care Center.
Read More
Adult Orthodontics (Braces)
Orthodontist Vs. Dentist: Who Should You See?
It can be confusing to determine the differences between an orthodontist vs. dentist. Here's what you need to know about these dental professionals.
Read More
Adult Orthodontics (Braces)
Retainers for Teeth: What Are They and Why Wear Them?
Although retainers for teeth are most commonly used to hold straight teeth in place after braces, the advantages go well beyond that. Here are a few:
Read More
Adult Orthodontics (Braces)
Spacers: Preparing Your Teeth for Braces
Even if you've had braces, you might not realize all the parts that make them function. Spacers for braces are just one of those parts. Learn more, here.
Read More
Adult Orthodontics (Braces)
Teeth Reshaping After Braces And Other Ways to Perfect Your Smile
You can use retainers, teeth whitening procedures, contouring and teeth reshaping after braces come off to perfect your smile.
Read More
Adult Orthodontics (Braces)
Teeth Reshaping Treatments and Costs
Teeth reshaping is a cost-effective way to fix chipped teeth. It's usually combined with bonding to create a beautiful new smile.
Read More
Adult Orthodontics (Braces)
The Benefits Of Invisible Braces
The idea of getting braces is not a pleasant one, but now the option of invisible braces helps remove some of the stigma, as… Read more at Colgate.com
Read More
Adult Orthodontics (Braces)
The Cost Of Invisalign Compared To Traditional Braces
Most orthodontists will offer patients Invisalign as an alternative to traditional braces, but does Invisalign cost more than it's worth?
Read More
Adult Orthodontics (Braces)
The Risks Of At-Home Braces
The use of at-home braces is a newer concept in dentistry that has many in the profession concerned. Learn more about at home braces and the risks, here.
Read More
Adult Orthodontics (Braces)
Tips For Adults With Braces
When you have braces on teeth, those teeth need extra attention to protect them from decay, staining and gum disease. You should also take precautions to avoid damaging the braces.
Read More
Adult Orthodontics (Braces)
Transparent Braces: Are They Right For You?
As an adult, the idea of wearing prominent metal braces may not be appealing, but there are many types of transparent braces that are less noticeable.
Read More
Adult Orthodontics (Braces)
Wearing And Caring For Your Retainer
Discover techniques for wearing and caring for your dental retainer. Orthodontic retainers are an important part of the orthodontic process and should be worn often. Find out more information at Colgate.com.
Read More
Adult Orthodontics (Braces)
What Are High Speed Braces?
You may not have the time or need for full-length braces, but still want a better smile. High Speed Braces is a new form of short-term orthodontics.
Read More
Adult Orthodontics (Braces)
What Are Lingual Braces?
Lingual braces, one of the more recent forms of orthodontic work, is proving popular for people conscious about the look of braces.
Read More
Adult Orthodontics (Braces)
What Are Nano Braces And Are They Right For You?
Nano braces, also referred to as
Read More
Adult Orthodontics (Braces)
What Are Power Chain Braces?
What are power chain braces and why might an orthodontist recommend them? Find out more about power chain braces and if they're right for you, here.
Read More
Adult Orthodontics (Braces)
What Are The Different Types Of Braces, and Which Is Right for Me?
Your orthodontist may recommend any of the following types of braces or dental appliances to help correct your particular problem.
Read More
Adult Orthodontics (Braces)
What Causes Crooked Teeth?
Crooked teeth can have a variety of causes, from genetics, malnutrition and oral habits to dental disease and poor dental hygiene. Learn more, here.
Read More
Adult Orthodontics (Braces)
What Do Incognito Braces Cost?
Unlike traditional braces, incognito or lingual braces are placed on the back of your teeth and cannot be seen easily. This… Read more at Colgate.com
Read More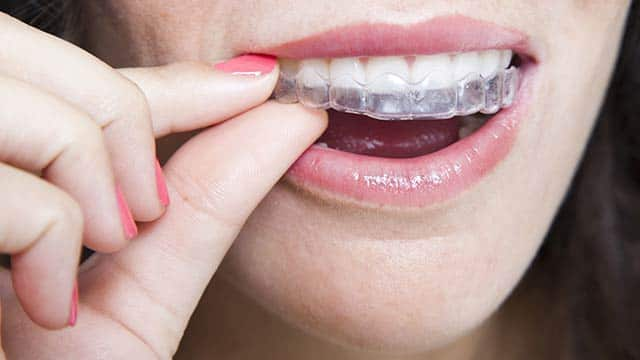
Adult Orthodontics (Braces)
Are Clear Aligners Worth the Cost?
Are you considering Invisalign braces? Invisalign is a type of orthodontic treatment that helps to straighten teeth without the use of the typical metal braces.
Read More
Adult Orthodontics (Braces)
What Is Orthognathic (Jaw) Surgery and How Much Does it Cost?
Orthognathic surgery is a corrective jaw surgery that straightens or realigns your jaw, and corrects related skeletal deformities that a patient may need.
Read More
Adult Orthodontics (Braces)
What is Dentsply Sirona ESSIX® Retainer?
Your orthodontist may recommend an ESSIX® retainer as the final stage in a course of orthodontic treatment, or an alternative to braces. Learn more here.
Read More
Adult Orthodontics (Braces)
What Is Tooth Wax?
Tooth wax, also called dental wax, is a soft material that can be used to temporarily cover sharp surfaces inside your mouth.
Read More
Adult Orthodontics (Braces)
What Swollen Gums with Braces Means for Your Oral Health
When receiving orthodontia for straighter teeth, you may find swollen gums with braces come with the territory. Here's how to care for them.
Read More
Adult Orthodontics (Braces)
Why Dental Braces For Adults Aren't So Bad
Many adults avoid braces, but they remain embarrassed about their crooked teeth. Dental braces for adults are not uncommon, and the benefits can be large.
Read More
Adult Orthodontics (Braces)
Why Does Teeth Shifting Happen?
Teeth shifting out of alignment can occur for several reasons other than when braces are removed. Learn more about preventative tips for teeth shifting.
Read More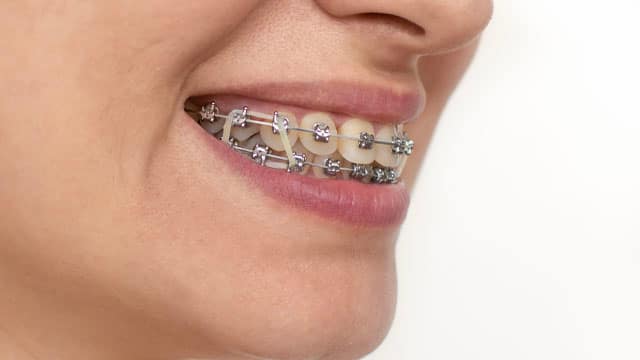
Adult Orthodontics (Braces)
Why Should You Use Rubber Bands With Braces?
Why do orthodontists use rubber bands with braces? Rubber bands are an important part of the orthodontic treatment. Learn more here.
Read More
Adult Orthodontics (Braces)
6 Ways to Get Affordable Braces
Orthodontic treatment is expensive, and often out of reach for the average person. However, there are a number of ways to find affordable braces. Find out more here!
Read More
Adult Orthodontics (Braces)
4 Things to Do When a Braces Bracket Breaks
A broken braces bracket is the most common inconvenience orthodontic patients face when wearing traditional braces. Follow these four steps to help fix your broken braces bracket.
Read More
Adult Orthodontics (Braces)
How To Clean Retainers
The two most common types of removable retainers are the Hawley retainer and the ESSIX® retainer. Learn how to clean retainers and avoid plaque buildup.
Read More
Adult Orthodontics (Braces)
Managing Discomfort Caused by the Rubber Bands on Braces
Braces can get you the straight smile you've always wanted, but they can sometimes cause pain. Here are some ways to manage rubber band braces pain.
Read More
Adult Orthodontics (Braces)
What Is Orthotropics?
Orthotropics is a branch of dentistry that treats teeth misalignment by correcting oral and head posture. Learn more about this specialty.
Read More
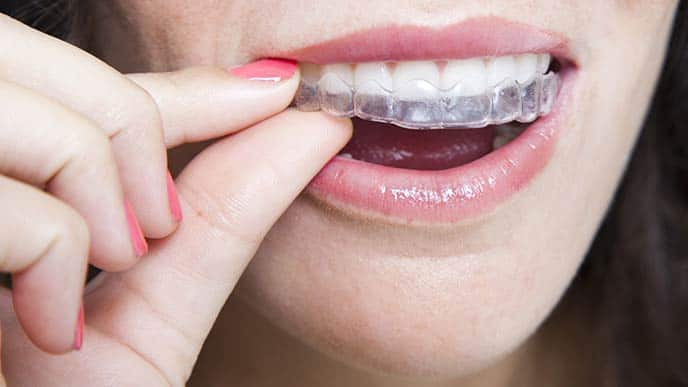
Adult Orthodontics (Braces)
Alternatives for Metal Braces: The Best Way to Straighten Your Teeth
Braces can make a huge difference in a person’s smile and self-confidence. However, wearing traditional metal braces for two or three years might not fit some lifestyles.
Read More
Adult Orthodontics (Braces)
What Are Damon Braces? Four Things You Should Know
Traditional braces can add to an already stressful school year for your kids. What are Damon braces? A solution to crooked teeth, minus tightening pain.
Read More
Adult Orthodontics (Braces)
What is a Bite Block?
What are bite blocks? How are they helpful if you have braces? Click here to learn more about bite blocks with Colgate®
Read More
Adult Orthodontics (Braces)
Clear Aligners 101: Aligner Attachments
What are clear aligners? Click here for the low-down on all things clear aligner attachments including their benefits and their costs with Colgate®.
Read More
Cleft Lip/Palate
Cleft Lip Causes, Drugs And Medications
Cleft lip is a birth defect characterized by a separation of the upper lip and can occur on one or both sides. Find out more about drugs and risks for newborns.
Read More
Cleft Lip/Palate
Cleft Lip Ultrasound
An ultrasound gives you a first glimpse of your growing baby and it can also show any birth defects such as a cleft lip. Here's why that's helpful.
Read More
Cleft Lip/Palate
Cleft Lip/Palate 101
Find out more about cleft lips and cleft palates from Colgate® Oral Care. Learn more about identifying a cleft lip and how cleft lips and cleft palates are treated.
Read More
Cleft Lip/Palate
How Does Your Child’s Cleft Palate Affect Their Oral Health?
How does a cleft palate affect your child's oral health? What can you do to take care of their smile? Learn more about oral clefts and teeth, here.
Read More
Cleft Lip/Palate
Identifying Cleft Palate Symptoms
Cleft palate is the result of a baby's upper jaw not fully closing during pregnancy. Learn what to look for to identify the symptoms of cleft palate, here.
Read More
Cleft Lip/Palate
Is Cleft Lip Genetic?
A cleft lip is a split or separation that occurs between the fourth and seventh week of pregnancy, wherein the developing tissues of the baby's lip don't join completely.
Read More
Cleft Lip/Palate
What Is Velocardiofacial Syndrome?
Velocardial facial syndrome (VCFS) is a disorder that has been associated with over thirty different features. Learn more about Velocardial facial syndrome, here.
Read More
Cleft Lip/Palate
What Is Cleft Lip and Cleft Palate?
A cleft lip is an upper lip that is split, something that affects one out of every 700 babies in the U.S. Find out more about cleft lip and cleft palate, here.
Read More
Cleft Lip/Palate
Why You Could Have A Swollen Soft Palate
A swollen soft palate is not a condition to take lightly. Learn more about what your palate is telling you including symptoms and treatments.
Read More
Cleft Lip/Palate
What Is a Submucous Cleft Palate?
Although most orofacial clefts are identified when the baby is born, a submucous cleft palate may not be diagnosed until later in his or her life. Learn more here.
Read More
Immune Disorders
Autoimmune Disorders 101: How Autoimmune Diseases Can Affect Oral Health
Most body parts can be affected by these diseases, and while treatments exist, there are no cures. Some of these diseases affect the oral cavity and have a negative effect on oral health.
Read More
Immune Disorders
Behcet's Disease: Symptoms, Diagnosis, and Treatment Options
Behcet's disease is a rare autoimmune disease that causes inflammation of blood vessels throughout the body. Learn how it affects the mouth.
Read More
Immune Disorders
Oral Psoriasis: What It Is and How To Treat It
Those who have psoriasis, and experience flareups that affect the mouth or tongue, should consult with a dermatologist or dentist to determine the best way to manage their symptoms.
Read More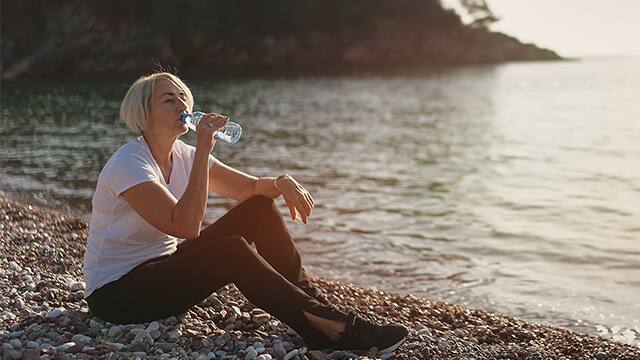
Immune Disorders
Immune Disorders 101
Learn more about how immune and autoimmune disease can affect your teeth, gums, and oral health. Find information on treating oral health conditions related to immune diseases.
Read More
Immune Disorders
What Is Tooth Resorption?
What is tooth resorption and how can your dentist diagnose and treat it? Learn more here.
Read More
Dental Sealants
Are There Dental Sealant Dangers?
Your dentist may recommend a tooth sealant to guard against cavities. What should you know? Are there potential dangers or risks associated? Learn more.
Read More
Dental Sealants
Dental Sealants 101
Dentists and dental hygienists can usually seal teeth in a single visit. Learn more about the steps involved with traditional, resin-based materials.
Read More
Dental Sealants
Is The Cost Of Dental Sealants Worth It?
Knowing more about dental sealant cost prior to the procedure can help you decide whether the treatment is right for you. Learn more about sealant costs.
Read More
Dental Sealants
Pit And Fissure Sealants: Why You Might Need Them
As you know, prevention is better than cure. Pit and fissure sealants are one of several methods for staving off the decay that leads to dental caries.
Read More
Dental Sealants
Sealing Molars: Five Benefits For Your Child
Few kids can maintain healthy teeth without help. Here are five benefits of sealing molars as one of the most cost-effective ways to protect their teeth.
Read More
Dental Sealants
What Is a Glass Ionomer Sealant?
A glass ionomer sealant is one of the latest alternatives to older, resin-based restorations. Its materials and application are a bit different.
Read More
Dental Sealants
Dental Sealants
What are dental sealants? Are they effective? Find out all of the answers to your burning questions on tooth sealants with Colgate. Click here.
Read More
Oral Care: Adults (18+)
How To Find Relief for Abscessed Teeth
You're experiencing some serious pain in your mouth. Are there any home remedies for abscessed teeth that could help you?
Read More
Oral Care: Adults (18+)
5 Pale Tongue Causes
If healthy your tongue should be pink. If your tongue looks lighter than normal it could be due to one of the following 4 pale tongue causes. Learn more.
Read More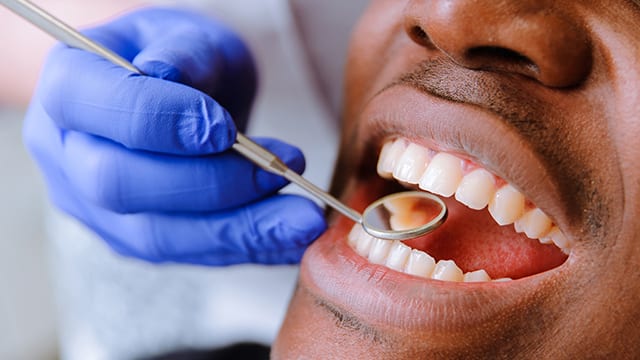
Oral Care: Adults (18+)
4 Professional Teeth Cleaning Tools You Should Know
Dental professionals use a range of teeth cleaning tools to perform expert cleaning & polishing. Learn about 4 teeth cleaning tools, here.
Read More
Oral Care: Adults (18+)
4 Tooth Pain Home Remedies
If you've ever had a toothache, you know tooth pain isn't fun. If you're unable to receive dental attention right away, try some tooth pain home remedies.
Read More
Oral Care: Adults (18+)
Adult Thumb Sucking: How To Break The Habit
While thumb sucking isn't an issue in babies or young children, adult thumb sucking may be embarrassing and in some cases may pose oral health problems.
Read More
Oral Care: Adults (18+)
Alcohol and Teeth: Three Things To Consider Before You Drink
Whether you prefer champagne to wine or mixed drinks to beer, be aware alcohol and teeth aren't natural allies. Here's how you can still enjoy yourself.
Read More
Oral Care: Adults (18+)
Sialolithiasis: What You Need to Know About Salivary Stones
Changes in salivary flow, dehydration and certain medications can all increase your chances of sialolithiasis. Here's what you should know about it.
Read More
Oral Care: Adults (18+)
An Overview Of Tooth Pathology
Dentists are well-versed in tooth pathology. Read more for an overview of congenital and acquired conditions that may affect your teeth.
Read More
Oral Care: Adults (18+)
Birth Control Side Effects and Oral Health
If you're considering starting birth control, you might be surprised that birth control side effects may impact your oral health. Learn more, here.
Read More
Oral Care: Adults (18+)
Blue Or Gray Teeth: Causes And Treatments
Gray or blue teeth may be natural or healthy, or this color may indicate problems needing professional attention. Learn the causes and treatments, here.
Read More
Oral Care: Adults (18+)
Bumps on the Back of the Tongue: Normal or Abnormal?
Bumps on the back of the tongue can occur due to sores and infections among other conditions. Consult your dentist if you notice abnormal bumps.
Read More
Oral Care: Adults (18+)
Burned the Roof of Your Mouth? Here's How To Manage.
Didn't wait long enough for that slice of pizza to cool off? A severely burned roof of mouth can last for hours, even days, as it works to heal itself.
Read More
Oral Care: Adults (18+)
Can a Migraine and Tooth Pain Be Related?
Migraines can come with a variety of symptoms. There can be a link between having a migraine and tooth pain including TMJ, teeth grinding, and toothaches.
Read More
Oral Care: Adults (18+)
Can Tooth Enamel Be Restored?
Can you restore your tooth enamel? Click here for everything you need to know on the subject of tooth enamel restoration with Colgate.
Read More
Oral Care: Adults (18+)
Causes Of Brown Spots On Teeth
Brown spots on teeth may worry you, but there's plenty you can do to fix them. Your dentist can offer a solution based on the following causes.
Read More
Oral Care: Adults (18+)
Chalky Teeth: Causes and How to Deal
Chalk belongs on a blackboard – not on your teeth. Find out if your chalky teeth are caused by food or a serious dental issue. Learn more.
Read More
Oral Care: Adults (18+)
Chattering Teeth: What's Behind It?
Your chattering teeth could just be a sign that you're cold. Though there may be underlying causes that are a little more serious. Learn more here.
Read More
Oral Care: Adults (18+)
Chew on This: Ice Crunching and Your Teeth
While blenders and ice crushers are perfect for crunching ice cubes, teeth are not. Find the perfect alternative to ice crunching here!
Read More
Oral Care: Adults (18+)
Cosmetic Contouring: Four Things You Need To Know
If you're looking into cosmetic contouring to fix your smile, check out the pros and cons and how to tell if it's the right procedure for you. Learn more.
Read More
Oral Care: Adults (18+)
Crooked Teeth? Here's How You Can Boost Your Confidence
Do you have crooked teeth? Here are some tips on how to take care of your teeth and how to correct crooked teeth to boost your confidence!
Read More
Oral Care: Adults (18+)
Dysgeusia: Symptoms, Causes, And Treatment
Dysgeusia is a taste disorder that causes foul, rancid, metallic, or salty taste perception. Learn more, including the causes, symptoms and treatment here.
Read More
Oral Care: Adults (18+)
Dysphagia Treatment That May Ease Swallowing
There are several dysphagia treatment options available depending on the cause and severity of a patient's swallowing disorder. Learn more, here.
Read More
Oral Care: Adults (18+)
Enamel Hypoplasia, Hypomineralization, And Teeth Effects
Enamel hypoplasia (EH), a developmental defect that weakens the surface of your teeth, can affect the primary and permanent teeth in one of two ways.
Read More
Oral Care: Adults (18+)
Everything About Atrophic Glossitis
Abnormal tongue conditions can look alarming. Atrophic glossitis is one of these conditions. Luckily, with a dental professional on your side, they can put your mind at ease and get your tongue back to its normal self.
Read More
Oral Care: Adults (18+)
Excessive Saliva? What It Could Mean (and How to Deal)
Excessive saliva could be a clue about the state of your overall health. Are there ways you can deal with this condition? Find out more, here.
Read More
Oral Care: Adults (18+)
Gum Stimulator: What Is It and How Do I Use It?
What is a gum stimulator and should you add one to your oral hygiene routine? Learn more, here.
Read More
Oral Care: Adults (18+)
How Do I Best Care for My Teeth as an Adult?
The key to keeping a bright, healthy smile throughout adulthood is to practice proper oral hygiene. Even adults can get cavities, as well as gum disease.
Read More
Oral Care: Adults (18+)
How The PH Of Toothpaste Can Affect Your Enamel
Whether it's for whitening or mineralizing, you may not have considered how the pH of toothpaste affects your enamel. Here's what you should keep in mind.
Read More
Oral Care: Adults (18+)
How To Strengthen Weak Enamel
At first glance, your dazzling teeth may seem healthy, but weak enamel can still undermine your oral health without discoloring your smile. Learn more.
Read More
Oral Care: Adults (18+)
Hydrogen Peroxide and Oral Care Benefits
Hydrogen peroxide is a whitening agent, but it can also help kill bacteria that damage your gums. Learn how hydrogen peroxide gums treatment works, here.
Read More
Oral Care: Adults (18+)
Improve Gum Health in Less Than 5 Minutes
You take the time to brush and floss your teeth because you want a brighter smile. But how often do you think about ways to improve gum health? Most...
Read More
Oral Care: Adults (18+)
Is Gum Reshaping Right For You?
Gum reshaping can help you get the beautiful smile you desire, especially if you have a
Read More
Oral Care: Adults (18+)
Is Indemnity Dental Insurance Right For You?
Dental insurance helps you pay for the oral care your family needs. Here's how indemnity dental insurance works and how it differs from other options.
Read More
Oral Care: Adults (18+)
Is Swallowing Your Tongue Possible?
Swallowing your tongue due to a seizure or head trauma is a myth, but other oral injuries can occur if a person falls unconscious. Learn more now.
Read More
Oral Care: Adults (18+)
Lithium Dental Side Effects
Bipolar disorder can often be successfully treated with lithium. However, this treatment does have side effects, including lithium dental side effects.
Read More
Oral Care: Adults (18+)
Median Rhomboid Glossitis: Occurrence, Symptoms, And Treatment
What is median rhomboid glossitis and what populations are most at risk of getting it? Learn more here.
Read More
Oral Care: Adults (18+)
Metallic Taste in Mouth: What Does It Mean?
Should you be concerned about a metallic taste in mouth? Here's what you need to know about the unpleasant taste, how to prevent it and how to treat it.
Read More
Oral Care: Adults (18+)
What Does an Oral and Maxillofacial Surgeon Do?
Learn more about oral care for adults, including how to properly brush and floss, adult toothbrushes, and much more, from the Colgate Oral Care Center.
Read More
Oral Care: Adults (18+)
Root Resorption: Complications, Causes, And Treatment
Root resorption is a natural process, but problems can sometimes arise. Learn what happens and what you can do about it, here.
Read More
Oral Care: Adults (18+)
Busting 7 Myths about Oral Health
Poorly regulated blood sugar makes it hard to curb common issues like gum disease, but it doesn't cause an infection of the gums. Learn more here.
Read More
Oral Care: Adults (18+)
So, You Have Geographic Tongue? No Need To Worry
Geographic tongue is a condition that may look a little strange in your bathroom mirror, but this oral anomaly is generally harmless.
Read More
Oral Care: Adults (18+)
Solving the Calculus Removal Mystery
Calculus removal is important for good oral health. Learn more aboutcalculus removal including calculus types, the calculus removal process, and more.
Read More
Oral Care: Adults (18+)
Ten Causes Of Yellow Teeth And How To Avoid Them
Yellow teeth can cost you your confidence and willingness to smile every day. Here are ten common causes of this undesirable tinge and how to avoid them.
Read More
Oral Care: Adults (18+)
The Dangers of Using a Plaque Scraper at Home
Plaque removal is important for good oral health, but it's not a DIY project. Leave the plaque scraper to your dental hygienist. Learn why, here.
Read More
Oral Care: Adults (18+)
Tongue Bacteria: Know What's Healthy (And What's Not)
Have you ever noticed a white film on your tongue? Here's what to look for when it comes to cleaning your tongue properly to have a good oral care routine.
Read More
Oral Care: Adults (18+)
Tongue Brush Vs. Toothbrush: Which Is Better?
A tongue brush or tongue scraper may provide a more thorough clean than most toothbrushes when it comes to the tongue. Why? Learn more, here.
Read More
Oral Care: Adults (18+)
Tooth Gap Jewelry: Is A Sparkly Smile Safe?
Tooth gap jewelry is a way to dress up your mouth with a removable bit of bling. Learn how to make sure it doesn't affect your oral health or hygiene.
Read More
Oral Care: Adults (18+)
Transient Lingual Papillitis: Location, Symptoms, And Treatment
Inflammation of the tongue's papillae can cause pain and difficulty eating. Learn why transient lingual papillitis happens and how to treat it, here.
Read More
Oral Care: Adults (18+)
Understanding Mouth Inflammation
Learn about the kinds of mouth inflammation and how your dental professional can help prevent and treat mouth sores and redness.
Read More
Oral Care: Adults (18+)
What a Lump on the Jawline Could Indicate
Swellings of the mouth or a lump on the jawline can indicate many different conditions and have many different symptoms. Why wait? Learn more now.
Read More
Oral Care: Adults (18+)
What a Tooth Sensitive To Pressure Means For Mouth Health
It's no fun when teeth can't handle cold temperatures, but when you have a tooth sensitive to pressure, there could be more structural issues at play.
Read More
Oral Care: Adults (18+)
What Are The Signs Of Dead Teeth?
Did you know that teeth can die? Find out more about why this happens, the signs your teeth are dying, and what your treatment options are, here.
Read More
Oral Care: Adults (18+)
What Causes a Gray Tongue?
A healthy tongue should be pink, so noticing that your tongue has turned gray can be distressing. Learn more about the causes and how it can be treated.
Read More
Oral Care: Adults (18+)
What Causes A Swollen Gum Around One Tooth?
It's common to suddenly spot something you didn't notice before. How, for example, could a swollen gum around one tooth form? Here are three explanations.
Read More
Oral Care: Adults (18+)
What Causes Black Gums?
Gum color can vary from one person to another, just like skin color. Some people naturally have black gums, and they aren't necessarily a health issue.
Read More
Oral Care: Adults (18+)
What Is A Dental Therapist?
Learn more about oral care for adults, including how to properly brush and floss, adult toothbrushes, and much more, from the Colgate Oral Care Center.
Read More
Oral Care: Adults (18+)
What Is a Melanotic Macule?
A dark area on the lips could be a melanotic macule, which is noncancerous hyperpigmentation of a mucous membrane. Learn more this common oral condition.
Read More
Oral Care: Adults (18+)
What Is A Meridian Tooth Chart?
A meridian tooth chart is one component of ancient Chinese medicine. Learn if it meets today's standards for dental care.
Read More
Oral Care: Adults (18+)
What Is a Salivary Stone?
Here's all you need to know about salivary stones, including where it's located in the mouth and how dental professionals treat it. Learn more, here.
Read More
Oral Care: Adults (18+)
What Is An Alveoloplasty?
Alveoloplasty is a surgical procedure that reshapes and smooths out the jaw where a tooth has been extracted. Learn more about how and why it is performed.
Read More
Oral Care: Adults (18+)
What Is Dens In Dente?
Dens in dente is a rare dental anomaly. It occurs when the enamel folds into the dentin during tooth development. Learn about causes and treatment options.
Read More
Oral Care: Adults (18+)
What Is a Fissured Tongue?
Fissured tongue refers to abnormal grooves on the surface of the tongue. Here's what you need to know if you notice any fissures on your tongue.
Read More
Oral Care: Adults (18+)
What Is Hyperparathyroidism?
Hyperparathyroidism is the condition that results when the parathyroid glands responsible for regulating calcium in the blood can't maintain the balance.
Read More
Oral Care: Adults (18+)
Enamel Hypocalcification: Definition, Causes, and Treatment
Hypocalcification, a disorder that affects tooth enamel, can threaten your oral health. Learn more about the condition and how to care for your mouth.
Read More
Oral Care: Adults (18+)
What Is Ozone Dentistry And How Does It Work?
The ozone molecule that makes up our atmosphere actually has uses in dentistry, as well. Here's how ozone dentistry works to help improve oral care.
Read More
Oral Care: Adults (18+)
What Is Referred Tooth Pain?
Sometimes a toothache isn't all it seems. Pain that feels as though it's coming from a tooth may be referred tooth pain. Learn more about it, here.
Read More
Oral Care: Adults (18+)
What Is The Difference Between Stomatology and Oral Medicine?
What is stomatology and why might a patient be referred to this specialist? Learn more here.
Read More
Oral Care: Adults (18+)
What Is Trigeminal Neuralgia?
Some people notice the symptoms of trigeminal neuralgia when brushing their teeth and may mistake it for a dental problem. Learn more about the disorder.
Read More
Oral Care: Adults (18+)
What It Means If Your Teeth Feel Rough
Do your teeth feel rough? Learn about possible teeth enamel causes and prevention including brushing your teeth twice per day and flossing once per day.
Read More
Oral Care: Adults (18+)
What To Expect From Tonsil Removal
Even though tonsils are an important part of the body, sometimes a doctor will recommend tonsil removal, a procedure called a tonsillectomy.
Read More
Oral Care: Adults (18+)
When Ear and Jaw Pain Indicates TMD
Facial pain can have non-dental causes, but ear and jaw pain especially in the area of the joint just below it is often a sign of TMJ. Find out more, here.
Read More
Oral Care: Adults (18+)
When to Receive Gum Abscess Treatment
The vast majority of periodontal diseases are painless and rarely require urgent dental attention. Gum abscess treatment is a common exception.
Read More
Oral Care: Adults (18+)
Which Dental Prosthesis Is Right For You?
A dental prosthesis is an implant, bridge, crown, veneer or denture made to replace missing teeth or improve the appearance of damaged teeth.
Read More
Oral Care: Adults (18+)
Why Sinus Infection Tooth Pain Occurs
Sinus infection tooth pain just adds to your problems when you're sick. You'll want to know why it's occuring and how to alleviate it. Learn more, here.
Read More
Oral Care: Adults (18+)
Yellow Tongue: Symptoms, Causes, And Treatments
What does a yellow tongue signal? Read more for common symptoms, causes and treatment options for yellow tongue.
Read More
Oral Care: Adults (18+)
Rinsing and Brushing with Salt: Three Factors to Consider in Your Oral Care
Whether you are moving to a natural lifestyle, DIY-ing your own bath bomb, or looking for the latest life hack for a beautiful smile—you have likely heard about utilizing salt from your cupboard. Touted first for its proficiency in flavoring and preserving food, the application of salt has made its way from the kitchen to the bathroom and everywhere in between.
Read More
Oral Care: Adults (18+)
Hydrogen Peroxide Gums and Teeth Treatment
Dental sealants are protective coatings applied to the chewing surfaces of a child's molars, and they may contain bisphenol A (BPA). Here's what to know.
Read More
Oral Care: Adults (18+)
What Is Good Oral Hygiene?
Your dentist or hygienist can help you learn good oral hygiene techniques and can help point out areas of your mouth that may require extra attention during brushing and flossing.
Read More
Oral Care: Adults (18+)
Colloidal Silver for a Tooth Infection: Does It Work?
Although you may be tempted to treat your tooth pain at home, using colloidal silver for a tooth infection will not solve the issue. Here's what to know.
Read More
Oral Care: Adults (18+)
How to Strengthen Teeth: 5 Tips for Preventing Enamel Erosion
Enamel erosion is permanent and can cause a host of dental issues, but it can be prevented. Here are five tips on how to strengthen teeth.
Read More
Oral Care: Adults (18+)
Is It Bad to Be a Mouth Breather?
Most people naturally breathe through their nose. But if you're a mouth breather, it's worth reviewing the causes, effects and treatments for this issue.
Read More
Oral Care: Adults (18+)
Odynophagia: Conditions That May Lead to Painful Swallowing
If you have pain when swallowing, it may be due to an underlying condition. Here are some conditions that can lead to odynophagia.
Read More
Oral Care: Adults (18+)
Periodontal Disease and Pregnancy: What's the Connection?
There is a link between periodontal disease and pregnancy. Here's what expecting mothers should know to maintain optimal oral health.
Read More
Oral Care: Adults (18+)
Pinhole Gum Surgery: Treatment for Gum Recession
Pinhole gum surgery is a treatment option that can help to treat a receding gumline. Find out how it works, as well as its advantages and disadvantages.
Read More
Oral Care: Adults (18+)
What Causes Sour Tongue and How to Prevent It
Have you ever had a sour tongue or experience a metallic or bitter taste in your mouth? Find out the possible causes and preventing it from happening, here.
Read More
Oral Care: Adults (18+)
The Risks and Benefits of Kissing on Oral Health
These benefits of kissing on your oral health may come as a pleasant surprise. Learn more about both the benefits and risks of sharing a kiss.
Read More
Oral Care: Adults (18+)
Toothpaste on Burns: Does This Home Remedy Work?
Is putting toothpaste on burns ever a good idea? Here's why you might want to rethink a popular home remedy and burn treatment and learn more.
Read More
Oral Care: Adults (18+)
What Causes Tooth Erosion?
Tooth erosion is a common dental concern. Knowing how to prevent tooth wear and tooth erosion can help your teeth stay strong and healthy.
Read More
Oral Care: Adults (18+)
What Is Menstruation Gingivitis? How Women's Periods Affect Gum Health
If you've ever noticed that your gums bleed or get swollen around the time of your period, you may have experienced menstruation gingivitis. Learn more.
Read More
Oral Care: Adults (18+)
What's The Best Tea For A Sore Throat?
Drinking hot tea is a natural remedy that may help ease sore throat symptoms. Here's a look at the best tea that could provide relief and comfort.
Read More
Oral Care: Adults (18+)
Are Artificial Sweeteners Bad for You and Your Teeth?
There is a lot controversies and debates about artificial sweeteners. Find out the pros and cons of these sugar substitutes to make an informed choice.
Read More
Oral Care: Adults (18+)
Cheek Biting: What You Need To Know
There are a few reasons why people bite their cheeks and other areas inside the mouth, including the tongue and inside of the lips. Learn more about cheek biting here and how to stop it.
Read More
Oral Care: Adults (18+)
What Is Oil Pulling? What You Need To Know
Oiling pulling has become a popular trend as a natural home remedy to whitening teeth and improve your dental health. Read on more to find out what oil pulling is and how it works.
Read More
Oral Care: Adults (18+)
Benefits of Mint on Your Teeth
If you're looking for a new way to treat and strengthen your teeth, read up on the benefits of mint and how it can improve your oral health.
Read More
Oral Care: Adults (18+)
Alcoholic Drinks to Avoid this Summer to Protect Your Teeth
Whether you prefer wine or beer, you should be aware that alcohol and teeth aren't natural allies. Here's how you can still enjoy alcohol.
Read More
Oral Care: Adults (18+)
What You Need to Know About Vegan Oral Care
Vegan Oral Care, what is it? Looking to adapt to a plant-based lifestyle and vegan oral care can be part of that change. For more information visit colgate.com
Read More
Oral Care: Adults (18+)
How to Achieve a Healthy Mind, Body & Mouth
Oral health is much more than just healthy teeth, it also includes the health of the gums, bones, and nerves. Learn about the benefit of oral care here.
Read More
Oral Care: Adults (18+)
How To Find Dental Insurance That Covers Braces For Adults
Orthodontia is pricey, and finding dental insurance that covers braces for adults can be challenging. Nonetheless, there are ways to afford your treatment.
Read More
Oral Care: Adults (18+)
How to Maintain Good Dental Care While Traveling
Maintaining proper dental care while traveling can be difficult. Learn how to keep your teeth clean on the road with Colgate. Click here now.
Read More
Oral Care: Adults (18+)
What is Oral Allergy Syndrome (OAS)?
What is oral allergy syndrome? Learn about OAS including the signs, symptoms & more with Colgate®. Click here for the full article.
Read More
Oral Care: Adults (18+)
What is Mewing?
A well-defined jawline and improved alignment of the chin and nose by mewing? Click here to learn more about Mewing with Colgate.
Read More
Oral Care: Adults (18+)
How Daily Habits Affect Your Smile’s Brightness
Discover why teeth stain and how to prevent discoloration with expert advice from dental professionals. Learn about the roles of diet, hygiene, and whitening technology.
Read More
Oral Care: Adults (18+)
Common Causes of Dry Mouth
By: Ann Eshenaur Spolarich, RDH, PhD, FSCDH
Read More
Oral Cancers
Dental Oncology 101: The Oral Health Experts On Your Cancer Treatment Team
Cancer and its treatments can also affect the mouth, which is why some dentists are specially trained as dental oncologists to help care for patients undergoing cancer treatment.
Read More
Oral Cancers
Tongue Cancer: Symptoms, Detection & Treatment
With respect to speaking and eating, it's crucial to know which tongue cancer symptoms to look for so your oral health doesn't threaten these functions.
Read More
Oral Cancers
Four Symptoms of Jaw Cancer
Oral cancer is deceptively common. If you experience any of the following jaw cancer symptoms, be sure to seek an evaluation by your dentist.
Read More
Oral Cancers
Gardner Syndrome Teeth: How Your Dentist Can Help
Gardner syndrome isn't a cancer, but a familial adenomatous polyposis (FAP). These conditions cause cancer through the growth of hundreds to thousands of benign polyps in the colon and rectum.
Read More
Oral Cancers
Gum Cancer Or Gingivitis? How To Tell The Difference
Although gum disease is a much more common oral condition, gum cancer is also a legitimate possibility, and can be easily confused with gingivitis.
Read More
Oral Cancers
Head And Neck Radiation Treatment & Your Mouth
Doctors use head and neck radiation to treat cancer because it kills cancer cells. But radiation to the head and neck can harm normal cells, including cells in the mouth.
Read More
Oral Cancers
How A Parotid Tumor Affects Oral Health
The parotid is the most common mouth gland for cancer to develop in. Here's what you need to know if you're diagnosed with a parotid tumor.
Read More
Oral Cancers
How Oropharyngeal Cancer Is Identified And Treated
Oropharyngeal cancer affects the tissues in the back of your mouth – the tonsils, soft palate and pharynx – and there are several signs and risk factors.
Read More
Oral Cancers
Hypercalcemia Teeth: What It Is & Treatment Options
Hypercalcemia teeth isn't a condition by itself, but many systemic issues like hypercalcemia, cancer and osteoporosis can have an effect on your teeth.
Read More
Oral Cancers
Is Erythroplakia a Red Flag for Oral Cancer?
Erythroplakia is a red lesion that could be an indicator of oral cancer. If you notice one in your mouth, it's best to have a dentist check it out.
Read More
Oral Cancers
Magic Mouthwash: A Solution for Mouth Sores?
Magic mouthwash is a treatment that may alleviate mouth sores caused by chemotherapy & reduce the effects of oral mucositis. Find out more about it, here.
Read More
Oral Cancers
Mucositis Treatment Options and Oral Care
Inflamed mouth tissues is a common side effect of chemotherapy, but there are some mucositis treatment options that may relieve your mouth pain.
Read More
Oral Cancers
Oral Cancer and Esophageal Cancer
Oral cancer and esophageal cancer have something in common: The majority of these types of cancer are diagnosed late and have high death rates.
Read More
Oral Cancers
Oral Cancer Screening – What To Expect
An oral cancer screening is a visual and physical exam of one's oral cavity and connected tissues, and takes place before the following symptoms even show.
Read More
Oral Cancers
Oral Cancer Signs And Symptoms
Learn more about the various signs and symptoms of oral cancer, how to prevent it, and how oral cancer is treated with Colgate®. Click here.
Read More
Oral Cancers
Oral Cancer Surgery: How to Prep for Your Procedure
Check out these tips and questions you should ask your doctor to prepare you for your oral cancer surgery. Learn more about pre-op, and post-op procedures.
Read More
Oral Cancers
Oral Cancer Survival Rate
Although an oral cancer prognosis used to be bleak, the oral cancer survival rate is now improving due to a number of factors. Learn more, here.
Read More
Oral Cancers
Oral HPV and Oropharyngeal Cancer
Learn more about the connection between specific types of the human papilloma virus (HPV) & oropharyngeal cancer, including signs, symptoms, and treatment.
Read More
Oral Cancers
Palate Cancer: Signs, Symptoms And Risk Factors
How is cancer of the hard and soft palate different from other oral cancers? Learn more about palate cancer here, including the signs, symptoms, and risks.
Read More
Oral Cancers
What is Palliative Dental Care?
Palliative care aims to help patients with serious illnesses feel more comfortable. Dental treatment often plays an important role in this type of care.
Read More
Oral Cancers
Radiation Side-Effects and Your Oral Health
Some radiation side-effects can cause your treatment to delay or stop altogether. Here's what to watch for and what you can do to prevent them.
Read More
Oral Cancers
Three Good Reasons To See A Dentist (Before Cancer Treatment)
Your cancer treatment may be easier if you work with your dentist and hygienist. Make sure you have a pretreatment dental checkup.
Read More
Oral Cancers
How Lymphoma Can Affect Your Oral Health
Lymphomas are cancers that affect the lymphatic system, an important part of the body's immune system and blood network. Learn more today.
Read More
Oral Cancers
What Is Verrucous Carcinoma?
Verrucous carcinoma may occur in various regions of the head and neck. The oral cavity is the most common site for this type of tumor. Learn more, here.
Read More
Oral Cancers
What to Expect from a Tongue Biopsy
Learn about what you can expect from a tongue biopsy, including how it's performed and the after-care.
Read More
Oral Cancers
Lymphomas: What Your Dental Visit Can Reveal
Routine physicals can discover lymphomas, but sometimes an ordinary dental checkup can be critical in revealing signs before other symptoms present.
Read More
Oral Cancers
Early Signs of Mouth Cancer
Learn more about the signs, symptoms, and treatment of oral cancer. Other types of cancer can also have an affect on your oral health. Learn more here.
Read More
Oral Cancers
What is Lip Cancer? Causes, Signs and Symptoms
Lip cancer doesn't get as much attention as other types of oral cancer, but it's not an uncommon condition. See the warning signs of lip cancer, here.
Read More
Oral Cancers
How Chemotherapy Can Affect Your Teeth and Mouth
While chemotherapy helps treat cancer, it can also cause other chemotherapy side effects in your mouth. Learn more here.
Read More
Oral Cancers
Cancer From Dip: The Facts About Smokeless Tobacco
If you're concerned about the risk of cancer from dip, or smokeless tobacco, read on to learn about its potential consequences. Why wait? Learn more today.
Read More
Implants
Are Same Day Dental Implants Right For You?
Implant placement is typically a multistep process that can take several months, but same day dental implants might be a viable alternative. Here's how.
Read More.jpeg)
Implants
Bone Augmentation And Nerve Repositioning
Patients with insufficient bone to support implants could be candidates for bone augmentation, which is the process of rebuilding the bone. Learn more.
Read More
Implants
Understanding Bone Grafts for Dental Implants
In a bone graft procedure, the surgeon will take a section of bone from another area of your body, or - as is most often the case now - use a special bone grafting material, and graft it onto your jaw bone.
Read More
Implants
Bridge Or Implant: Which Is Best For You?
A dental bridge or implant are two options your dentist can provide to replace a missing tooth, and each option has different advantages.
Read More
Implants
Common Dental Implant Problems and How to Treat Them
The vast majority of implants are successful, but occasionally, dental implant problems occur. Fortunately, they can almost always be treated by a dentist.
Read More
Implants
Dental Implant Surgery
Dental implants are artificial teeth that are implanted into the mouth and jaw, often used when adults lose adult teeth. Learn more about cost, recovery and more.
Read More
Implants
Dental Implants: A Permanent Tooth Replacement to Consider
Dental implants are a comfortable and aesthetically pleasing permanent option for those who have lost a tooth
Read More
Implants
Dental Implants And MRI Procedures
Dental implants and MRI procedures: If you have the former, can you undergo the latter? Learn more.
Read More
Implants
Dental Implants Cost Explained
Learn more about dentures, including dental implant procedures, and much more, from the Colgate Oral Care Center.
Read More
Implants
Do I Need Dental Implants?
If you have lost teeth, there are many options to fix your smile. Are jaw implants the right treatment for you? Find out more about jaw implants, here.
Read More.jpeg)
Implants
Endosteal Implant: What You Need To Know
The endosteal implant is one type of dental implant to replace a missing tooth. Find out more about endosteal implant components, placement, and aftercare.
Read More
Implants
How Does an Implantologist Differ from a General Dentist?
A general dentist can be your mouth's best friend. But if you need implants, your dentist may ask you to seek out the services of an implantologist.
Read More
Implants
How To Find Dental Insurance That Covers Implants
When it comes to replacing missing teeth, dental implants are effective — but they can be costly. Here's how to find dental insurance that covers implants.
Read More
Implants
How To Keep Your Abutment Tooth Healthy
After getting a dental implant, it's important to care for your abutment tooth properly to ensure long-term success and optimal oral health. Here's how.
Read More


Implants
Implants 101
Learn more about dentures, including dental implant procedures, and much more, from the Colgate Oral Care Center.
Read More.jpeg)
Implants
Jaw Implants Provide Patients A Reason To Smile
To replace a missing tooth or retire a set of dentures, jaw implants can improve your smile and overall oral health. Learn more about jaw implants, here.
Read MoreImplants
Peri-Implantitis and Protecting Your Dental Implants
Peri-implantitis is an infection that develops around a dental implant. Knowing how to care for your implant can help you save your smile.
Read More
Implants
Signs of a Failed Dental Implant
A failed dental implant is an unusual situation, but if it happens to you there's no need to panic. Read on to learn how to recognize an implant problem.
Read More
Implants
Titanium Rejection Symptoms: Are You Allergic to Your Dental Implant?
Dental implants are generally safe but can, occasionally, cause issues. Here are the titanium rejection symptoms to look for and discuss with your dentist.
Read More
Implants
What Are Mini Dental Implants?
Mini dental implants are an option for patients looking to replace lost teeth but who don't want (or can't receive) conventional restorations.
Read More.jpeg)
Implants
What Is A Subperiosteal Implant?
If you need a dental implant but are suffering from bone loss in your jaw, you may be a candidate for a subperiosteal implant. Learn more here.
Read More
Implants
What Is an Allograft Procedure?
An allograft is a type of bone graft typically used to enhance an area of the mouth in preparation for dental implant placement. Learn more here.
Read MoreImplants
What Occurs During Implant Surgery
This video includes the extraction of a molar, and the restoration with an implant.
Read More
Implants
Your Comprehensive Guide to Dental Implant-Supported Bridges
When you are missing several teeth in a row, a dental implant-supported bridge may be the best option to restore your smile. Find out what an implant bridge is as well as what's in store if you choose this tooth replacement solution.
Read More
Implants
Sinus Lift Surgery: Answering Common Questions
Sinus lift, or sinus augmentation surgery, adds bone to your upper jaw to make it taller. Sinus lift surgery is typically performed when there is not enough bone in the upper jaw, or the sinuses are too close to the jaw, to receive dental implants.
Read More
Implants
Single-Tooth Implants: What To Expect
Single-tooth dental implants can be a great solution for people missing one or more teeth — helping to improve chewing, talking and, of course, smiling!
Read More
Implants
What is a Dental Implant?
Dental implants are metal posts or frames that are surgically positioned into the jawbone beneath your gums. Once in place, they allow your dentist to mount replacement teeth onto them.
Read More
Implants
Restorative Dentistry: Single Tooth Loss. What Is An Implant?
Learn more about dentures, including dental implant procedures, and much more, from the Colgate Oral Care Center.
Read More
Implants
3 Titanium Implant Side Effects and How to Minimize Your Risk
As with any surgical procedure, getting dental implants can pose risks. Here's a look at some rare titanium implant side effects and how to treat them.
Read More
Implants
Is Your Dental Implant Pain Normal?
After dental implant surgery, it's normal to have some postoperative pain. However, in some cases, it can be a sign of something more serious. Learn more.
Read More
Implants
Zirconia vs. Titanium Implants: Which One Is Right for You?
Choosing between zirconia and titanium implants can be tricky. Here are some pros and cons to consider when discussing your options with your dentist.
Read More
Pregnancy Oral Care
Oral Health During Pregnancy
To avoid a toothache during pregnancy, or any other dental problem when expecting a baby, your best strategy starts with a dental visit.
Read More
Pregnancy Oral Care
Bleeding Gums During Pregnancy: Should You Worry?
Chances are good that, during your pregnancy, you will experience a myriad of symptoms you have never had before. Bleeding gums is one such condition.
Read More
Pregnancy Oral Care
4 Things To Know About Oral Health & Pregnancy
What are the top 4 things you should know about oral health & pregnancy? Click here to find out with this article on oral health and pregnancy with Colgate.
Read More
Pregnancy Oral Care
Is A Tooth Extraction During Pregnancy Safe?
Can you safely undergo a tooth extraction during pregnancy? The answer, as far as medical professionals are concerned, is yes. Learn more, here.
Read More.png)
Pregnancy Oral Care
Maintaining Healthy Teeth And Gums While Pregnant
After you conceive, your hormones, especially progesterone, start increasing and changing. But hormones don't affect only the growth of your little one.
Read More
Pregnancy Oral Care
Relief For Dry Mouth During Pregnancy
What can you do about dry mouth during pregnancy? While dry mouth may not be as talked about as other common pregnancy symptoms, that dry, sticky...
Read More
Pregnancy Oral Care
Sensitive Teeth During Pregnancy: What To Expect and How To Cope
Your body changes during pregnancy, and teeth are no exception. Sensitive teeth during pregnancy is completely normal, but you can reduce the irritation.
Read More
Pregnancy Oral Care
Swollen Gums During Pregnancy
Learn more about caring for swollen gums during pregnancy and the necessary questions to ask your dentist.
Read More
Pregnancy Oral Care
Teeth Cleaning While Pregnant
So while moms-to-be have plenty on their minds, they shouldn't forget about teeth cleaning while pregnant. Find out more about pregnancy & oral care.
Read More
Pregnancy Oral Care
Teeth Whitening When Pregnant: Is It Safe?
Everyone wants a whiter, brighter smile, but teeth whitening when pregnant may not be the best idea for an expectant mother. Learn why here!
Read More
Pregnancy Oral Care
The Effects Of Sugar During Pregnancy On Your Baby, Your Body And Your Mouth
Does eating sugar during pregnancy have a lasting effect on your health or the health of your child? Here's what expecting mothers should know.
Read More
Pregnancy Oral Care
What Is A Pregnancy Tumor? Maintaining Oral Health During Pregnancy
Pregnancy hormones can affect a woman's body in many ways, but one lesser-known oral complication is a pregnancy tumor. Here's what you need to know.
Read More
Pregnancy Oral Care
What Red Gum Color Can Mean for Women
Women are likely to notice a red gum color and other symptoms of gum disease at certain times in their lives. Find out more about what red gums can mean.
Read More
Pregnancy Oral Care
The Facts On Canker Sores And Pregnancy
Be on the lookout for these signs if you experience canker sores and pregnancy. Find out more about what they mean and how to prevent them, here.
Read More
Pregnancy Oral Care
7 Healthy Foods to Eat When Pregnant
Eating a healthy, well-balanced diet is always a good idea, but it's even more important when you're pregnant. Here are seven healthy foods to consider.
Read More
Pregnancy Oral Care
7 Ideas For Healthy Pregnancy Lunches
With unexpected cravings and bouts of nausea, pregnancy can be a tough time for healthy eating. Here are some ideas for healthy pregnancy lunches.
Read More
Pregnancy Oral Care
What Is Asymmetric Crying Facies?
Asymmetric crying facies (ACF) is a rare congenital anomaly occurring to newborn babies. Find out more about the causes, symptoms, and treatment.
Read More
Pregnancy Oral Care
Can You Take Antibiotics During Pregnancy?
If pregnant, you're likely watching your health, but do you know if you can take antibiotics during pregnancy? Learn more about antibiotics and pregnancy.
Read More
Pregnancy Oral Care
Healthy Breakfast For Pregnancy: 5 Ideas To Kick-Start Your Day
Healthy, nutritious eating is essential when you're pregnant. Try these five meals to kick-start your day with a healthy breakfast for pregnancy.
Read More
Root Canals
Antibiotic Prophylaxis Before Dental Work
Before you undergo dental treatment, your dentist or medical provider may recommend antibiotic prophylaxis. Learn what it is and how it works.
Read More
Root Canals
Root Canal Pain: What to Expect
While severe pain after root canal isn't common, it is common to experience a bit of discomfort in the treated area. Learn what to do for root canal pain and when to contact a doctor here.
Read More
Root Canals
Can Root Canal Infections Spread?
Has your dentist told you that you need a root canal? If you're worried about the procedure and wondering if root canal infections spread, read on.
Read More
Root Canals
Dead Nerve In A Tooth: Causes And Treatment
If your dentist has found a dead nerve in a tooth, don't panic: Your tooth can be saved, even when it is no longer vital. Why wait? Learn more today.
Read More
Root Canals
Do Root Canals Cause Health Problems?
Do root canals cause health problems? Here's your answer to this and other concerns you might have about your upcoming procedure.
Read More
Root Canals
Explaining The Root Canal Causes Cancer Myth
Have you heard that root canals cause cancer? It's a common myth; completely false. Learn more about where this myth comes from and actual complications.
Read More
Root Canals
Ferrule Effect: What Is It?
Teeth or crowns may flex or move. This movement can lead to fracture. The ferrule effect helps reduce the risk of the tooth fracturing, though it doesn't guarantee it.
Read More
Root Canals
Gutta Percha: What Is It And When Is It Used
What is Gutta Percha? If you polled folks to name the first dental procedures that come to mind, they might say fillings, crowns and root canals.
Read More
Root Canals
Here's What To Eat After A Root Canal
The healing period after a root canal procedure isn't what most would describe as fun, but it's critical to follow your dentist's aftercare instructions to protect your sensitive, restored tooth.
Read More
Root Canals
What Is Pulp Capping?
What is pulp capping and why may your dentist recommend a cap for you or your child? Learn more, here.
Read More
Root Canals
Pulpotomy In Adults
A pulpotomy is a procedure a dentist may use to preserve your tooth when portions of a tooth's pulp is injured. Learn more, here.
Read More
Root Canals
Relieving Root Canal Infection Symptoms
Root canal infection symptoms should not be ignored because they may indicate your tooth needs further treatment. Find out morea about them, here.
Read More
Root Canals
Root Canal Complications: What You Need To Know
When you think about a root canal, you likely envision a painful dental treatment that requires a fair bit of recovery. A root canal is normally done...
Read More
Root Canals
Root Canal Vs. Extraction: Which Is Right For You?
Choosing between root canal vs. tooth extraction can prove to be a difficult decision, learning more about both methods can help you choose.
Read More
Root Canals
Root Canals And Breast Cancer: Debunking Common Root Canal Myths
Is there a connection between root canals and breast cancer? Here's your answer to this myth, as well as other root canal concerns.
Read More
Root Canals
Should You Remove a Tooth that has had Root Canal Treatment?
If you've had a root canal and the tooth is bothering you again, you might be wondering when it's time to remove a root canal tooth. Here's what to know.
Read More
Root Canals
What Alternatives To Root Canals Should You Consider?
Popular theories abound about alternatives to root canals, but beware: not all of them are effective. Find out more about root canal alternatives, here.
Read More
Root Canals
What Is Condensing Osteitis?
Condensing osteitis is a condition that results in increased bone density at the base of a tooth's root. It can be treated by your dentist or a specialist.
Read More
Root Canals
What Root Canals Cost And Why The Cost Varies
Ever wonder what a root canal cost? Find out what a root canal costs and what factors may cause the price to vary, here.
Read More
Root Canals
When Is A Root Canal Without Crown Protection Wise?
Weighing the pros and cons can help you decide if a root canal without crown placement is the best and most cost-effective option for you.
Read More
Root Canals
What Is Endodontic Retreatment and When Is It Needed?
Pain and discomfort at the site of an old root canal may mean you need endodontic retreatment. Learn more about what the procedure entails.
Read More
Root Canals
Why Old Root Canal Infection Symptoms Return And What To Do Next
Root canal treatment is typically very successful. However, old root canal infection symptoms may sometimes return. Here's how your dentist will help.
Read More
Root Canals
What is an Endodontist? Facts About This Tooth-Saving Specialist
The American Association of Endodontists (AAE) sums up the profession neatly, stating that endodontists are the tooth-saving specialists of dentistry. Learn more about how they can help you here!
Read More
Root Canals
What Is A Root Canal? A Step-By-Step Guide
Usually, root canals are recommended or needed when there is an infection deep within the tooth. Check out our illustrative guide to root canals here!
Read More
Root Canals
Do I Need a Root Canal? A Step By Step Guide to Ease Your Worries
Do I need a root canal? Click here to find out & read our step-by-step guide on what you can expect before, during, and after the procedure with Colgate.
Read More
Root Canals
Apicoectomy and Apicoectomy Healing
An apicoectomy, also known as root end surgery, is a surgical procedure where a tooth's root is removed and a root end cavity is filled. Learn more about this and the healing time here.
Read More
Root Canals
Root Canals 101
Do I need a root canal? Click here to find out & read our step-by-step guide on what you can expect before, during, and after the procedure with Colgate.
Read More
Root Canals
Endodontics 101
If the roots of your teeth are causing you pain, you may be referred to an endodontist. Check out more about the endodontics field, here.
Read More
Root Canals
What Is Root Canal Treatment?
A root canal can save a tooth that would have otherwise been lost due to damage or disease. Find information on what a root canal is, and learn the steps used in root canal treatment at Colgate.com.
Read More
Root Canals
Do You Need Antibiotics Before A Root Canal Treatment?
If you have severe tooth pain, it's possible that you need a root canal. Learn why your dentist may recommend antibiotics before a root canal treatment.
Read More
Root Canals
Pulpotomy Vs. Pulpectomy: Which Procedure Will Heal Your Tooth?
What's the difference between a pulpotomy vs. pulpectomy, and which treatment will heal your tooth? Learn more and discuss with your dentist.
Read More
Root Canals
Severe Dental Pain: How Do Dentists Remove A Tooth Nerve?
Many people will experience a toothache at some point. When severe dental pain strikes, your dentist may remove a tooth nerve. Here's how.
Read More
Root Canals
The Truth About Root Canal Dangers
The fear of false root canal dangers should not deter you from having this tooth-saving treatment. Here's what to know before your procedure.
Read More
Root Canals
What Is A Calcified Tooth? Causes And Treatment Options
A calcified tooth can develop after dental trauma, such as from a sports injury. Here's what to know about this dental condition.
Read More
Root Canals
Myths About Root Canal Treatment
A root canal treatment can be scary to some people who are not familiar with the procedure. Learning the truth about these root canal myths and misconceptions can help you get a better understanding of what a root canal really is and for.
Read More
X-Rays
Is the Cost of Dental X-Rays Worth It in the Long Run?
If you're on a tight budget you may worry if the cost of dental X-rays is worth it, even if your dentist does recommend it. Find out more about costs here.
Read More
X-Rays
The Importance of Dental X-Rays or Radiographs
Thanks to dental x-rays dentists can accurately diagnose and treat dental problems before they become more serious. Learn more here.
Read More
X-Rays
What Is a Cephalometric X-Ray?
A cephalometric X-ray is one type of X-ray that is used for both diagnostic and treatment planning in dentistry and medicine. Here's what you should know.
Read More
X-Rays
What Is A Panoramic Dental X-Ray?
Unlike A traditional radiograph, a panoramic dental x-ray creates a single image of the entire mouth including upper and lower jaws, TMJ joints, teeth, and more.
Read More
X-Rays
X-Rays 101
X-rays, also known as radiographs, are an essential part of any dental care treatment plan. Learn more about the benefits of X-rays at Colgate® Oral Care.
Read More
X-Rays
X-Rays for Children
Children's mouths should be x-rays in accordance with your child's development and dental health. Find out more about dental x-rays for children, here.
Read More
X-Rays
Types of X-rays
X-Rays are divided into two main categories, intraoral and extraoral. Find out more about intraoral and extraoral radiographs, here.
Read More
X-Rays
Oral And Maxillofacial Radiology: The Dental Specialty Dedicated To X-Rays
X-rays are an important part of your dental visit, and there's a whole specialty dedicated to them called oral and maxillofacial radiology. Here's more.
Read More
Plaque & Tartar
5 Effective Methods to Remove Biofilm
Biofilm removal is essential to a healthy mouth. Biofilms are slimy layers of bacteria that can lead to oral health problems if not removed. Learn more.
Read More
Plaque & Tartar
Black Tartar On Teeth
Black tartar on teeth forms below the gum line and causes many dental issues. Though it isn't difficult to treat, only dentists can remove it.
Read More
Plaque & Tartar
Can You Dissolve Tartar?
Explore if you can dissolve tartar and what your dental hygienist thinks. Get expert advice and oral care tips for a healthier smile. Read more on Colgate.
Read More
Plaque & Tartar
Dental Plaque Germs: What You Need to Know
Learn about dental plaque germs, their impact on oral health, and effective prevention strategies. Colgate provides essential insights for a healthier smile.
Read More

Plaque & Tartar
Is Flossing Necessary?
Maintaining proper oral hygiene requires the cultivation of several good oral care habits which, when performed together… Read more at Colgate.com
Read More
Plaque & Tartar
How Bacterial Plaque Causes Gum Disease and Tooth Decay
When bacteria overstay their welcome in your mouth, numerous dental problems can set in. Bacterial plaque causes gum disease in the following ways.
Read More
Plaque & Tartar
Calcium Deposits on Teeth: Treatment and Prevention
Calcium buildup on teeth can often be prevented by regular brushing, but you'll need the help of your dentist to remove it if it decides to stick around.
Read More
Plaque & Tartar
Plaque: What Is It and How do I Get Rid of It?
By following easy steps for keeping your teeth and gums healthy – plus seeing your dentist regularly — you can have your teeth for a lifetime!
Read More
Plaque & Tartar
Are Probiotics Good For Oral Health?
Probiotics for oral health are an effective, natural and economic means of fighting gum disease, plaque and bad breath. Here's how these microbes help you.
Read More

Plaque & Tartar
The Role Of The Dental Pick For Plaque Removal
Is a dental pick the right tool for you to remove plaque? Find out more about how a dental plaque can help you fight plaque.
Read More
Plaque & Tartar
What Disclosing Tablets Can Tell You About Plaque
Plaque disclosing tablets can help you see where the plaque is plaguing your teeth and help you do your best to get rid of it. Find out more about them.
Read More

Plaque & Tartar
What Is Tartar?
Do you think you might have tartar? But first, what is tartar? Learn more about how to prevent, and how to remove tartar at Colgate® Oral Care.
Read More
Plaque & Tartar
What Is Veillonella?
Veillonella is in the family of oral flora responsible for periodontal (gum) disease and tooth decay that affects so many people. Learn more, here.
Read More
Plaque & Tartar
What is a Mouth Debridement?
Full mouth debridement involves the extensive removal of plaque and calculus from teeth. Click here to learn more about full debridement with Colgate.
Read More
Plaque & Tartar
Plaque On Teeth – Causes And Treatment
When left alone, plaque on teeth turns to tartar and can increase your risk for cavities or gum disease. And as scary as it sounds, it happens to everyone.
Read More
Plaque & Tartar
Biofilm Formation: How To Protect Your Mouth From Harmful Bacteria
Your mouth is home to many species of bacteria, both good and bad. Learn about the stages of biofilm formation and how to protect your mouth.
Read More
Plaque & Tartar
How Subgingival Calculus Forms And How To Prevent It
You might know about dental plaque, but what about subgingival calculus? Here's how this substance impacts your dental health.
Read More
Plaque & Tartar
What Is Supragingival Calculus?
You've probably heard your dentist talk about plaque, but what about supragingival calculus? Here's what to know about this dental health concern.
Read More
Plaque & Tartar
The Impact of Streptococci on Oral Health
Discover how bacteria like streptococci can contribute to plaque development and sometimes lead to bacterial infections affecting your well-being.
Read More
HIV/AIDs & STDs
Dental Care for Men and HPV
Human Papilloma Virus (HPV) is an incredibly common virus with over 150 types. Click here to learn more about the prevention and treatment with Colgate.
Read More
HIV/AIDs & STDs
Dental Problems Associated With HIV/AIDS
If you are anxious, spending a few minutes asking your dentist any questions you may have about health and safety precautions can put your mind at ease.
Read More
HIV/AIDs & STDs
Everything You Should Know About Herpes Stomatitis
Find out more about herpes stomatitis - including the how you contract it, diagnosing, signs, symptoms, and how to manage it, here.
Read More
HIV/AIDs & STDs
Five Oral Manifestations Of HIV
In fact, according to the NIH, more than a third of those who are HIV-positive suffer from oral health problems that are a direct result of their condition.
Read More
HIV/AIDs & STDs
HIV/AIDS STDS 101
Find out more about the affects of AIDS & HIV on oral health. HIV manifest as mouth ulcers and a weakened immune system can affect your oral health. Find out more, here.
Read More
HIV/AIDs & STDs
How Herpes On Gums Affects Your Oral Care
Herpes simplex infections are very common, even around the mouth. And although herpes on gums can be distressing, it is manageable with the right approach.
Read More
HIV/AIDs & STDs
HPV In Men
Although human papillomavirus (HPV) in men is often misunderstood, it is a growing medical condition found in the oral cavity. Here's how to identify it.
Read More
HIV/AIDs & STDs
What Are Mulberry Molars?
Mulberry molars are a tooth abnormality caused by congenital syphilis, resulting in teeth that have many small bumps, like mulberry fruits.
Read More
HIV/AIDs & STDs
STDs of the Mouth; Types, Symptoms, and Treatment
Sexually transmitted diseases (STDs) are contracted through various forms of sexual activity. The following STDs of the mouth can require unique responses.
Read More
HIV/AIDs & STDs
STDs Of The Mouth And How To Avoid Them
The most common STDs of the mouth are herpes, chlamydia, gonorrhea and syphilis. Learn more about these STDs here.
Read More
HIV/AIDs & STDs
Oral Thrush Causes & It's Connection To HIV
Oral thrush can be common for people with conditions that suppress the immune system, such as HIV. Click here to learn more about oral thrush with Colgate®
Read More
Jaw Pain (TMD)
3 TMJ Physical Therapy Exercises To Try
Looking for pain relief for your temporomandibular joint pain (TMJ)? There are several options for physical therapy to alleviate pain. Learn more, here.
Read More
Jaw Pain (TMD)
Are TMJ and Vertigo Related?
TMJ affects your jaw joints in front of your ears. It can, though rarely, it can affect your inner ears and lead to TMJ and vertigo. Learn more, here.
Read More
Jaw Pain (TMD)
Can A Chiropractor Alleviate TMD Symptoms?
When a patient's TMD is due to incorrectly positioned bones and neck muscles, a TMJ chiropractor might be able to help. Find out more about it, here.
Read More
Jaw Pain (TMD)
Could Your Lateral Pterygoid Muscle Be Causing TMJ Pain?
The lateral pterygoid muscle is one of the four muscles of mastication and is responsible for moving your jaw. Learn how it relates to the TMJ.
Read More
Jaw Pain (TMD)
Do Braces Help Treat TMD?
For some patients, TMJ braces can help reduce strain on the jaw joints, alleviating the symptoms of TMD. Find out more about the relationship, here.
Read More
Jaw Pain (TMD)
Does Acupuncture Work for TMJ?
If you have pain caused by temporomandibular joint disorder, commonly known as TMJ or TMD, you may be wondering if acupuncture for TMJ could work for you.
Read More
Jaw Pain (TMD)
Foods To Eat When Your TMJ Is Aching
Suffering from TMJ and don't know what to eat? Here are the best foods to eat to help ease the pain of TMJ.
Read More
Jaw Pain (TMD)
Can Your TMJ Cause Dizziness?
Dizziness is a sign of TMD that may leave you concerned that it may be caused by a serious condition. Learn more here.
Read More
Jaw Pain (TMD)
Is Surgery An Option For TMD Problems?
How long is TMJ surgery recovery time? Learn more about the different types of surgeries and what you can expect from the healing process, here.
Read More
Jaw Pain (TMD)
How TMJ And Ear Pain Are Related And Treated
Here's a look at disorders of the TMJ and ear pain, how to differentiate this sensation from other types, why it occurs, and how to find ear pain relief.
Read More
Jaw Pain (TMD)
Jaw Pain: Causes And Treatments
There are several medical conditions that can be contributing factors to jaw pain; this possibility makes diagnosis and treatment much more difficult.
Read More.png)

Jaw Pain (TMD)
Neuromuscular Dentistry: A Definition
What is neuromuscular dentistry? Check out this great article to learn more about this specialty and when this type of dental treatment is necessary.
Read More
Jaw Pain (TMD)
TMJ Disorder Treatment Options
If you experience pain in your neck and jaw area, a clicking or popping noise when you open or close your mouth, or a limited ra...
Read More
Jaw Pain (TMD)
Snap, Crackle, Ouch! Causes Of Jaw Pain
The potential causes of jaw pain are manifold. TMJ disorder is reported by more women than men and may occur on one or both sides of the face.
Read More.png)
Jaw Pain (TMD)
Temporomandibular Disorders
If you have questions about TMD, you are not alone. Researchers, too, are looking for answers to what causes TMD, what are the best treatments, and how can we prevent these disorders.
Read More
Jaw Pain (TMD)
Temporomandibular Joint Anatomy And 3 Common Complications
Temporomandibular joint anatomy is complex, and there are several conditions that can affect it. Learn about the three most common TMJ issues. Learn more.
Read More
Jaw Pain (TMD)
Three Ways A TMJ Massage Can Relieve Jaw Pain
TMJ is usually the result of inflamed and painful chewing muscles around your jaw. Luckily, a TMJ massage can act as an effective, non-medicinal solution.
Read More
Jaw Pain (TMD)
TMJ Anatomy: What To Know
Because of the complexity of your TMJ anatomy, disorders and pain can be common. Let's take a look at what makes up this joint.
Read More
Jaw Pain (TMD)
TMJ And Teenagers: Treatment Options
There is a rising concern with the temporomandibular joint (TMJ) and teenagers.
Read More
Jaw Pain (TMD)
TMJ Arthralgia Symptoms and Treatment Options
TMJ arthralgia is a condition within TMD that refers to pain and inflammation inside your joints. Learn more about the symptoms and treatment, here.
Read More
Jaw Pain (TMD)
TMJ Arthrocentesis: Everything About The Procedure
TMJ arthrocentesis is a minimally invasive surgery that helps alleviate a stiff or painful jaw joint. Learn more.
Read More
Jaw Pain (TMD)
Can Essential Oils Relieve TMJ Jaw Pain?
Essential oils are used to treat a range of maladies. Learn what the science says and how TMJ essential oils may help relieve your jaw pain, here.
Read More
Jaw Pain (TMD)
TMJ Exercises For Pain Relief
Although the discomfort can go away on its own, many people have found that TMJ exercises help ease an irritated jaw. Here are some of them.
Read More
Jaw Pain (TMD)
Understanding Jaw Joint Pain And How To Find Relief
When your jaw hurts it's common to experience irritation from basic movement. There are many causes of jaw joint pain and several ways to treat. Learn more.
Read More
Jaw Pain (TMD)
What's Causing Your Facial And Jaw Pain?
Your facial or jaw pain could be caused by one of numerous sources, but here are some of the common culprits.
Read More
Jaw Pain (TMD)
What Is A TMJ Appliance?
How does a TMJ appliance work and how may it relieve TMD discomfort? Find out more about what a TMJ appliance is here, and if its the right option for you.
Read More

Jaw Pain (TMD)
What Is TMJ Arthritis And How Is It Connected?
Is temporomandibular joint dysfunction a cause of TMJ arthritis or a result? Find out more about the connection between TMJ and arthritis, here.
Read More
Jaw Pain (TMD)
What Is TMJ Arthroscopy?
If you have jaw joint discomfort, your dentist may recommend a TMJ arthroscopy to alleviate pain. What should you know about it? Find out, here.
Read More
Jaw Pain (TMD)
What Is TMJ?
What is TMJ vs TMD? Every time you talk, yawn and chew, you’re using your TMJs. Learn more about how to treat the problem at Colgate® Oral Care.
Read More
Jaw Pain (TMD)
When A Clicking Jaw Is A Sign Of TMD
If "snap," "crackle" and "pop" aren't coming from your cereal, it may be from your temporomandibular joint (TMJ). TMJ complications affect over 10 million people. Learn more here.
Read More
Jaw Pain (TMD)
Your Mandible Bone And Your Dental Health
The mandible bone is the lower jawbone, and it plays a critical role in your dental and overall health. Learn how to keep this bone healthy.
Read More
Jaw Pain (TMD)
Temporomandibular Joint Disorder: Symptoms and Treatment
Discover the full list of available temporomandibular disorder treatments at Colgate.com. From simple changes in your diet, to ice packs to medication – there are a number of treatments that will lesson the symptoms and relieve pain.
Read More
Jaw Pain (TMD)
Temporomandibular Joint (TMJ) Dislocation: Symptoms, Treatment & Prevention
Read More
Jaw Pain (TMD)
The Relationship Between TMJ And Neck Pain
If you have pain in your neck and jaw, you may have an issue with your temporomandibular joint (TMJ). Here's how TMJ and neck pain are connected.
Read More
Jaw Pain (TMD)
Yoga For TMJ Pain Relief: Does It Work?
You often hear about the health benefits of yoga to relieve body pain. But what about yoga for TMJ disorders? Here's how yoga might help you.
Read More
Digestive (Gastrointestinal) Disorders
Are You Having Difficulty Swallowing?
Are you having difficulty swallowing? Find out more about dysphagia, the signs and symptoms, and when to contact your doctor, here.
Read More
Digestive (Gastrointestinal) Disorders
Gardner Syndrome Teeth: Early Oral Implications
What are Gardner syndrome teeth and how may they provide insight into a potentially serious condition? Find out more about this rare disease, here.
Read More
Digestive (Gastrointestinal) Disorders
Identifying Mouth Ulcers From Crohn's Disease
Bowel diseases aren't limited to gastrointestinal issues. Here's how to identify if you have Crohn's mouth ulcers, and how to manage them.
Read More
Digestive (Gastrointestinal) Disorders
Sulfur Burps: What Are They?
A little gas from your stomach is normal, but sulfur burps smell bad and can leave you feeling embarrassed. Find out more about sulfer burps, here.
Read More
Digestive (Gastrointestinal) Disorders
Gastrointestinal Disorders 101
Find out more about how gastrointestinal disorders can affect your teeth, gums, and overall oral health. For more information on your dental health, visit Colgate.com
Read More
Digestive (Gastrointestinal) Disorders
Oral Manifestations of Celiac Disease: Enamel Defects, Mouth Sores and Dry Mouth
The sores caused by celiac disease are very similar to aphthous stomatitis or oral ulcers. Learn more about celiac mouth sores here.
Read More
Bridges & Crowns
After A Dental Bridge Procedure: What To Expect
After a dental bridge procedure, you can expect to eat and chew without problems, but you need to make some changes to your dental care routine.
Read More
Bridges & Crowns
Bridges & Crowns 101
Both dental crowns and bridges are fixed prosthetic devices. Find out more about the different types of dental bridges and crowns as well as its effect on your oral health.
Read More
Bridges & Crowns
Dental Bridge Vs. Implant: Which Is Right For You?
What's the difference between a dental bridge vs. implant? Often the dental implant is ideal, but the following should be considered before deciding.
Read More
Bridges & Crowns
Different Types Of Dental Crowns
Before differentiating between the different types of dental crowns, consider the functions they serve. Learn more here about dental crowns.
Read More
Bridges & Crowns
All About Front Tooth Crowns
Don't be afraid that a front tooth crown will ruin your smile. With these facts, you can rest assured that your smile can still look healthy and natural.
Read More
Bridges & Crowns
Getting Dental Impressions? Here's What to Expect
Whenever your dentist introduces your teeth to a foreign object, dental impressions are taken to ensure the restoration won't interfere with your bite.
Read More
Bridges & Crowns
Gold Tooth Crown Facts and History
Besides the obvious unique smile you'll have after completion, a gold tooth crown provides many positive benefits. Find out more about gold tooth crowns.
Read More
Bridges & Crowns
How Much Does a Dental Crown Cost?
Do you need a dental crown? There are many types of dental crowns and materials. Which type and material will impact cost. Find out average cost is, here.
Read More
Bridges & Crowns
Common Dental Bridge Problems and How to Avoid Them
It's remarkable how bridges can correct your smile; however various dental bridge problems may arise if they're not well-maintained. Find out more here.
Read More
Bridges & Crowns
Removable Dental Bridge: What To Expect
A removable dental bridge is a partial denture that you take out to clean every day, but usually not until after an adjustment period.
Read More
Bridges & Crowns
Restorative Dentistry: Explanation Of Crowns And Broken Teeth
Both dental crowns and bridges are fixed prosthetic devices. Find out more about the different types of dental bridges and crowns as well as its effect on your oral health.
Read More
Bridges & Crowns
Porcelain Crowns and Your Valuable Smile
A white smile is a powerful statement. Porcelains crown can spruce up a tooth and restore confidence. Find out more about porcelain crowns and its perks.
Read More
Bridges & Crowns
The Role An Abutment Plays In A Dental Implant
In a dental implant, an abutent is needed to connect the post to the crown. Learn more about the important role a dental abutment plays in an implant.
Read More
Bridges & Crowns
Tooth Crown Pain: Causes And Treatment
If you're experiencing tooth crown pain, whether it's a new crown or an established one, you'll need to get it sorted out before you can have real relief..
Read More
Bridges & Crowns
Tooth Tattoo: What's That?
Want to add flair to your smile? Your dentist can help you prepare for a tooth tattoo, a unique form of body art where a design is drawn on a crown.
Read More.jpeg)
Bridges & Crowns
Understanding A Dental Bridge Procedure
A dental bridge is one item that can help restore your natural smile in the event of tooth loss. Here are the ins and outs of a dental bridge procedure.
Read More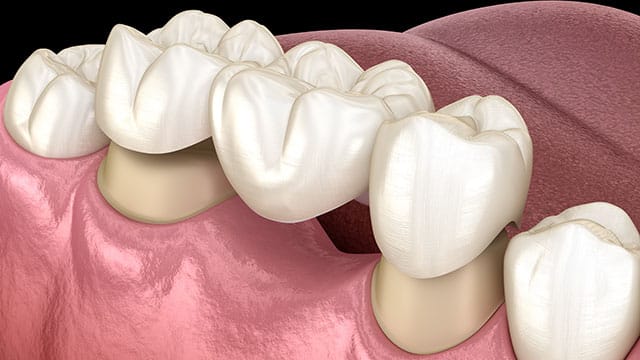
Bridges & Crowns
What’s the Difference Between Dental Crowns and Tooth Bridges?
Before either a crown or a bridge can be made, the tooth (or teeth) must be reduced in size so that the crown or bridge will fit over it properly. Learn more here.
Read More
Bridges & Crowns
What Is a Clinical Crown?
You've heard of a crown, and might even have one, but what is a clinical crown? Learn more about the part of your tooth not covered by tissue, at Colgate®.
Read More
Bridges & Crowns
What Are Zirconia Crowns?
Zirconia is a metal classified as a member of the titanium family. Learn more about how and why zirconia is used in dental crowns and if they're for you.
Read More
Bridges & Crowns
What To Know About A Metal Cap On Teeth
Is your dentist recommending a metal cap on teeth? Learn about the different types of caps, or crowns, and their important role in repairing your teeth.
Read More
Bridges & Crowns
When You Need Dental Bridge Repair
Dental bridges replace missing teeth with the help of your other teeth, and can last for decades. But you may need dental bridge repair if it has broken.
Read More
Bridges & Crowns
Why Do I Need A Temporary Crown?
Even if a tooth is slated for a crown, dentists need to protect it while the item is being made and delivered. Here's why you might need a temporary crown.
Read More
Bridges & Crowns
Why You Might Want A Tooth Bridge Over Implants
A tooth bridge provides support you need to prevent surrounding teeth from moving out of place. But how does it differ from an implant? Learn more here.
Read More
Bridges & Crowns
Your Dental Crown Procedure: What To Expect
Your dentist may recommend that you undergo a dental crown procedure for one of several reasons: you have a particularly weak… Read more at Colgate.com
Read More
Bridges & Crowns
Four Types of Dental Bridges
Are you missing teeth? Don't worry, you're not alone. Here are four types of dental bridges that your dentist may recommend.
Read More
Bridges & Crowns
What You Need to Know About Dental Crowns
A crown is a tooth-shaped cover placed over a tooth that is badly damaged or decayed. Read more here on whether or not you need a crown for your tooth.
Read More
Bridges & Crowns
How Long Do Dental Bridges Last?
How long do dental bridges last? Professional opinions vary, but it certainly depends on your diet and how well you care for them.
Read More
Bridges & Crowns
How Your Dentist Will Recement A Crown
If your dental crown becomes loose or pops off, it can be concerning. Luckily, your dentist can recement a crown. Here's how the process works.
Read More
Bridges & Crowns
Is a Molar Dental Implant Right For You?
If you lose a molar, what are your options for replacing it? Here's what to know about a molar dental implant, its benefits and its risks.
Read More
Bridges & Crowns
Maryland Bridges: What to Know About This Tooth Replacement Option
Maryland bridges can be great solutions for patients who are missing a single tooth. Here's what to know about this tooth replacement device.
Read More
Bridges & Crowns
Pros and Cons of Cantilever Bridges
Cantilever bridges are one type of dental restoration commonly used to replace missing front teeth. Here's what to know about the tooth replacement option.
Read More
Bridges & Crowns
What's a Luting Agent? Types of Dental Cements to Secure Your Restoration
A luting agent in dentistry refers to the cement your dentist uses to adhere a restoration to your tooth. Here are some of the types they might use.
Read More
Fillings
Caring For Your Temporary Dental Filling
There are many reasons a dentist may place a temporary dental filling. Perhaps you've just had a root canal, or maybe you're… Read more at Colgate.com
Read More
Fillings
Chewing Tips After A Filling
After you get a filling in one or more of your teeth, soreness and tooth sensitivity may persist for hours, or even days,… Read more at Colgate.com
Read More
Fillings
Dental Fillings Are Durable But Don't Last Forever
A dental filling, also called a dental restoration, is intended to replace tooth structure lost to decay. Dental fillings may last many years but eventually all fillings need to be replaced. Learn more about the longevity and durability of dental fillings here.
Read More
Fillings
Fillings 101
Learn more about the basic of tooth fillings and your Oral health at Colgate.com. Read about the different types of dental fillings, oral health risks, and more.
Read More
Fillings
Fillings For Teeth: What Are Your Options?
If your most recent dentist appointment informed you of a cavity, you have plenty to keep you positive. There are many types of fillings for teeth today.
Read More
Fillings
How Long Does It Take to Fill a Cavity?
How long does it take to fill a cavity? While getting a cavity isn't fun, the treatment only takes about an hour, so book a visit with your dentist.
Read More
Fillings
Is Tooth Drilling Necessary In Dental Treatment?
Tooth drilling is often necessary to take care of a cavity, but new technologies including plasma jets or lasers could make it a thing of the past.
Read More
Fillings
Lithium Disilicate 101: Use, Benefits & Care
Lithium disilicate is a ceramic material used in dental restorations. Learn more about its uses and how to care for your restorations, here.
Read More
Fillings
Onlay Preparation and Expectations
Onlays can set you up for years of tooth health, but the restorations require some preparation. Here's what to expect for your onlay preparation.
Read More
Fillings
What Happens When Your Child Gets a Filling?
Going to the dentist is a regular event, but it can be stressful if you or your kids get sensitive teeth after filling work. Here's how to make it easier.
Read More
Fillings
When a Dental Inlay Is Your Best Option
What is a dental inlay and in what situations would your dentist recommend one? Find out more about dental inlays and if they're going to be right for you.
Read More
Fillings
White Fillings Can Make Your Smile Last
Before deciding if white fillings are a good choice for you, here's what you need to know about two other common options out there. Learn more, here.
Read More
Fillings
Tooth Pain After A Filling: Is It Normal?
There are several reasons why you may experience tooth pain after a filling. Is it normal? Is there anything you can do about it? Learn more, here.
Read More
Fillings
What is a Filling
A filling is a way to restore a tooth damaged by decay back to its normal function and shape. Learn more about what a filling is and when you may need one here.
Read More
Fillings
Jaw Pain After a Filling: What Might Be the Cause?
If you have jaw pain after receiving a dental filling, you may be concerned that something went wrong with your procedure. Here's why you may have pain.
Read More
Fillings
Let's Compare Metal vs. Metal-Free Fillings
Hearing that you have a cavity can be upsetting, but there are many types of fillings that can solve the problem. Learn more about metal-free fillings.
Read More
Fillings
Dental Amalgam: Is it Safe?
Dental amalgam was once one of the most common materials used to fill cavities. Also known as “silver fillings,” amalgam fillings are silver in appearance, but not in composition.
Read More
Dentures
3 Teeth Replacement Options: What's Right For You?
Don't know what to do about a lost tooth? Knowing all your teeth replacement options will help get your smile up and running again. Find out more, here.
Read More
Dentures
4 Common Denture Problems And How To Solve Them
There are some common problems that people can encounter when they first get dentures. Here's what to expect when you first start wearing dentures.
Read More
Dentures
Adjusting to New Dentures May Take Time
For people who have lost their teeth due to disease or injury, dentures can restore their smile and help them with everyday tasks such as eating and speaking. However, getting used to wearing dentures may require a period of adjustment.
Read More
Dentures
All About Relining Dentures
What if a dental prosthetic doesn't fit as comfortably as it used to? It may be time to talk to your dentist about relining dentures. Find out more, here.
Read More
Dentures
Denture Repair: Why It's Needed And How It's Done
The longer a denture is worn, the more likely it will merit a visit to your dentist for repair. Find out more about why dentures need repair and more.
Read More
Dentures
Eating With Dentures
Adjusting to eating with dentures takes a little practice, but over time you should be able to return to your normal diet – with one or two exceptions.
Read More
Dentures
Extractions and Dentures in the Same Day: Are You a Candidate?
Looking to get a tooth extracted and a denture implant in the same day? Find out here whether you are a candidate or not and what to expect.
Read More
Dentures
5 Tips For Getting Comfortable Wearing Dentures
Getting used to dentures and how to wear them well is paramount to your health. Fortunately, you don't need to sacrifice comfort for a great new smile.
Read More
Dentures
How To Clean Dentures To Avoid Bacteria Buildup
Learning how to clean dentures is important to maintaining good daily hygiene, but occasionally you may find it necessary to take these additional steps.
Read More
Dentures
How to Tell if You Need Denture Adhesive
Denture adhesive can improve the fit of full or partial dentures. Well-fitting dentures usually do not need help staying in, but many people still use them for a sense of security.
Read More
Dentures
Is a Flipper Denture Right for You?
If you've lost a front tooth, a flipper denture may be the right option for you to restore your smile. Learn more about flipper dentures, here.
Read More
Dentures
Living With Dentures When You're Young
You can be confident about living with dentures by adapting and maintaining your lifestyle so they have only a small impact on your day-to-day.
Read More
Dentures
Mini Dental Implants: The Best of Both Worlds
Mini dental implants are a more comfortable and more affordable alternative to dentures and implants. Learn more if mini dental implants are right for you.
Read More
Dentures
How to Fix Poorly Fitting, Damaged, or Broken False Teeth
Whether false teeth break or don't fit well, the best solution is to visit a dentist – not your toolbox. Here's how to address these various conditions.
Read More
Dentures
Taking Care Of A Partial Denture
Handling a partial denture requires proper dental care. Always remember to brush the denture each day to remove food deposits and plaque. For more ways to care for your partial denture, continue reading here.
Read More
Dentures
The History Of Wooden Teeth (And Other Clever Dentures)
What did our ancestors stick in their mouths when they were out of choppers? Learn more about the history of wooden teeth, George Washington, and dentures.
Read More
Dentures
The Pros And Cons Of Snap-On Dentures
Snap-on dentures are also called removable implant-supported dentures or overdentures. Learn how they compare to conventional dentures.
Read More
Dentures
What Are Dentures Made Of?
Dentures are replacements for missing teeth that can be taken out and put back into your mouth. Learn more about the materials and proper denture care here.
Read More
Dentures
What Are Dentures?
If you have missing or damaged teeth, getting dentures can help you look and feel your best. Learn about the types of dentures available and find tips for caring for your dentures so you can get a beautiful, healthy smile.
Read More
Dentures
What Are Flexible Dentures?
Flexible dentures are an alternative to a traditional pair. Here's what you need to know and if you should ask your dentist about this option.
Read More
Dentures
What Are Temporary Dentures?
By bridging the gap until your permanent dentures are ready, temporary dentures ensure you never have to go a day without teeth. Find out more, here.
Read More
Dentures
What Do Immediate Dentures Cost?
Not sure if you need immediate or conventional dentures? Check out our article to compare prices as well as which denture type is the best choice for you.
Read More
Dentures
Why You Might Need a Vestibuloplasty Procedure Before Dentures
Vestibuloplasty is a surgical procedure to improve the fit of a prosthetic device. Here's what to expect if a dental professional recommends the treatment.
Read More
Dentures
How To Whiten Dentures: Stain Removal And Prevention
You want your smile to shine, but dentures can become stained. Learn how to whiten dentures at home and with a dentist's help, here.
Read More
Dentures
What Are Implant-Supported Dentures?
What are denture implants? Permanent implant supported dentures are a type of overdenture that is supported by and attached to dental implants in the jawbone that extend outward from the gums.
Read More
Dentures
Tips for Proper Denture Storage
During the day, your dentures give you the confidence to smile, talk and eat the way you did before you lost your teeth. But at night when you're ready...
Read More
Dentures
Types of Removable Partial Dentures to Consider
If you're missing teeth, you have many options to restore your smile. Here's an overview of the different types of removable partial dentures available.
Read More
Dentures
Your Guide to Denture Alternatives: Let's Build Your New Smile
If you're missing all or some of your teeth, you may be wondering what denture alternatives are available. Here's what to discuss with your dentist.
Read More
Nutrition & Oral Health
10 Healthy Alternatives To Satisfy Your Sweet Tooth
You know you want to take care of your teeth but you just can't help it — you have a sweet tooth! So you're asking, \"What should I eat when I crave sweets?\" Luckily, there are lots of easy options to choose from. Here are ten healthy (and tasty!) alternatives to sweets:
Read More
Nutrition & Oral Health
12 Drinks Ranked: Best And Worst For Your Teeth
Trying to turn the page on your oral care and brighten that smile? Avoiding these drinks will help you on your way.
Read More
Nutrition & Oral Health
3 Snacks To Avoid If You Don't Want It Stuck In Your Teeth
Food stuck in teeth can cause numerous problems. Find out the top 3 foods that get stuck in teeth easily and the most effective ways to remove them.
Read More
Nutrition & Oral Health
5 Essential Vitamins for Teeth and Gum Health
Proper nutrition is beneficial for your whole body, including your teeth and gums. By ingesting the right vitamins through food or supplements, you can help protect your oral health.
Read MoreNutrition & Oral Health
A Food Guide Pyramid For Kids Helps Teach Good Nutrition
Good nutrition plays a major role in building a healthy body and strong teeth. The Food Guide Pyramid for Kids was developed for parents and caregivers...
Read More
Nutrition & Oral Health
An Apple Smiles Snack Is Sure To Please
Most parents can attest to the fact that children are not always all that daring when it comes to trying new foods.
Read More
Nutrition & Oral Health
Brown Tongue: Symptoms, Causes And Treatment
A few lifestyle habits may cause a brown tongue, but luckily, changing a few of your habits can fix your brown tongue.
Read More
Nutrition & Oral Health
Calcium-Rich Foods: What To Eat For Healthier Teeth
Even if you brush and floss regularly, you could be neglecting an important component of oral health: your diet. Learn more here.
Read More
Nutrition & Oral Health
Can Spicy Foods Damage Your Teeth?
Do you love eating spicy foods, but worry it will damage your teeth? Learn more about the effects of spicy foods on your teeth here.
Read More
Nutrition & Oral Health
Why Should We Eat Food Slowly & Chew Properly
Chewing food might seem simple & instinctive, but how you chew may impact your oral health. Learn more about why and how to chew correctly. Click here.
Read More
Nutrition & Oral Health
Does Toothpaste Expire?
Colgate products typically have a two-year expiration date to ensure that the fluoride is at an optimal level of stability, as the ions in the fluoride are at their most effective within two years.
Read More
Nutrition & Oral Health
Eating Healthy For Kids: Four Ways To Make It Fun
There are countless benefits to eating healthy for kids, but encouraging them can be difficult. Luckily, there are ways to inspire them to stay healthy.
Read More
Nutrition & Oral Health
Enjoy Halloween Candy Responsibly And Avoid Tummy Aches And Cavities
Halloween candy is a treat, not a meal, so you must avoid letting your children gorge themselves on sweets this season.
Read More
Nutrition & Oral Health
Finding Good Foods For Your Teeth
While the American Dental Association (ADA) recommends following a balanced, low-sugar diet, there are also certain foods that… Read more at Colgate.com
Read More
Nutrition & Oral Health
Folic Acid: The Oral and Prenatal Health Supervitamin
Folic acid is a vital super vitamin for expectant mothers. This promotes a healthy pregnancy as well as keeping your teeth strong. Learn more here.
Read More
Nutrition & Oral Health
Foods For A Healthy Mouth
A nutritious and well-balanced diet of foods for a healthy mouth is simple and delicious.
Read More
Nutrition & Oral Health
Foods Low In Sugar Are Better For Your Teeth
Keeping teeth healthy, whether your own or your children's, relies on several factors. You know you should floss once a day,… Read more at Colgate.com
Read More
Nutrition & Oral Health
Foods That Prevent Tooth Decay
Sugary treats, sticky snacks and syrup-laden sodas are bad news for your teeth, of course, but did you know there are some foods that prevent tooth decay?
Read More
Nutrition & Oral Health
Good Nutrition For Kids: Tips To Help Their Teeth
Your child needs a nutritious diet to grow up big and strong, but good nutrition for kids also plays a big role in the health of his or her mouth.
Read More
Nutrition & Oral Health
Is Chewing Gum Good for Your Teeth?
Chewing any regular sugar free gum can help prevent cavities by removing food particles from the surfaces of your teeth. Learn more here.
Read More
Nutrition & Oral Health
Halloween Candy Safety: What Is In Your Child's Treat Bag?
Do you know what is in your child's trick-or-treat bag? Before letting the little ones feast on chocolates, suckers and gummy treats, inspect the candy.
Read More
Nutrition & Oral Health
4 Healthy Breakfasts to Start Your Day
Breakfast wakes up your metabolism and you'll get a healthy dose of vitamins and minerals, which keep organs and bones healthy, including your teeth.
Read More
Nutrition & Oral Health
Healthy Breakfast For Children: Start Their Day Right
Breakfast is the most important meal of the day, for you and for your children. A nutritious morning meal helps you fulfill… Read more at Colgate.com
Read More
Nutrition & Oral Health
Healthy Breakfast Ideas: Calcium Rich Cheesy Vegetable Omelet
Omelets are a great place to begin when you're looking for healthy breakfast ideas because they are high in protein and are generally low in calories,...
Read More
Nutrition & Oral Health
Healthy Foods For Kids: Lowering Sugar Intake
Eating a nutritionally balanced diet is very important for your child's health. Obese and overweight children are at an increased risk of serious ailments.
Read More
Nutrition & Oral Health
The Best Foods For Your Teeth
One of the first areas to decline when your diet is less than ideal is your oral health. Use this healthy foods list to improve your diet and the health of your mouth.
Read More
Nutrition & Oral Health
Healthy Fruit Drinks To Make You Smile
You've probably heard it said that soda is bad for your teeth; not only is soda highly acidic, but it also leaches the calcium… Read more at Colgate.com
Read More
Nutrition & Oral Health
Healthy Halloween Treats: Low Sugar Alternatives To Sweets
When it comes to worrying about tooth decay on Halloween, the focus is generally on trick-or-treating and candy, but with parties and festivals galore...
Read More
Nutrition & Oral Health
Healthy Halloween Treats Satisfy Kids And Dentists Alike
You care about the dental health of neighborhood children, but you do not want to be a joyless Halloween witch who dispenses only toothbrushes and floss.
Read More
Nutrition & Oral Health
Healthy Holiday Snacks For You And Your Kids
One of the biggest culprits of poor dental health in kids is sugar. These healthy holiday snacks can help protect tooth decay.
Read More
Nutrition & Oral Health
Healthy Holiday Treats The Whole Family Will Love
Sugary holiday desserts can take a toll on your dental health. Try these healthy holiday treats as practical, delicious alternatives to traditional sweets.
Read More
Nutrition & Oral Health
Healthy Packed Lunches Save Money And Protect Your Teeth
You might always pack a lunch for your child, but if you hit the drive-through on a regular basis, your pocketbook, as well as y...
Read More
Nutrition & Oral Health
Healthy Thanksgiving Tips For A Tooth-Friendly Holiday
Thanksgiving is a holiday infamous for rows of food, many of which are not especially good for you. Here are some tips for keeping your holiday healthy.
Read More
Nutrition & Oral Health
How 3 Trendy Diets Affect Your Teeth
Planning on starting a new trendy diet? Learn about the effects on oral health before getting started.
Read More
Nutrition & Oral Health
How Acidic Foods Affect Teeth And Which To Avoid
When you indulge during the holiday season, acidic foods are often on the menu. Here are some common acidic foods, and how to protect your teeth from them.
Read More
Nutrition & Oral Health
How High-Alkaline Foods Benefit Your Teeth
An alkaline-based diet starts and ends with fruits and veggies. Whether or not a food is alkaline has to do with how it metabolizes in the body as opposed to its composition.
Read More
Nutrition & Oral Health
How To Fix Wine Stained Lips After A Glass Of Red Wine
Find out more about wine stained lips. There are things you can do before, during, and after drinking a glass of red to avoid wine stained lips.
Read More

Nutrition & Oral Health
How to Stop Drinking Soda: Six Ways To Kick Your Soda Habit and Improve Your Oral Health
Soft drinks have been linked to tooth decay for all ages. Click here to find out the six ways to kick your soda habit & improve your oral health with Colgate.
Read More
Nutrition & Oral Health
Hypoglycemia and Managing Glucose Levels
Hypoglycemia occurs when the glucose levels in your blood fall too low. Learn how to manage the symptoms of this condition and establish healthy habits.
Read More
Nutrition & Oral Health
Is Milk Good for Your Teeth?
Dairy products keep your teeth as healthy as your bones throughout your life. So, is milk good for your teeth? The answer is a resounding yes, and here's why.
Read More
Nutrition & Oral Health
Loss of Taste: Causes and Treatments
Food lacking flavor these days? Here's what could be disrupting your ability to taste and what you can do about loss of taste. Learn more, here.
Read More
Nutrition & Oral Health
Nutrition and Oral Health 101
Discover how nutrition impacts your oral health & simple adjustments you can make to ensure a healthy smile for you and your family with Colgate.
Read More
Nutrition & Oral Health
Nutrition for Healthy Teeth, Child Growth and Development
Here is how to ensure your kids get the nutrition they need for healthy teeth and proper child growth and development.
Read More
Nutrition & Oral Health
Nutrition For Kids: 5 Healthy Foods That Improve Dental Health
There are many ways to help your kids have better dental health. You can encourage your kids to brush at least twice a day and f...
Read More
Nutrition & Oral Health
How Eating Healthy Impacts Your Oral Health
By knowing how to eat healthy, you can improve your physical and oral health, prevent disease and promote healthy growth and development for children and adolescents.
Read More
Nutrition & Oral Health
Oral Care During The Holidays: Sugar-Free Countdown To Christmas
Maintaining good oral care during the holidays can be tough with the bombardment of sugary sweets all season. Counting down to Christmas with an advent...
Read More
Nutrition & Oral Health
Pregnancy And Dental Health: Foods to Eat
How to protect teeth during pregnancy? Click here here for our list of powerhouse foods that will keep your smile healthy throughout your pregnancy.
Read More
Nutrition & Oral Health
Prevent Tooth Decay With Halloween Candy Alternatives
Halloween is a night for trick-or-treat, goblins, superheroes, princesses and lots of fun. However, it can also be a time for tooth decay.
Read More
Nutrition & Oral Health
Preventing Obesity In Children And Teens
Obesity in children is a growing problem. It is associated with numerous health-related conditions and ailments such as diabetes and heart disease.
Read More
Nutrition & Oral Health
Smart Snacks For Healthy Teeth
Healthy teeth start with smarter snacks, learn more here.
Read More
Nutrition & Oral Health
Soda Or Pop? It's Teeth Trouble By Any Name
Acids and acidic sugar byproducts in soft drinks soften tooth enamel, contributing to the formation of cavities. Learn more about the damage soda causes to teeth here.
Read More
Nutrition & Oral Health
Soft Food Diet Options: What To Eat After Dental Treatment
A soft food diet is required after certain dental procedures, like extractions and implants, to prevent damage to your teeth, mouth or new prosthetic.
Read More
Nutrition & Oral Health
Surprisingly Simple Food Tips For Healthy Teeth
Consider a few tips for healthy teeth involving simple foods that may be more helpful to your dental health than you thought they were.
Read More
Nutrition & Oral Health
Tea Tree Oil & Your Teeth
Tea tree oil has become a very popular natural remedy for oral health. Learn more about the benefits and how to properly use it.
Read More
Nutrition & Oral Health
Teeth Care For Toddlers: Trying Tooth-Friendly Foods
What your toddler eats can have a huge impact on oral health, and most toddlers are drawn to sweet foods full of refined carbohydrates.
Read More

Nutrition & Oral Health
Tooth Cupping: Causes, Prevention, And Treatment
What is tooth cupping? How might your habits lead to these indentations on your teeth? Learn more here.
Read More
Nutrition & Oral Health
What Is Dental Public Health?
Dental public health programs assist those with limited access to oral healthcare receive proper treatment and help them prevent problems. Learn more here.
Read More
Nutrition & Oral Health
What to Eat After Tooth Extraction
Once you've scheduled the surgery, you might wonder what to eat after tooth extraction. And as you might expect, soft foods are ideal during the first few days of recovery.
Read More
Nutrition & Oral Health
Does Taking Vitamin K2 Benefit Your Oral Health?
You are what you eat, and the vitamins you include your diet can benefit your overall health. Here's what to know about vitamin K2 benefits.
Read More
Nutrition & Oral Health
What You Need to Know About Getting a Lip Tattoo
If you are thinking about getting a lip tattoo, here's what you need to know how to prepare yourself and take care of it.
Read More
Nutrition & Oral Health
Acidic Foods And How They Affect Your Teeth
Fruits can be good for both your dental health and overall health. Acidic fruits however, can also be damaging to your tooth enamel. Learn more, here.
Read More
Nutrition & Oral Health
Sugar-Free Drinks: Are They Safe For Teeth?
Phosphoric acid, citric acid and tartaric acid are some of the ingredients in diet sodas and fruit juices that damage teeth, but you can reduce the effects of acidic drinks by taking these precautions.
Read More
Nutrition & Oral Health
Ketosis Breath: When Your Diet Affects Your Oral Health
If you follow the keto diet, you may notice you start to have bad breath. Learn more about ketosis breath, plus other considerations for oral health, here.
Read More
Nutrition & Oral Health
4 Non-Acidic Drinks to Help You Avoid Enamel Erosion
Choosing these non-acidic drinks over indulgences such as soda, coffee and alcohol can help remineralize your enamel before it completely wears away.
Read More
Nutrition & Oral Health
Tooth Nerve Pain: Triggers & Treatment
Whether it's a sharp, stabbing sensation or a dull ache, tooth nerve pain can take the enjoyment out of eating. Find out what can trigger tooth nerve pain.
Read More
Nutrition & Oral Health
Does Drinking out of Cans Affect Your Risk for Tooth Decay?
What you eat and drink has an effect on the health of your teeth and gums. But does drinking out of cans affect your oral health? Here's the scoop.
Read More
Nutrition & Oral Health
Family Dinners and Oral Health: Mouth-Healthy Food Choices and Habits
Read More
Nutrition & Oral Health
Five Halloween Treats for Kids: Keep It Healthy and Spooktacular
If you ask children to name their favorite holiday, chances are that Halloween will rank high on their list.
Read More
Nutrition & Oral Health
How To Rebalance The PH Of Your Mouth
You may not think about it on a daily basis, but your salivary pH is an important part of your oral health. Here's how to rebalance the pH of your mouth.
Read More
Nutrition & Oral Health
Is Popcorn Bad For Your Teeth?
Is popcorn bad for your teeth? Here's what you need to know about how this popular snack can affect your dental health.
Read More
Nutrition & Oral Health
Make Food for Healthy Teeth a Part of Your Family's Diet
Picking out the right food for healthy teeth will go a long way toward keeping your family from dealing with oral problems. Learn more with Colgate.
Read More
Nutrition & Oral Health
Promote Healthy Kids Dental Care With Apple Recipes
Apples are one of the most popular fruits in the world. They are tasty, beautiful and full of vitamins and minerals that keep us healthy.
Read More
Nutrition & Oral Health
What Are The Best Foods For Gum Health?
What are the best foods gum health? Learn about what the current nutrition research says about the best foods for gum health at Colgate® Oral Care.
Read More
Nutrition & Oral Health
What Are the Effects of Sugar on Your Teeth?
What are the effects of sugar on your teeth? Learn about the oral care routine to combat negative impact of sugar on your teeth at Colgate® Oral Care.
Read More
Nutrition & Oral Health
Does Chewing Gum Help You Lose Weight?
Can chewing gum help with weight loss? Click here to find out more information on the health effects of chewing gum with Colgate.
Read More
Brushing & Flossing
How Long Should I Brush? Answering your Toothbrushing Questions
The key to preventing and controlling gum disease is brushing around and under the gumline where bacteria and plaque tend to accumulate. Learn more here.
Read More.jpg)
Brushing & Flossing
5 Healthy-Mouth Habits That You Can Totally Do
Looking for new ways to boost your oral hygiene routine? Here are 5 simple oral care habits to keep your mouth healthy. Start now!
Read More
Brushing & Flossing
5 Tips To Improve Your Confidence And Your Smile
Feeling down about your smile? Fret no more. These 5 tips will help improve your confidence and your smile!
Read More
Brushing & Flossing
All About Silicone Toothbrushes
Having the right toothbrush is as important as the act of brushing your teeth. Learn about whether a silicone toothbrush is right for your oral health.
Read More
Brushing & Flossing
Baby's First Teeth: Should You Use Toothpaste?
When should you start brushing my baby's teeth with toothpaste? Find out here about the easy steps for keeping your little one's teeth in perfect condition.
Read More
Brushing & Flossing
Best Remineralizing Toothpaste For Enamel
The best remineralizing toothpaste for your needs may be an over-the-counter product or a prescription from your dentist. Learn more here how it works.
Read More

Brushing & Flossing
Brushing and Flossing 101
Here are the steps for the best and easiest ways for your oral care health. Use Colgate's techniques and products for brushing and flossing teeth.
Read More
Brushing & Flossing
Brushing Baby's First Teeth
Brushing baby's first teeth is an important process to establish early oral hygiene. Here are tips for when your baby's teeth start to come in.
Read More
Brushing & Flossing
Can an Electric Flosser Make Flossing Easier?
Flossing is an essential part of an oral hygiene routine, but it can be difficult for some people. An electric flosser might make the task easier.
Read More
Brushing & Flossing
Causes And Signs Of Dental Abrasion
Dental abrasion is the result of external mechanical action on the teeth removing the tooth enamel. Learn how to spot and treat this dental issue.
Read More
Brushing & Flossing
Children's Dental Care: Flossing
Although brushing is the focal point of your child's daily dental routine, flossing is just as important. Flossing helps to remove the food particles and plaque that build up between the teeth and gumline… Read more at Colgate.com
Read More

Brushing & Flossing
Disinfecting Toothbrush Tips
Disinfecting toothbrush bristles after an illness leaves them clean and fresh and helps prevent the spread of germs. Here are a few ways to brush up.
Read More
Brushing & Flossing
Do I Need Toothbrush Sanitizer?
Is a toothbrush sanitizer necessary to keep your oral hygiene routine clean at home and on the go? Find out more about toothbrush sanitizers here.
Read More
Brushing & Flossing
Do Your Gums Bleed When Flossing?
If your gums bleed when flossing, you probably need to change your dental care regimen a bit. That doesn't mean your mouth is un...
Read More
Brushing & Flossing
How to Help Your Child Floss
Take the time to teach your kids how to floss properly to ensure that their teeth are healthy and beautiful for years to come.
Read More

Brushing & Flossing
Fight Germs: Keep Your Toothbrush Clean
It's a fact, germs are lurking everywhere. From the people we come in contact with, to the objects we touch throughout the day, we are constantly near them. This is no different for your toothbrush. Learn how to keep it clean here.
Read More
Brushing & Flossing
Five Easy Ways To Improve Dental Health
There's a link between your overall health and your dental health, and not taking great care of the latter can increase your risk for several conditions.
Read More
Brushing & Flossing
5 Ways to Save Water When Brushing Your Teeth
You can protect the environment by contributing to water conservation in simple ways while brushing your teeth. Here are five ways to do so.
Read More
Brushing & Flossing
Flossing Alternatives On The Go
Flossing alternatives can come in handy when you're on the go to keep your smile fresh and clean. Find out more about flossing alternatives, here.
Read More
Brushing & Flossing
Flossing: How Important Is Flossing to You?
How important is flossing to you? Many people hate flossing. Why? Because for many, it may be a challenging task. Here's why you shouldn't skip this step.
Read More
Brushing & Flossing
Flossing Teeth Properly: How To Floss
Choosing the right toothpaste and toothbrush and their regular replacement is important. Use Colgate's techniques and products for brushing and flossing teeth.
Read More
Brushing & Flossing
Garlic & Tooth Pain
Garlic can be used to reduce or stop the pain from toothache because if can kill the bacteria in your mouth. Find out how to use it properly for your tooth pain.
Read More
Brushing & Flossing
Hacks: Forgot Your Toothpaste, Now What?
Whether you forgot to pack your toothpaste don’t have time to pick some up or you realize you ran out before bed, here a few hacks to get you through!”
Read More
Brushing & Flossing
What To Do If Your Child Swallows Toothpaste
For some children, brushing their teeth can be more than a good hygiene practice, it can be an opportunity to snack on some… Read more at Colgate.com
Read More
Brushing & Flossing
The Ancient History of Toothbrushes and Toothpaste
Toothbrushing tools date back to 3500-3000 BC when the Babylonians and the Egyptians made a brush by fraying the end of a twig.
Read More
Brushing & Flossing
How Long Should You Brush Your Teeth For?
If you're concerned about keeping up with good oral hygiene, you may be wondering how long to brush your teeth for the best… Read more at Colgate.com
Read More
Brushing & Flossing
How Often Should You Change Your Toothbrush?
It's easy to know when to replace worn out shoes or faded clothes. But how often should you change your toothbrush? This depends on several factors
Read More
Brushing & Flossing
How Often Should You Clean Your Teeth?
Keeping your teeth clean goes a long way toward keeping them strong and healthy. So, how often should you clean your teeth?… Read more at Colgate.com
Read More
Brushing & Flossing
How Often Should You Floss?
You know that flossing is good for your teeth and gums, but how often should you floss? Here's what you need to know to establish a good flossing habit.
Read More
Brushing & Flossing
How to Take Care of Your Teeth and Gums: 5 Tips for Optimal Oral Health
Read on for a quick refresher on brushing, flossing and eating well for healthy teeth and gums.
Read More
Brushing & Flossing
How To Fight Mouth Germs And Keep Your Smile Healthy
Does the thought of mouth germs taking up residence on your teeth make you feel a little uncomfortable? It should! Masses of harmful microorganisms in...
Read More.png)
Brushing & Flossing
How To Look Forward To Flossing
Incorporate meditation into your flossing routine can benefit both of your oral health and mental health. Learn a simple way to motivate yourself to floss.
Read More
Brushing & Flossing
How To Make Brushing Your Teeth Exciting Each Day
Brushing your teeth may feel like an arduous task, but these tips can make it the best part of your day.
Read MoreBrushing & Flossing
In-Depth Cleaning Brushing Technique
This video demonstrates a brushing technique
Read More
Brushing & Flossing
Infant Dental Care: The Basics
Most babies don't start getting teeth until they are six months old. However, infant dental care is important before teeth emerge. Learn more here!
Read More
Brushing & Flossing
Is Brushing Teeth After Eating Good For You?
Certain foods and drinks - especially those high in carbohydrates and sugars - spur the creation of certain bacteria in your… Read more at Colgate.com
Read More
Brushing & Flossing
7 Essential Tips to Keep Your Teeth Healthy
There is more to keeping your teeth healthy than simple brushing & flossing. Brush up on your oral care with these essential habits for excellent dental health.
Read More
Brushing & Flossing
Looking After Your Teeth: Five New Year's Resolutions For A Healthier Mouth
If you want to take better care when looking after your teeth and gums this year, these five simple resolutions can keep you diligent.
Read More
Brushing & Flossing
Myth Busting: Is Nap Breath A Thing?
Similar to morning breath, sometimes you can get bad breath after napping. Find out what causes nap breath and how you can manage and prevent nap breath.
Read More
Brushing & Flossing
Orange Juice and Toothpaste: Why They Don't Mix
If you've ever taken a sip of OJ after brushing your teeth, you know what a surprise orange juice and toothpaste can be. Learn why, here.
Read More
Brushing & Flossing
3 Possible Causes of Tooth Pain After Brushing
Do you have pain after cleaning your teeth? Pain from brushing and flossing may be a sign that there is something wrong with your oral health or with.
Read More
Brushing & Flossing
How to Store Your Toothbrush Safely
Safe storage for family toothbrushes isn't difficult or complex, but it can help keep extra germs and contaminants away from your toothbrushes and your mouth.
Read More
Brushing & Flossing
Simple Ways To Improve Oral Health: Are You Healthier Than An Olympic Athelete?
Being in better health than an Olympic athlete may not have been on your to-do list, but there are ways to improve oral health beyond the competition.
Read More

Brushing & Flossing
How to Teach Your Children to Brush Their Teeth
Taking care of your child's oral health begins with proper habits. Read more for great tips to teach your children about good oral hygiene with Colgate.
Read More
Brushing & Flossing
Ten Dental Hygiene Tips For A More Thorough Clean
Brushing your teeth every day doesn't guarantee you're giving your mouth all the attention it needs. Consider these dental hygiene tips to ensure it does.
Read More
Brushing & Flossing
The Best Flossing Tools For A Healthy Smile
There are several flossing tools available. Which one is the best tool for you and your mouth? Learn more here.
Read More
Brushing & Flossing
This Is What Happens When You Don't Brush Your Teeth
Here's a 'brush up' on what happens when you don't brush your teeth, and why committing to good oral care benefits your health — and your wallet.
Read More
Brushing & Flossing
Planning Your Back-To-School Oral Care Kits
By putting together these oral care kits for each of your children, you can rest assured they walk in their classroom with a perfect smile.
Read More
Brushing & Flossing
Travel Toothpaste Holder? How To Protect Your Oral Care Supplies On The Go
Protecting your toothbrush and toothpaste, with something like a travel toothpaste holder, can help you maintain good oral care while on the go.
Read More
Brushing & Flossing
Turn Toothbrushing Time Into Family Time
Brushing is vital to your oral health. Now you can make it a healthy routine and a fun family activity for everyone.
Read More
Brushing & Flossing
Using a Floss Threader: Flossing Made Easier
Do you avoid flossing because you have braces, a dental bridge or a permanent retainer? A floss threader may be just the tool… Read more at Colgate.com
Read More
Brushing & Flossing
Using A Proxy Brush To Clean Between Teeth
Some people who have trouble with string floss opt for alternative flossing devices. A proxy brush can serve as another tool in your oral care toolbox.
Read More
Brushing & Flossing
Waxed or Unwaxed Dental Floss? Assessing Your Oral Health Needs
Waxed and unwaxed dental floss are two of the most common types, and they both have their merits. Here's how they differ and how to know which to use.
Read More
Brushing & Flossing
What Are Microbeads In Toothpaste?
Learn more about microbeads in toothpaste and how the recent ban is good news for your health and the environment. Also learn about alternatives.
Read More
Brushing & Flossing
What Is Good Oral Hygiene?
If your gums do hurt or bleed while brushing or flossing, or you are experiencing persistent bad breath, see your dentist. Any of these conditions may indicate a problem.
Read More
Brushing & Flossing
What Is the Right Way to Floss?
Flossing teeth is the quick, effective way to keep your teeth and gums healthy. Discover flossing techniques at Colgate.com and learn the types of floss you should use. Colgate is your partner in dental health so visit us online.
Read More
Brushing & Flossing
Three Tips For Brushing Baby Teeth
Help your children learn good brushing habits as soon as they can pick up a toothbrush. Brushing baby teeth together makes the task productive and fun.
Read More


Brushing & Flossing
Water Flossing vs. Traditional Flossing
Everyone should floss every day, but what method does the best job: traditional or water flossing? Find out more about water flossing and how it compares.
Read More
Brushing & Flossing
Is Over Brushing Your Teeth Bad?
If you care about your oral hygiene, you brush your teeth twice a day. But if frequent brushing is a good thing, then how can over brushing teeth be risky?
Read More
Brushing & Flossing
Dental Tape or Floss: Which Is Best for You?
Flossing is a critical dental health habit that all too often falls by the wayside. Here's how to use interdental products, such as dental tape or floss.
Read More
Brushing & Flossing
How to Brush Your Teeth and Floss Properly
Read on for a quick refresher on brushing, flossing and eating well for healthy teeth and gums.
Read More
Brushing & Flossing
How to Recycle Your Toothbrush
If you’re looking for ways you can go green with your oral care routine, there are steps you can take to help reduce your carbon footprint without sacrificing your oral health.
Read More
Brushing & Flossing
How is a Toothpaste Tube Recycled
Discover what happens to a Toothpaste tube when it is recycled & why it is important with this article from Colgate®
Read More
Brushing & Flossing
Is Dental Floss Eco-Friendly?
Dental floss is one of those materials that can leave you questioning, should I recycle this? Get your answers here!
Read More
Brushing & Flossing
Should You Use Mouthwash Before or After Brushing?
Should you use mouthwash before or after brushing? Here's the answer that will help you improve your daily oral care routine.
Read More
Brushing & Flossing
Beyond the Brush: A Deep Dive Into Dental Hygiene's Unsung Hero
Don't just brush—brush right. A dental professional explains how to choose the best toothbrush, from bristles to head size, for a healthier smile.
Read More
Brushing & Flossing
From Battle to Bonding: Making Brushing Fun for Your Kids
By: Mandy Dennis
Registered Dental Hygienist
Read More

Brushing & Flossing
The Big Switch: Moving from Training to "Big Kid" Toothpaste
By: Dr. Natalie Carr-Bustillo, DDS, MS
Board Certified Pediatric Dentist
Read More
Gum Disease (Gingivitis)
Chlorhexidine Gluconate Mouthrinse: Your Questions Answered
Chlorhexidine gluconate, a prescription oral rinse, is effective in targeting plaque and treating gingivitis and periodontitis. Discover the advantages of using it as a mouthwash.
Read More
Gum Disease (Gingivitis)
5 Causes Of Bleeding Gums When Brushing Your Teeth
Your gums bleed when you brush or floss? What are the possible causes of bleeding gums? Click here to learn more about tooth infections.
Read More.png)
Gum Disease (Gingivitis)
AAP Clears Up Misconceptions About Periodontal Health
The AAP says more than 75 percent of adults over age 35 have a form of periodontal disease, which is characterized by bacterial gum infections. Learn more here.
Read More
Gum Disease (Gingivitis)
Antimicrobial Therapy For Gum Disease
Antimicrobial therapy is a form of oral treatment used to eliminate or reduce the development of bacterial infections in the mouth.
Read More
Gum Disease (Gingivitis)
Are You At Risk For Periodontal (Gum) Disease?
Periodontal (gum) disease is a common inflammatory infection of the gum tissue and bone surrounding the teeth. It's easy to treat if you know if the risks.
Read More
Gum Disease (Gingivitis)
Why Do You Have Bleeding Gums & Bad Breath?
Bleeding gums? Bad breath? Did you know that it may be a sign of gingivitis? Learn more about the symptoms of gum disease.
Read More
Gum Disease (Gingivitis)
Bleeding Gums Treatment
Bleeding gums when you brush or floss is often a symptom of gingivitis, an early stage of gum disease. Learn more about possible treatments.
Read More
Gum Disease (Gingivitis)
Coconut Oil for Receding Gums: Does It Work?
You may have heard that coconut oil helps keep your gums healthy. It's important to speak with your dentist before you use coconut oil for receding gums.
Read More
Gum Disease (Gingivitis)
Dental Scaling And Root Planing To Keep Your Teeth And Mouth Clean
Read More.png)
Gum Disease (Gingivitis)
Do You Know The Signs Of Gingivitis?
Gingivitis (no attachment apparatus loss or bone damage) is a common reversible disease of the oral cavity. In the United States, gingivitis is most...
Read More.png)
Gum Disease (Gingivitis)
Family History Affects Your Risk For Gum Disease
A family history of gum disease increases your risk, hinting at its hereditary nature, according to the American Dental Association.
Read More
Gum Disease (Gingivitis)
Fighting Gum Disease: How To Keep Your Teeth
The good news is that in most people gum disease is preventable. Attention to everyday oral hygiene plus visits to the dentist could keep your teeth healthy and strong.
Read More.png)
Gum Disease (Gingivitis)
Finding A Gingivitis Home Remedy Cure For Your Gums
People seeking a gingivitis home remedy cure have a variety of options available to alleviate their pain, or prevent the problem entirely.
Read More

Gum Disease (Gingivitis)
Four Signs Of Healthy Interdental Papilla
Although it has a complicated-sounding name, interdental papilla have a simple function: It's the term for the gums between your teeth. Learn more.
Read More
Gum Disease (Gingivitis)
Gingival Hyperplasia: What Is It and How Is It Treated?
Gingival hyperplasia is an enlargement or overgrowth of the gum tissue. Learn the facts about gingival hyperplasia, what causes it, and how it is treated.
Read More
Gum Disease (Gingivitis)
Gingivectomy Surgery: What You Need To Know
A gingivectomy may be performed to heal the effects of periodontal disease or to correct a gum condition involving the structure of teeth. Learn more here.
Read More.png)
Gum Disease (Gingivitis)
Gingivitis: Overview And Prevention
Gingivitis is a treatable and reversible form of gum disease. It is the first and mildest stage.
Read More.png)
Gum Disease (Gingivitis)
Gingivitis Treatment Methods For You And Your Family
The easiest type of gingivitis treatment to maintain is a regular brushing, flossing and professional-cleaning routine.
Read More
Gum Disease (Gingivitis)
Gum Disease 101
Gum disease is an inflammation of the gums that can progress to affect the bone that supports your teeth. Find out the causes of gum disease and how to prevent it.
Read More
Gum Disease (Gingivitis)
Gum Disease Treatment For Kids
Teenagers and even younger children are at risk for gum disease or its milder form, gingivitis, which may require a gum disease treatment for kids.
Read More
Gum Disease (Gingivitis)
Gum Disease Treatment Options
Millions of Americans have gum disease but are not aware that they have this serious infection. Periodontal diseases are infections of the gum tissue.
Read More
Gum Disease (Gingivitis)
Gum Graft Pain: What To Expect & How To Relieve Pain
A periodontist performs gum graft surgery to treat gum recession and bone issues. Post-surgery, patients may experience gum graft pain as part of recovery.
Read More
Gum Disease (Gingivitis)
Gum Graft Recovery: What To Expect
If you have gingival recession, your dentist may recommend a gum graft. Here's what you should know about gum graft recovery.
Read More
Gum Disease (Gingivitis)
Gum Grafting Treatment For Receding Gums
Gum recession occurs gradually, and it may sneak up on you. But gum grafting treatment for receding gums can help prevent any further loss of gum tissue.
Read More
Gum Disease (Gingivitis)
4 Simple Causes of Irritated Gums
Gum irritation, or irritated gums, can stem from various sources. Discover key habits that could be causing your gum irritation here.
Read More
Gum Disease (Gingivitis)
Gum Surgery — What Do I Need To Know?
After gum surgery, it is important that the periodontist or dental hygienist inform you how to clean the teeth and gum tissue with a toothbrush and an antimicrobial fluoride toothpaste.
Read More.png)
.png)
Gum Disease (Gingivitis)
How Gum Infection Treatment Changes Based On Condition
Gum disease is an inflammation of the gums that can progress to affect the bone that supports your teeth. Find out the causes of gum disease and how to prevent it.
Read More
Gum Disease (Gingivitis)
How Laser Periodontal Therapy Treats Gum Disease
Gum disease is an inflammation of the gums that can progress to affect the bone that supports your teeth. Find out the causes and how to prevent it.
Read More
Gum Disease (Gingivitis)
How Periodontal Disease Affects Your Lungs
Periodontal disease is a gum condition caused by the buildup of bacteria along the gum line. If left untreated, it can lead to infection within your lungs.
Read More
Gum Disease (Gingivitis)
How Poor Dental Care Can Affect Your Overall Health
Although you probably understand that poor dental care can lead to cavities, did you know that other, more serious health issues can arise? Learn more here.
Read More
Gum Disease (Gingivitis)
How Sore Gums Relate To Your Oral Habits
Sore gums are a problem all ages of people can experience, and for various reasons. Here's the first step in identifying the source of your own pain.
Read More
Gum Disease (Gingivitis)
What to Expect After Deep Cleaning Treatment
Getting a teeth deep cleaning to treat gum disease can remove the infection so your gums can heal. But what happens next? Learn more here.
Read More
Gum Disease (Gingivitis)
How To Identify And Stop Receding Gums
Hairlines aren't the only part of the body that recedes; your gums can, too. Learn how to stop receding gums before they become a problem.
Read More.png)
Gum Disease (Gingivitis)
What Are The Signs Of Gum Disease?
Gum disease goes through a progression of stages, with the later ones posing a serious risk to your oral health. Learn more at Colgate.com Read more at Colgate.com
Read More
Gum Disease (Gingivitis)
How To Treat Gum Disease: What To Do When You Don't Have Dental Insurance
An unfortunate reality is that not everyone can afford to have dental insurance. Poor dental health has a negative effect on… Read more at Colgate.com
Read More.png)
Gum Disease (Gingivitis)
How Treating Gum Disease Varies With Severity
There are two ends to the periodontal (gum) disease spectrum: gingivitis and periodontitis. Treating gum disease depends on the type you have.
Read More
Gum Disease (Gingivitis)
Is Gingivitis Curable?
Gingivitis is an inflammation of the gums around the teeth. Because it is usually painless, or has very mild symptoms, many peop...
Read More.png)
Gum Disease (Gingivitis)
Is Gingivitis Gum Disease?
Many preventable conditions can have similarities that make diagnoses confusing. For example, is gingivitis gum disease? Yes and no.
Read More
Gum Disease (Gingivitis)
Is Gum Contouring Right For You?
Gum contouring changes the line of your gums – whether you have too much or too little – for a healthy and beautiful smile. Learn more here.
Read More
Gum Disease (Gingivitis)
Mouthrinse for Gum Disease: Another Good Tool
Although gum disease comes from bacteria living in your mouth, mouthwash for gum disease is actually the ideal complement to traditional oral care.
Read More.png)
Gum Disease (Gingivitis)
My Experience With Gum Health
Dentists instruct their patients on proper brushing and flossing techniques for good reason. Gum health requires brushing twice a day and flossing.
Read More.png)
Gum Disease (Gingivitis)
Parent Primer: What Is Gum Disease And How Can It Affect Your Child?
What is gum disease? Parents should be aware of it, not only for themselves but for their kids as well, who are just as susceptible to getting it.
Read More
Gum Disease (Gingivitis)
Periodontal Charting: What It Is & Why It's Important
Have you ever noticed that the dental hygienist or dentist was taking measurements of your gums? Periodontal charting is a part of your preventative care.
Read More.png)

Gum Disease (Gingivitis)
What Are the Risk Factors for Periodontitis?
Your gums play an important role in your oral health. Learn more about what causes periodontitis in order to keep your teeth healthy and happy. Click here.
Read More.png)
Gum Disease (Gingivitis)
Prevent Gum Disease With The Right Oral Care Products
Do you have what it takes to stop plaque from harming your mouth? The first stage of gum disease, gingivitis, is caused by plaque that has built up...
Read More.png)
Gum Disease (Gingivitis)
Professional Gingivitis Treatment And Home Care
If you have tender, red, swollen, and bleeding gums you will need gingivitis treatment. This is the earliest form of gum disease that can resolve with...
Read More
Gum Disease (Gingivitis)
How to Fix Gum Recession
Receding gums cannot grow back. However, your dentist or periodontist can help you treat and prevent it from getting worse.
Read More.png)
Gum Disease (Gingivitis)
Receding Gums Treatment: Surgical Options
Receding gums can lead to serious oral health problems when the problem is ignored. To keep your mouth healthy, look into receding gums treatments.
Read More
Gum Disease (Gingivitis)
Reverse Gum Disease: Don't Miss Your Window Of Opportunity
Treating diseases early on is key to preventing serious health problems, and the same goes for gum disease. Reversing gum disease early on can be easy.
Read More
Gum Disease (Gingivitis)
Safe Home Gingivitis Remedies To Complement Your Regular Cleaning
In addition to regular preventive care like brushing and flossing, safe-at-home gingivitis remedies may help you address plaque buildup on your teeth.
Read More
Gum Disease (Gingivitis)
Why Do My Gums Hurt? Causes & Treatments
Worried about bleeding or sore gums? Find out what may be causing them and what you can do to prevent gum pain and damage. Learn more.
Read More
Gum Disease (Gingivitis)
What Treatments Can Fix Periodontal Disease?
Successful treatment options are now available for advanced periodontal disease, so losing teeth doesn’t have to be your next option due to an unhealthy gumline.
Read More.png)
Gum Disease (Gingivitis)
Symptoms Of Gingivitis And Tips For Prevention
What Is Gingivitis?Symptoms of gingivitis start with just a mild inflammation of the gum tissue. Many people do not initially re...
Read More
Gum Disease (Gingivitis)
When Do My Teeth Need a Deep Cleaning?
Deep cleaning is not necessary for every patient but is recommended for those suffering from gingivitis. Learn more about what is it and when you need it.
Read More.png)
Gum Disease (Gingivitis)
The Three Phases Of Periodontal Disease Symptoms
Familiarizing yourself with periodontal disease symptoms is critical to a lifetime of oral care.
Read More.png)
Gum Disease (Gingivitis)
Understanding Diabetes Gum Problems
Due to the prevalence of diabetes, it is critical to know how it can affect your body, and what to do if you detect gum problems.
Read More
Gum Disease (Gingivitis)
What Are Periodontal Pockets?
Periodontal pockets signal advancing gum disease, highlighting the critical separation between gums and teeth that endangers bone support.
Read More
Gum Disease (Gingivitis)
What Are The Stages Of Gum Disease?
Gum disease is an inflammation of the gums that can progress to affect the bone that supports your teeth.
Read More
Gum Disease (Gingivitis)
What Causes A Black Spot On Gums?
A black spot on gums can have different causes and may prove a difficult diagnosis for your oral health care provider. Find out more about the causes here.
Read More.png)
Gum Disease (Gingivitis)
What Causes Bleeding Gums?
What causes bleeding gums? This usually is a sign of gum disease, also known as gingivitis. Gingivitis is an inflammation of the gums and one of the...
Read More
Gum Disease (Gingivitis)
What Dental Hygienists Do When Scaling and Root Planing Teeth
Routine cleanings prevent gum disease, while scaling and root planing, involving teeth scaling, treat it by removing plaque and tartar below the gum line.
Read More.png)
Gum Disease (Gingivitis)
What Does Gingivitis Treatment Entail?
Receiving a diagnosis of gingivitis can be alarming at first, but the good news is that gingivitis is actually a mild form of gu...
Read More
Gum Disease (Gingivitis)
What Is A Furcation Defect?
Periodontitis, or advanced gum disease, causes various complications, notably furcation defects, where tooth roots divide, impacting oral health.
Read More
Gum Disease (Gingivitis)
What Are the Signs and Symptoms of Gingivitis?
Gingivitis is an inflammation of the gums and a symptom of the first stages of gum disease. Learn more about gingivitis symptoms and treatment here.
Read More.png)
Gum Disease (Gingivitis)
What Is Gum Disease?
Have you ever noticed a pink tinge on your toothbrush after brushing? It may have made you wonder if you have gum disease. So, what is gum disease?
Read More.png)
Gum Disease (Gingivitis)
What Is Periodontal Disease And How Can It Be Prevented?
What is periodontal disease's greatest enemy? Regular oral hygiene.
Read More
Gum Disease (Gingivitis)
What Is The Best Toothpaste For Gingivitis?
What is the best toothpaste for gingivitis? Brushing with the right toothpaste can help to protect against gingivitis and prevent it later. Read more from Colgate.
Read More
Gum Disease (Gingivitis)
What Is The Periodontium?
The periodontium surrounds and supports the tooth roots. Gum disease and periodontal disease affect this area and may cause bleeding and tooth loss.
Read More
Gum Disease (Gingivitis)
What Is Trench Mouth?
Trench mouth is one of the most serious and troublesome forms of gum disease. Understanding the risk factors for trench mouth is crucial to its prevention.
Read More
Gum Disease (Gingivitis)
What To Do If You Spot Gingivitis Symptoms?
Gingivitis is the only stage of gum disease that's fully reversible. The sooner you spot gingivitis symptoms, the quicker your mouth can return to normal.
Read More
Gum Disease (Gingivitis)
Why Do You Have Itchy Gums?
Itchy gums are typically caused by plaque buildup. Check in with your dentist so they can properly examine your gums and teeth.
Read More.png)
Gum Disease (Gingivitis)
Why Is Mouthwash For Bleeding Gums Beneficial?
Bleeding gums are an early sign of gum disease. Using an antimicrobial mouthwash for bleeding gums can help stop it in its tracks. Here's how it works.
Read More.png)
Gum Disease (Gingivitis)
Working Toward A Gingivitis Cure
Gingivitis is a common oral disease that affects people of all ages. In fact, some experts believe most individuals have some form of gingivitis....
Read More
Gum Disease (Gingivitis)
What is Crown Lengthening?
Unless you're a dental trivia champion, the term crown lengthening probably isn't familiar to you. However, crown lengthening procedures are actually pretty common. Learn more about this procedure.
Read More
Gum Disease (Gingivitis)
Can Receding Gums Grow Back?
Receding gums, or gum recession, result from harsh brushing to teeth grinding. Discover the causes and treatments for this condition.
Read More
Gum Disease (Gingivitis)
What To Do About Gum Swelling
Swollen gums are a common problem and can have a number of different causes. Learn more about what to do if you are experiencing gum swelling here.
Read More.png)
.png)
Gum Disease (Gingivitis)
Severe Gingivitis And Your Children
Although gingivitis is the earliest and mildest form of gum disease, severe gingivitis can lead to chronic cases that require more diligent management.
Read More
Gum Disease (Gingivitis)
Things You Can Do If Your Gums Are Bleeding
Altering your oral care routine can lead to bleeding gums, at least initially. Here's how to respond if you notice some bleeding from your gums.
Read More
Gum Disease (Gingivitis)
All About Aggregatibacter Actinomycetemcomitans
Of the thousands of bacteria living in your mouth, some are helpful but others can be harmful. Learn about Aggregatibacter actinomycetemcomitans.
Read More
Gum Disease (Gingivitis)
What Is Strawberry Gum Disease?
What is strawberry gum disease? Click here to read more about strawberry gum disease and the signs with Colgate.
Read More
Gum Disease (Gingivitis)
Periodontal Disease & How You Can Prevent It
Are your gums tender or bleeding? Learn about the causes, treatments, and preventative measures for periodontal disease in this detailed guide.
Read More
Gum Disease (Gingivitis)
Can Receding Gums Grow Back?
While receding gums don't grow back on their own, you can talk to your dentist or periodontist about treatments to correct the issue and prevent it from getting worse.
Read More
Gum Disease (Gingivitis)
The Connection Between Porphyromonas Gingivalis and Gum Disease
Porphyromonas gingivalis is a species of bacteria that is closely linked to advanced periodontal disease. Here's what to know to keep your mouth healthy.
Read More
Gum Disease (Gingivitis)
How to Cure Gingivitis
Seeking a gingivitis home remedy? Learn more about options available to alleviate pain, or prevent the problem entirely.
Read More
Gum Disease (Gingivitis)
The Link Between Gum Disease and Blood Pressure
Discover the link between gum disease and its potential role in causing high blood pressure. Understand how oral health can influence your blood pressure.
Read More
Gum Disease (Gingivitis)
Beat the Bleeding: Why Your Gums Bleed (And How to Fix It)
By: Mandy Dennis, RDH
Read More
Gum Disease (Gingivitis)
What Type of Mouthwash is Right for Me?
By: Ann Eshenaur Spolarich, RDH, PhD, FSCDH
Read More
Tooth Sensitivity
Are Your Teeth Sensitive to Sugar?
Did you know that your teeth can be sensitive to sugar? Read on to know the signs of tooth sensitivity and how to treat it at Colgate Oral Care.
Read More
Tooth Sensitivity
Budget Friendly Sensitive Teeth Treatment Options?
Learn more about teeth sensitivity. Find out how teeth sensitivity is caused, and how you can not only treat sensitivity, but prevent it in the future. Find out more, today!
Read More
Tooth Sensitivity
Causes And Treatments Of Extremely Sensitive Teeth
Find out what causes extremely sensitive teeth and discover effective treatments and home remedies to manage pain and find lasting relief.
Read More
Tooth Sensitivity
Exposed Tooth Root: Causes And Symptoms
An exposed tooth root may be the cause of your tooth pain. Learn more about these causes, symptoms and treatment of an exposed tooth root here.
Read More
Tooth Sensitivity
How Does Mouthwash for Sensitive Teeth Work?
Regular rinsing with mouthwash for sensitive teeth can actually bring relief to many who suffer from tooth sensitivity. Here's how it kills the pain.
Read More
Tooth Sensitivity
How Sensitive Teeth Can Occur And How To Respond
Learn more about teeth sensitivity. Find out how teeth sensitivity is caused, and how you can not only treat sensitivity, but prevent it in the future. Find out more, today!
Read More

Tooth Sensitivity
How To Pursue Sensitive Teeth Treatment
Ice cream is a futile craving if you have sensitive teeth. With the proper sensitive teeth treatment, you can dive right (back) into your favorite flavor.
Read More
Tooth Sensitivity
How to Stop Sensitive Teeth
Although desensitizing toothpastes can help ease the pain, you might wonder how to help sensitive teeth naturally and skip the pain next time.
Read More
Tooth Sensitivity
How Tooth Nerve Pain Occurs
Understand the causes of tooth nerve pain and find effective solutions with Colgate. Learn how to manage sensitivity and protect your smile from dental nerve discomfort.
Read More
Tooth Sensitivity
Is Sparkling Water Bad For Your Teeth?
Is sparkling water bad for your teeth? Discover the effects on dental health and practical advice to safeguard your teeth while enjoying sparkling water.
Read More
Tooth Sensitivity
Managing Sensitive Teeth After Whitening
Tooth whitening is a great option for the removal of surface stains and discoloration. However, many people experience sensitive teeth after whitening.
Read More
Tooth Sensitivity
Potential Causes of Toothaches: It’s Not Always a Cavity
Discover effective toothache relief and causes. Get tips on prevention and treatments for lasting oral health.
Read More
Tooth Sensitivity
Preventing and Treating Exposed Dentin
Exposed dentin can be annoying and painful, but there are many ways to prevent enamel erosion and treat tooth sensitivity. Find out more, with Colgate®.
Read More
Tooth Sensitivity
Sensitive Gums? Here Are Three Surprising Causes
Gum disease is typically to blame for sensitive gums, but there may be another issue hiding right under your nose. Here are a few causes of sensitive gums.
Read More
Tooth Sensitivity
Why Are My Teeth Sensitive After A Dental Cleaning?
Whether you have sensitive teeth or gums, they're both a recipe for oral pain. Find out the difference between gum and tooth sensitivity at Colgate® Oral Care.
Read MoreTooth Sensitivity
Sensitive Teeth To Cold What You Should Know
Determine the cause of your tooth sensitivity and the possible treatments available.
Read More
Tooth Sensitivity
The Best Toothpaste for Sensitive Teeth: What's in It?
Explore the best toothpastes for sensitive teeth on Colgate, designed to reduce discomfort and strengthen enamel for a healthier smile.
Read More
Tooth Sensitivity
Three Sensitive Teeth Treatment Options When You're On A Budget
Learn more about teeth sensitivity. Find out how teeth sensitivity is caused, and how you can not only treat sensitivity, but prevent it in the future. Find out more, today!
Read More
Tooth Sensitivity
Tooth Whitening at Home: Four Ways to Stop Sensitivity
Discover effective remedies for tooth sensitivity after whitening with our guide on safe at-home tooth bleaching techniques.
Read More
Tooth Sensitivity
Tooth Pain: What Could It Mean?
You go to the dentist every six months. You are cavity free. So what is the deal with all of this tooth pain? Learn more about tooth pain causes here.
Read More
Tooth Sensitivity
Tooth Recession
Learn about tooth recession which happens when the gums recede or pull away from the teeth leaving the root surface exposed.
Read More
Tooth Sensitivity
Tooth Sensitive to Hot or Cold? What It Means and How to Help
Discover why your teeth react to hot and cold and find effective solutions for tooth sensitivity. Get expert advice and tips for relief.
Read More
Tooth Sensitivity
Dentin Hypersensitivity Diagnosis and Solutions
Learn more about dentin sensitivity. Find out how teeth sensitivity is caused, and how you can not only treat hypersensitivity, but prevent it in the future. Find out more, today!
Read More
Tooth Sensitivity
Toothpaste For Sensitive Teeth Can Help Relieve The Pain
Using special toothpaste for sensitive teeth is one of the most common methods that dentists try with the many patients dealing with sensitive teeth.
Read More

Tooth Sensitivity
How To Treat Sensitive Teeth
Explore effective treatments for tooth sensitivity on Colgate. From fluoride applications to desensitizing toothpaste, find relief for sensitive teeth.
Read More
Tooth Sensitivity
What Causes Tooth Sensitivity & How to Treat It
Approximately 40 million adults in the United States experience tooth sensitivity. So what causes sensitive teeth? Any number of dental problems. Find your answers here.
Read More

Tooth Sensitivity
Why Are My Teeth Sensitive? Is It Related To Age?
Every day, people ask themselves,
Read More
Tooth Sensitivity
Why Does Tooth Sensitivity Occur?
Major factors that lead to tooth sensitivity are gum recession and loss of cementum, and loss of enamel. Learn what causes it and how to prevent it, here.
Read More
Tooth Sensitivity
Potassium Nitrate Dental Uses: Relieving Your Tooth Sensitivity
For tooth sensitivity, consider potassium nitrate toothpaste, recommended by dentists for its benefits. Learn how potassium nitrate for teeth improves oral health.
Read More
Tooth Sensitivity
Should You Use Non-Mint Toothpaste for Sensitive Teeth?
Suffering from sensitive teeth & looking for a toothpaste alternative? Learn about whether mint-free toothpaste is right for you.
Read More
Cracked Tooth Syndrome
Cracked Front Tooth: What You Can Do
Accidents happen, and when these accidents involve your mouth, they can sometimes lead to a cracked front tooth. Learn about treating a cracked front tooth, here.
Read More
Cracked Tooth Syndrome
Cracked Tooth Syndrome 101
Learn more about cracked tooth syndrome at Colgate® Oral Care. Find out about the symptoms, causes, and treatments for cracked tooth syndrome, here.
Read More
Cracked Tooth Syndrome
Detecting and Treating a Cracked Tooth
While you may think that a cracked tooth would be difficult to overlook, the truth is that many people have trouble spotting this dental problem. Learn more, here.
Read More
Cracked Tooth Syndrome
What To Do if You Have a Cracked Molar
What do you do if you have a cracked molar? Molars are vulnerable to cracks because they absorb most of the force during chewing. Learn more, here.
Read More
Cracked Tooth Syndrome
What is Cracked Tooth Syndrome?
Some teeth have cracks too small to show up on X-rays, or cracked are under the gum. These small cracks are known as cracked tooth syndrome. Learn more here.
Read More
Teeth Bonding
Acid Etching: How Does It Work?
Acid etching is used to successfully bond existing tooth structure with a prosthetic or repair, whether it be a crown, a filling or a veneer. Learn more.
Read More
Teeth Bonding
How Long Does Tooth Bonding Last?
Before deciding if this composite resin is appropriate for you, consider this about the procedure's result: How long does tooth bonding last? Learn more.
Read More
Teeth Bonding
Improving My Smile: Tooth Whitening and Tooth Bonding
Bonding uses composite resins or veneers to cover the surface of stained teeth and give a nice even appearance to broken or misshapen teeth. Learn more.
Read More
Teeth Bonding
Is Composite Resin Bonding Right For You?
Composite resin bonding can be a fast, minimally invasive option for the beautiful smile you're looking for. Here's what to expect for your investment.
Read More
Teeth Bonding
Teeth Bonding Disadvantages to Consider
Although bonding does have some major advantages over crowns and veneers, there are also a few teeth bonding disadvantages worth considering.
Read More
Teeth Bonding
Teeth Bonding for Gaps Between Your Front Teeth
Teeth bonding for gaps may be a suitable treatment for you, and if not, you should be open to similar treatment methods. Here's what the procedure entails.
Read More
Teeth Bonding
Tooth Bonding: Before, During, and After
Tooth bonding is a simple and relatively comfortable procedure for those who need to restore broken or weakened teeth. Here's what you can expect.
Read More
Teeth Bonding
What Is Tooth Bonding?
There are endless ways to chip a tooth & one solution is tooth bonding. Click here to learn more about tooth bonding with Colgate®
Read More
Oral Care: Teens (13-17)
What Is Orthodontics?
The benefits of orthodontic treatment include a healthier mouth, a more pleasing appearance, and teeth that are more likely to last a lifetime.
Read More
Oral Care: Teens (13-17)
Preventing Obesity in Children and Teens
The CDC has also reported that, as the prevalence of obesity increased among children and adolescents, incidents of tooth decay also rose, which suggests a link between dental health and weight
Read More
Oral Care: Teens (13-17)
Hawley Retainer: Proven To Maintain Your Straight Smile
The hawley appliance is one of the oldest types of retainers used post-treatment. A removable item, it's made of a combination of plastic and metal that is molded custom to fit your mouth.
Read More
Oral Care: Teens (13-17)
What Is A Compound Odontoma?
A compound odontoma might sound like a scary diagnosis, but the growth is typically harmless. Learn more about how these tumors are diagnosed and treated.
Read More
Oral Care: Teens (13-17)
Can Your Kid Play Football If He Has Braces?
There are many options to choose from when considering a mouthguard for your football player, and deciding which type of mouthguard is best can be confusing. Learn more here.
Read More
Special Occasions
How To Prevent Cavities From Halloween Candy
It is nearly impossible to avoid Halloween candy altogether, but there are some simple and fun ways in which you can minimize the sugar overload after trick-or-treating is over.
Read More
Special Occasions
Fun Holiday Treats For Kids With Braces
When preparing a few fun holiday treats with your child, you can include numerous healthy options that build strong teeth and go easy on braces.
Read More

Special Occasions
Worst Candy for Teeth Around the Holidays
The holiday season is a time when many folks indulge in sugary treats. Find out which of these are the worst candy for teeth, and what to do about it.
Read More
Special Occasions
How To Look Great In Wedding Day Photos
A wedding might only last for a single day, but wedding day photos are forever. Although in 10 years' time you might look back and wonder what you were...
Read More
Special Occasions
A New Year's You: Dental Health Resolutions
Your dental health is an important part of your overall wellness, and the New Year is a great time to create resolutions for improving your health.
Read More
Special Occasions
How to Celebrate National Children’s Dental Health Month this February
With a focus on hygiene and health, National Children's Dental Health Month may be even more important than Valentine's Day this February.
Read More
Special Occasions
Family Dinners And Oral Health: 5 Tips For Mouth-Healthy Food Choices And Habits
When it comes to family dinners and oral health, follow these tips to reinforce good eating and oral health habits.
Read More
Special Occasions
How to Get a Wedding Day Smile
Let's show brides & grooms-to-be how to get the wedding smile of their dreams. Follow this simple timeline so your teeth can look as fabulous as they feel.
Read More
Special Occasions
How To Make Your Teeth White For The Holidays
Looking for sparkling teeth this holiday season? Check out our teeth whitening guide from Colgate for white & bright just in time for all your holiday photos.
Read More
Oral Care: Adults (55+)
Edentulism: How Can You Avoid This Common Condition?
Total adult tooth loss, also known as edentulism, affects many people in the United States. How can you keep your teeth as you age? Learn more here.
Read More
Oral Care: Adults (55+)
Oral Care Age 55+ 101
Learn more on oral hygiene and oral health for seniors, including dentures and dental implants, bone augmentation, tuberosity reduction and more.
Read More
Oral Care: Adults (55+)
Oral Health for Seniors
Good dental hygiene habits are important at any age. Learn about how your dentist can help you with your oral health in your senior years. Click here today.
Read More

Oral Care: Adults (55+)
Dental Health After 45: A Proactive Guide to Staying Smile-Strong
By: Mandy Dennis
Registered Dental Hygienist
Read More
Oral Care: Babies (0-4)
Teething Biscuits to Soothe Your Baby
When your baby is teething, there are a few do's and don'ts to relieve the discomfort. Are teething biscuits OK for your baby? Find out more, here.
Read More
Oral Care: Babies (0-4)
Teething Gel: Cautions And Alternatives
Because it causes pain, teething can be a challenging time for both parent and child. In the past, the application of teething. Read more at Colgate.com
Read More
Oral Care: Babies (0-4)
Teething Remedies That Aren't Worth The Risk
Find out about oral care & oral health for infants, including when to start brushing baby teeth, baby toothpaste, and more, from the Colgate Oral Care Center.
Read More.jpeg)
Oral Care: Babies (0-4)
When Should Babies Stop Using Bottles?
When should babies stop using bottles? Here are some signs that indicate that they're ready for a cup, as well as tips on how to transition successfully.
Read More
Oral Care: Babies (0-4)
When To Take Your Toddler To The Dentist
Taking a child to his first dental visit can be a bit daunting for a new parent. You may have questions about when to take your toddler to the dentist.
Read More
Oral Care: Babies (0-4)
Will My Baby Develop Pacifier Teeth?
Many parents are concerned that pacifiers can cause dental problems. With proper use, however, your baby can find comfort in it without pacifier teeth.
Read More
Oral Care: Babies (0-4)
Your Baby's Binky: The Pros And Cons
A binky, also known as a pacifier, has been a comforting tool for babies for the generations. Sucking is a natural way for babies to comfort themselves.
Read More
Oral Care: Babies (0-4)
Your Baby's First Tooth: What To Expect
Do you see a white bud that could be your baby's first tooth? Between four & six months of age, your little angel will begin teething. Read more at Colgate.com
Read More.jpeg)
Oral Care: Babies (0-4)
Your Child's Pacifier Habits: Possible Complications
To make a fully informed decision, it is important to know the pros & cons of pacifiers, taking into consideration your child's age and individual temperament.
Read More
Oral Care: Babies (0-4)
Getting Dental Work and Breastfeeding: Is It a Good Idea?
Can you get dental work while breastfeeding? Click here to learn more about dental health routine to keep your body in the best condition with Colgate®.
Read More
Oral Care: Babies (0-4)
What Causes Baby Snoring and What Should You Do About It?
Here are some common causes of baby snoring and when you should seek medical advice or treatment.
Read More
Oral Care: Babies (0-4)
What Is an Orthodontic Pacifier?
A binky is a source of comfort for many infants, but it can be confusing to choose the right one. Here's what to know about an orthodontic pacifier.
Read More
Oral Care: Babies (0-4)
Breastfeeding And Teething: Your Baby's Oral Health
Welcoming a newborn into the world is exciting for the whole family, but as most new mothers now, breastfeeding and teething will be your immediate focus.
Read More
Oral Care: Babies (0-4)
Baby's First Smile and Laugh: How to Get Your Infant to Giggle
Nothing is more precious than the playful giggle of an infant. If you haven't heard it yet, here's how to get your baby to laugh.
Read More
Oral Care: Babies (0-4)
More Than Just a Cute Smile: Why Your Baby’s Tiny Teeth Are a Big Deal
By: Mandy Dennis
Registered Dental Hygienist
Read More
Discover your smile’s perfect match
Explore our unparalleled range of oral health science-backed products and solutions tailored to meet your smile goals. Use our tool and find your perfect match!
Discover your smile’s perfect match
Explore our unparalleled range of oral health science-backed products and solutions tailored to meet your smile goals. Use our tool and find your perfect match!
ORAL HEALTH QUIZ
What's behind your smile?
Take our Oral Health assessment to get the most from your oral care routine
ORAL HEALTH QUIZ
What's behind your smile?
Take our Oral Health assessment to get the most from your oral care routine





